People at the Heart of Care: adult social care reform
Updated 18 March 2022
Applies to England
Presented to Parliament by the Secretary of State for Health and Social Care.
December 2021
CP 560
ISBN 978-1-5286-3015-3
Correction slip
Title
People at the heart of care. Adult social care reform white paper
Session: 2019 to 2021
CP 560
ISBN: 978-1-5286-3015-3
Correction 1
Page 35, Section 4.9 – text currently reads:
We will therefore invest at least £300 million for the period 2022 to 2023 through to 2025 to 2026.
Text should read:
We will therefore invest at least £300 million for the period 2022 to 2023 through to 2024 to 2025.
Date of correction: 10 December 2021
Correction 2
Page 36, Section 4.15 – text currently reads:
Therefore, we will continue to invest in the Care and Support Specialised Housing (CASSH) Fund, with £70 million per year capital funding available per year between 2022 to 2023 and 2025 to 2026
Text should read:
Therefore, we will continue to invest in the Care and Support Specialised Housing (CASSH) Fund, with £71 million per year capital funding available per year between 2022 to 2023 and 2024 to 2025
Date of correction: 10 December 2021
Foreword by the Secretary of State
For too long, successive governments have ignored the challenges facing adult social care.
That changed on 7 September 2021 when the Prime Minister set out long overdue reforms for how people in England will pay for their social care. From October 2023, no one will be forced to pay unlimited and unpredictable costs for their care, giving them the certainty and peace of mind that this government will step in and look after those most in need of support.
How individuals pay for their social care is not the only challenge the sector is facing. That is why today, following the commitment to system reform in the Prime Minister’s September announcement, we are setting out the next steps on our social care reform journey. And I stress that it is a journey. The proposals outlined will not solve all of the problems, but they are a significant step in moving us towards a new vision for social care that the whole of government is committed to.
For the vast majority of people, care begins at home. Carers play a vital role in our communities and we all owe them a debt of gratitude. And so our vision for adult social care puts people and families at its heart. It is a vision that:
- offers people choice and control over the care they receive
- promotes independence and enables people to live well as part of a community
- properly values our exemplary and committed social care workforce, enabling them to deliver the outstanding quality care that they want to provide
- recognises unpaid carers for their contribution and treats them fairly
To deliver on this vision, I want to encourage investment and innovation right across the sector, to shift away from a reliance on residential care, and offer people genuine options for drawing on outstanding care at home and in the community. The new funding for our workforce, housing and innovation are just a handful of the proposals that will start to make our vision a reality.
This vision is a shared vision shaped by national and local government, care providers, care staff, the NHS, and those who draw on care and support and their carers. I am immensely grateful for the input and support that these groups have provided in developing our vision and the policies within this white paper. I look forward to continuing to work with these groups over the months and years ahead.
Executive summary
The government is firmly committed to reforming adult social care. We want people who draw on care and support to lead a fulfilling life, playing a full role in society. We want to acknowledge the important role of families and friends in caring for one another, while also enabling those who provide unpaid care to a friend or loved one to be supported to achieve their own life goals. We want the adult social care workforce to feel recognised and to have opportunities to develop their careers.
This white paper, People at the Heart of Care, sets out an ambitious 10-year vision for how we will transform support and care in England[footnote 1]. Our vision puts people at its heart and revolves around 3 objectives:
-
People have choice, control and support to live independent lives.
-
People can access outstanding quality and tailored care and support.
-
People find adult social care fair and accessible.
Person-centred care is a key theme running through this vision. Genuine choice and control about personalised care and support can enhance quality of life and promote independence in a way that matters to individuals. We know that there are already strong examples of our vision in action, where people can choose the type of care and support that really works for them, happening in pockets across the country. Therefore, an important part of what we want to do is make this happen more consistently, so that everyone – no matter where they live – can benefit.
We are not starting from scratch. The Care Act 2014 – particularly its focus on wellbeing – provides a strong foundation for our vision. We recognise that the ambition of the Care Act has not consistently been achieved in the way we would have liked. New measures currently going through Parliament will strengthen how care and support is delivered. and give us the tools to ensure we deliver on both the letter and the spirit of the Care Act.
To take us further towards our 10-year vision, this document sets out a range of policies that we will work with the sector and those who draw on care and support to implement over the next 3 years. These include:
- at least £300 million to integrate housing into local health and care strategies, with a focus on increasing the range of new supported housing options available. This will provide choice of alternative housing and support options
- at least £150 million of additional funding to drive greater adoption of technology and achieve widespread digitisation across social care. Digital tools and technology can support independent living and improve the quality of care
- at least £500 million so the social care workforce have the right training and qualifications, and feel recognised and valued for their skills and commitment. We want the workforce to also have their wellbeing prioritised
- a new practical support service to make minor repairs and changes in people’s homes to help people remain independent and safe in their home, alongside increasing the upper limit of the Disabilities Facilities Grant for home adaptations such as stairlifts, wet rooms and home technologies
- up to £25 million to work with the sector to kick-start a change in the services provided to support unpaid carers
- £30 million to help local areas innovate around the support and care they provide in new and different ways, providing more options that suit people’s needs and individual circumstances
- a new national website to explain the upcoming changes, and at least £5 million to pilot new ways to help people understand and access the care and support available
- more than £70 million to increase the support offer across adult social care to improve the delivery of care and support services, including assisting local authorities to better plan and develop the support and care options available
There are many more things we are doing over the next 3 years contained in this white paper. These proposals are backed by the new Health and Social Care Levy announced in September this year, of which £5.4 billion is being invested into adult social care over the next 3 years. Beyond the next 3 years, an increasing share of funding raised by the levy will be spent on social care in England.
Why 10 years? We know that some of the challenges in social care cannot be quickly fixed. Therefore, over the months and years ahead, we will continue working with a range of voices from across the care and support landscape to deliver the changes that we all want to see. This will include working closely with local authorities and supporting them, so they have the right tools and capability to deliver the right care and support that puts wellbeing and personalised support front and centre.
We will also engage with a diverse range of organisations and people, including those who draw on care and support or provide unpaid care, to consider how we can measure success of our 10-year vision.
Who cares
Social care is at the heart of our communities, providing support to those who need it so that as many people as possible can live the life they want to lead. It matters to everybody, yet people’s experiences of social care – either those who draw on formal care and support, their families, unpaid carers or the social care workforce – can vary widely.
People who draw on care and support
The scale of social care and support is vast – affecting the lives of over 10 million adults of all ages in England[footnote 2] at any one time. People draw on care and support in different ways and at different stages of their life – for example, after a hospital stay or discharge from a mental health inpatient facility. Some people will require support throughout their life and become experts in their own care needs. For others, care needs develop suddenly or, for others, gradually, and they will have to navigate an unfamiliar landscape at a uniquely stressful time of their life. Some people may only use social care for a short period – for example, after a hospital stay.
Social care supports adults of all ages – including young people moving into adulthood and those of working age – with a diverse range of needs, including:
- autistic people
- people with a learning disability or physical disability
- people with mental health conditions
- people with sensory impairments
- people who experience substance misuse
- people with dementia
- other people with long-term conditions
Care and support cover a wide range of activities to promote people’s wellbeing and support them to live independently, staying well and safe. It can include ‘personal care’, such as support for washing, dressing and getting out of bed in the morning, as well as wider personalised support to enable people to stay engaged in their communities and live their lives in the way they want. This can include support to engage in work, training, education or volunteering, or support to socialise with family and friends and maintain personal relationships.
In 2020 to 2021, local authorities received over 1.9 million requests for support from 1.3 million new clients[footnote 3]. In total, 841,000 people were receiving state-funded long-term care in 2020 to 2021[footnote 3]. Demand for social care services will continue to grow[footnote 3] as a result of better diagnosis, higher survival rates for premature babies and longer life expectancies[footnote 3]. In addition to these long-run trends, the legacy of the coronavirus (COVID-19) pandemic on both physical and mental health will also contribute to future demand for social care.
People who provide support and care
The care and support workforce are our biggest asset. Trusting relationships with carers provide the bedrock for outstanding social care. It is a relationship built over time, and one which gives people confidence that their care needs are well understood and will be consistently met.
There are a huge number of people across the country who provide support and care. Over 1.5 million individuals – representing 4.6% of the 32.4 million people employed in England[footnote 4] – work in partnership with families and communities across the country to provide support and care. The workforce covers (among others):
- care workers
- personal assistants
- social workers
- occupational therapists
- registered nurses
- housing support workers
- those in managerial roles
We rely on the crucial contribution of those who provide care to a family member, friend or neighbour[footnote 5], either in part or totality. We will continue to celebrate and support the amazing work they do. This encompasses a diverse range of people, whose roles may differ – for example:
- young or older carers
- carers of people with dementia or for people who have had a stroke
- employed carers providing a high volume of care per week
- economically inactive carers.
Unpaid care is provided by people of all ages. Many carers have jobs and other caring responsibilities. Carers are people who often have their own jobs, life pressures and things that matter to them. We know that the support provided by unpaid carers is often physically and emotionally demanding, with consequences for carers’ own health and wellbeing. While many carers enjoy caring for their loved one, it should not define them unless they wish it to.
This white paper
On 7 September 2021, we announced £5.4 billion over 3 years solely for adult social care reform. At the Spending Review in October, we announced that this investment will be used for the following areas:
- £3.6 billion to pay for the cap on care costs, the extension to means test, and support progress towards local authorities paying a fair cost of care, which together will remove unpredictable care costs
- £1.7 billion to improve social care in England, including at least £500 million investment in the workforce
This white paper describes our priorities for investment in social care and describes where the money will be used. This investment in adult social care is being funded from the new Health and Social Care Levy. As we implement the cap on care costs and remove the unpredictable care costs people can face, the proportion of the levy that is required to support investment in adult social care in England will increase.
Today, we outline an ambitious strategy of reform that will touch on all those who interact with adult social care, whether that’s those who draw on support and care, unpaid carers, the care and support workforce, care providers both large and small and for and not-for-profit, local authorities, voluntary organisations and others.
This white paper is the product of extensive engagement with the adult social care sector, and we are grateful to the hundreds of organisations and individuals who have contributed to its development (see Annex A). We are particularly grateful to Think Local Act Personal and the Health and Wellbeing Alliance for facilitating direct engagement with people with lived experience of care and support, whose views are so important in getting reform right. No significant reform can be achieved by central government alone, and we look forward to continuing to work with the local authorities, think tanks, professional bodies, charities, care providers, unions and people with experience of care to deliver this white paper.
The remainder of this document starts by outlining our 10-year vision for adult social care followed by a summary of opportunities that we want to build on to achieve our vision . We then set out a number of policy chapters that will move us towards achieving our vision, covering areas such as:
- housing, technology and embedding innovation
- how we can empower those who draw on support and care, unpaid carers and families
- our strategy for the social care workforce
- how we will make sure the proposals in this white paper are effectively delivered to support our vision
This white paper forms a central component of the government’s vision to ensure that disabled people of all ages, both those with physical and hidden disabilities, have the opportunity to live full and happy lives in their communities. It follows on from the recent publication of our all-age national autism strategy and the National Disability Strategy, which set out specific actions to level up support for disabled people and autistic people across the country.
This white paper also precedes the forthcoming publication of a standalone strategy focused on those living with dementia and their carers.
Our 10-year vision for adult social care
People are at the heart of our vision for adult social care. No matter where they live, their age, race, culture, religious beliefs, sex, sexual orientation, gender identity, disability, housing status or their personal circumstances. This white paper therefore focuses on people and outcomes, not just the systems behind them.
The government is committed to reforming adult social care across the whole of England, and our 10-year vision sets out our long-term aspirations for how people will experience care and support. This has a particular focus on 3 key objectives:
- How we will support people to have choice, control and independence.
- How we will provide an outstanding quality of care.
- How we will ensure that care is provided in a way that is fair and accessible to everyone who needs it.
This vision has been co-developed with the sector. We have engaged directly with people who draw on care and support and unpaid carers, and it has been shaped by what they have told us they need to enable them to live the fulfilling lives that they choose.
The starting point for our vision is embedding personalised care, which is vital to providing the user-led social care we envisage. It has been proven to improve outcomes and enhance quality of life, enabling people to take the level of control and responsibility that they feel comfortable with. Fundamentally, it recognises a person as an individual with specific needs, wishes and aims. It is our ambition to make personalisation the expected standard and for high-quality personalised care to be the norm across health and care. Our 10-year vision describes how this will look and feel for people who draw on care and support, and the steps we will take to achieve this.
People have choice, control, and support to live independent lives
People who draw on care and support have told us that the core purpose of adult social care should be to help them to maintain or gain their independence, allowing them to have control over their lives. Rather than focusing on approaches to delivering care that intervene at a time of crisis, care and support services should intervene early to support individuals, helping people retain or regain their skills and confidence, and prevent needs from developing. When care supports people’s independence, it allows them to have real choice and control over the things that matter, enabling them to live healthier, happier and more fulfilling lives in the place that they choose.
In parts of the country where communities, the voluntary sector, local authorities and providers are working together with people who draw on care and support to develop new, collaborative approaches to delivering care, we can see this vision already coming to life. By investing in preventative services, increasing the care and support options available, and providing the right information and advice to allow people to plan for the future, we can enable people to remain in their own homes and communities for longer, and achieve the outcomes that matter to them.
We must embed this best practice across the country so everyone can reap the benefits. These methods also have the potential to deliver improvements in service delivery and greater efficiency in the future.
We want greater choice, control and independence to mean that someone who draws on care and support can say:
I can live as part of a community, where I am connected to the people who are important to me, including friends and family, and I have the opportunity to meet people who share my interests.
I lead a fulfilling life with access to support, aids and adaptations to maintain and enhance my wellbeing.
I am valued for the contribution I make to my community and feel supported to achieve my goals.
I can live in my own home, with the necessary adaptations, technology, and personal support as designed by me, to enable me to be as independent as possible.
I have a good choice of alternative housing and support options, so I am able to choose where I live and who I live with, with the opportunities to plan ahead and take up those options in a timely fashion.
I have control over my care and support, including what services I receive and how, when and where my care is provided, with access to the necessary information and advice to help me make these decisions and plan for the future.
Choice, control, and independence are not limited to those who draw on care and support. We know that families and unpaid carers must be supported. Therefore, we want unpaid carers to be able to say:
I am supported to provide care as I wish and do so in a way that takes into account my own access to education, employment, health and wellbeing.
I have a life outside of caring and I am able to remain connected to the people who matter to me.
I know my needs are equally recognised and my goals and aspirations are respected and fulfilled.
I have the right information and advice to be able to make informed decisions.
I have access to appropriate support, that suits my needs including respite care and carers breaks.
To ensure everyone is provided with greater choice, control and independence, the government, the NHS, local authorities, care providers, voluntary and community groups, and the wider sector will work together to:
- ensure people can adapt their homes and access practical tools and technology, to live independently and live well in their own home
- make sure that people can access a range of personalised support that reflects their own choices and circumstances – including finding new approaches to improve on the ways we have traditionally delivered care and support
- ensure that the opportunity to receive help as a direct payment is understood, with encouragement and support to be able to use it flexibly and innovatively to provide the greatest benefits for each individual
- help people to achieve the outcomes that matter to them, by promoting wellbeing and supporting equitable participation in work, community and other activities.
- ensure care and support decisions are co-designed with people and their unpaid carers, working with them as equal partners, and combining respective knowledge and experience to support joint decision-making
- champion early health and wellbeing interventions through community support to delay and prevent care needs and reduce the number of people with preventable diseases
Choice, control and independence in action: Charlotte’s story
Charlotte (changed name) is 46 and lives at Hill House in Cheshire. Following a stroke, Charlotte has limited mobility and often finds it difficult to make herself understood. Leonard Cheshire’s Assistive Technology team has been working with Charlotte to identify the best new innovative technologies to help her communicate.
Charlotte has been given an iPad, which has been a revelation. A special mount, which sits on the floor of Charlotte’s room, enables her to use the device from her wheelchair using a specially crafted stylus. Through a series of taps, Charlotte can type words, navigate social media websites and read dozens of electronic books in the Kindle app.
Charlotte is also involved in pilot-testing a technology that teaches Amazon Alexa to recognise her speech so that she can control lamps, technology and a tabletop fan with either her voice or the app’s touch interface.
Charlotte can maintain a close relationship with her family by video-calling her children and parents without needing to wait for a staff member to be available to facilitate the dialling or hold the phone for her. These communication devices have given Charlotte access to, and control over, her environment, which she hasn’t had in years.
Leonard Cheshire is in the second year of a 3-year assistive technology project introducing residents and staff to technologies that are transforming their day-to-day lives – leading to increased confidence, greater control over their space and time, and wider social inclusion.
People can access outstanding quality and tailored care and support
While safety, protection from abuse and neglect, and delivering the appropriate standards of care are vitally important, services must go beyond these basic requirements and promote an individual’s wider wellbeing. Therefore, care and support should be bespoke to individuals, building on their strengths and enabling them to achieve the outcomes that matter to them.
We believe an outstanding quality of care should be of a standard that anyone would be happy for their own child, partner, close friend, parent, grandparent or other family member to receive – no matter where you live in the country. Health and care professionals should work together with people who draw on care and support, and their families, to achieve this aim.
We want outstanding quality and personalised support to mean that someone who draws on care and support can say:
I receive care and support that is safe, responsive to my needs and respects my rights.
I receive personalised and inclusive support, where the people who care for me know me as an individual, and recognise me as having unique strengths and aspirations, and know that my background, values and requirements are unique to me.
I am supported by a workforce who have the right training, qualifications and values, and are concerned about what matters to me.
I receive care from a workforce whose careers are valued and whose professional development and wellbeing are prioritised.
I experience a seamless care journey, where health and care services are joined up around me and I only have to tell my story once.
I receive care and support that is co-ordinated, and everyone works well together and with me to plan my care, bringing together services to achieve the outcomes that are important to me.
I know that, if I want, I can receive help as a direct payment instead of having care services organised for me, and that I will be encouraged and supported to use my direct payment in whatever way will best suit my own needs and achieve my outcomes.
I can make the last stage of my life as good as possible because everyone works together confidently, honestly and consistently to help me and the people who are important to me, including those who care for me.
The care and support workforce are central to achieving this vision. Our ambition is that we create a qualified and valued workforce that works together, with people who draw on care and support and with other organisations, including the NHS, to deliver outstanding quality care that is sensitive to individual needs. We therefore want someone who works in adult social care to be able to say:
Social care is a rewarding career with clear opportunities to develop and progress and where I feel valued in my role.
I feel recognised for the important role I play in helping people who draw on care and support receive high-quality, personalised support that enriches their lives.
I feel recognised for my existing skills, and am able to develop new skills and take on new challenges as I become more experienced.
There is a culture in my workplace that supports my health and wellbeing.
I have the confidence to use technology that supports people’s needs and frees up time to deliver outstanding care.
I am able to work effectively with professionals from other organisations including the NHS, housing and community services, learning from each other’s practice and supporting each other to achieve shared goals.
To enable people who draw on care and support to receive outstanding quality care, government, local authorities, care providers and the wider sector will aim to make sure:
- safeguarding and appropriate standards of support are enforced to protect everyone receiving and providing social care
- assurance is strengthened to drive up standards of care, making brilliant outcomes easier to identify and share and address areas where improvements can be made
- there is high-quality and timely data available nationally, regionally and locally to help identify best practice and address areas of improvement
- technology is fully utilised to enable proactive and preventative care, and to support people’s independence
- social care is recognised by the public as a valuable and high-quality service on par with the NHS
- social care is provided by a qualified, professionalised and valued workforce, which has a low turnover to ensure continuity of care
- all professionals involved in providing care have access to the right digitised information at their fingertips to provide safe, outstanding quality care
- health, social care and other services – such as housing, homelessness and community support – are joined-up to provide a seamless care experience of person-led support, which also recognises and supports unpaid carers
Outstanding quality and tailored support in action: Will and Jakob’s story
Will, 70, is in hospital with a hip fracture following a recent fall. Will also has depression.
