Health matters: reducing health inequalities in mental illness
Published 18 December 2018
Summary
People with severe and enduring mental illness are at greater risk of poor physical health and reduced life expectancy compared to the general population.
This edition of Health matters sets out the scale of the problem and presents actions that local areas can take to reduce health inequalities, improve physical health and life chances of people living with mental illness.
Although the focus is on adults with more severe and enduring mental illness, many of the actions will be of benefit to all people experiencing mental illness.
Scale of the problem
Mental health problems can affect anyone and have a significant effect on the lives of individuals, their families, communities and wider society. Together with substance misuse, mental illness accounts for 21.3% of the total morbidity burden in England.
One in six of adults have had a common mental health disorder, such as anxiety, in the last week, according to survey data. Three quarters of mental health problems are established by the age of 24. Recent data indicates that there are close to 551,000 people in England with more severe mental illness (SMI) such as schizophrenia or bipolar disorder. This is likely to be an underestimate as figures only include those who are diagnosed and recorded on GP registers.

Mental health in numbers
Mental illness is closely associated with many forms of inequalities. Health inequalities are avoidable and unfair differences in health status and determinants between groups of people due to demographic, socioeconomic, geographical and other factors.
These differences can be in relation to prevalence, access to, experience and quality of care and support, as well as opportunities and outcomes. Health inequalities can mean reduced quality of life, poorer health outcomes and early death for many people.
People living with SMI experience some of the worst inequalities, with a life expectancy of up to 20 years less than the general population. This is the same life expectancy that the general population experienced in the 1950s, and evidence suggests that the mortality gap is widening.
Economic cost to society
Poor mental health is estimated to carry an economic and social cost of £105 billion a year in England. This includes indirect costs of lost employment, as well as direct costs relating to health and care provision and the human costs of reduced quality of life.
The long-term costs of perinatal depression, anxiety and psychosis collectively are estimated to be around £8.1 billion for the total number of babies born in a year. Most of this cost relates to adverse impacts on the child rather than the mother.
Inequalities experienced by people with mental illness
What drives inequalities in health?
Inequalities in health are largely due to inequalities in society, meaning the conditions in which people are born, grow, live, work and age. It is the unequal distribution of the social determinants of health, such as education, housing and employment, which drives inequalities in physical and mental health, although the mechanisms by which this happens can be complex and inter-related.
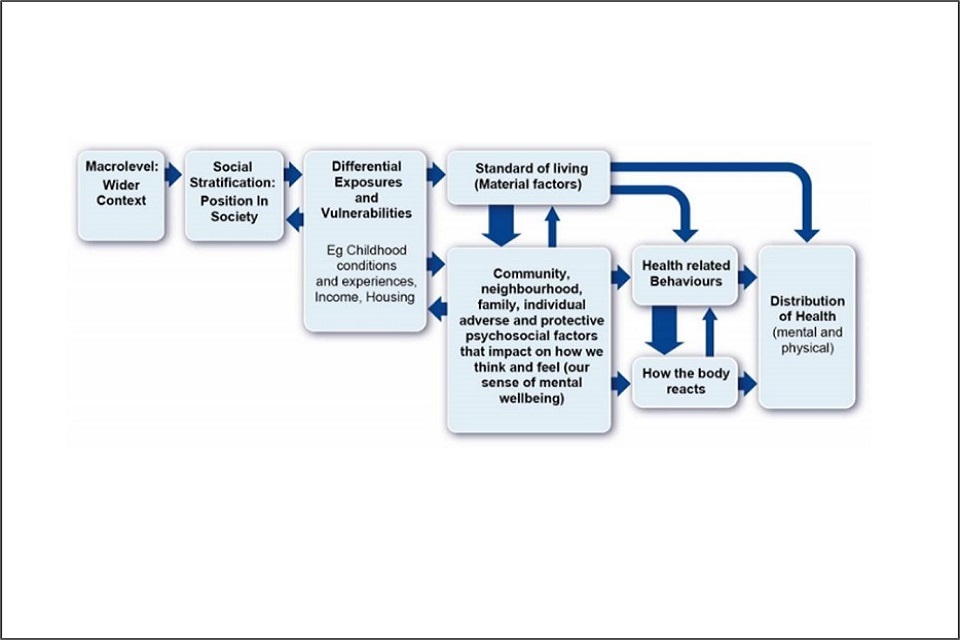
Infographic showing psychosocial pathways
Disadvantage can start even before a child is born, and can accumulate over time and impact on future generations.