After hospital treatment for his fracture, the medical team refer Will to a social worker who is named as the single responsible person who will co-ordinate his care going forward.
At home, Will is supported by his husband Jakob. Together, Will, Jakob and his social worker complete a needs assessment for Will and a carers assessment for Jakob, and together they agree on the additional support that will help when Will returns home from hospital. Will’s social worker ensures the community reablement team arrange for Will to be visited by a carer and a physiotherapist, to help him regain his independence. Will’s physiotherapist suggests that Will attends free swimming sessions at his local leisure centre to build up strength in his joints. This also reconnects Will to his community and reduces his feelings of depression.
The social worker also arranges for an occupational therapist and housing officer to visit Will and Jakob, and together they are able to provide home adaptations such as installing a handrail for the stairs, a bath lift and a telecare system. This consists of fall sensors that alert a professionally staffed monitoring centre if they sense a sudden downward movement or a lack of movement for a long period of time. The home adaptations reduce the risk of Will having future falls that may require emergency hospital admission while supporting him to stay living at home. The sensors also provide Jakob with peace of mind that if he goes out and Will does fall over, the centre will be alerted and he will be able to get help.
By bringing health, housing, community and social care services together in an integrated way, Will is provided with outstanding personalised support that treats him as an individual and ensures he gets the support and care he needs at the right place and at the right time, supporting both him and Jakob to live more independent, healthy and happy lives.
People find adult social care fair and accessible
Care and support should be accessible. Everyone – whether that be people who already, or may need to, draw on care and support, their families or unpaid carers – should be able to access the right information and advice at the right time to understand the different options available to them that best meet their preferences and circumstances, including options for where care and support would best be delivered and costs they may need to meet. This will help people to plan for the future, make well-informed choices about their care and support, and ensure their needs are met without delay.
We want to create a fairer system of adult social care, where:
- people contribute towards the costs of care if they are able to
- there is a more generous safety net for those who are unable to pay
- people who self-fund their care do not have to pay more than local authorities for the same service
We want to ensure the public understands the need to contribute to the costs of their care so that they can plan for it, but no one should be required to pay unpredictable and unlimited care costs.
We want fair and accessible adult social care to mean that someone who draws on care and support can say:
I receive affordable care, and do not have to face unpredictable and unlimited care costs.
I will have access to the same fee rates for care in care homes that local authorities pay.
I know where to find user-friendly information and advice that is inclusive of my communication and accessibility needs so I can make informed and empowered decisions about my life – now and in the future.
I know what my rights are and can get information and advice on all the options for my health, care and housing.
I have accessible care and support to ensure that my needs are met without delay.
We want fair and accessible adult social care to mean that an unpaid carer can say:
I am able to navigate the health and care system with ease.
I understand the support that is available to me in my area to maintain my own health and wellbeing, and achieve the outcomes that matter to me.
I am provided with the necessary information and advice to make informed decisions about the care I provide.
I am provided with the tailored information and advice I need to support and meet the needs of the person I care for.
To ensure the adult social care system is fair and accessible, the government, with the support of local authorities, care providers and the wider sector, will aim to:
- reform how people in England pay for their care so no one needs to pay more than £86,000 for their personal care costs, alongside more generous means-tested support for anyone with less than £100,000 in chargeable assets
- ensure that self-funders can access the same rates for care costs in care homes that local authorities pay, ending the unfairness where self-funders have to pay more for the same care, while ensuring local authorities move towards paying a fair cost of care to providers
- ensure fees for care are transparent to allow people to make informed decisions
- improve information and advice to make it more user-friendly and accessible, helping people to navigate the care system and understand the options available to them
- provide information and advice that is accurate, up to date and in formats that are tailored to individual needs
Fairness and accessibility in action: Zain and Yara’s story
Zain, 55, cares for his wife, Yara, 52, who has progressive multiple sclerosis. She also receives state-funded domiciliary care.
When Yara first developed a care need, her doctor referred her to a support officer at the local community hub who gave her information on the formal care services available in the local area, such as physiotherapists, and a speech and language therapist. The support officer also gave information to them on the support that would be available to Zain as he cared for Yara. A social worker from the local authority visited Zain and Yara and, following the needs assessment that they completed together, arrangements were made for Yara to receive domiciliary care support.
Yara’s symptoms have increased recently, and the social worker reviewed her needs with her and Zain and provided Yara and Zain with comprehensive, personalised information, including a referral to an occupational therapist to advise on how Zain could safely lift Yara when she requires.
When Zain first started caring for Yara, he sometimes found it stressful and tiring, and felt that he was less able to be a good dad to their teenage son Sami. After his local authority undertook his carer’s assessment, the social worker arranged for Yara to access a respite service over some weekends, so that Zain could take a break and spend quality time with Sami.
Zain and Yara can plan for their future, considering all the options for Yara’s health, care and housing, including being able to compare ratings of providers if Yara were to choose to attend residential care in the future. Zain and Yara are also able to financially plan for the future, having read up on the fee rates and the £86,000 cap on Yara’s lifetime personal care costs.
This vision is ambitious but achievable, and we need to work together to ensure it becomes a reality. To achieve it, we need to re-imagine how we do things. Where there are already examples of innovative approaches to providing care and support, we need to build on this, rolling out and adopting these approaches systematically at scale.
It will require change from national government, local government, care providers, housing providers, health and social care professionals, the care workforce, and other partners. We will work together with the full diversity of the sector on this mission. The type of changes we want to see will not happen overnight, but the proposals set out in this white paper will accelerate our reform journey over the next 3 years and move us towards achieving our 10-year vision.
Strong foundations to build on
We are not starting from scratch. There is an abundance of good practice, aspiration and legislation that provides strong foundations for our 10-year vision. However, we recognise there are a number of challenges in the current system that affect how people experience care and support.
In this chapter, we summarise some of the key legislative underpinnings for reform, as well as some of the problems in social care that the proposals outlined later will seek to address.
Underpinning legislation
The origins of our reforms can be traced back to the Mental Capacity Act 2005, the Health and Social Care Act 2008, the Health and Social Care Act 2012, the Care Act 2014, and more recently the Health and Care Bill currently going through Parliament.
In addition, the Mental Health Act 1983 – for which we have set out plans for reform and have consulted on these in a white paper published in early 2021 – the Children and Families Act 2014 and the Autism Act 2009 form the wider legislative framework and context for social care reform. There will be links between these and the proposed social care reforms.
Local authorities are accountable to their local populations in how they deliver their statutory duties under the Care Act and are best placed to understand the care needs of their local populations. Stakeholders have told us that the Care Act was, and still is, an ambitious piece of legislation that should serve as the foundation for social care reform and our long-term vision.
Overview of Care Act 2014
The Care Act 2014:
- places a duty on local authorities to promote an individual’s wellbeing, including unpaid carers, when making decisions
- embeds an individuals’ right to choice, placing focus on their needs and what they want to achieve, and a legal right to a care and support plan
- places a duty on local authorities to provide or arrange services to keep people well and independent, and help prevent people developing needs for care and support, and delay people deteriorating such that they would need ongoing care and support arising from a physical disability, mental impairment or mental illness
- places a duty on local authorities to ensure that their local care market is healthy and diverse
- introduced a duty on local authorities to assess unpaid carer’s needs for support
We acknowledge that the full spirit of the Care Act is not currently being met.
Reforms in the Health and Care Bill and others described later in this white paper will seek to rectify this, to ensure that local authorities and providers are able to develop new, innovative and collaborative approaches across the social care landscape. Subject to successful passage of the bill, the health and care system will be much better equipped to collaborate, make joint decisions and form alliances to tackle shared problems.
Of course, legislation is only part of the solution, and so it is right that we also focus on moving to a system that invests in our health and wellbeing when we are well, and supports us when we need it. That is why, in addition to this white paper, we will also be publishing our white paper on integration in due course.
Opportunities for improvement
Social care faces some well-documented challenges, and we know there are improvements that need to be made to how people experience care and support before our vision becomes a reality. Our conversations with stakeholders have identified a number of interdependent issues. Below provides a brief overview of some of these problems, but we recognise the challenges in social care are not limited to these, and many people will have different views on what the issues and causes are.
Rising to the challenge of increased demand
We rightly celebrate the advances in health and social care that enable people to live longer and fuller lives. Between 2018 and 2040, the number of adults aged 85 and over is projected to increase by a further 77% (from 1.4 million to 2.4 million).[footnote 6] Among younger age groups too, we are seeing continuing progress in terms of better diagnosis, longer life expectancies and higher rates of survival of premature babies. We must therefore plan ahead to ensure that people’s needs are met both now and in the future.
Amid rising demand for social care and a suite of competing responsibilities, councils have sought to protect social care spending, but it has inevitably taken some of the strain. The significant and growing demand for care inevitably puts pressure on carers, families and communities who also play an essential role.
In the following chapters, we explore the approaches for keeping pace with this growth in demand. For example, through investment in preventative activities, where evidence shows that 40% of dementias are preventable through action across the life course[footnote 7], and by securing an adequate supply of supported housing that is appropriate to people’s needs.
Shaping healthy and diverse social care markets
High-quality, personalised care and support can only be achieved where there is a vibrant, responsive market of service providers. It is the responsibility of local authorities to ensure their local care market is healthy and diverse. However, there is variability in the culture and strategic leadership across different localities, which impacts the quality and choice of services available for people.
In many local authorities, we see low fee rates and cross-subsidy between care home residents paying for themselves, and those who are funded by their local authority.[footnote 8] Uncertainty over future funding stifles provider investment and, along with low fee rates, can result in poor workforce conditions, inadequate quality care, market fragility and pose a threat to continuity of care.
Collectively, we are not sufficiently encouraging new innovative, community-based organisations that have the potential to give people greater choice, independence and wellbeing. Market shaping should be managed in an orderly way that does not cause disruption to those receiving care.
Support for sustainable care markets, including moving towards paying providers a fair rate for care, are outlined in supporting local authorities to deliver social care reform and our vision.
Addressing variation in quality and safety of care
Currently, the primary mechanism for monitoring quality is the Care Quality Commission’s (CQC’s) assessment regime of care services, which looks at 5 key questions, including safety, leadership and whether services are responsive to peoples’ needs.
As of November 2021, 84% of all social care settings were rated ‘good’ or ‘outstanding’. However, 14.3% of providers have a ‘requires improvement’ rating and a further 1.4% are rated as inadequate.[footnote 9] There is also stark geographic variation, with evidence of poorer quality care in less prosperous areas where local authorities often pay lower rates for care and self-funders are less affluent. Several local authorities have 100% of social care services rated ‘good’ or ‘outstanding’, while the worst has around 65%. The government is committed to levelling up the country and addressing this geographical inequality so that everyone, everywhere receives outstanding quality and tailored care.
Improving the quality of social care can directly improve individuals’ quality of life. Proposals outlined throughout this white paper will seek to raise quality, especially our workforce strategy, and the proposals on enhanced local authority assurance, improvement support and data in the chapter on supporting local authorities to deliver social care reform and our vision.
Supporting our adult social care workforce
The social care workforce is our biggest asset – in 2020 to 2021, there were an estimated 1.56 million jobs with adult social care employers, with a further 110,000 NHS jobs providing adult social care.[footnote 10] Those who draw on care and support particularly value continuity of care and want to get to know their carers, so their needs are well understood. However, the social care workforce suffers from very high levels of staff turnover (overall annual staff turnover rate in 2020 to 2021 was 30%), particularly among frontline care workers and nurses. Vacancies rates are also persistently high, particularly for regulated professional roles such as nurses, social workers and registered managers.[footnote 10]
Much of the workforce suffers from poor mental health and burnout, especially following the huge sacrifices they made during the COVID-19 pandemic. 26% of care home workers were likely to be experiencing some form of depression at the start of this year, and 27% likely experiencing an anxiety disorder (compared with 20% and 18% at the national average).[footnote 11]
Finally, large parts of the workforce are unregistered and undertrained with no clear career structure or learning offer. This is a missed opportunity[footnote 12] and our workforce strategy explains how, by improving the skills offer, we hope to make social care a more rewarding career with attractive progression opportunities.
Navigating the system, and finding the right care and support
Individuals have told us that they find it hard to understand what they are entitled to or how to access care and support. The majority of people think the NHS provides social care services, while just under half (47%) wrongly think social care is free at the point of need.[footnote 13] A recent Social Care Institute for Excellence (SCIE) survey found greater awareness of some social care settings than others, with 98% of over-65s aware of care homes compared with 66% aware of extra-care housing, 40% of shared lives housing and 56% of supported living.
People often do not know where to start when looking for information and advice, while others find that the volume of information available is overwhelming and poorly tailored to their own circumstances. A lack of knowledge and understanding can result in people drawing on the wrong type or amount of support, which may impact on their wellbeing as well as put further pressure on unpaid carers, affecting their health, wellbeing and employment.
We will set out how we want to empower people who draw on care and support, their carers and their families so they can make informed decisions based on accessible, trusted, and high-quality information and advice.
Accelerating adoption of technology
During the COVID-19 pandemic, the use of digital technologies transformed the delivery of care and helped people stay connected with friends and family. These digital tools supported people’s care through remote monitoring, ensured care teams had the right information at their fingertips and helped services to identify those in need. Looking ahead, in a recent survey, 90% of care providers said they will continue to use technology as they have during the pandemic.[footnote 14]
Although technology has been a lifeline for millions of people, it has also laid bare inequalities in access. Recent research by Age UK highlighted that the older population are still less likely to be digitally included – among those aged 75+, more than 40% do not use the internet. Office for National Statistics data shows that 14.9% people with a disability have never used the internet, compared with 6.3% of the UK population.
Recent research showed that 23% of care home staff cannot access the internet consistently at work. In addition, 45% of providers express concern that care staff lacked digital skills.[footnote 14]
Providing the right care in the right place at the right time sets out a range of measures to accelerate digitisation and adoption of technology across social care.
Expanding the choice of housing options
Today, too many people with care and support needs live in homes that do not provide a safe or stable environment within which care and support can be effective – whether for older people or those of working age with a physical or learning disability, for autistic people, or for those with long-term mental health conditions.
Some people’s care and support needs mean that specialised housing is likely to offer the best option for them. Projected demand for supported housing in England is estimated to increase by 125,000 by 2030, and we therefore want to provide more people with this option. However, we recognise that most people will continue to live in mainstream housing, and we need to ensure they can adapt their homes to meet their needs where necessary.
In fact, around 1.9 million households in England are home to someone with a health condition that requires an adaptation to their home to support everyday tasks like washing and using the bathroom, cooking, or getting out and about easily. In 2019 to 2020, 53% of households requiring an adaption do not have all the adaptations needed, a rise from 45% in 2014 to 2015.[footnote 15]
The actions set out in providing the right care in the right place at the right time describe how we will support local communities to:
- build the partnerships and plans to embed housing as part of the local health and care system
- boost the availability of specialised housing
- make it easier for everyone to adapt their home to enable them to live independently and safely
Driving integration of health and care services
The health and care system too often treats discrete episodes of mental or physical illness rather than considering a person’s care needs holistically. This means that opportunities for prevention are missed and people may go into hospital when they could be better cared for at home, causing people to lose their independence and choice.
A lack of join-up between services leads to problems, including:
- confusion in accessing care and unco-ordinated care: multiple visits may have to be made to see different professionals, resulting in people having to tell their story multiple times
- discontinuity of care and disjointed transitions between care settings – from childhood to adulthood, from NHS to social care or from GP to hospital
- worse outcomes: individuals have a worse experience of care and their conditions escalate until requiring emergency admission.
- a lack of consistency identifying unpaid carers across health and care, and providing them with the right information and support for caring
The upcoming integration white paper will outline proposals to improve person-centred care and improve the interface between health and care services.
Providing the right care in the right place at the right time
We want people to be able to say…
I can live as part of a community, where I am connected to the people who are important to me, including friends and family and I have the opportunity to meet people who share my interests.
I lead a fulfilling life with access to support, aids and adaptations to maintain and enhance my wellbeing.
I can live in my own home, with the necessary adaptations, technology, and personal support as designed by me, to enable me to be as independent as possible.
I have a good choice of alternative housing and support options, so I am able to choose where I live and who I live with, with the opportunities to plan ahead, and take up those options in a timely fashion.
For everyone who draws on care and support – no matter their age or circumstances – achieving the choice, control and independence set out in our 10-year vision starts with making sure they are listened to, understood, and get the right care in the right place and at the right time.
Wherever possible, that care and support should be in a person’s own home and personalised in line with their specific needs, although recognising that not everyone has a home of their own, and sometimes specific needs are best met in a supported living or care home setting.
People of all ages are clear about what matters most to them when it comes to care and support. A recent survey by SCIE asked: “Which of these things would be most important to you if you need or needed care or support?” and the top 3 priorities were:
- Remaining independent.
- Having access to the internet, phone and technology.
- Being able to stay in my current or own home.
Care and support needs are dynamic, so we should not only be trying to meet a person’s needs in the here and now, but also planning for changing needs. Supporting people to plan for the future – for themselves and their loved ones – includes preventing and reducing future care needs. When the basic layout of a home, its contents, and technology are all considered as a complete package, these can make a real difference to the daily lives of people who draw on care and support, their carers, and their families.
In this chapter, we set out how we plan to support the provision of outstanding quality care and move towards the choice, control and independence that people want by:
- making every decision about care a decision about housing. We want people, wherever they live, to have choice over their housing arrangements – whether that is a new home or their existing home, purpose-designed or not, and with access to the adaptations or technologies to help them live well. We also want to ensure local areas ‘think housing and community’ when they plan and deliver services
- using the full potential of technology to support people’s lives and aspirations. This means:
- putting practical digital tools in the homes and the hands of those who draw on care and support and their carers
- equipping the social care workforce with the digital tools, knowledge and confidence they need to deliver outstanding quality care
- creating the digital and data infrastructure needed to drive future transformation in care delivery
- building a system that can develop and adopt new ways of providing care and support to people at scale. This means ensuring that local areas have the ambition, culture and capability to embed innovation, as well as the provider market being well equipped to help deliver this change. We want to create the conditions for new ideas to flourish so that we can deliver care in the way that people want
- focusing on prevention and health promotion to support people to live healthier lives for longer. We want people to live healthy, independent lives. Prevention in social care is about encouraging people to be more proactive about their health and wellbeing. We must make prevention and early intervention a much stronger element of our model of support and of care pathways as part of a decisive focus towards improving population health
Overview of main proposals
We will:
- invest at least £300 million over the next 3 years to embed the strategic commitment in all local places to connect housing with health and care, and drive the stock of new supported housing
- invest at least £150 million of additional funding over the next 3 years to drive digitisation across the sector, and unlock the potential of caretech innovation that enables preventative care and independent living.
- launch a £30 million Innovative Models of Care Programme to support local systems to build the culture and capability to embed into the mainstream innovative models of care. This will work for a changing population, with more options for people that suit their needs and circumstances
- fund a new service to make minor repairs and changes in people’s homes, to help people remain independent and safe. This will happen alongside increasing the upper limit of the Disabled Facilities Grant
- continue to invest in the Care and Support Specialised Housing Fund with £210 million available for the period 2022 to 2023 through to 2024 to 2025
Making every decision about care a decision about housing
Ensuring that people receive the right care and support all begins with where they live, and the people they live with. For people of working age with a physical disability, a learning disability, autistic people, those with mental health conditions or substance misuse needs or those experiencing homelessness, a suitable home enables them to build and sustain their independence, connect with their community and achieve their ambitions. For older people, having a home that sustains safe, independent living can help prevent ill-health, reduce the amount of care and support they need, and delay or avoid altogether the need for residential care.
However, at present, there are too many people with care and support needs living in homes that are not enabling them to live well or safely. Many homes are poorly designed for accommodating changing care and support needs or older age, and there are some people who do not have a home to call their own. People who are thinking about the future for themselves – or for their loved ones – often do not feel like they have options. A lack of suitable housing options results in too many people staying in hospital unnecessarily or moving to residential care prematurely, even if that is not what they want, instead of recovering at their own home.
Our ambition is to give more people the choice to live independently and healthily in their own homes for longer. This means adults of all ages being able to access or remain in the home of their choice – whether that be their home of today or one they might move into – which forms part of a community they have chosen to call home. Existing planning flexibilities enable householders to extend their property without the need to submit a planning application, which can help to accommodate families. We want people to be able to draw on care and support centred around the person at home, optimal to their needs. Living healthier lives for longer can mean lower cost to people and their families. Optimal provision of care and support can mean lower costs to the system too.
To realise the ambition, we set out we need to ensure that “every decision about care is also a decision about housing”.[footnote 16] We first need to embed a series of enablers:
-
Strong leadership and partnerships: no organisation can deliver this change alone. Change requires collaboration across commissioners and providers of health, adult social care and housing, and homelessness support services, as well as local planning functions and voluntary organisations. Underpinning them all is the need for strategic leadership that sees the local provision of health, care and housing services not as separate systems, but as a coherent system that seeks to deliver the best outcomes for people, using all the tools available in a joined-up way to deliver the best possible outcomes for their communities.
-
Long-term funding certainty: housing providers need to take decisions on where and when to invest that look decades into the future, confident that people will be supported to live in those homes for many years to come.
-
Wider influence: housing that better meets future care and support needs must be delivered within a complex wider housing market. For changes to be embedded we need to influence beyond the adult social care system.
We also need to actively shape the specialist housing market – to establish and consolidate local strategic leadership, and create the right incentives for local areas and housing providers to invest, including in new and innovative models of provision. We will therefore invest at least £300 million for the period 2022 to 2023 through to 2025 to 2026. This new investment will allow local authorities to deliver the vision set out in this white paper by integrating housing into local health and care strategies, with a focus on boosting the supply of specialist housing and funding improved services for residents. This in turn will drive increased confidence in the social supported housing market, stimulating a positive cycle of further innovation and private investment.
To achieve this, there will be a critical role for integrated care partnerships (ICPs) in driving the necessary integration of housing within health and care, both through the development of local strategies and in the delivery of services. The upcoming integration white paper will set out more detail of how we will support local places, working with ICPs and integrated care boards (ICBs) to deliver effective joined-up care.
With this context, our intention is that, over the 3-year period, the new investment will:
- enable all local areas to agree a plan embedding housing in broader health and care strategies, including investing in jointly commissioned services
- boost the supply of supported housing, coupled with driving innovation in how services are delivered alongside housing where possible
- increase local expenditure on services for those in supported housing
Increasing the supply of supported housing
For some of us, the nature of our care and support needs will mean we need a home that is specifically designed to support independent, healthy living. These homes are generally known as supported housing. There is evidence that for both working age adults and older adults, supported housing can be the best model of care to provide better health and greater independence, as well as closer connection with our friends, family and community. In addition, supported housing can be better value than institutional care (such as residential care) which is often more intensive, and so there is the potential to reduce costs to the health and social care system.
As far back as 2015, which saw the publication of NHS England’s Building the right support national plan, supported housing was identified as an important way to improve outcomes for autistic people and people with a learning disability, and prevent people from ending up in inpatient mental health settings. Yet the fact is we do not have enough supported housing to keep pace with demand, and we are not building enough to close that gap.[footnote 17]
The UK has a far smaller proportion of people living in these types of accommodation, compared with other countries – around 0.6% compared with around 6% in the United States, 5.5% in New Zealand and 5% in Australia.[footnote 18] An important priority for the government in achieving our 10-year vision is therefore to grow investment in both grant-funded and private supported housing to incentivise their supply.
Across the country, we see some exciting high-quality new housing developments, some of which are among the best examples from around the world. These:
- incorporate fresh thinking about technology and connectivity
- place residents at the heart of the community through models such as intergenerational living or housing-with-care
- blend housing with other services on site (including residential care) so that care and support can flex according to users’ changing needs
While we want to grow supply, we also want to encourage and support innovation that helps more people access this model of care.
Therefore, we will continue to invest in the Care and Support Specialised Housing (CASSH) Fund, with £70 million per year capital funding available per year between 2022 to 2023 and 2025 to 2026, to incentivise the supply of specialised housing for older people and people with a physical disability, learning disability, autism or mental ill-health. This is in addition to the Department for Levelling Up, Housing and Communities’ Affordable Homes Programme (AHP) 2021 to 2026, which will continue to support the delivery of support housing. We will work with Homes England and the Greater London Authority to ensure that CASSH is well targeted, and is easy for applicants to access and navigate.
Alongside this continued investment in existing funds, the new investment in housing will drive an increase in the availability of supported housing by providing funding to local areas to modernise and improve existing housing units, and to support the people living in them. Improvements in the quality and availability of appropriate housing, alongside integrated care and support services wherever possible, will generate confidence in the model, prompting future investment and increasing demand for the capital subsidies provided by CASSH and AHP.
We will also work with Homes England, the Greater London Authority, and the Regulator for Social Housing to understand the barriers to accessing capital grants to increase the supply of supported housing, and ensure value for money is provided for both self-funders and welfare spend.
Supported living in action: Joni’s story
Joni has learning disabilities, epilepsy and communicates through sign language.
Until the age of 17, she lived in the family home, her parents providing round-the-clock care and support to help her with everyday living. As her needs grew, her parents could no longer give Joni the support she needed and made the decision to get help from the local authority.
Joni moved to a long-stay hospital. Living here, Joni shared with 7 other people and found it quite depressing and not very homely, as it was very bare without any pictures on the wall. The building was in poor condition and the surrounding grounds were not maintained.
Over time, Joni’s behaviour changed, she didn’t get on with anyone and she became quite challenging – it was her way of communicating she was unhappy. Joni lived at the hospital for over 10 years. However, following an abuse scandal at a local hospital, several mental health hospitals closed in Cornwall and she was supported to move into her own home with 24/7 support.
Joni’s new home better meets her needs as it is situated within a quiet setting in large grounds within a residential area of Liskeard, which is close to her family.
Joni’s life has been transformed since moving into supported living. As a result of the move, Joni’s support needs are now better met. Due to her very complex needs, she has 3:1 staff support during the day along with 2 sleep-in staff at night as well as a waking night. Joni has a good relationship with the staff team.
She now has vagus nerve stimulation to help with her epilepsy and associated feelings, which has reduced her challenging behaviour.
Joni has more choice about how she leads her life than in her previous accommodation, and she now has access to the community and activities. Consequently, moving to specialised supported housing has improved her quality of life.
Helping people to ensure their current homes meet their needs
Nine out of 10 people aged over 65 live in mainstream housing that is not specialised for people with care and support needs. We recognise that, although we want to provide more specialised homes, most people who draw on some form of care and support will continue to live in mainstream housing.
Stairlifts, wet rooms, grabrails and other adaptations can enable people to lead independent lives, reducing the amount of formal care and support they need, and even making the difference between being able to continue living in their current home or not.
We want more people to benefit from home adaptations to meet their needs, and therefore we will commit a further £570 million per year (between 2022 to 2023 and 2024 to 2025) to provide funding to local areas to deliver the Disabled Facilities Grant (DFG). Through this long-standing and proven programme, around 50,000 people each year get financial and practical help to adapt their homes. The government is publishing updated DFG guidance to advise local authorities in England how they can effectively and efficiently deliver DFGs to best serve the needs of local older and disabled people.
We are doing more than continuing that funding. Following the findings of a government-commissioned review into the DFG in 2018, we are taking steps to ensure that the grant can reach more people who will benefit from it. We:
- are increasing the amount that the grant can pay for an individual adaptation. This will mean that more people who need the grant across the country will be able to access it. We will publicly consult on this change in 2022
- will look at the way DFG funding is allocated to local authorities. This will help ensure better alignment with local demand so that more adaptations reach those who need them most. The government will consult on a new approach in 2022
- are also funding a new service to make minor repairs and changes in peoples’ homes. These small repairs and changes in peoples’ homes can help them stay safe and independent, and reduce demand for more substantial adaptations through the DFG
- recognise that the means test underpinning the DFG is complex and can be difficult to navigate. We will therefore be considering how best to align the means test with the charging reforms. We will publicly consult on this change in 2022
To make sure that people can quickly access the adaptations they need in a way that is co-ordinated with other practical support they receive, local co-ordination and collaboration is essential. The DFG Fund is delivered by local places through the Better Care Fund, which means local areas should be taking advantage of these opportunities for coordination and collaboration.
Currently, the majority of adaptations funded by the DFG are for showers, wet rooms and stairlifts – adaptations that have been the mainstay of its 30-year history. But there are now many affordable technologies that can help make someone’s home environment easier to use, such as smart devices, personal alarm systems and sensor technologies. Although DFG grants can already be used to fund these technologies, we want to raise awareness among people, their families and those providing care of how assistive technology can support people to live independently. More information on this will be shared in the forthcoming DFG guidance and via other web resources.
We can also do more to ensure that new-build homes are designed to be more accessible in the first place. The Department for Levelling Up, Housing and Communities has consulted on options to raise the accessibility of new homes, recognising the importance of suitable homes for older and disabled people. We are currently considering responses and will publish a government response setting out next steps in due course.
Looking to the future
The work described above represents the next important steps towards our 10-year vision for transforming the role that housing plays in adult social care. By the end of the 3-year spending review period, we will have achieved a step change in the ambition. Partnerships and strategic capability will be in place locally, new investment to support more people to live independently will have been made, and we will have stimulated growth of new models of care for people living outside of residential settings.
We know the landscape of housing options for older people is wide and complex. Therefore, in the coming months we will continue to work with partners across government, with local government and the NHS, and across the social care, housing, financial and other sectors to develop our ambitions and practical ideas.
In the first instance, we will explore the following themes:
Supporting providers across the housing sector to develop more options for people in the private housing market
We want to help boost supply across the country and ensure we build a diverse range of specialist housing that matches local need and gives consumers greater choice to find the right housing solution for them.
We will continue to work across government to explore options to support and incentivise market growth, including ways to give developers greater clarity, investors more confidence and provide consumers with the necessary protections.
This will also build on the ‘place-making’ impacts of our new investment as it drives the embedding of holistic strategies across housing delivery, local planning and spatial development.
Support people to take up those options, and plan financially and practically for their older age
For many people, their home represents their main asset, and decisions about downsizing or rightsizing are major financial and personal decisions. As we develop and implement our charging reforms, we will ensure that the new arrangements act as an enabler for people to find and finance the right housing options and tenure models for them.
This will include supporting people to access the information and impartial advice they need to help them plan financially for their future care needs. We will work to understand how people can be supported to access housing options as they plan financially for later life.
Supporting local places to create lifetime neighbourhoods
Initially with the help of our new investment in housing to ensure neighbourhoods are accessible and inclusive and have positive impacts on residents health and wellbeing.
Identify and open up new areas of innovation – in design, financing and local collaborations
The new investment in housing and the Innovative Care Models Programme described below are important steps in building local capability and culture for innovation, and in providing the financial headroom and support to implement local solutions. But we also want to capture the collective value of local innovation across the country at national level, and use the outcomes and evidence to inform our future direction.
We want to support the growth of a thriving older peoples’ housing sector that:
- builds enough homes to match growing need
- gives certainty to developers and investors
- empowers consumers with choice from a diverse range of housing options to suit their needs
To achieve this vision, we need to draw on the expertise of the sector to help us find solutions and consider where government can best intervene. That is why we remain committed to working closely with stakeholders from across both private and social sectors to inform future cross-government action that will help stimulate a specialist housing market that delivers effectively for both consumers and providers across the country.
Using the full potential of technology to support people’s lives and aspirations
When technology is embedded seamlessly into care and support services, it can be transformative, helping people to live happy, fulfilled lives in their homes and communities. Digital tools can also be used to identify risk, prevent incidents from occurring and ensure quick and appropriate responses to avoidable events such as falls, urinary tract infections, medication errors and bedsores.
At least 1.7 million people in England already use assistive technologies, such as personal alarm systems, to support their care and give them more choice, control and independence.[footnote 19] Many people use smart devices to help them with routine tasks such as medication reminders, while sensor technologies are increasingly used to monitor movement and identify falls at home.
Digital technology is also making the provision of social care more efficient for the workforce. E-rostering solutions can reduce administration demands for care managers. Similarly, digital social care records can improve transfers of care and handovers between shifts by ensuring staff have up-to-date information about people’s health and care needs. They also enable more joined-up, timely and accurate data.
The use of technologies in social care should:
- enhance the quality of care
- free up time for meaningful human interactions
- create stronger connections between people and their friends, family and care networks
We must ensure that technology reduces rather than exacerbates loneliness and isolation, and that it supports the mental health and wellbeing of people and carers. And, while not all people will want to use technology as part of their care or daily life, we must make sure that professionals and care teams have the right digital tools and data to provide the outstanding, safe care that all people deserve.
Through the rich discussions we have had to shape this white paper we have developed a 10-year vision for what a digitally enabled social care system would look like.
People, families and unpaid carers
As people increasingly manage their care through personal budgets, self-fund, and arrange their support with family and carers, it needs to be as easy as possible for people to purchase and use the technology that would best support their goals.
We want them to:
- have confidence in selecting and using the most appropriate digital tools to support their independence, safety, and wellbeing, knowing which technologies meet essential standards
- know their needs, goals and preferences are shaping the design and delivery of digital transformation in health and care
- have access to a comprehensive and up-to-date digital social care record, allowing vital information including end of life preferences to be shared securely, giving confidence that professionals have access to the right information and avoiding people having to repeat their history
- know that, when they are being discharged from hospital to a care setting, appropriate technology will be put in place and accurate information will be available to the team supporting their transition
- routinely use technology to enjoy greater reassurance about their loved one’s safety, through access to real-time information
Adult social care providers and staff
Technologies can complement and enhance the quality of care delivered by the workforce, while digitisation of care records will ensure care staff and multidisciplinary teams have the information they need to provide holistic, person-centred care in any setting.
We want them to:
- fully understand the benefits of digital technology, and have the confidence and capability to drive digitisation in their own organisations, sharing learning and best practice across the sector
- be confident to identify, recommend and use appropriate technology to deliver high-quality care
- work as part of a multidisciplinary team able to communicate and collaborate securely to ensure all professionals have access to the information they need
- take informed steps to protect people’s health and personal information against cyber risks, giving health and care professionals the confidence to appropriately use and share information
Commissioners, integrated care systems (ICSs) and NHS partners
Commissioners to support people in the community and following discharge from hospital by integrating technology into their care and support plans, as well as providing more proactive and preventative care supported by improved availability of data.
We want them to:
- fully understand the benefits of digital technology and have the evidence to target spending to effectively deploy technology that meets people’s needs
- proactively identify areas for improvement and share best practice across the health and care system
- draw on accurate and timely data to inform commissioning, and understand the needs and requirements of their local populations
Industry and innovators
There is a significant opportunity for UK-based innovators to develop the next generation of care technologies to meet the demands of global demographic trends and ageing populations in line with the ambitions set out in the UK Life Sciences Vision.
We want them to:
- develop user-friendly, accessible and interoperable technology by default, supporting a highly integrated and personalised experience of care for everyone
- be at the forefront of global care technology innovation, drawing on the existing strengths of the UK’s life sciences and research sector to develop, deploy and scale care technologies that improve people’s lives and their care outcomes
To make the vision a reality, over the next 3 years, we will invest at least £150 million of new funding to deliver a programme of digital transformation.
Caretech
With this funding to support people to live independently in their own homes for longer, we will launch a new scheme to:
- test ideas
- scale those where there is proven benefit
- build the case for change
With local authorities, the voluntary and community sector, people who draw on care and support and their care networks, we will produce a shared roadmap of priorities. This will build on best practice across the country, including the Social Care Digital Innovation Programme and the Social Care Digital Innovation Accelerator 2020 to 2021 delivered by the Local Government Association.
An early priority is to protect the 20% of most vulnerable residents in care homes with technologies that prevent falls. Half of people over 80 will experience a fall at least once a year, with many experiencing a fracture and requiring hospitalisation. As well as life-altering effects on older people, falls cost the NHS over £2 billion a year. Most falls happen in people’s own homes but many also happen in care homes. The use of technology such as acoustic monitoring could reduce falls by 20% or more and avoid admissions to hospital. These technologies have shown additional benefits including better quality of sleep for care home residents through enabling more proactive and responsive care.
Digital social care records
Digital social care records also dramatically improve care quality and safety, allowing real-time sharing of information about someone’s care. Right now, only 40% of social care providers are fully digitised with the remainder using paper records. Without targeted support, the rate of adoption has been slow at just 3% a year. By March 2024, we will ensure that at least 80% of social care providers have a digitised care record in place that can connect to a shared care record – a commitment that was set out in the draft Data saves lives: reshaping health and social care with data strategy.
To support care providers in adopting proven technologies that can transform quality of care and safety, we will fund implementation support within each integrated care system and invest in the infrastructure and skills required for the future. By rapidly digitising social care, we can ensure a more equal partnership with colleagues in the NHS and achieve wider ambitions for joined-up care around the individual.
Infrastructure and cyber security
To make the most of these technologies, staff need access to fast, reliable and affordable internet connections. We will therefore deliver fibre broadband upgrades to those care homes still dependent on poor connections.
In addition, we will work in partnership with the Department for Digital, Culture, Media and Sport and the telecommunications industry to ensure home care providers have the infrastructure they need to work digitally. We already have work underway to understand the telecare sector’s readiness for the digital switchover, which will switch all analogue phone lines across the country to digital connections by 2025.
As the sector’s integration with NHS systems deepens, good cyber security practices must be in place to safeguard people’s information and their interactions with health and care professionals. Building on the Better Security, Better Care programme, we will continue to broaden our data and cyber security support and drive uptake of the Data Security and Protection toolkit. This sets out minimum cyber security and information governance requirements for all health and care providers.
Digital skills
Our ambitions for a digitally enabled care system cannot be realised without a workforce that is skilled and confident in the use of technology. Building on the findings from the recent digital skills baseline report, we will provide a comprehensive digital learning offer that includes accessible training and online resources to build transferrable digital skills as well as practical guidance on using technology in all care settings.
This will include targeted digital leadership support for decision-makers who can drive cultural change at a senior level.
It will complement the workforce investment outlined in our workforce strategy.
Technology in action: Matthew and Niki’s story
Technology can help unpaid carers to support their loved ones and look after their own wellbeing too.
Niki cares for her husband Matthew. Matthew has mytonic dystrophy, which makes movement hard. Both in their 50s and adept with technology, they use a host of technologies in their home to maintain their independence. Google Broadcast helps them keep in touch: Matthew, who cannot raise his voice, can contact Niki or ask for a cup of tea wherever she is, and Niki can let Matthew know when she’s popping outside. They also have voice-controlled lights and TV, and a Ring Video doorbell.
Niki says:
Tech reduces a whole series of micro-stresses that would otherwise build up over the day into major ones.
Matthew agrees:
Tech enables me to stay in control of my life, to make decisions when and where I want to, and not rely on others as much. There is no doubt that it improves my quality of life and allows me to do much more.
Technology also helps to manage Matthew’s health needs. Remote monitoring now automatically uploads his blood pressure readings:
This is so much easier for us and quicker – we much prefer it. We feel we can be quickly in touch with health professionals if need be.
Thanks to technology, Niki can continue working while she cares for Matthew. She loves her job:
It gives me a sense of self. It means I’m not just Matthew’s carer, but a wife and friend too. Work allows me to talk about and focus on things other than caring.
But I could not do what I do without wifi, remote working and the technology that Matthew and I use to support his care – it gives us both independence. Being connected is no longer a luxury, it’s a necessity.