Factors include:
- adverse childhood events such as being a victim of abuse
- poor housing
- poverty
- traumatic events
- poor working conditions
Children facing multiple risks have a heightened risk of multiple and sustained childhood mental health difficulties.
Protective factors such as social support and good quality of work and employment conditions can help buffer the impact of adverse conditions on poor health.
Social inequalities
People with mental illness are more likely to have higher rates of:
- poverty
- homelessness
- incarceration
- social isolation
- unemployment
As an example, psychosis is up to 15 times higher among people who are homeless compared to the general population.
Levels of psychotic disorders are 9 times higher in people in the lowest fifth (quintile) of household income compared to the highest.

Infographic illustrating social inequalities and mental illness
People with severe mental illness are also more likely to live in less safe neighbourhoods, have less access to healthy foods and fewer opportunities to be involved in healthy activities.
Stable, good quality and rewarding employment is protective for health and can be a vital element of recovery from mental health problems. Yet challenges remain for people with mental health problems in gaining and maintaining employment; sometimes because of negative attitudes and stigma. They are also often over-represented in low-pay and temporary work.
Many people want to work but are not always offered opportunities to do so or the most effective help when they do ask for it. The 2018 National Clinical Audit of Psychosis identified that less than half (46%) of patients who were unemployed and seeking work were receiving some form of support towards this goal.
Improving lives: the future of work, health and disability sets out the government’s plans to transform employment prospects for disabled people and those with long-term health conditions over the next 10 years. This includes an NHS England ambition to double national access to Individual Placement and Support (IPS) services by 2020 to 2021, allowing more people who experience SMI to find and retain employment.
Stable and appropriate housing is another important part of the recovery pathway and can reduce the need for inpatient care. People with mental health problems can experience significant barriers to accessing appropriate accommodation including stigma, discrimination, poverty as well as limited supply. Just over half (54%) of working-age adults in contact with secondary mental health services on the Care Programme Approach are living independently, with or without support.
Citizens Advice report that a growing number of people with mental health problems are turning to them for advice for social issues and that their needs tend to be more complex and urgent.
The main advice areas include finances and debt, essential services, housing, employment and the welfare system.
Having a practical problem can impact on a person’s ability to manage their health and lead to worsening mental health. The report calls for essential service providers, local authorities, landlords and employers to do more to support people with mental health problems effectively.

Infographic showing people with mental health problems have more practical problems
Physical health inequalities
Compared to the general population, people with mental illness experience a greater burden of physical health conditions. It is estimated that for people with SMI, 2 in 3 deaths are due to physical illnesses such as cardiovascular disease (CVD) and can be prevented.
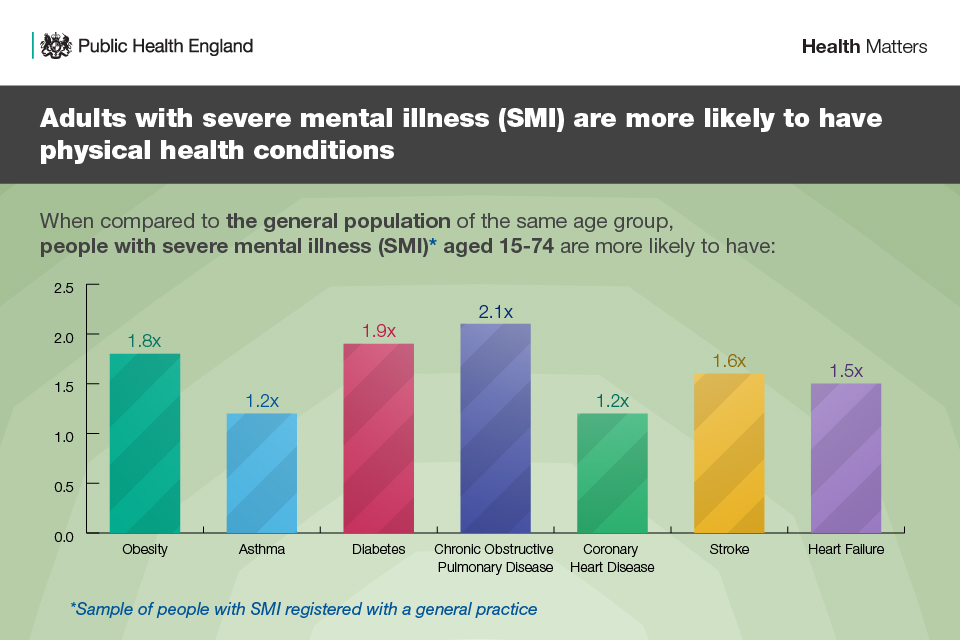
Infographic showing adults with mental illness more likely to have physical health probs
This increased burden of physical health problems affects all ages. Recent analysis by PHE found that younger adults with SMI are 5 times more likely to have 3 or more physical health conditions compared to younger adults overall.