Separately, as announced in the National Disability Strategy, we are investing up to £1 million in 2021 to 2022 to develop a new Centre for Assistive and Accessible Technology, and we will report progress on this by summer 2022. As part of this work, we will assess the assistive and accessible technology needs of disabled people in England to establish where these are being met and where improvements can and should be made.
Building a system that can develop and adopt new ways of providing care and support to people at scale
The needs of our population are evolving, and supporting more people to live independently outside of residential settings will have important implications for the level and type of support people need. As these needs change, the ways in which we provide care and support will need to change too.
In the future, we need to embed new, diverse and innovative models of care that will provide personalised support that reflects an individual’s own choices. The care system has been innovating for decades, yet there is a tendency for impactful innovations to remain on the margins, rather than becoming the mainstream way of delivering care and support. This must change.
Importantly, this means that local areas must have the capability, culture, and ambition to adopt and scale up new models of care that deliver care in the way local people want.
Embedding innovative models of care
When we talk about innovation, we are talking about it in its broadest sense – specifically, the practices adopted by providers, service users, local authorities or government to implement new models to solve a problem. Innovation can involve technology, as illustrated above, but it can also relate to innovation in policy as well as innovation in delivery, investment and business models or in market-shaping and commissioning practices.
There are great examples of different models that have been implemented to meet people’s needs. For example, shared lives schemes have been scaled up across the country to offer greater flexibility and more community-based care.[footnote 20]
Similarly, to improve outcomes and provide more personalised care, providers and commissioners have looked to the Buurtzorg model, which was founded in 2006 in the Netherlands by a small team of professional nurses. The model integrates health and care services. It involves small, autonomous, neighbourhood-based teams that provide a range of care and support services to people in their homes, building a care and support plan around a ‘self-managing’ client, involving the person’s informal and formal support networks.
Local authorities and providers are also establishing different ways of delivering care to their population.
Innovative models of care in action: Somerset’s alternative commissioning model
In 2014, Somerset Council wanted new ways to meet home care demand and meet the needs of people in rural areas. Pooling council and NHS funds, they raised an initial investment of £75,000 a year, and worked with social enterprise Community Catalysts CIC to launch the micro-provider initiative, which helps people start and run small, independent enterprises offering care and support in their local area.
Following 4 years of initial support from Community Catalysts to set up and embed the Somerset Micro-enterprise programme, it is now managed solely by the council and has developed 867 new micro-providers that provide approximately 6,000 people with over 26,000 hours of support a week.
Micro-providers typically support people with personal care, managing their home, going out, social contact and maintaining their usual routine. Alongside this programme, Somerset County Council also introduced ‘Village Agents’ – trained people employed by the council who offer a range of support including help with securing transport for the rurally isolated, countering loneliness with get-togethers and connecting people with services they need.
These kinds of hyper-local care services have attracted new people into care, created 728 new jobs, and have helped ease pressure on hospitals and social care. Offering people more choice and control over their care has also resulted in a 43.6% increase in people using a direct payment.
This new model has resulted in significant savings – a 2020 survey of 125 micro-providers indicated savings of around £2.9 million a year compared with commissioned home care services. Most importantly, people who use the services of micro-providers are reporting better outcomes. A 2017 survey of people who have used both traditional home care services and micro-providers found that all 45 respondents felt that the support they received from micro-providers was more consistent, reliable and focused around the person.
The greatest endorsement comes from the service users themselves. Jane Williams, a micro-provider service user in Somerset says:
All the micro-providers I have met are professional, charming, intelligent and able. They take on a variety of work, such as bed-making, meal prep and shopping. But what is more important is that they know about empathic listening, which allows you to have your own voice. I had lost my own voice through loneliness, isolation and fear.
I was a counsellor myself in the past, so I know about professional empathic listening – that is the most valuable thing they can offer you. There is nothing like the emotional support of being able to express yourself to someone who is sharing with you the experience that you have… There is nothing to compare with that.
However, we know that the challenges of embedding new and innovative models in a system are significant and, in reality, the job of dealing with the day to day and providing good care now – rather than thinking about how to deliver care in the future – often comes first.
Wider system and structural issues – such as the complex regulatory and legislative system, workforce churn and supply issues, challenging financial circumstances, and conflicting outcomes between different parts of the system – also act as barriers, making innovation and the adoption of new models harder to implement, embed and, importantly, scale.
Embedding innovation takes dedicated leadership and good relationships, it requires consultation, engagement and co-production with people who need support and a workforce that are supported to champion and embrace new ways of working. It also requires national support to help establish the conditions for innovation to thrive.
A new Innovative Models of Care programme
We will invest up to £30 million in a new Innovative Models of Care programme that will address the key barriers to embedding and ‘mainstreaming’ innovation in the sector. There is no ‘one-size-fits-all’ solution – different models will be needed in different places, and local authorities, providers, people who draw on care and support, and their family members will be best placed to develop and choose models that work for them. We will help provide the capability and ambition to innovate so they can continue to improve their local care landscape, increasing diversity and choice.
The programme will provide the vehicle for local areas to come together to trial and embed ambitious new services for addressing key priorities such as:
- prevention
- reablement
- better support for unpaid carers (for example, through respite provision)
- key enablers such as local community capacity-building or outcomes-based commissioning for improved outcomes
The programme will support local authorities and partner providers to develop, commission and deliver new models of care for people living in non-residential settings. We are designing the programme in consultation with the sector to ensure it addresses the key barriers to embedding innovation. As part of the programme, we intend to convene innovation partnerships based on a number of agreed innovative models. These will provide expert support, building local authority and provider capacity, skills and knowledge-sharing into the process.
Alongside this, we will provide risk-sharing funding to a number of local authorities to mitigate the additional costs arising from system change, as well as business development support to care providers to build capacity in the sector. All of this will be underpinned by evaluation, so that we can scale and embed successful models across the sector, and learn ‘what works’ to help local systems to implement successful innovations.
Focusing on prevention and health promotion to support people to live healthier lives for longer
We recognise there is more to be done on preventing the causes of ill health that can increase the demand for adult social care services.
The newly formed Office for Health Improvement and Disparities (OHID) gives increased focus on improving the health of the population, working across government departments to co-ordinate efforts and impact.
OHID will focus the whole health family on delivering greater action on prevention and – working with a new cross-government ministerial board on prevention – drive and support the whole of government to go further in improving health and tackling health disparities, addressing the wider drivers of good health, from employment to housing and education to the environment.
OHID will tackle the top preventable risk factors for poor health, including obesity, smoking and alcohol.
Improving quality of life in the last 5 years of life will enable older people to do what they have reason to value, for example, work, caring or volunteering, as recommended by the World Health Organization in its UN Decade of Healthy Ageing strategy.
Maximising independence of older adults to reduce falls risk
Levels of physical activity have fallen as a result of the coronavirus (COVID-19) pandemic and the mitigation measures put in place to reduce levels of disease transmission. There has been a particularly large fall in strength and balance activity among older adults over 65, which has led to an increase in deconditioning.
Deconditioning is a change in physical fitness due to inactivity – including the loss of physical, psychological and functional capacity due to inactivity. It can occur rapidly in older adults and is not straightforward or quick to remedy. It has a range of negative health impacts, including falls, depression, type II diabetes, cardiovascular disease and musculoskeletal problems.
The most immediate outcome of deconditioning is likely to manifest as an increase in falls. Government modelling of the expected increase in falls resulting from deconditioning puts the number of additional falls at over 250,000 a year, leading to costs to the health and social care system of £210 million. Based on the usual healthcare pathways for falls, it is plausible that:
- nearly 26,000 of these additional falls will require a GP visit
- 30,000 will require an ambulance call out
- over 14,000 will require an inpatient stay
- over 12,000 will require a care home package
Despite the lifting of restrictions, there is evidence that levels of physical activity have remained low throughout 2021, meaning that many people are likely in need of additional support.[footnote 21][footnote 22][footnote 23][footnote 24]
We are committed to taking action to support the older adult population by finding innovative ways to increase strength and balance activity among those who have been most affected by deconditioning – in particular:
- people who shielded
- those living with multi-morbidity or dementia
- those living in social care settings
- people from more deprived backgrounds
We will invest up to £3 million over 3 years towards the establishment of a deconditioning inequality innovation fund to enable local authorities to support people at particularly high risk of deconditioning. This fund will be administered by OHID and will help to retain capacity across the health and care system, reduce falls and facilitate COVID-19 recovery by enabling older adults to resume their pre-COVID-19 activities safely and confidently.
By its very nature, prevention activity is an investment – it involves acting now to realise benefits over an extended period of time. Benefits come in the form of enhanced health and wellbeing outcomes for individuals, and driving efficiency in the delivery of public services.
Measures set out in the Health and Care Bill and the forthcoming integration white paper focus on driving joined-up decision-making across health and care systems, of which prevention is a key part.
Empowering those who draw on care, unpaid carers and families
We want people to be able to say…
I know where to find user-friendly information and advice that is inclusive of my communication and accessibility needs to make informed and empowered decisions about my life – now and in the future.
I know what my rights are and can get information and advice on all the options for my health, care and housing.
I understand the support that is available to me in my area to maintain my own health and wellbeing and achieve the outcomes that matter to me.
I am provided with tailored information and advice to support the person I care for.
Every proposal in this white paper is aimed, in some way, at improving the daily lives of people who draw on care and support, their families and their carers.
Even before people are able to draw on support and care services, they struggle navigating a complex system and understanding what might be available to them. Equally, unpaid carers can also find it difficult to find support they may be entitled to, and in some cases, feel that the support on offer is insufficient to maintain their own health and wellbeing, support their employment, and achieve the outcomes that matter to them.[footnote 25]
We know that being able to access user-friendly information, advice and advocacy to navigate the health and care system with ease, so that everyone can understand what their rights are, is essential for enabling people to make informed decisions.
In this chapter, we outline policies that are designed to empower those who draw on care and support, their families and unpaid carers. Specifically:
- improving information and advice
- empowering unpaid carers
- supporting autistic people and people with a disability into employment
Overview of main policies
-
Invest at least £5 million to test and evaluate new ways to help people navigate local adult social care systems.
-
A national website providing information and simple explainers about adult social care reform.
-
Invest up to £25 million to work with the sector to kick-start a change in the services provided to support unpaid carers.
-
A new obligation for ICBs and NHS England to involve carers when commissioning care for the person they care for.
-
The Department for Work and Pensions (DWP) will launch local supported employment to identify effective ways local authorities can support autistic people and people with learning difficulties into employment.
-
The Department for Business, Energy and Industrial Strategy (BEIS) will introduce a carer’s leave entitlement of 5 days of unpaid leave a year for eligible employees.
Improving information and advice
People who draw on care and support, their friends and family, and their unpaid carers need to understand:
- what they may be entitled to
- what is available to them in their area
- how to access that support
We know that people often access care and support at a time of crisis, and some struggle to understand how adult social care works and what is available to them.
Information and advice[footnote 26] services are currently delivered both locally and nationally by a range of different organisations. Nationally, resources are available that set out the basic facts about adult social care, and entitlements to care and support, which apply equally wherever people live (for example, the NHS social care and support guide. However, adult social care services are managed and delivered locally, and local authorities have duties under the Care Act 2014 to ensure that information and advice services are available to their local populations. Information and advice about where and how to access support is therefore best provided locally.
Stakeholders have noted that some people do not know how to, or do not want to, go to their local authority, and may seek help or advice from family and friends, community groups, the voluntary sector, or doctors and nurses. This means that people end up seeking advice from multiple fragmented places, potentially receiving confusing or conflicting advice.
A package to improve information and advice
The Making it Real framework sets out that good information and advice is about “having the information I need, when I need it”.
We want to make the experience of accessing care and support as simple and as informative as it can be, ensuring that information and advice services are available and accessible to everyone who may need them. The overall framework is already set by the Care Act, but the government has an ongoing role to play in providing oversight, and building an evidence base of effective approaches and strategies.
There is also a role for national government to raise awareness of the upcoming reforms to adult social care. As a result of the new cap on care costs, people will no longer face unpredictable or unlimited costs and it will be easier to start to plan financially for care in later life, including thinking about their housing arrangements.
To take the first steps towards our vision, we have designed with stakeholders a package of measures for the next 3 years. It targets those challenges identified as the highest priority to improve the current information and advice system. The package has 3 principles:
- everyone should be aware of basic information about adult social care and the upcoming reforms to the system
- people should have access to personalised advice about adult social care when they need it
- there should be oversight and accountability of information and advice services
a) Informing the public about social care reform
Under the current system, around half of all older adults in care receive some state support for their care costs. This will rise to roughly two-thirds under the upcoming reforms. This represents a major shift in eligibility for state support.
We will therefore create a national website providing information and simple explainers about adult social care reform for the public to be launched this year.
b) Personalised advice about adult social care
A lack of easily accessible, personalised advice was highlighted by stakeholders as the biggest gap in the current system and the area where there is most scope for innovation.
Personalised advice is best delivered locally, so it can link to services and support that are available in a particular area. There are some national and local initiatives that already provide personalised advice[footnote 27], but access to these depends on where a person lives and their needs. Despite these efforts, people still struggle to understand the system, so there is clearly a need to do more.
We will therefore provide dedicated funding worth at least £5 million over 3 years to local organisations to pilot and evaluate new ways to provide personalised advice to help people navigate local adult social care systems. We will start by reviewing existing local initiatives, and identifying strengths and gaps. We will convene an expert panel of stakeholders and academics from the adult social care and advice sectors, along with people who draw on care and support and carers, to help shape the way funding is used and provide guidance to those delivering the pilots. We will also consider international comparisons and learn from examples such as Japan, where social care practitioners are embedded into the system and offer personalised support to individuals to navigate social care.
The evaluation of these pilots will enable government to provide guidance to the care and advice sectors about the impact of different initiatives, including ‘what works’ and what is good value for money. This evidence will also be used to inform national policies, and support local authorities and their local partners on how best to use budgets on advice services.
c) Improving oversight of local authority information and advice offers
We will not achieve our vision unless everyone has access to high-quality information and advice, wherever they live in the country.
The upcoming chapter on how we will support local authorities to deliver social care reform and our vision explains how the government intends to increase oversight of local authority practices and their delivery of their social care duties, and this will include how local authorities empower people and enable them to make informed decisions, including the quality of the information and advice provided.
This will allow for improved evidence and understanding of local provision of information and advice services, including what is working well, which we can disseminate across the country.
d) Providing people with the basic information they need to compare providers
There is little comparable information on the types of care and support available, and often very little transparency on what price people might expect to pay over time.
This is out of step with an accessible care system and so, as a first step, we will consider changing the Care Quality Commission (Registration) Regulations 2009 to require CQC-registered providers to be more transparent about their fees to help people make informed decisions. Some providers already do this but, in order to allow people to easily compare and choose services, it needs to be universal.
To help people choose the right provider for them, we also want to explore how to allow better, more transparent feedback about services, and other comparative information on quality, effectiveness and availability.
Effective information and advice in action: Julie’s story
Julie worked as a nurse and social worker before being diagnosed with young-onset dementia in her 50s. Following the diagnosis, she wasn’t offered any ongoing support, information or advice.
Fortunately, due to her professional knowledge and experience, Julie knew where to go for advice, as she had previously signposted those she worked with towards the Alzheimer’s Society. Julie went to her local Alzheimer’s Society and felt such relief when she sat down with a dementia adviser over a coffee to have a chat.
Dementia advisers provide tailored information and advice so that people can consider their options, and provide support to people with dementia to access local professionals and services. Julie’s dementia adviser shared some written information resources and they talked through local support options.
With support from her local Alzheimer’s Society and local ‘staying well’ group, Julie was able to set up her own local peer support group for people with young-onset dementia. It was through holistic, person-centred advice, taking account of Julie’s particular circumstances such as her age, that Julie was able to access the type of support that was important to her.
For people like Julie, it is really important that information and advice contains positive messages, concentrating on people’s strengths and abilities rather than disabilities, so they can be supported to live well with a diagnosis.
A key component of better information includes a strong feedback culture and we recognise the importance of this in adult social care. This culture should enable organisations to continuously improve and ensure people have effective routes of redress if they are unhappy with the care or support they receive. The current system requires local authorities and social care providers to have their own complaints procedures.
If someone is not satisfied with the way a care provider or local authority has dealt with a complaint, they may escalate it to the Local Government and Social Care Ombudsman.
The Care Act 2014 includes a provision to introduce a new system to allow the public to appeal certain social care decisions made by local authorities. While we do not intend to introduce such a system immediately, we are keeping it under ongoing review as the new reforms are implemented and will continue to gather evidence to inform future thinking.
Direct payments and personal budgets
Direct payments and personal budgets are a vital way in which people can have more choice and control over their care and wellbeing. During the COVID-19 pandemic, direct payments were made to family and friends who did not normally live with the person drawing on care and support to provide greater flexibility to support families who were left in desperate situations without their usual carers.
We want to ensure that local authorities, in line with the Care and Support (Direct Payments) Regulations 2014, offer people direct payments, including advice and support in using their direct payments.
Following the announcement of a cap on care costs, we will explore how direct payments could be used as a mechanism for making payments once the cap has been reached. We will work with the sector to consider what changes could be made, sharing examples of best practice.
We will also consider international models and how other countries make use of different direct payments systems to inform our thinking. For example, Germany gives all care recipients the option of receiving cash benefits for family members, whether through direct payments or individual service funds, and Australia has introduced a National Disability Insurance Scheme model for people with disabilities, which provides funding directly to individuals.
If we get this right, we can make the most of the expertise, capacity and potential of people, families and communities to deliver better health and wellbeing outcomes and experiences for everyone who interacts with the support and care system.
Empowering unpaid carers
For the vast majority of people, care begins at home with their families. Many people wish to play a role in caring for their friends and family, and we recognise that for some this can be a significant commitment. The 2011 Census reported that almost 1 in 4 (23% or 1.3 million) of those providing unpaid care were caring for over 50 hours a week. We expect this figure to be higher when the new 2021 Census figures are released. A variety of estimates also exist for the value of unpaid care provision, including the Office for National Statistics who estimate that the gross value added of unpaid care in the UK was £59.5 billion in 2016.
Caring is not always easy or straightforward. There is a wide variety in caring circumstances, experiences and needs among carers. Caring can be rewarding, but it can also have negative impacts on the carer, such as making it difficult to balance paid employment with care, or preventing people from socialising or undertaking other activities as much as they would like.
Just over 1 in 10 (11%) adult unpaid carers report not being in employment due to their caring responsibilities, and this figure rises to 36% among those providing 20 or more hours of care a week. Almost half (45%) of unpaid carers report caring having an impact on their personal and social lives, and 52% report that providing care has an impact on their health, including physical strain, stress or exacerbating an existing condition.[footnote 28]
The way the adult social care system works in partnership with and supports carers is critical. Our vision for adult social care is one that places people at its heart – and that includes recognition and support for unpaid carers so that they are empowered to live happy, healthy and fulfilling lives.
The Care Act 2014 requires local authorities to deliver a wide range of sustainable high-quality care and support services, including support for unpaid carers. We know that the full spirit of the Care Act has not always been realised, but it continues to provide a clear foundation for support for unpaid carers.
Local authorities are required to undertake a carer’s assessment of any carer who appears to have a need for support. This is an opportunity to record the impact caring has on a carer and will look at all of the carer’s needs, including whether they are willing or able to continue caring. If a carer is assessed as having needs that are eligible for support, then the local authority has a legal duty to meet these needs on request from the carer and to draw up a support plan with the carer setting out how these needs will be met.
The local authority can provide services itself or arrange services through another organisation. Depending on their financial situation, the carer may have to contribute towards or pay the full cost of the services. Alternatively, if the local authority is contributing towards the cost, the carer may be able to request a direct payment to buy services to meet their eligible needs.
Carers action plan
In June 2018, the government published the carers action plan 2018 to 2020 with the aim of setting out its short-term programme of action to support unpaid carers.
The action plan contained 64 actions that draw on a wide range of government departments and carer representative organisations including:
- Carers UK
- Carers Trust
- The Children’s Society
- NHS England
- Health Education England
- Public Health England
- Association of Directors of Adult Social Services (ADASS)
The plan focused on 5 themes:
-
Services and systems that work for carers.
-
Employment and financial wellbeing.
-
Supporting young carers.
-
Recognising and supporting carers in the wider community and society.
-
Building evidence and research to improve outcomes for carers.
Good progress has been made in some areas since the plan was published, including:
- achievements that help carers in their everyday lives by increasing awareness among employers of the impact that caring has on their workforce
- supporting health and social care professionals to better identify and work with carers
A detailed summary of these achievements is in Annex B.
As we move towards a new vision for social care, we will build on the foundations of the carers action plan to set out a new strategic approach centred around 3 core strands:
-
Working with the sector to kick-start a change in the services provided to support unpaid carers.
-
Identifying, recognising and involving unpaid carers.
-
Supporting the economic and social participation of unpaid carers.
Working with the sector to kick-start a change in the services provided for unpaid carers
We have heard that unpaid carers value services and support provided for them and the people for whom they care, such as respite and breaks. As shown by Carers UK in the State of Caring 2021: a snapshot of unpaid care in the UK, the availability and accessibility of these services is not always as easy or straightforward as it should be.
To address this, we will invest up to £25 million to work with the sector to kick-start a change in the services provided to support unpaid carers. We expect that this funding will identify and test a range of new and existing interventions that support unpaid carers, which could include:
- respite and breaks
- peer group and wellbeing support
- new ways to combine these to maximise their impact
The projects initiated through this funding will build commissioner and service provider understanding of what support works best for those with different caring circumstances, acknowledging the wide variety in caring experience and need among carers.
There will be extensive impact and process evaluation conducted to generate evidence on efficient and effective ways to support unpaid carers. By continuing to build and share the evidence, our aim is to drive the development of a strong investment case for commissioners, and therefore stimulate the growth, development and roll-out of services across the country.
We have heard that respite is a particular area of concern and so, during development of the policy, we will work with the sector (including local authorities) to further explore:
- the different models of respite
- how respite services are accessed by carers
- any barriers to accessing these services that carers might experience
At the core of our approach is recognising that people who provide care are diverse and varied – different services and interventions are likely to be effective for different groups of carers depending on individual circumstances. For example, the rates of depression are higher among those who provide care for people with dementia than among caregivers of people with other chronic illnesses.[footnote 29] Another example might be unpaid carers from ethnic minorities, where there is a particular lack of self-identification as an unpaid carer.[footnote 30]
Support for unpaid carers in action: Linda and Ken’s story
Linda Barnes looks after her husband Ken who was diagnosed with Alzheimer’s disease in 2016 at the age of 53 – a process which Linda describes as a battle to prove his difficulties were not a result of anxiety, depression or stress.
Linda knew very little about dementia, despite her nursing background, and had to do her own research initially. She then found herself educating her GP as he did not know how to help. She has had to learn how to understand Ken and what he is trying to communicate and has become an expert in his care. Ken’s Alzheimer’s affects the parietal lobe.
His comprehension of money and time are affected, as well as his recognition of words and their relationship to objects or activities they are describing – known as semantic dementia. This is very different from the man who had built their house and received an award as Special Constable of the Year. For these reasons, Linda started a blog to educate others about the realities of dementia and caring for someone with the condition. She is amazed that – unlike other long-term incurable conditions such as cancer – there is so little support available for people with dementia and their carers.
After diagnosis, Ken was prescribed Aricept and they were given a big batch of leaflets but had no follow-up or offers of help and support. Linda had to give up work and felt lost about her role: she was no longer the wife that she used to be and the dementia has changed their relationship:
The day when I realised I was responsible for absolutely everything – finance, healthcare, running the household, his personal care – was a huge shock and I felt very alone.
Linda was contacted by a social worker the day after she appeared on local TV as part of an awareness-raising campaign about the needs of younger people with dementia. They were not on social services’ books. A visit was arranged and Linda had a carer’s assessment that led to a Blue Badge being issued, which she described as “really helpful”.
The hardest thing for Linda is the uncertainty. How long will this go on for? How quickly will things change?
Life can’t carry on without us as carers – Ken is totally dependent on me and I don’t know where he would be without me.
Identifying, recognising and involving unpaid carers
As well as valuing the services provided to support unpaid carers, we have also heard that carers want to be recognised, and more extensively involved across health and adult social care services.
Improving the ability to identify carers is crucial for recognising and supporting unpaid carers and improving policy-making. Better information will enable local authorities and health and care services to better understand who is being cared for by friends or loved ones, and to better support carers’ health and wellbeing. However, data relating to unpaid carers can be difficult to collect and use.
We will therefore look to increase the voluntary use of unpaid carer markers in NHS electronic health records by simplifying current approaches to data collection and registration. We will also introduce a new marker indicating the presence of a contingency plan, where one is available, that describes the actions to take if the carer is no longer able to provide care.
Additionally, the move away from aggregate data collections on carers towards client-level data, which will take place over the next 3 years, will also improve our understanding of unpaid carers. Further information on the client-level data project can be found in the upcoming chapter on supporting local authorities to deliver social care reform and our vision.
The Health and Care Bill provides an opportunity to create a health and care system that is more accountable and responsive to the people that use it. As part of this, we are committed to ensuring that the voices of carers – as well as those who access care and support – are properly embedded in ICSs. The Bill provides a duty on ICBs to involve carers when exercising their commissioning functions. There are equivalent provisions for NHS England commissioning services. This means the services commissioned through these routes in the area where the carer lives will have considered the impact on carers in that community.
Supporting local authorities to deliver social care reform and our vision also outlines our intention to introduce a new assurance framework for local authorities. This will include assessing how local authorities are meeting the needs of unpaid carers.
Supporting the social and economic participation of unpaid carers
Empowering those who draw on care and support – and their carers – is not only about being able to understand and access the right services. Empowerment also means that people feel able to lead a fulfilling life and achieve the goals that matter to them.
We recognise that unpaid carers, as a group, are disproportionately impacted by loneliness compared with non-carers.[footnote 31] 45% of carers experience an impact on their personal and social lives as a result of the care that they provide. This increases to 71% among those that provide 20 or more hours of care a week, with just over one-third of this group (34%) feeling unable to socialise at all due to their caring responsibilities.[footnote 28]
The Department of Health and Social Care (DHSC) is working with NHS England and the Carers Partnership, formed of the Carers Trust and Carers UK, to produce a social prescribing summary document to be disseminated to local carers organisations. It will upskill staff at carers organisations on social prescribing as an intervention for loneliness, and to increase unpaid carer health and wellbeing. This work will increase the consistency of the social prescribing offer to carers across England, as the government’s provision of social prescribing link workers continues to increase.
The DHSC is working with these same organisations to evaluate good practice in social prescribing to reduce unpaid carer loneliness, as well as testing loneliness interventions among unpaid carers. This will increase the evidence base on unpaid carer loneliness interventions, which can then be used to inform future national policymaking and local voluntary, community and social enterprise interventions.
In addition, the challenges of providing care can have a big impact on the careers of carers and limit their participation in the workplace. This impact is felt disproportionately by women, who tend to be the main carers within households. 28% of adult female carers felt that their employment had been impacted as a result of providing unpaid care, including needing to reduce responsibility at work or work fewer hours. This is compared with 17% of adult male carers.
Empowering workers to have more say over where and when they work makes for more productive businesses and happier employees. Flexible working allows employees to balance their work and home life, including helping people manage caring responsibilities. In September, BEIS published a consultation on measures to increase the availability and uptake of flexible working.
This is an important part of our drive to provide more choice and control to unpaid carers to help them to access and stay in work whatever their personal circumstances. Under the proposals, every employee would be given the right to request flexible working – freeing employers and employees alike from the default 9-to-5 model to find ways of working that best suit their needs.
The government has also confirmed its commitment to introduce carer’s leave in its response to a 2020 public consultation. Carer’s leave will support working people who are also carers to balance employment with their caring responsibilities. This will be a day one right, available to all employees who are providing care for a dependent with a long-term care need. Eligible employees will be entitled to 5 days of unpaid leave a year, which will be available to take flexibly in individual or half days.
When caring responsibilities prevent or limit the amount of work an individual can do, then they may be able to receive support through the benefit system. This includes Carer’s Allowance, which provides a measure of financial support and recognition for people who give up the opportunity of full-time employment to provide regular and substantial care for a severely disabled person.
The new rate of Carer’s Allowance from April 2022 means that, since 2010, the rate of Carer’s Allowance has increased from £53.90 to £69.70 a week, providing an additional £800 a year for carers. To make the whole process easier for carers to navigate and for money to be paid more quickly and more accurately, the government has a programme underway to modernise the way it delivers Carer’s Allowance.
Supporting young carers
The government believes that young people should be protected from inappropriate and excessive caring responsibilities, and that adult and children’s services need to work together and take a ‘whole family’ approach to the identification and support of young carers.
Too often the important role they play goes unnoticed, putting their education, training or health at risk, and preventing them from enjoying their childhood in the same way as other children. To address this, local authorities must now offer young carers assessments and consider young carers’ needs when assessing support for adults.
But we know we must build on the legal framework and do more for young carers – including as a result of the pandemic. The Department for Education (DfE) has highlighted young carers’ needs in their guidance to schools on use of education recovery programmes and funding (including their recovery premium and pupil premium guidance, and list of vulnerable children who can access schools or educational settings), and will, for the first time, take steps to better quantify the numbers of young carers and understand the direct impact that being a carer has.
DfE will amend the school census, at the earliest opportunity, to include young carers. This change has the potential to be truly transformative – it will, by its very nature, raise the visibility of young carers in the school system – and will also give us a wealth of demographic evidence on the young carer population. Equally as important is the light it will shine on their educational achievement – allowing us to understand the impact of caring, including hard evidence on attendance and absenteeism, as well as headline information on educational progress and attainment.
Given the annual nature of the census, we will also be able to establish long-term trend data, and evidence the impact of any future support or investment that we may introduce as a result of the new evidence base.
Supporting autistic people and people with a learning disability into employment
A key priority for the government is making sure that groups who face challenges in the labour market have the required support to allow them to obtain – and crucially keep – a job. A job is not only a means for earning an income – it supports an individual to be independent, make new connections, save for their own retirement, and provides a sense of accomplishment and worth.
People with disabilities face particular barriers in the labour market, and autistic people and those with a learning disability face heightened challenge. The employment rate for autistic people is 26.5% and 25.6% for those with a severe or specific learning disability, which compares with 52.7% for the disabled population as a whole. For people with a learning disability receiving long-term social care support, the rate has been around 5 to 6% for many years (5.1% in 2020 to 2021). Autistic people and people with a severe learning disability often find it hard to navigate recruitment processes and demonstrate their skills before starting a job, and can need support settling in to work.
With the right support in the right job, they often prove to be valuable and committed employees who will stick at jobs, and there are benefits for the individuals concerned in terms of their own health and wellbeing outcomes. Supported employment helps individuals into employment using a ‘place - train - maintain’ approach. This internationally recognised model focuses on employment rather than a lengthy period of pre-employment training. There is a strong focus on working with the employer, as well as the individual, to get the right job match.
The DWP funded a proof of concept of the local supported employment approach from 2017 to 2019 as part of its Improving lives: the future of health, work and disability green paper. This aimed to increase the number of social care users in jobs, with local authorities providing individuals with significant barriers to work with intensive one-to-one support to enter and stay in work.
Following on from this, DWP will now fund a local supported employment scheme, working with 20 local authorities, expected to begin in 2022. The initiative will support approximately 1,200 participants with a learning disability or autistic people who use local authority social services.
Access to Work provides support beyond employers’ reasonable adjustments (funding support workers, travel to work, aids and adaptations).
A new proof of concept, Access to Work Plus, will test new enhanced support for disabled people with high in-work support needs, such as those receiving social care support. This will include a higher level of personal support and financial support for employers who are willing to do more to flex job roles and create supportive working environments. We want to see if this can open up new job opportunities for those who might otherwise be locked out of the labour market. The proof of concept is expected to start in 2022.
Our strategy for the social care workforce
We want people to be able to say…
I receive care and support that is safe, responsive to my needs and respects my rights.
I am supported by a workforce who have the right training, qualifications and values, and are concerned about what matters to me.
I receive care from a workforce whose careers are valued, and whose professional development and wellbeing are prioritised.
Social care is a rewarding career with clear opportunities to develop and progress, and where I feel valued in my role.
I feel recognised for the important role I play in helping people who draw on care and support to receive high-quality personalised support that enriches their lives.
I feel recognised for the skills I bring, and am able to develop new skills that help me tackle new challenges as I become more experienced.
There is a culture in my workplace that supports my health and wellbeing.
I have the confidence to use technology that supports people’s needs and to free up time to deliver outstanding-quality care.
Social care staff have been unwavering in their dedication for those they support, which is a truly incredible achievement, both before and throughout the pandemic.
We know working in social care can be rewarding but challenging as well, particularly dealing with the impact of COVID-19, including working long hours. It is why the government has made significant additional funding available since the beginning of the pandemic to help employers and local authorities support local workforces.
As the sector emerges from the pandemic this winter, we will continue to work closely with local authorities and care providers to monitor workforce pressures, including whether further action may be required.
Looking ahead, we want all those working in adult social care to feel valued for their dedication and their vital role in enabling the dignity and independence of the people they support and their families. Our vision is for an adult social care workforce where people can experience a rewarding career with opportunities to develop and progress now and in the future. We want staff to be empowered to deliver the highest quality of care.
With over 1.65 million jobs, the adult social care workforce is larger than the NHS, construction, transport, or food and drink service industries. The number of jobs in adult social care is forecast to grow by almost one-third by 2035. As the population grows, and the way care that is delivered evolves and diversifies, the adult social care workforce will need to grow and develop with it.
There are already pressing recruitment and retention challenges and barriers, which we have been discussing with sector representatives and staff. We recognise the ongoing hard work by providers and local authorities – working with system partners such as the NHS – to address difficult workforce capacity issues.
To meet these challenges, we need to ensure that:
- those working in social care feel recognised, rewarded and are equipped with the right skills and knowledge
- staff health and wellbeing is prioritised across all organisations
- new government policies are implemented in partnership with the sector and at a consistent standard across the country
That is why we are investing at least £500 million over the next 3 years to begin to transform the way we support the social care workforce. This dedicated investment in knowledge, skills, health and wellbeing, and recruitment policies will improve social care as a long-term career choice. It will complement the government’s Plan for Jobs by boosting the sector’s skills with the expertise employers need. As part of this, by harnessing and building on the significant skills and expertise already within the workforce, we will develop new universal career structures and training opportunities to enable people to progress and realise their potential.
The government is increasing the National Living Wage by 6.6% in 2022 alone, with a commitment for it to reach two-thirds of median earnings by 2024. This will give the lowest-paid care workers a real-terms pay rise.
We also want to work with commissioners and providers to make sure care workers are paid for all the hours they work, and to improve the terms and conditions of the workforce, to help ensure a sustainable future supply of care staff. This includes acknowledging the prevalence of zero-hour contracts in the sector, which can result in uncertainty around employment status and rights. Further detail on a new approach to assurance is set out later in supporting local authorities to deliver social care reform and our vision.
Recognising the diversity of the social care system, with its wide range of organisations, settings and people, we will seek opportunities to work alongside the sector in local and national partnership to ensure it can continue to empower people to live as independently as they choose. We want to continue to listen to and engage with the full breadth of the workforce, including:
- care workers
- personal assistants
- registered managers
- regulated healthcare professionals
- social workers
The workforce strategy set out here is just the beginning. The government will need to work closely with adult social care leaders and staff, as well as people who draw on care and support, to implement it and take forward these policies, now and in the future.
Overview of main policies
At least £500 million to transform the way we support and develop the workforce including:
- a knowledge and skills framework, careers pathways and linked investment in learning and development to support progression for care workers and registered managers
- funding for Care Certificates, alongside significant work to create a delivery standard recognised across the sector – this will improve portability, so that care workers do not need to repeat the Care Certificate when moving roles
- continuous professional development budgets for registered nurses, nursing associates, occupational therapists and other allied health professionals
- investment in social worker training routes.
- Initiatives to provide wellbeing and mental health support, and to improve access to occupational health
- a new digital hub for the workforce to access support, information and advice, and a portable record of learning and development
- new policies to identify and support best recruitment practices locally
- exploration of new national and local policies to ensure consistent implementation of the above, as well as higher standards of employment and care provided
Wellbeing support in action: Isaac’s story
Isaac is an employer and has received self-directed support for over 10 years. He has experienced a variety of support, and realised that factors such as training and development, staff wellbeing, and opportunities to develop a career in social care have a huge impact on the quality of support he receives.
As an employer, he has made changes to support the wellbeing and development of his personal assistants (PAs). For example, Isaac holds wellbeing meetings to discuss how their feelings and lives are affected by work. They discuss how to arrange more flexible support to help them manage other caring duties, create wellbeing plans and talk about their future career ambitions.
As a result, Isaac and his PAs can look at training and development opportunities to meet these goals, including building their skills and confidence.
This provides Isaac with the security of knowing someone wants to continue in the role and helps retain vital skills in the care sector. He can trust his PAs fully to plan his care and support. In his own words:
It is a two-way relationship, and supporting people who provide my care and support means that I am able to get on with my life, confident that my team have everything they need.
Over the next 3 years, these policies aim to create a:
- well-trained and developed workforce
- healthy and supported workforce
- sustainable and recognised workforce
A well-trained and developed workforce
Figure 1: knowledge and skills framework, and career structure
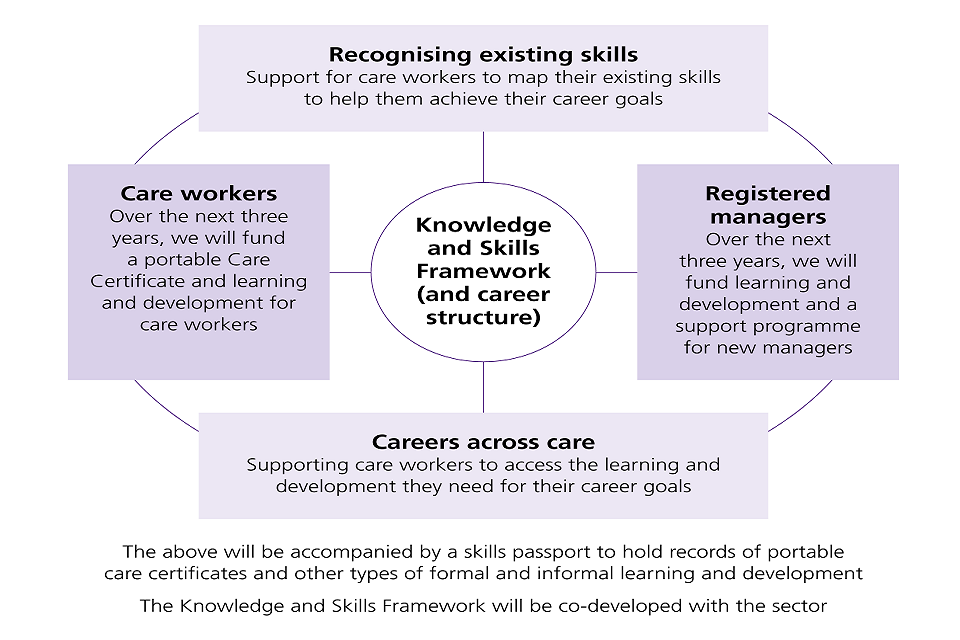
Knowledge and skills framework and career structure
Over the next 12 months, we will work with the adult social care sector, including providers and the workforce to co-develop a universal knowledge and skills framework (KSF) and career structure for the social care workforce as shown in Figure 1 above.