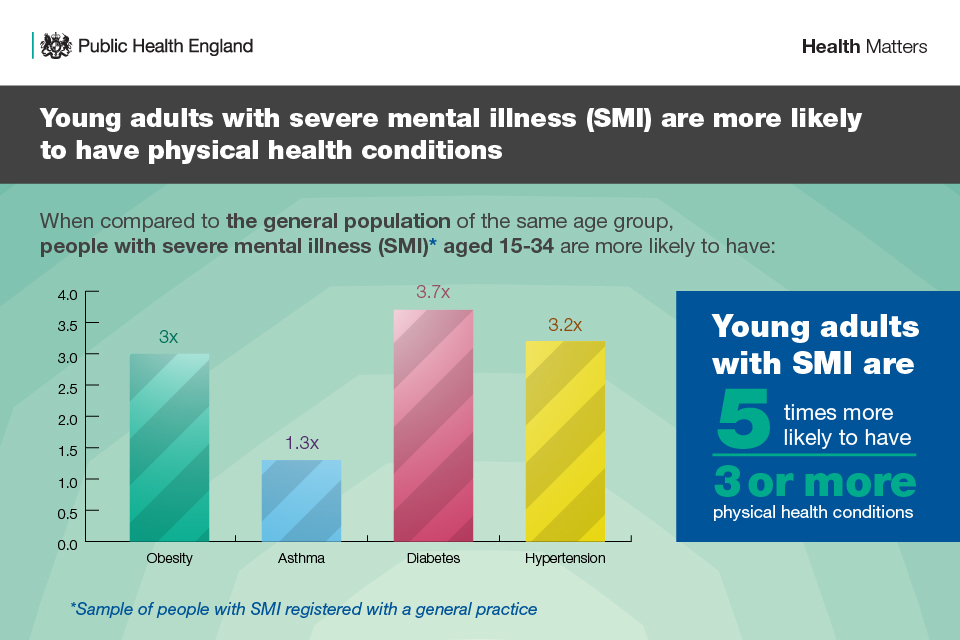
Infographic showing physical health problems linked with SMI in young adults
Those living in more deprived areas are likely to have a higher prevalence of physical health conditions.
Excess premature mortality rates are more than 3 times higher amongst people with mental illness in England compared to the general population.
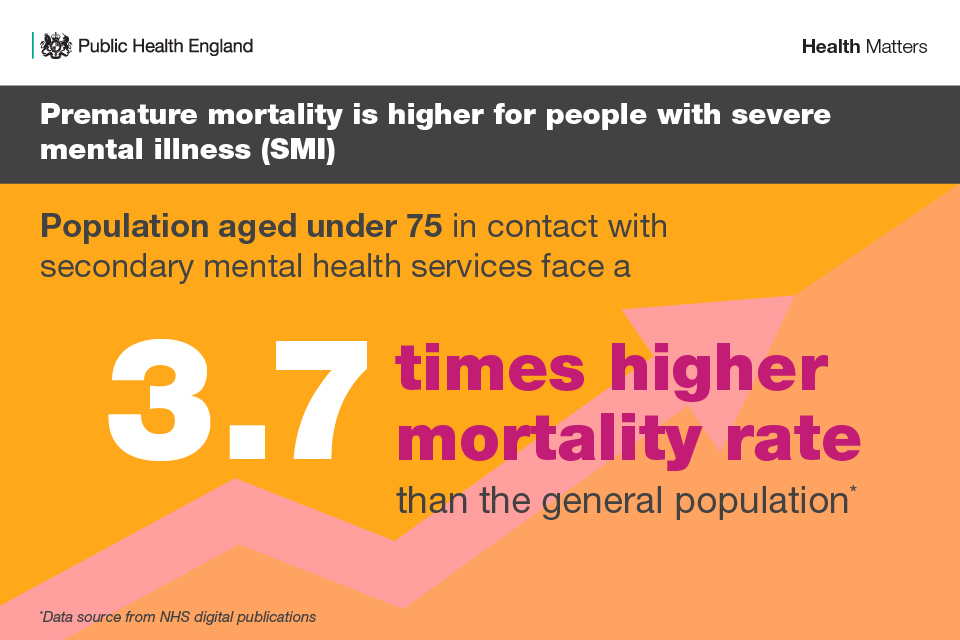
Infographic illustraing premature mortality in people with severe mental illness
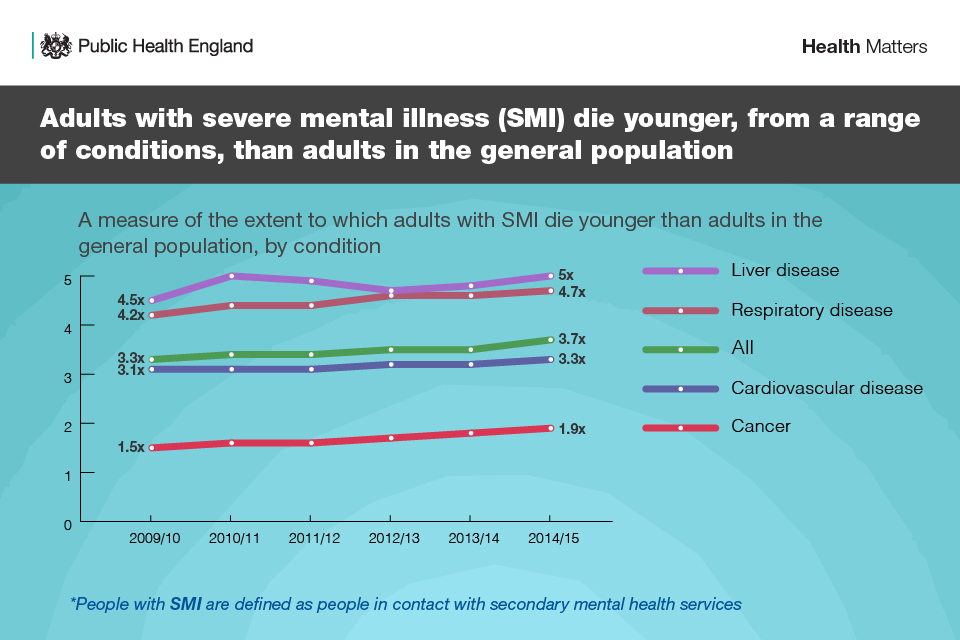
Infographic showing people with SMI die younger from a range of conditions
Although CVD accounts for the majority of premature deaths among people with SMI, health disparities are greatest for liver disease and respiratory disease and there has been little improvement over time.
The reasons for this increased burden of physical ill-health and reduced life expectancy are due to complex and interrelated factors.
These include:
- wider social factors such as unemployment and poverty
- increased behaviours that pose a risk to health such as smoking and poor diet
- lack of support to access care and support
- effects of medication which include weight gain
- stigma, discrimination, isolation and exclusion preventing people from seeking help
- diagnostic overshadowing, which is the misattribution of physical health symptoms to part of an existing mental health diagnosis, rather than a genuine physical health problem requiring treatment
Suicide is also a significant cause of death amongst people with mental illness. The 2018 National Confidential Inquiry reports that 28% of all suicides were in people who had contact with mental health services in the 12 months prior to death.
Older people may experience inequalities in access to care and treatment. A report from the Royal College of Psychiatrists highlights that older people who self-harm or have depression are much less likely to be referred to specialist mental health services than younger adults.
Perinatal mental illness can have a significant and long lasting effect on women, their babies and families if not identified early enough and managed effectively. Some groups may be more vulnerable to perinatal mental health problems such as women with a pre-existing psychiatric diagnosis. The Confidential Enquiry into Maternal Deaths and Morbidity shows that suicide remains one of the leading causes of maternal mortality in the UK.
People from minority ethnic backgrounds experience further disadvantage. For example, black people are more likely to be detained under the Mental Health Act, and have lower rates of recovery.