This will include exploring options to embed the KSF consistently across the sector so that it becomes a recognised benchmark for all social care roles.
Building on existing and emerging frameworks for the workforce, and working with the DfE in its development, this national framework will become an accessible articulation of the knowledge and skills required for roles within the sector, and set out clear pathways for career progression. We will also invest in hundreds of thousands of training places and certifications to enable the workforce to develop and progress within the KSF now and in the future, building on existing skills and expertise.
The KSF will draw on and complement the existing skills offer delivered via colleges and training providers in England. DfE funds a range of skills and training provision for the social care sector, as part of a wider programme of reform that is helping to generate the skills needed for a strong and productive future economy. This involves:
- working with employers to deliver apprenticeships and traineeships
- helping adults access fully funded Level 3 (A-level equivalent) qualifications in social care, if they do not already have one, as part of the Lifetime Skills Guarantee
- extending that offer from April 2022 to any adult earning under the National Living Wage regardless of their prior qualifications
- funding a wide range of social care courses via the adult education budget
We will continue to ensure that high-quality apprenticeships meet the skills needs of social care employers, and provide people of all ages and backgrounds with the opportunity to benefit.
We have worked with employers and training providers in the sector to promote more flexible models of apprenticeship delivery, including the front-loading of training and accelerated apprenticeships. We know that, as the demands and complexity of providing care increases, apprenticeships will need to keep pace to continue providing high-quality training. We will therefore continue to work with the DfE, Institute for Apprenticeships and Technical Education, and sector partners to support apprenticeship growth, address barriers and increase quality.
We will also work with DfE to explore opportunities (for example, via Local Skills Improvement Plans) to:
- strengthen local collaboration between employers and training providers
- maintain high standards of training
- share intelligence on the local demand for and supply of skills
- cement a strong pipeline of skilled individuals into the future
Care workers
Portable Care Certificates
Investment in a portable Care Certificate is a key part of our offer. The Care Certificate represents a key set of standards that form part of a robust induction programme for those new to social care. However, it is not always delivered in a consistent way, meaning care workers often have to repeat training when they move roles.
We will work with the sector to design new training delivery standards, exploring options for external validation and accreditation, to ensure Care Certificate training is high-quality and portable, so that care workers can carry it with them throughout their careers.
Longer term, we want to reach a position where it is a requirement for all care workers to have reached this baseline standard, and we will explore options for how to achieve that.
KSF-linked learning and development offer
The new national KSF will be accompanied by a funded learning and development offer, creating opportunities for the workforce to become experts in their field or progress into new roles.
Over 3 years, the learning and development offer will provide hundreds of thousands of training places and qualifications at all levels so that the workforce can access knowledge and skills to meet both individual career goals and the needs of people who draw on care and support. This funding will be linked to the KSF and targeted to address skills gaps, as well as support career development and expertise.
Skills passport
A new skills passport will help to address issues of portability of staff training and development. We will embed this as a function in a new digital care hub for the workforce. It will provide a permanent and verifiable record of skills, behaviours and achievements that can be shared with new or potential employers.
Registered managers and regulated professions
Leadership development and tailored support for registered managers
We need to recognise the vital role registered managers have in ensuring the delivery of high-quality care and developing a skilled workforce in their organisation.
We will explore options to develop new pathways into the registered manager role. We will fund accredited Level 5 diplomas for registered managers who do not hold relevant formal qualifications. In addition, we will introduce a bespoke support programme for new registered managers in their first year, which will offer learning and development opportunities, peer support and mentoring.
Regulated professionals within the social care workforce, including registered nurses, nursing associates, social workers and occupational therapists, play a pivotal role working alongside care workers and registered managers to deliver person-centred care. Our long-term aim is to complement the existing frameworks for regulated professionals working in social care by ensuring that there are sufficient high-quality training routes and access to effective post-qualification support, including Approved Mental Health Professional accreditation.
In July 2021, we commissioned Health Education England to work with partners and review long term strategic trends for the health and social care workforce. For the first time ever, the long-term strategic framework will include professionals working in social care, such as nurses, social workers and occupational therapists. Once published in spring 2022, the framework will inform long-term workforce planning, and ensure we have the right numbers, skills, values and behaviours to deliver world-leading clinical services and continued high standards of care.
Registered nurses, nursing associates, occupational therapists and other allied health professionals who work in social care will be supported with a new fund to help them meet their continuous professional development objectives, including meeting the standards set by their respective regulatory bodies, and to develop their skills and experience further.
We are committed to improving the quality of social work education and training, and maintaining a sufficient supply of social workers with the right skills, knowledge and values. We will invest in new training routes for people who want to become social workers. In addition, over the course of the next 3 years, we will work with the Chief Social Worker for Adults, Chief Social Worker for Children and Families, DfE, and Social Work England to improve the overall pre- and post-qualification landscape for social workers.
Alongside our existing initiatives – such as providing support and development for the Principal Social Workers Network, Education Support Grants and social work bursaries – this will ensure we lay the right foundations now to meet future demand for social workers and for the continued success of the social worker profession in the long term.
Staff training in action: Jamal’s story
Jamal is a mental health and learning disability support worker, and has worked in 2 different organisations in the last 5 years. Jamal’s clients experience a range of learning disabilities, mental health needs and substance abuse issues, so Jamal personalises his approach to support every person.
The support Jamal receives himself as a support worker differed a lot between the 2 employers. His second employer, although much smaller, gives personal support to Jamal, including a culture where his manager makes time for him, and invites him regularly to discuss and reflect on how he feels. Management also use sessions for group reflections, looking at how the organisation could perform better, which makes Jamal feel heard and supported.
Jamal has found the training he received at both organisations to be really good but, upon moving organisation, a lot of the training was not recognised as being transferable, causing him to repeat things he’d already learnt. During the onset of the COVID-19 pandemic, Jamal saw clients with higher levels of need, such as more complex medication regimes, and felt that he would benefit from training packages to ensure he was suitably trained to deal with the levels of complexity.
In terms of career progression, Jamal found that, while he was able to move around the sector at his level, it would be very hard to move up. Jamal felt that, if training was standardised, it would help him articulate and build his capabilities, and for employers to recognise his potential – which could help him progress in a care career.
A healthy and supported workforce
Figure 2: wellbeing and occupational health offer

We recognise the immense sacrifice made throughout the pandemic by the social care workforce, which, alongside the NHS, has been at the forefront of society’s response to the COVID-19 pandemic. We know this has been a difficult time and appreciate the impact of this on many people’s personal lives and mental health.
Our new wellbeing and occupational health offer aims to provide immediate relief from burnout, trauma and mental illness. We want to work with local authorities and care providers to reduce mental and physical sickness, and develop a more positive experience for everyone working in social care.
We want this new funding to kick-start a focus on wellbeing. We will work closely with the sector to evaluate the success for wider roll-out and establish a culture that focuses on employee wellbeing. We will also promote an awareness campaign and use the digital hub to make our offer more accessible.
The offer includes:
- counselling: we will invest in one-to-one therapeutic sessions offering tailored mental health and wellbeing support to care workers
- peer support: we will invest in group mental health and wellbeing sessions for care workers, with facilitated peer support, including online events led by leaders in the sector
- bespoke support helpline: we will ensure a confidential listening service is available for carers to call and be listened to when they need it
- mental health training: access to accredited Mental Health First Aid training for line managers, supervisors and wellbeing leads to raise awareness of mental health issues and how to recognise them in staff.
- coaching: we will invest in a coaching offer to help support psychological wellbeing and resilience and reduce burnout
- workplace wellbeing fund: this fund will enable employers and local organisations to access funding for a range of holistic interventions to support staff wellbeing.
- occupational health portal: we aim to set up a bespoke portal for social care providers to obtain information about occupational health, and link themselves with occupational health providers or initiatives in their area
- occupational health pilot: we will design and run a pilot scheme to explore collective purchasing and subsidies of occupational health provision for small and medium-sized care providers
- Freedom to Speak up Guardians: we will introduce a pilot, in collaboration with the National Guardian Office, to explore ways in which Freedom to Speak up Guardians can be introduced in the social care sector, providing a route for workers to raise concerns, and escalate issues around their wellbeing and quality of care, and support providers with their employees’ concerns
Personalised care and support in action: Sharon and Jan’s story
Sharon and Jan are Level 2 support workers who work together to support a couple. The wife has struggled on her own to manage caring for her husband, and the support provided by Sharon and Jan allows her to rest.
Sharon and Jan were creative to ensure all activities were tailored specifically to the couple. They planned a range of activities including making memory books. They additionally organised trips to local parks and made sure to celebrate the wife’s birthday in style.
Sharon and Jan took the time beyond their care duties to tidy up the garden as the couple had been unable to do it themselves. They created a lovely space in which they could both to sit outside and enjoy the fresh air.
Of Sharon and Jan’s support, the wife said:
The home carers services were unbelievable over the lockdown period. The staff brought love to my house that I’ve never even dreamed of.
It was not only for my husband’s care but also lifted my depression. I thought they were as the angels to me because I knew how to smile again when they were here.
A sustainable and recognised workforce
We want to celebrate the social care workforce and give them the acknowledgement and appreciation that they deserve. This includes combatting inequalities, which is why we will be expanding the roll-out of the Social Care Workforce Race Equality Standard (SCWRES) – developed by Skills for Care – so that local authorities will use data to create plans for ensuring staff from ethnic minority backgrounds are treated equally, feel included and valued, their health and wellbeing are prioritised, and they have access to culturally appropriate support.
We will also develop a new care workforce hub as a central digital platform for the workforce. It will allow staff to easily identify themselves as working in care, signpost the new support available for the workforce and allow all care workers to more easily find resources to help them in their careers.
The hub will also embed the skills passport. Both the hub and skills passport will be voluntary in the first instance, establishing a foundation for registration of staff in the future in a way that benefits staff and care providers alike, which we intend to explore further.
The hub and skills passport will be delivered alongside new development opportunities, including digital skills training (see previous chapter on providing the right care in the right place at the right time for information on our digital learning offer for the social care workforce), to help staff access and benefit from online forms of support and easily evidence their training electronically.
We want to ensure that we can recruit people with the right skills and values to meet care needs now and in the future. Local authorities have an important role to play in ensuring sufficient workforce capacity, as set out in care and support statutory guidance. The adult social care recruitment market is hyperlocal and local areas are best placed to support providers with recruitment, utilising their oversight of local labour markets and future service demand.
However, we recognise that this is challenging. We will provide funding to support local authorities to prepare their local markets for reform, including by moving towards paying providers a fair rate for care that reflects local costs, including workforce, where appropriate. We will be working closely with local authorities and providers as we produce future guidance.
We will also provide support to identify best recruitment practice at a local level and highlight examples across the country, and explore what further action government can take to support local areas to recruit new people into the care sector. This could include supporting local campaigns to better align with our ongoing national recruitment campaign or investment in technology.
We will also continue to work with the DWP to promote social care careers to jobseekers and support employers through local DWP infrastructure, such as jobcentres. We will also promote government Plan for Jobs skills and employment schemes – including sector-based work academy programmes – to relevant employers and candidates.
Following the UK’s exit from the EU and the introduction of the points-based immigration system in January 2021, we recognise that many adult social care roles will not be eligible for a sponsored work visa. The Migration Advisory Committee are undertaking a review of the impact of the UK’s exit from the EU on the adult social care sector, which is due to be published in spring 2022. We will consider the outcomes of this review and whether further action is necessary to mitigate against any impact on recruitment into the sector.
The package of reform outlined above will help to address some of the structural barriers that prevent people from working in adult social care by making adult social care a career of choice with development and progression opportunities, and access to wellbeing and occupational health support. This will help to make adult social care a more competitive and attractive sector to work in.
These policies will sit alongside the increase in the rate of the National Living Wage, which will support existing initiatives and campaigns to attract new staff.
The 3 aims and underpinning policies summarised in this chapter are a start. They will provide a foundation for longer-term change and a culture of innovation. Our new career pathways, national KSF, investment in training opportunities and other policies will deliver a radical shift in experience felt by staff and though the quality of care delivered.
Supporting local authorities to deliver social care reform and our vision
We have seen, and continue to see, local authorities, providers, the care workforce, carers, and local communities finding new ways to enable people to live fulfilling, independent lives with choice and personalisation central to their care. It is vital that we have the right architecture in place to underpin and support the implementation of our 10-year vision for reform.
In this chapter, we outline:
- a new approach to assuring the delivery of care by local authorities
- our proposals for supporting local authorities, including a specific focus on strengthening market-shaping and commissioning functions
- our plans for improved data that will allow us to understand how local areas are achieving our vision for reform, identify strong performance and spread best practice
Overview of main policies
We will:
- from 2022 to 2025, provide £3.6 billion to reform the social care charging system, enabling all local authorities to move towards paying providers a fair rate for care, and prepare local care markets for implementing reform.
- provide more support to local authorities, including specific support to strengthen their market-shaping and commissioning capabilities. In total, we will provide an increase in improvement funding of more than £70 million between 2022 to 2023 and 2024 to 2025, ensuring local authorities are well set up to deliver our vision for reform
- introduce a duty for the CQC to independently review and assess local authority performance in delivering their adult social care duties under part one of the Care Act 2014
- put in place new legal powers for the Secretary of State for Health and Social Care to intervene in local authorities to secure improvement where there are significant failings in the discharge of their adult social care functions under part one of the Care Act 2014
- establish an adult social care data framework by spring 2022, and improve the quality and availability of data nationally, regionally and locally
Supporting sustainable care markets, and tackling variability in market-shaping and commissioning
We want to support a sustainable care market where care and support providers are paid a fair rate for care, which encourages diversity of provider models, prioritises outcomes, and enables people to have a wide range of high-quality care and support options to choose from that provide personalised support to live a fulfilling life.
To achieve a sustainable care market and provide a strong basis for our reforms, providers must be paid a fair rate. However, as our previous chapter on strong foundations to build on highlights, the problem of underpayment exists in some parts of the country.
Therefore, from 2022 to 2025, we will provide £3.6 billion to reform the social care charging system and enable all local authorities to move towards paying providers a fair rate for care. Further details will be announced shortly.
We will work closely with the sector to:
- shape the implementation of fair rates for care
- help deliver sustainable services
- prepare local care markets for implementing the other reforms outlined in this white paper
We recognise that charging reform will mean local authorities and providers need to work together to ensure care markets remain sustainable, and continuity of care is in place in their local areas.
From October 2023, more self-funders will be able to ask their local authority to arrange their care for them to give them a choice of better-value care. This presents an opportunity for local authorities to achieve greater oversight of their local care markets, improving information about people who fund their own care, which can be used to strengthen strategic planning.
We recognise the necessity of effective contingency planning arrangements to ensure that the needs of people continue to be met should their care provider become unable to continue to provide care because of business failure. These, as well as other adult social care market oversight mechanisms, remain an area of importance that we commit to keep under review, as we continue to ensure that they remain functional, adequate and fit for purpose.
Local authority market shaping and commissioning is a critical underpinning for delivering our reform ambitions to:
- embed new models of care that can transform people’s lives at scale
- ensure sustainable markets
- implement charging reforms announced in September 2021
However, we know creating an effective market is challenging and we want to provide more support for local authorities to do this.
We want to build on excellent examples of market-shaping practice to support delivery of our reform ambitions. This includes, for example, the collaborative work of 11 local authorities coordinated by the ADASS East Region who have adopted a single regional contract for care with a range of outcome-focused care standards, helping the authorities to manage their markets more effectively. This also includes the strengths-based approach adopted by Tameside who have changed the way people are supported to live at home through the introduction of their Living Well service, investing in people’s support so it is focused on what really matters to them.
We want to ensure excellent market-shaping practice is universal. Although local authorities are tasked with this duty to shape their market, stakeholders have told us that a more joined-up approach is needed across:
- health
- social care
- housing providers
- people with lived experience
- unpaid carers
- the wider community
- providers of care and support
A new ambition for market shaping
Commissioners across health and social care developing plans to shape the local care market should:
- work in partnership with people with lived experience, unpaid carers, the wider community, providers of care and support and housing, and care workers
- map what works and existing community assets so they can be built upon, recognising that a strong approach to prevention improves outcomes for individuals
- use varied channels to understand what people with lived experience want from care and support, and what best supports wellbeing, personalisation and independence
- understand what current and future need (including people who fund their own care) across different markets will look like, utilising a population health approach
- understand what skills and knowledge the social care workforce will need to provide paid local care and support services that reflect what people want
- work in a collaborative and integrated way with health, housing, transport, leisure and other services to deliver person-centred care and support, create new opportunities to improve outcomes for people and maximise the use of resources
- understand what care and support providers are able to provide, their key drivers and how to incentivise and scale what works, and consider how to develop the diversity of models of support to better engage more marginalised communities
- consider where there may be opportunities to work with neighbouring authorities to generate efficiencies and better outcomes
This will require a step-change in market shaping, commissioning and contract management. The government is determined to ensure local authorities have the right capacity and skills to deliver reform.
Therefore, in addition to the investment in new models of care and innovation outlined in providing the right care in the right place at the right time and the measures for improving data outlined later in this chapter, we will provide support for sustainable care markets and investment in strengthening market-shaping capability.
Innovative service delivery in action: Wirral community care market
Wirral Council has been proactive in identifying those with care and support needs, and working with local care providers to encourage innovative service delivery.
They actively work with their care market to co-produce good local service offers in ways that are open, fair and transparent. Their co-production approach aims to provide a sustainable and diverse range of care providers to deliver good-quality, innovative and cost-effective services, while supporting the wellbeing of every person.
When considering the actual cost of care, fees have been set with due regard to providers’ costs, efficiencies and planned outcomes for people using services, which has helped to stimulate a responsive and flexible marketplace. This includes suitable provision for people with dementia. This approach reflects the integrated approach taken between Wirral Council and Wirral Clinical Commissioning Group.
The council also introduced an opportunity to incentivise providers to pay the Living Wage Foundation’s voluntary rate for frontline staff. This helped to support the market with its response to COVID-19 to attract and retain staff within the sector, and to recognise the valuable role of the social care workforce undertaken during the pandemic. Fee rate increases ensured that providers were able to meet their statutory responsibilities, such as paying the National Living Wage and, where they chose to do so, pay the voluntary Living Wage Foundation rate as an enhanced offer.
The council has also continued to invest in the development of viable care alternatives, such as extra care housing and a range of reablement and community services, to reduce and delay the need for long-term care, with a strong ‘home first’ ethos, caring for people at home wherever possible. Continued investment in technologies to support and reduce demand for care has resulted in the deployment of equipment in people’s homes to predict interventions and prevent longer-term demand.
The council’s good working relationship with their local care market helps providers respond to the local need, which in turn supports the council’s mission to deliver good-quality, consistent care for the people of Wirral.
Strengthening market-shaping capability
Good market shaping underpins several of our reform ambitions, but this is complex. We will therefore:
- act to strengthen the capacity of local authorities to manage market changes and assist them in successfully implementing fair rates of care
- as part of our £70 million of new improvement funding, invest in market-shaping, commissioning and contract management capability in local authorities. It is our intention that this offer includes a focus on areas such as access to continuous professional development, support for developing a clear career path for commissioners, and strengthening leadership
- work in partnership with the sector to undertake a review of existing market-shaping capability initiatives to identify gaps and what action could address them to accelerate a universal strengthening of the role
A new assurance framework
We want to create the right frameworks so that it is easy for local people, providers and national government to see how well local authorities are meeting their adult social care duties under part one of the Care Act 2014.
Our assurance and support proposals will:
- help the sector to better identify and share strong practice
- ensure that improvement funding meets any support needs
- provide a basis upon which we might exercise new legal powers to intervene where a local authority is failing or has failed to discharge its duties under part one of the Care Act 2014
They are based around:
- independent assessment of local authorities by the CQC
- an enhanced improvement support, led by the sector
- a mechanism to intervene, as a last resort, if a local authority is failing
- better data
CQC assessment of local authorities
The ability to review and assess how well local authorities are fulfilling their key adult social care functions is key to ensuring that our vision for reform is delivered.