Black people with SMI are more likely than other groups to come into contact with secondary care services through non-health agencies, in particular, the police. Adverse experiences of hospital mental health services among minority ethnic groups continue to be a cause of concern. These issues can lead to a mistrust of services and delays in seeking care.
The commitments being taken forward by national organisations in response to the Five Year Forward View for Mental Health (FYFVMH) are underpinned by a need to achieve equality in mental health, particularly for BAME groups.
Behavioural health risk factors
People living with mental illness also have higher rates of health risk factors. Wider social factors and stressors can impact people’s psychological wellbeing and their health behaviours. These connections are complex but many health behaviours are perceived as immediate coping and survival mechanisms despite their impact being damaging to health.
Smoking remains the largest single cause of preventable death in England. Whilst smoking prevalence in the general population is at an all-time low at 14.9%, amongst people with SMI registered with a GP, it is almost 3 times that at 40.5%.
The Tobacco Control Plan for England recognises the need for urgent action in inpatient and community mental health settings to reduce the stark difference in smoking rates, and ensure people with a mental health condition are not left behind as we move towards a smokefree generation.

Infographic showing smoking is a risk factor for people with severe mental illness
Alcohol and drug misuse are also very common among people with mental illness, and vice versa. Research shows that mental health problems are experienced by the majority of drug (75%) and alcohol (85%) users in community substance misuse services.
Death by suicide is also a major risk, with a history of alcohol or drug use being recorded in 54% of all suicides in people experiencing mental health problems in England.
Preventative care and support
People with SMI experience more risks to remaining well but are not always offered timely and appropriate health assessments for early detection of physical health problems. They may be less likely to receive preventative care or health promotion interventions.
The National Clinical Audit of Psychosis 2018 found that physical health monitoring is gradually improving, with 42% of patients having 5 major physical health risk factors monitored annually compared to 27% 6 years ago in the first audit.
National screening programmes save lives, improve health and enable choice.
However screening services are not always as accessible as they should be, and groups such as those with mental health problems face significant barriers in making an informed personal choice about screening and accessing services. These barriers include:
- lack of registration with a GP
- lack of knowledge and confidence about screening amongst health staff in some health care settings
PHE’s screening inequalities strategy sets out the case for change and identifies key actions that PHE will take to support the health system to reduce inequalities in national screening programmes.
Amongst these actions is a commitment to better understand and support the system to address the barriers faced by people with severe mental illness, for example, by putting in place mechanisms to ensure that people receiving long term hospital care, with or without a GP, receive an invitation for screening.
Screening providers need to be aware of all local mental healthcare settings in their catchment area and work collaboratively to make sure all eligible patients are supported to make an informed decision about screening, for example through the provision of appropriate and accessible information materials.
NHS England guidance, Improving physical healthcare for people living with severe mental illness in primary care sets out what good quality physical healthcare provision in primary care must include. A Kings Fund report Bringing together physical and mental health sets out what an integrated approach to physical and mental health would look like for people with mental illness.
People in contact with the criminal justice system living with mental illness
People in contact with criminal justice are more likely to experience mental ill-health than people in the general population. These mental health needs are often compounded by coexisting social disadvantage, such as substance misuse, poor physical health, homelessness or insecure accommodation, offending behaviour, unemployment, persistent poverty and debt.
Prevalence of self-inflicted deaths and self-harm in prisons remain higher than in the general population. In 2017, the likelihood of self-inflicted death in prisons was 5.1 times greater than the risk in the community. Current research shows that effective strategies should focus on 2 main interventions: targeted individual support and population or environmental approaches such as improving the safety of the prison environment and linking to wider community programmes post release.
However, this population is often described as being ‘underserved’, with services provided that are not appropriate or accessible to this population. This can be due to personal and structural barriers such as stigma, low levels of help seeking behaviour, complex commissioning arrangements leading to fragmented pathways as well as challenging personal and social circumstances.
This can restrict the opportunities for early detection, monitoring and treatment of health and social problems resulting in the health needs of this population going unmet and often escalating levels of conflict with law enforcement.
Local actions to reduce inequalities in mental illness
Good health and wellbeing demands a broader focus than just health care services. Prevention is better than cure sets out the government’s plans to rebalance healthcare with greater emphasis on prevention. Creating the right conditions for good health and wellbeing will require taking a whole person approach, addressing the root causes of poor health amongst people with mental illness, and empowering people to make informed choices. This will need system wide action at both a local and national level with targeted action for those most at risk.