The Health and Care Bill creates a new duty for CQC to independently review and assess the performance of local authorities in delivering their adult social care functions, as set out under part one of the Care Act 2014. These assessments will provide a greater understanding of practice and provision at local level, making it easier to see what is working well, and make good practice, positive outcomes and outstanding quality easier to spot and share nationally.
The Health and Care Bill currently going through Parliament:
- builds on existing non-statutory ICSs through the creation of ICBs and ICPs in each local area
- introduces a duty for the CQC to review how partners are working together within the areas of an ICB
- places a new duty on CQC to review how local authorities deliver certain adult social care functions, under part one of the Care Act 2014
- gives new powers to allow the Secretary of State for Health and Social Care to intervene in local authorities to secure improvement
- introduces new provisions to mandate information standards, along with new powers to collect information from providers.
The emerging approach to assessment
Our ambition is for CQC to use its powers and duties to help improve outcomes for people who draw on care and support by assessing how local authorities are meeting individual’s needs.
To make these assessments, they will need to look at a range of local authorities’ activities. Our initial thoughts, informed by working with the sector, are that assessments may look at some or all of the following, for example:
- maintaining oversight of the social care workforce in their local area, supporting staff retention and professional development
- managing transitions between services – for example, between health and social care, and the transition from children’s to adults’ services
- preventing people from requiring social care in the first instance – for example, by supporting and developing community organisations working on prevention and reablement
- carrying out their safeguarding duties
- ensuring good outcomes for people through effective leadership
- managing their commissioning and contracting responsibilities
- shaping the care market to meet people’s needs with diverse and quality provision, enabling choice and independence
- meeting the needs of unpaid carers
- assessing the needs of people who may be eligible for care and support them to access what they need, whether or not they receive local authority support or will fund their own care
It is our intention that the approach for assessments will be flexible enough to react to risks and changes in circumstances in an agile way. Assessments will be informed by a range of information and data, including insights gathered from discussions with local authorities and providers, as well as people who draw on care and unpaid carers, whose views and experiences will be central to CQC’s assessment approach.
CQC’s new strategic direction includes plans to assess local authorities, ICSs and providers using a new single assessment framework. This framework will build on the approach that is currently used to assess providers, and will also draw upon the ‘I’ statements used in Think Local Act Personal’s Making it Real framework as the basis for its single assessment framework, which seek to reflect the most important aspects of personalised, culturally appropriate care. For example:
I am treated with respect and dignity.
‘We’ statements will also be used to clarify what standards CQC expects. For example, for a local authority this might be:
We understand the health and care needs of individuals and local communities, so care provision is planned and delivered to ensure flexibility, choice and continuity of care.
As the CQC develops this framework, it will work collaboratively with Think Local Act Personal, National Voices and other stakeholders to design further statements to cover the whole range of its assessment framework.
We will also continue working with CQC and a wide range of stakeholders, including people who draw on care and support, local authorities and providers, to further refine our vision for the scope and methodology of assessments. This will include making sure the outcomes of assessments are presented clearly and accessibly, while minimising any burden on local authorities.
Following extensive collaboration, we expect that the CQC’s assessment of local authorities will launch no sooner than April 2023.
The Secretary of State for Health and Social Care will set out the priorities and objectives for the system to the CQC. The CQC will be required by legislation to publish the methods it will use to assess local authorities before assessments begin. We will lay secondary legislation in due course to specify which functions of local authorities, under part one of the Care Act 2014, will form the basis of assessments.
Improvement support and intervention
Local authorities and providers constantly strive to make care and support better, and we want to ensure the sector has the support it needs to achieve a genuine step change in people’s experiences of care.
We recognise that staff across the sector made phenomenal efforts during the COVID-19 pandemic, and we do not underestimate the challenge of building back better. We currently provide funding for improvement activity that is designed and delivered by sector partners. We know that the resources, training, expert advice and support provided to local authorities and providers, as well as the opportunities to collaborate through this offer, are valued by those who use them. Recognising the value of sector-led improvement, our approach remains to enable the sector to drive its own improvement.
To deliver our reform ambitions, we believe that we need to increase the scale and reach of the support offer available. We will increase improvement funding to over £70 million over the next 3 years to step up improvement activity across the sector, designing an offer that supports delivery of our reform ambitions in a way that has the greatest impact and meets local authorities’ needs.
We also intend to play a more proactive role in ensuring support is targeted where it is needed most, informed by data, intelligence, and the views and experience of people who draw on care and support, and their carers.
We want to build on the department’s regional assurance team, which was set up to work with local authorities during COVID-19. The valuable relationships developed in local areas – alongside access to more real-time data, such as those collected via the Vivaldi pilot[footnote 32] – have allowed us to build a better understanding of what is happening on the ground, improved our understanding of the care sector, and enabled us to quickly respond to emerging issues. We will continue to see the regional assurance team broaden their focus to understand how reform is being implemented and what is happening in practice.
The improvement offer
We know that a universal support offer that makes guidance, toolkits and resources, training and collaboration opportunities available to everyone is a crucial foundation for improvement. Local authorities, providers and the sector want to learn from the most up-to-date, evidence-based practice as it emerges.
We want to expand the universal offer to strengthen that proactive approach to self-improvement, making resources, materials and training opportunities available to everyone.
We will also include more bespoke support to help tackle particular problems that local authorities might be facing, such as the additional work on market-shaping and commissioning described above.
Through this bespoke offer, local authorities and other local partners will be able to request additional expert support to develop and apply universal tools that will help them on specific challenges they are facing. This will be delivered in partnership with the sector, tailored to local circumstances, and could include workshops and consultancy-style support. By providing this tailored support early, local authorities and others will drive their own improvement, and reduce the risk of the need for more intensive support later.
Bespoke support in action: Think Local Act Personal and Leicester City Council
Think Local Act Personal (TLAP) provided bespoke support to Leicester City Council to support them in changing the way services are designed. The council wanted services to be designed in partnership with people who draw on care and support, but found it difficult to secure engagement.
TLAP helped to build interest and enthusiasm for the project in the local area. Key to this was securing commitment from local leaders to meaningfully engage and provider resources that were needed to deliver. They ran a series of workshops with local people and council staff and facilitated honest, challenging conversations that helped the group find a productive way of working together.
The group, supported by TLAP, began to build trust by starting to make changes that, although small, had a real impact on people. Agreeing clear actions and following through on promises enabled the group to build momentum.
Feedback from the people involved, carers and local authority staff shows that this has transformed their relationship, facilitated genuine co-production, and delivered much more responsive and appropriate services. A local person said:
As a person who receives support, I have been proud to be part of this process. I have already seen the power the changes have had, how everyone feels better about the work they are doing and people are happier with the support they receive.
We will continue working with stakeholders in the coming months, including local authorities and providers, to develop our improvement offer, and will begin rolling out this offer during 2022 and 2023.
Local authorities struggling to meet their Care Act 2014 duties
Where improved data, intelligence from our regional team, and CQC’s assessment of a local authority’s performance identifies a serious and persistent risk to people’s safety and wellbeing, we want to take a more active role in supporting local authorities to improve.
Our priority will remain supporting local authorities to lead their own improvement wherever possible. In these circumstances, we will offer ‘directed support’, asking the local authority to produce and implement an improvement plan. Where the local authority demonstrates improvement, directed support may be withdrawn or tapered off.
We will work with the sector to design the directed support offer and monitoring arrangements to align with the launch of CQC’s assessment framework.
Statutory intervention
If a local authority has not been able to tackle sustained problems, we want to put in place a mechanism to escalate improvement.
The new powers in the Health and Care Bill will provide the Secretary of State for Health and Social Care with clear levers to intervene and address the most serious concerns in local authorities’ delivery of adult social care. We expect that the Secretary of State for Health and Social Care would only use these powers in exceptional circumstances, where the CQC has identified a serious and persistent risk to people’s safety, and where other forms of support are insufficient to drive improvement.
The Secretary of State has committed to consulting the Secretary of State for Levelling Up, Housing and Communities before taking a decision to use statutory powers, so that government can co-ordinate its approach to local authorities in the most worrying cases. Local authorities will have a legal right to make representations to the Secretary of State before any decision to use statutory intervention powers is made.
We will continue to work closely with the sector to develop the operational details of these intervention measures, and intend to publish operational guidance following passage of the Health and Care Bill.
These improvement and intervention measures recognise local authorities’ statutory roles and responsibilities underpinned by local democratic accountability. We know that the sector strives to ensure their local care and support offer enables local people to live the life they want and, through these measures, we will be able to better support them in achieving this.
Data
We have an ambitious vision for reform – but we do not currently have good enough data to know whether people are consistently getting the care they need. As we invest in reform, we need to tackle this data gap. At a local level, providers and commissioners of services need high-quality and timely data to commission and deliver services that meet the needs of their populations and improve the quality of care. Local authorities also need to manage local provider markets to provide choice and continuity of care.
The COVID-19 pandemic has brought into sharp focus the need for high-quality data and information to be shared and used well. Prior to the pandemic, we had no national source of data from providers on capacity, workforce status and numbers of people in receipt of care, and most data was captured through aggregate annual returns from local authorities. This data did not capture individuals who are privately funding their care or receiving unpaid care, and therefore they were almost entirely absent from our understanding of how the care system is operating.
While many bodies collect information like this, along with data at provider and local level, there is limited standardisation in how it is collated, shared and used, and how different collections sit alongside each other. We also know there are other data gaps, as highlighted by the Office for Statistics Regulation in their 2020 review of adult social care data.
Emergency data measures taken in response to COVID-19 have given us near real-time data to manage the pandemic, and shown us the benefits of using data to respond to emerging risks and issues. While there are lessons to be learned about the implementation of these measures, particularly around the collection and sharing of data, they have led to a step change in our understanding of how the system works and the sector-wide benefits that can accrue from increased data sharing.
In partnership with providers, local authorities and their partners, we will review current data collections and publications, ensuring they have a clear purpose and are proportionate, and fill remaining data gaps to ensure we have robust data flows. For the data that is collected, we want to ensure it is shared more widely so that those in the sector have the data and local intelligence needed to operate effectively and deliver improved outcomes for those receiving care and support.
The commitment to implement digital social care records over the next 3 years (see providing the right care in the right place at the right time will also benefit providers by enabling the automated collection of necessary data in a secure and transparent way, reducing the administrative burden on providing information and freeing up more time to care.
Over the next 3 years, we will implement the commitments outlined in the draft Data saves lives: reshaping health and social care with data strategy. We will continue to work with data providers, users and key stakeholders to agree data needs for local authorities, providers, regulators and people who need care and support and their carers.
Specifically, we will:
- establish an adult social care data framework by spring 2022, setting out what data the sector needs to collect, the purpose of those collections and the standards it is collected to. We will engage with the sector, including local authorities and providers, to develop the framework, which will set out how we will improve the quality of data and rationalise collections so that we minimise the collection burden
- update the Adult Social Care Outcomes Framework by autumn 2022, working with the sector to set out the indicators that will:
- enable local authorities to benchmark their performance against similar authorities
- provide a good national indication of performance to inform or direct CQC assessments
- provide local people with a simple mechanism to hold their local authorities to account
- over the next 3 years, increasingly move away from collecting aggregate data to using (anonymised) client-level data. This will bring social care collections more into line with person-level NHS collections, using the NHS number to enable data to be accurately and appropriately linked, and will address known data gaps, such as on personal outcomes, waiting times for assessments and services, and care hours provided. We will be able to link to health data sets, which will help us understand how people move between health and social care so that we can gain better insights into care outcomes, which interventions work best and how local system partners work together. We have begun to collect client-level data from local authorities through a voluntary collection process, with the intention of moving to a mandatory collection from April 2023
- agree a core provider data set for the sector with our partners (including the CQC), along with a means of collecting it that will minimise collection burdens. Providers will be able to use this data to support more effective and efficient delivery of care
- revise the Survey of Adult Carers in England and the Adult Social Care Survey, broadening their reach and refreshing the collection mechanisms. This will ensure both surveys are fully representative of the social care population (as defined in the Care Act 2014). Initial work is underway to develop the surveys with a full timetable for implementation to be set out following completion of the discovery phase by spring 2022
- develop an easily accessible data-sharing solution with local authorities and providers that supports real-time decision-making at local, regional and national levels. To manage the pandemic, we developed an adult social care COVID-19 dashboard using data from providers, which is viewed by local authorities in real time, at national, regional and local levels. A new data-sharing solution will build on the lessons learned from the pandemic and seek to ensure different actors in the system have access to the same rich data sets over the next 3 years
- continue to invest in undertaking research and evidence gathering that will inform our developing policies over the next 3 years and evaluate our reforms to see that they are delivering as intended so policies can continue to evolve
- work with partners to co-design a suite of standards for social care to support and underpin the data specification and interoperability requirements for a wide range of system-wide programmes. This will support uptake of interoperable care technology that can provide information flows to enable smarter planning
We want to maximise the use of technology and use data intelligently to support commissioning and delivery of high-quality services, while minimising collection burdens. These proposals are fundamentally linked to the support we will offer providers to digitise and agree data architecture standards that will make data-sharing between providers, local authorities, health bodies and national organisations easier, as outlined in the earlier chapter providing the right care in the right place at the right time.
Access to care
Local authorities are responsible for assessing an individual’s eligibility for care and support and, where the individual is eligible for financial support, for meeting those needs. Where individuals are not eligible for financial support, local authorities will support them, should they require assistance, to make their own arrangements for care services.[footnote 33]
There is a lack of data and evidence on the extent to which care needs are not being met. Estimates of unmet and under-met need vary considerably depending on the definition used. For example, definitions that include people with lower-level or one-off needs are significantly higher than a definition more closely aligned to that established by the Care Act 2014. There is also limited evidence on the drivers of unmet need, but we know these can be broad, from a lack of awareness of entitlement and options to not wanting to ask for more help or a lack of confidence to ask for help. Truly tackling issues around access to care requires an understanding of the extent to which the various drivers apply and what works in addressing them.
We believe that better-quality data, including client-level data, will help us to:
- understand more about who accesses care, how and with what impact
- better understand who is not accessing care
- better understand how much barriers or choices (or a mix of both) may be a cause of this
Where we go from here
People at the Heart of Care is an ambitious 10-year vision for adult social care. We have some way to go to make this vision a reality, but existing legislation provides a strong foundation, and measures in the Health and Care Bill will complement this.
Over the next 3 years, the policies outlined in this white paper will take us further on our reform journey.
This white paper has been informed by voices across social care, including unpaid carers, and people who draw on care and support. Over the past year, we have spoken to over 200 organisations large and small across England, and we are immensely grateful to all of them for their contribution.
Annex A outlines in more detail the far-reaching engagement programme we have undertaken.
Next steps
The measures we have announced will bring tangible benefit to the lives of people who draw on care and support, their families, and their carers – moving us towards our 10-year vision of person-centred care where people:
- are offered choice, control and support to lead an independent life
- can access outstanding-quality care and tailored support
- find adult social care fair and accessible
But social care reform is a shared endeavour. To deliver the bold measures in this white paper, we must involve people and organisations across the sector. Therefore, we will:
- work in partnership with stakeholders and people who draw on care and support to develop and design the implementation of the measures set out in this white paper
- explore with local authorities and other key stakeholders how best to deliver the numerous investments outlined in this document, which are funded by the new Health and Social Care Levy. We want to ensure the investments meet their intended objectives while also making it as simple as possible for local authorities and others to access the new funding
- engage with a diverse range of voices across the sector, including those who draw on care and support, to identify measures of success for the delivery of our reforms
- collaborate with TLAP and members of the Health and Wellbeing Alliance to set up co-productive forums to ensure that the voices of those who draw upon care and support are involved in the ongoing design and implementation of social care reform
We will work with local authorities, housing providers and others to agree how we will target our new investment in housing and to design our new Innovative Models of Care programme, which will support local places to bring proven innovations from the margins to the mainstream.
We will be consulting on the detail of the changes to the upper limit for the DFG, and we will be working with partners across the housing sector and wider to better understand the opportunities to drive more choice for older people’s housing.
To deliver our ambitious digital transformation programme, we will continue to work closely with our key partners and people with experience of health and care services over the coming months. We will publish a social care technology blueprint, as well as developing advice on ‘what good looks like’ for social care technology, to help everyone involved in the provision of care understand what they should be aiming for.
To improve information and advice, we will take the lessons learned from our research, testing of new ideas, and increased oversight of local authority offerings to develop and refine further policy proposals over the longer term. This could include a focus on reducing any fragmentation of information and advice services, in line with wider changes on integration, or on upskilling and educating health and social care professionals to ensure consistency in what those looking for care and support and their families are told.
On unpaid carers, our immediate focus will be on working towards the development of the new funded proposals. Taking an evidence-driven approach, we will target a range of projects on a ‘test-and-learn’ basis. We will develop the focus with carer organisations, carers, commissioners, academics and others in the sector to ensure we learn from the most effective ways to support carers, for example, through new multi-dimensional support models. We will set up a series of workshops with stakeholders to inform the development and direction of the funding in early 2022.
As the needs of those who draw on support and the models for providing care evolve over time, we need to ensure the workforce evolves too. Our strategy for the workforce will require national government to work alongside local sectors in partnership now and in the future. We will co-develop our new career pathways, national KSF, investment in training opportunities and policies on wellbeing, occupational health and recruitment. In the longer-term, we will work with local areas as they build on this foundation to establish profound and lasting change for adult social care careers.
The measures outlined later in this document will provide greater information on how care is being delivered and the impact of our reforms. We will use this information to inform and regularly assess our improvement support function to ensure it is targeting the areas where it is needed most. Importantly, we will have improved capability and capacity to support a partnership approach to market-shaping and commissioning, leading to an increase in the diversity of care and support options available for people who drawn on care and support. These measures will help accelerate the adoption of the proposals outlined in providing the right care in the right place at the right time and empowering those who draw on care, unpaid carers and families.
Finally, a challenge for both the public and the adult social care sector is that, as a society, we do not tend to think about or plan for care and support needs that may arise in older age. The cap on care costs will mean that people no longer face unpredictable or unlimited care costs and make it easier to plan financially. And, over the next 10 years, we want to start working across government to encourage people to think ahead about the life they would like to live in older age.
We also want to support groups drawing on care and support
The government is committed to delivering a standalone dementia strategy in 2022. The strategy will focus on the specific health and care needs of people living with dementia and their carers, including looking at:
- dementia diagnosis
- risk reduction
- prevention
- research
This white paper also makes a crucial contribution to our plans to transform the provision of community mental health support for people living with severe mental illnesses and complex needs in the NHS Long Term Plan.
This, in turn, is key to realising our ambitions set out in the recent Reforming the Mental Health Act white paper to deliver a modern mental health service that respects people’s voice, and gives them choice over their care and treatment under the Mental Health Act 1983. The reforms will ensure that care under the act is given in the least restrictive setting, and people are supported to be discharged from the act and live independently at home where possible.
In addition, people at risk of and experiencing homelessness often have a combination of needs and encounter a range of public services, including:
- housing
- health and social care
- drug and alcohol treatment
- the criminal justice system
We will therefore continue to work with the Department for Levelling Up, Housing and Communities and other key stakeholders to ensure that health and care needs are met, and to support our manifesto commitment to end rough sleeping by 2024.
Monitoring and evaluation
In supporting local authorities to deliver social care reform and our vision, we discussed the importance of good data for ensuring adult social care is operating effectively and meeting the needs of those within in it.
To ensure our reforms have reached their intended aims and are making progress towards the vision set out, it will be crucial to devise a robust monitoring and evaluation process. This is especially important given the complexity of the reforms being implemented and the scale of anticipated costs. These reforms present a significant opportunity to learn lessons about what works – several of our proposals have been established explicitly to test new and innovative ways of delivering support, with monitoring and evaluation fundamental to these plans.