This section highlights a range of preventative actions that local areas can take to reduce inequalities and improve health outcomes and the lives of people with mental illness.
Examples of PHE tools and resources that can support are also highlighted.
1. Understand local population need
Understanding the mental health needs of the local population is vital for good service planning and commissioning. All local areas should have a mental health and wellbeing Joint Strategic Needs Assessment (JSNA) in place to build a picture of local needs, including an understanding of variations in prevalence, risk and protective factors for people with or at risk of mental illness and amongst different populations, for example BAME.
PHE provides a range of data tools and resources to support the JSNA development process and inform local decision making:
- PHE’s Mental Health and Wellbeing JSNA knowledge guide provides an overview of the areas to consider when thinking about the mental health needs in a local area, with a focus on understanding place factors and population groups across the life course. This is accompanied by a Mental Health and Wellbeing JSNA data profile and updated PHE’s Health profiles for England. A report on key features of a good Mental Health JSNA is also available.
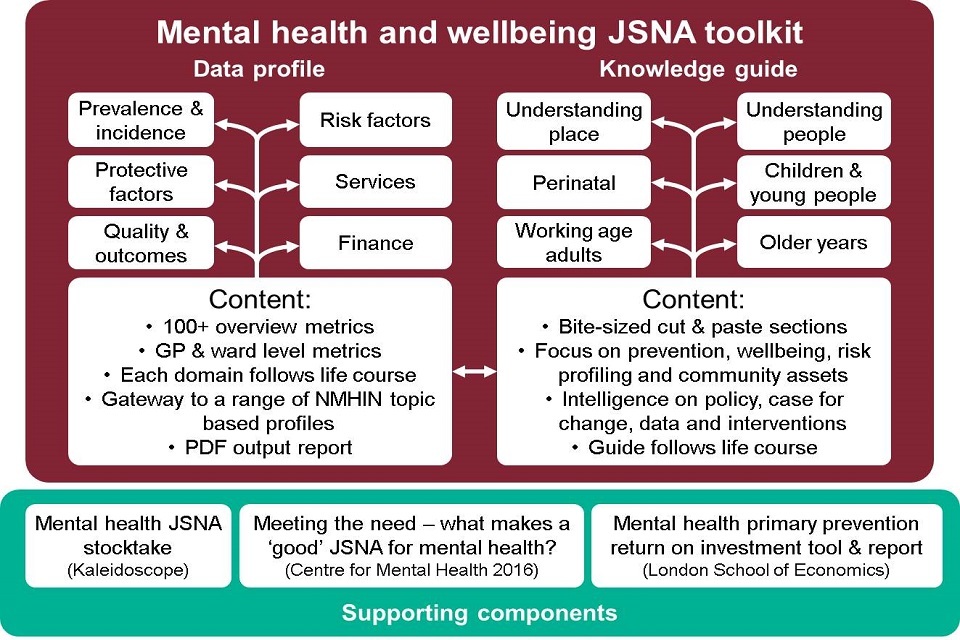
Infographic showing outline of JSNA mental health and wellbeing knowledge guide
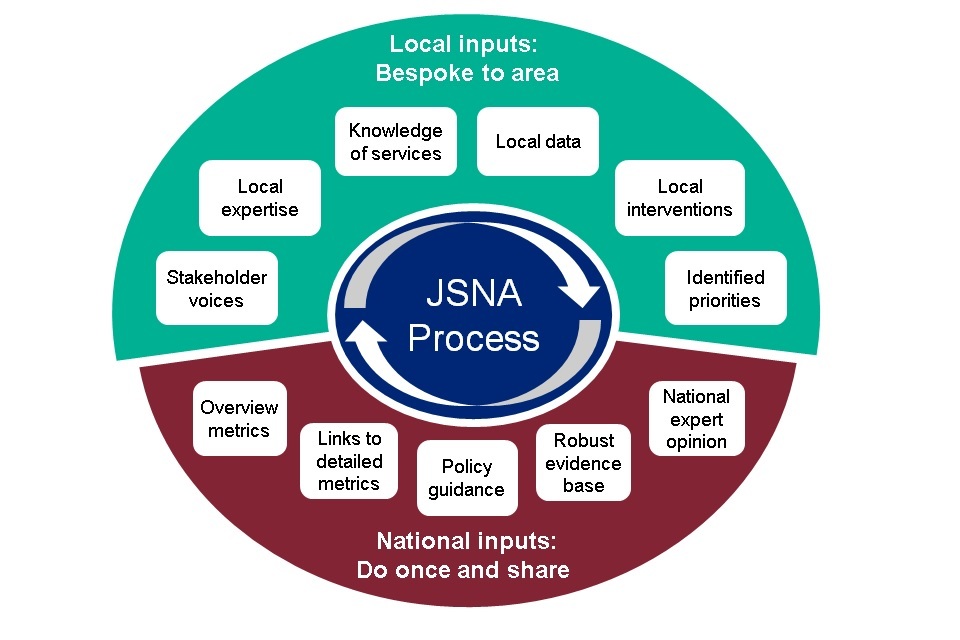
Infographic showing JSNA process
- PHE Fingertips Mental Health Profiles support local areas to focus on specific themes, such as severe mental illness and co-occurring substance misuse and mental health. Data can be filtered at different levels such as by local authority and sustainability and transformation partnerships (STPs).