We are in the process of developing an overarching evaluation framework, which will seek to:
- monitor and appraise the delivery of individual policies – where appropriate, to facilitate learning to inform future phases of delivery
- provide evidence of specific outputs and emerging outcomes linked to individual policies. Due to the heterogeneity of the policies implemented, it is likely that a variety of methodological approaches will be adopted
- going beyond individual policy-level evaluation, monitor the success of the overall programme of reform. The specific contribution of individual policies to successful overall reform will be difficult to isolate, but we will seek to outline the causal mechanisms through which policies are expected to lead to reform outcomes.
To inform monitoring and evaluation plans, we have developed a logic map (see figure 3 below) that shows how a combination of our underpinning policies and our reform policies will complement each other and deliver a range of intermediate outcomes.
For example, the underpinning policy of sustainable long term funding and adequate resourcing for local government combined with reform policies for improved data channels and technology, new models of care and housing funding is expected to result in a resilient provider market that encourages competition, incentivises innovation, and serves the needs of local populations.
Underpinning policy
- greater assurance of local authorities, for example through the Health and Care Bill
- sustainable long term funding and adequate resourcing for local government
- robust market oversight and assurance
Reform policy
- improved data channels
- technology funding, new models of care, housing and so on
- policies to improve consumer transparency
- more support for unpaid carer
- workforce training and development
Intermediate outcomes
- greater transparency and more informed consumers
- more collaboration between councils, providers, central government and so on
- ensure local authorities pay providers a fair rate of care
- a resilient provider market that encourages competition, incentivises innovation, and serves the needs of local populations
- “world class” market shaping and commissioning
- improved workforce capacity and capability, with better reward and retention
Over the longer term these policies are expected to support a social care system that fits our long-term vision that:
- every person finds adult social care fair and accessible
- a more sustainable, affordable care system that effectively works with other public services
- every person who is provided has choice, control, and support to live independent
- every person can access outstanding quality and tailored care and support
Figure 3: Logic map showing how policies relate to expected reform outcomes

We will develop the evaluation framework to ensure it meets the above objectives and we will build in flexibility so that it aligns with policy implementation.
As part of this planning process, we will consider whether – and to what extent – it would be appropriate to involve external organisations in delivering the monitoring and evaluation.
We will engage with stakeholders to refine monitoring and evaluation plans, and more detail on the approach will be published in due course.
Annex A: engagement on this white paper
Since March 2021, the department has been engaging extensively to shape the government’s vision and priorities for adult social care system reform. We have worked with over 200 organisations to shape the content of People at the Heart of Care, including representatives from:
- local government
- providers
- provider representative bodies
- workforce representatives
- trade unions
- charities
- think tanks
- professional bodies
- lived experience representative groups
- those with lived experience of delivering unpaid care, and drawing on care and support
Our engagement programme
Our far-reaching engagement programme this year has included, but is not limited to:
- bilateral discussions, beginning in March 2021, with disabled people’s organisations and lived experience representative groups
- an initial sequence of roundtables in April 2021, engaging over 70 national stakeholders to inform the shape of the vision and outline priorities for change
- a themed series of workshops in June 2021 involving over 90 national stakeholders to address 4 specific questions on reform that emerged from the first series – this included:
- integration
- market shaping
- workforce strategy
- new models of care, technology and innovation
- in-depth workshops across all regions in England in August 2021, to engage with a diverse range of local stakeholders including providers, local authorities, local charities and support groups, as well as people who draw on care and support. Local engagement recognised that social care is felt differently across England and reform priorities differ accordingly. Further workshops in August also took place in collaboration with Carers UK and Social Care Futures to hear from unpaid carers and those who draw on care and support
- following the publication of Build Back Better: Our Plan for Health and Social Care on 7 September 2021, we have intensified our work with the sector to shape this white paper, as the next step on the reform journey, by:
- setting up advisory groups of diverse stakeholders for each theme of the paper including assurance, unpaid carers, technology, market shaping, workforce, models of care, housing, and information and advice
- working with TLAP and members of the Health and Wellbeing Alliance to ensure that our approach to reform is informed by voices of those who draw on care and support
- arranging detailed workshops with over 60 organisations and individuals across all regions in England to discuss choice control and independence, outstanding quality, and fairness and accessibility as the core pillars of our vision for reform
- supporting and collaborating to deliver workshops on specific audiences of reform including with a range of working-age adult charities, providers, unpaid carers and local authorities.
- working closely with stakeholders to refine the language used in People at the Heart of Care
Acknowledgements
We thank the following organisations for engaging with us over the past year on social care reform:
- Ace Anglia
- Active Independence
- Active Prospects
- Age UK
- Age UK East London
- Age UK Gateshead
- Age UK Leicester Shire & Rutland
- Alzheimer’s Society
- Anchor
- Archbishops’ Commission on Reimagining Care
- Associated Retirement Community Operators
- Association of County Council Chief Executives
- ADASS
- Association of Directors of Public Health
- Association of Mental Health Providers
- Autism Bedfordshire
- Autistica
- Barchester Healthcare
- BelleVie Care
- Bespoke Consultancy and Education Ltd
- Bracknell Forest Council
- Bradford Metropolitan District Council
- Bristol City Council
- British Association of Social Workers
- British Institute of Learning Disabilities
- Brunelcare
- Buckinghamshire Council
- Bupa
- Calderdale Council
- Cambridgeshire County Council
- Camden Council
- Care and Repair England
- Care and Support West
- Care Association Alliance
- Care England
- Care Provider Alliance
- Care Quality Commission
- Carers First
- Carers Trust
- Carers UK
- Caring Together
- Central Bedfordshire Council
- Centre for Ageing Better
- Centre for Mental Health
- Chartered Institute of Housing
- Cheshire West and Chester Council
- City and County Healthcare Group
- Collaborative Newcastle
- Community Catalysts
- Community Integrated Care
- County Councils Network
- Court House Care
- Coventry City Council
- Cumbria County Council
- Demos
- Derby City Council
- Developing Health and Independence
- Devon Care Homes Collaborative
- Dimensions
- Disability North
- Disability Resource Centre
- Disability Rights UK
- Doris Jones
- Durham County Council
- Ealing Council
- East Sussex County Council
- Elderly Accommodation Counsel
- EMCARE
- Enthuse
- Epilepsy Action
- FaithAction
- Fosse Healthcare
- Four Seasons Health Care
- Getta Life
- Golden Lane Housing
- Good Things Foundation
- Grapevine
- Greater London Authority
- Greater Manchester Coalition of Disabled People
- Greater Manchester Housing Providers
- Hartlepool Borough Council
- HASCA Ltd
- Haven Care
- Havering Care Homes
- HC-One
- Healthwatch
- Healthwatch Cheshire
- Healthwatch Dorset
- Healthwatch Worcestershire
- Helping Hands Home Care
- Herefordshire Care Homes
- Hertfordshire Care Providers Association
- Hertfordshire County Council
- Hightown
- Home Group
- Home Instead
- Homecare Association
- Homeless Link
- Housing Learning and Improvement Network
- Inclusion East
- Independent Care Group
- Independent Lives
- Institute for Fiscal Studies
- Institute for Public Policy Research
- Isle of Wight Council
- Kent County Council
- Kirklees Council
- Landermeads
- Learning Disability England
- Leeds City Council
- Legal and General
- Leicester City Council
- Leicestershire Homecare Alliance
- Leonard Cheshire
- LGBT Consortium
- LGBT Foundation
- Living Longer Better
- Local Government and Social Care Ombudsman
- Local Government Association
- Locality
- London Councils
- Longfield Hospice
- MacIntyre
- Manchester City Council
- McCarthy & Stone
- Mencap
- MHA
- Mind
- Motor Neurone Disease Association
- Multiple Sclerosis Society of Great Britain
- National Association of Care and Support Workers
- National Association of Financial Assessment Officers
- National Autistic Society
- National Care Association
- National Care Forum
- National Co-production Advisory Group
- National Development Team For Inclusion
- National Housing Federation
- National Innovation Centre for Ageing
- New Local
- Newcastle Carers
- Newcastle City Council
- Newton Europe
- Norfolk Local Authority
- North West ADASS
- Northamptonshire Carers Association
- Northumberland County Council
- Nottinghamshire Care Home Association
- Nottinghamshire County Council
- Oakdown House Ltd
- Oxfordshire Association of Care Providers
- Oxfordshire County Council
- Palliative and End of Life Care Strategic Clinical Network
- Parkinson’s UK
- Policy Connect
- Policy Exchange
- Power to Change
- Principal Social Workers Network
- Race Equality Foundation
- Reclaiming Our Futures Alliance
- Registered Nursing Home Association
- Renaissance Care
- Resolution Foundation
- Resonance
- Rethink Mental Illness
- Right at Home
- Royal Borough of Kingston upon Thames
- Royal College of Occupational Therapists
- Salford Integrated Care Organisation
- Sefton Council
- Self Directed Futures
- Sense
- Share and Care Homeshare
- Shared Lives Plus
- Sheffield Mencap & Gateway
- Shropshire Partners in Care
- Skills for Care
- Skills for Care London
- Skills for Care Midlands
- Skills for Care South West
- Slough Borough Council
- Social Care Future
- Social Care Institute for Excellence
- Social Enterprise UK
- Solace
- Solihull Action through Advocacy
- Solihull Metropolitan Borough Council
- Somerset County Council
- Somerset Sight
- Sortified
- South East Care Association
- Southampton Voluntary Services
- Southend-on-Sea Borough Council
- St Margaret’s Hospice
- Staffordshire County Council
- Stockton-on-Tees Borough Council
- Storyboard Consulting Ltd
- Suffolk Association of Independent Care Providers
- Supporting Adult Social Care Innovation research group (London School of Economics)
- Surrey County Council
- Sussex Community NHS Foundation Trust
- Swindon Borough Council
- Swindon Carers Centre
- Technology Enabled Care Services Association
- Telford & Wrekin Council
- The Care Workers’ Charity
- The Children’s Society
- The Council of St Monica Trust
- The Health Foundation
- The King’s Fund
- The Nuffield Trust
- The Orders of St Johns Care Trust
- The Queen’s Nursing Institute
- Thera Trust
- Think Local Act Personal
- Together in Dementia Everyday
- Together All Are Able
- UK Research and Innovation
- UNISON
- UNISON North West
- Valorum Care Group
- VOICE
- VoiceAbility
- Voluntary Organisations Disability Group
- Walnut Care Limited
- Welcome Independent Living
- West Midlands ADASS
- West Midlands Care Association
- West Sussex County Council
- West Yorkshire and Harrogate Health and Care Partnership
- WHM Work Connections
- Wiltshire Centre For Independent Living
Annex B: carers action plan 2018 to 2020
As mentioned in empowering those who draw on care, unpaid carers and families, in June 2018 the government published its cross-government carers action plan to increase identification, recognition and support for unpaid carers.
It was an essential step towards realising the government’s commitment to valuing, recognising and supporting unpaid carers to provide care in a way that supports their own health and wellbeing, and life choices such as education and employment.
The carers action plan was informed by a call for evidence, which provided a rich and informative evidence base on the experiences of carers and the changes that they would like to see.
The carers action plan set out the government’s commitment to supporting carers through 64 actions across the following 5 priorities:
- Services and systems that work for carers.
- Employment and financial wellbeing.
- Supporting young carers.
- Recognising and supporting carers in the wider community and society.
- Building evidence and research to improve outcomes for carers.
Within the first year of the carers action plan, good progress had been made towards fulfilling its commitments and, in July 2019, we published the carers action plan: 1-year progress review.
The work on the carers action plan came to an end in December 2020. Below are some of its key achievements.
Services and systems that work for carers
Action 1.1
NHS England’s general practice quality markers offer practical ideas that have been developed in partnership with carers, primary care teams and other key stakeholders. Collectively, these provide a framework for general practice to improve how it can better identify and support carers of all ages.
Action 1.7
Health Education England has developed a suite of Supporting Unpaid Carers learning resources that help carers to look after themselves as well as providing information that can help them in their caring role.
Action 1.13
SCIE’s good practice guides on commissioning short breaks for carers of all ages and young carers.
Action 1.14
Preparing for adult life – these pages bring together information about key aspects of the transition from child to adult support services for families with disabled children.
Employment and financial wellbeing
Action 2.1
Employers for Carers’ Carer Confident benchmarking scheme for employers. The 3-level scheme is designed to support employers towards building a supportive and inclusive workplace for all staff who are, or who will, become carers.
Action 2.3
The BEIS’s response to the consultation on carer’s leave, which confirms the intention to deliver on the government’s manifesto commitment to introduce a new entitlement to one week of leave for unpaid carers.
Action 2.8
Timewise Foundation’s flexible jobs hub, which, according to Timewise, has featured over 44,000 flexible jobs for carers since the hub was launched in 2018.
Action 2.14
The Government Equalities Office’s best practice guidance and toolkit for employers has provided opportunities for those who have been out of work for caring responsibilities. In addition, the Government Equalities Office has launched a dedicated return to work webpage featuring practical guidance for employers and returners. This includes a toolkit for returners as well as infographics for returners and employers.
Supporting young carers
Action 3.2
Carers Trust and the National Centre for Social Research published a good practice resource aimed at local government and others to help ensure timely identification and access to support of young carers.
Action 3.9
The Children’s Society’s Shaping our future: Improving Assessment and Support for young carers Transition into Adulthood’ report on supporting young carers transition into adulthood. Alongside this, they published a tool to help professionals support young carers and a guide for young adult carers to help them through the transition period.
Recognising and supporting carers in the wider community and society
Action 4.2
The Carers’ Tech Toolkit continues to get significant interest from professionals who are keen to understand how technology can improve the quality of care they provide and reduce the burden on carers, and from suppliers keen to ensure their technology meets the priority requirements of carers.
Action 4.5
Carers UK together with Carers Trust established a Carer Passport scheme to increase the recognition of carers. This included the development and promotion of a toolkit, and resources for local organisations and others to develop their own Carer Passport offer.
Building evidence and research to improve outcomes for carers
Action 5.3
Additional questions for the Health Survey for England 2019 on providing care to family and friends to help improve the evidence base for future-proofing unpaid carers policies.
Action 5.6
The establishment of the Carer-Related Research and Evidence Exchange Network which now has worldwide recognition as a source of information and evidence about carers and carer practice, policy and innovation work and continues to be an evolving evidence exchange of information-sharing.
The exchange has enabled those across the globe to access carer-related knowledge, in the form of research evidence, and information about practice and policy.
-
Social care is devolved in Wales, Scotland and Northern Ireland. ↩
-
Encompassing those in receipt of formal and informal care, the workforce, and unpaid carers. ↩
-
NHS Digital, Adult Social Care Activity and Finance Report, England – 2020-21, published October 2021. ↩ ↩2 ↩3 ↩4
-
Office for National Statistics, Employment in the UK: September 2021, published September 2021. ↩
-
At the time of the 2011 Census, there were over 5.4 million people providing unpaid care in England. The 2021 Census will provide an updated count of the number of people providing unpaid care in England. ↩
-
Office for National Statistics, National population projections: 2018 based, published October 2019. ↩
-
Livingston, G, Huntley, J, Sommerlad, A, et al, Dementia prevention, intervention, and care: 2020 report of the Lancet Commission, published July 2020. ↩
-
Competition and Markets Authority, Care homes market study: Final report, published November 2017. ↩
-
Department of Health and Social Care analysis of Care Quality Commission, Care Directory with Filters, published November 2021. ↩
-
Skills for Care, The State of the Adult Social Care Sector and Workforce in England, published October 2021. ↩ ↩2
-
Office for National Statistics, Depression and anxiety among adults in selected care occupations: Great Britain, published February 2018. ↩
-
Social Care Workforce Research Unit, Kings College London, Moriarty, J, Manthorpe, J, Harris, J, Recruitment and retention in adult social care services, published 2018. ↩
-
Ipsos MORI, State of the State 2017–2018, published October 2017 ↩
-
Forthcoming Ipsos MORI, Institute of Public Care and Skills for Care, NHSX Adult Social Care Technology Innovation and Digital Skills Review. ↩ ↩2
-
Ministry of Housing, Communities and Local Government, English Housing Survey 2019-20: home adaptations, published July 2021. ↩
-
ADASS, Adult Social Care – Shaping a Better Future: Nine Statements to Help Shape Adult Social Care Reform, published July 2020. ↩
-
Personal Social Services Research Unit, Wittenberg, R, Hu, Bo, Projected demand for supported housing in Great Britain 2015 to 2030, published March 2017. ↩
-
ARCO, The Housing-with-Care Task Force overview, published 2020. ↩
-
TSA, Sector Insight Report, published July 2020. ↩
-
In shared lives, an adult or young person who needs long-term support is matched with a carefully approved shared lives carer. Together, they share family and community life. Half of the circa 15,000 people using shared lives move in with their chosen shared lives carer to live as part of their household and half visit for day support or overnight breaks. People get safe, personal support and care in a place that feels like home. ↩
-
Brown, L, et al, Life in lockdown: A telephone survey to investigate the impact of COVID-19 lockdown measures on the lives of older people (greater than or equal to 75 years), Age and Ageing 2021: volume 50, issue 2, pages 341-346 36, published November 2020. ↩
-
Fancourt, D, et al, Psychological response and behaviours during lockdown, COVID-19 Social Study, published 2021. ↩
-
Sport England, Active Lives Adult Survey November 2019-20, published April 2021. ↩
-
Age UK, Impact of COVID-19 on older people’s mental and physical health: one year on, published 2021. ↩
-
Care Policy and Evaluation Centre, National Institute for Health Research Workforce Research Unit, London School of Economics, Fernandez, J-L, et al, Supporting carers following the implementation of the Care Act 2014: eligibility, support and prevention as part of the Carers in Adult Social Care study, published 2020. ↩
-
There is a distinction between ‘information’ and ‘advice’. By information, we mean material supplied that could explain entitlements, processes or services. By advice, we mean the guidance offered to someone to explain the information relevant to their circumstances that allows entitlements or services to be accessed. ↩
-
HertsHelp in Hertfordshire provide both a community and hospital navigation service. Community navigators help people to identify and access community support that will help people to maintain their independence, health and wellbeing. Hospital navigators offer information, advice and practical support to help people get home safely and get the support they need. In Grimsby, Rethink Mental Illness have been trialling the use of a Mental Health Navigator to improve the community support for people severely affected by mental illness. The navigator can provide support with money issues, employment, housing, physical health or social connections within the community. ↩
-
NHS Digital, Health Survey for England 2019, published December 2020. ↩ ↩2
-
Schoenmakers, B, Buntinx, F, Delepeleire, J, Factors determining the impact of care-giving on caregivers of elderly patients with dementia: a systematic literature review, Maturitas, 66(2), pages 191–200, published March 2010. ↩
-
Greenwood, N, Habibi, R, Smith, R, Manthorpe, J, Barriers to access and minority ethnic carers’ satisfaction with social care services in the community: a systematic review of qualitative and quantitative literature, published August 2014. ↩
-
Carers UK, ‘The world shrinks: carer loneliness research report‘, published 2017. ↩
-
The Vivaldi study was set up to understand the factors influencing high mortality in care homes during the COVID-19 pandemic. The study has developed data infrastructure for health surveillance and research in adult social care by linking testing data to routine data sets. It has provided crucial insights to inform the government’s pandemic response in social care on infection, vaccination and immunity. ↩
-
According to the Adult Social Care Activity and Finance Report, England – 2020 to 2021, of the 1.9 million requests for support in 2020 to 2021, 0.5 million resulted in ‘universal services or signposting to other services’. ‘Universal services’ are defined as any service or support for which national eligibility criteria (following the Care Act 2014) are not relevant. It includes the provision of information and advice. ‘Signposting’ indicates that the client will not be supported by the local authority and there is no universal service that will help them. Details are therefore given of other organisations (for example, in the voluntary sector) that might be able to provide assistance. ↩