- PHE Alcohol, drugs and tobacco: commissioning support pack has been developed to help commissioners and local authorities develop joint strategic needs assessment and health and wellbeing strategies to reduce the harm caused by smoking, drinking, substance use and misuse in both adults and children.
- The Prevention concordat for better mental health is helping galvanise adoption of effective place based arrangements to promote good mental health and prevent onset, development and deterioration of mental health problems. PHE has produced resources to support prevention focused planning and leadership, secure cross sector action, and deliver an increase in health equity.
- Guidance on local suicide prevention planning is available. There is also a PHE Fingertips suicide prevention profile to support local areas to ensure prevention plans are based on local need.The National Confidential Inquiry into Suicide and Safety in Mental Health have published a self-assessment toolkit for mental health services and primary care to help reduce suicide rates and improve safety for all mental health patients.
- PHE’s report on understanding and reducing ethnic inequalities provides material on ethnicity and health for use in local JSNAs and local health and wellbeing strategies.
In addition, local areas should explore and analyse their own service level data to identify and reduce health inequalities, where local agreements for access exist.
2. Address the social determinants of poor health
Addressing social factors and improving the conditions in which people live and work can help reduce the stressors faced by the population, improve physical and mental health and reduce health inequalities. Efforts to improve outcomes should include action to reach and support specific groups who face particular disadvantage and exclusion. Commissioners and providers should collaborate and work with their system partners and people with lived experience to address social factors and reduce inequalities.
Local areas can use the ‘understanding place’ section of the PHE JSNA toolkit to help understand the social and contextual factors that impact mental health in their local area and to inform interventions to improve health. A Wider Determinants of Health Profile is also available. Emphasis should be placed on enhancing the protective factors for health and factors that promote health alongside reducing risk factors.
Interventions to improve employment opportunities and employment retention of people with mental illness are likely to contribute towards reducing health inequalities. PHE has produced local data packs on work, worklessness and health for each county and unitary authority in England. The pack includes data on the mental health employment gap for each local area and further information to inform local conversations and action.
Examples of local interventions can be found in the PHE and the Institute of Health Equity’s evidence review on increasing employment opportunities and improving workplace health. They include using a regional trainer approach to accelerate implementation of IPS across mental health services. In line with this, NHS England and the Joint Work and Health Unit have jointly funded a national support programme, designed to drive consistent delivery of high-quality IPS services among existing and new services within secondary mental health care.
Further PHE resources are available to help local areas make plans to reduce health inequalities and improve health and wellbeing through the places people live such as creating healthy communities and neighbourhoods, preventing homelessness and improving access to green spaces.
Increasing the use of good quality green space for all social groups is likely to improve mental health outcomes and reduce health inequalities, as well as bring other benefits such as greater community cohesion and less social isolation. Research shows there is a positive association between living near green space and higher levels of physical activity.
3. Build stronger communities and social connections
Addressing loneliness, social isolation, building a sense of belonging and participation in a local area and creating good social networks and social support are important outcomes for reducing inequalities in mental illness.
Community-centred approaches can also be an effective way of engaging marginalised groups and vulnerable individuals, therefore helping to reduce health inequalities within a local area. These types of approaches are about mobilising the assets within communities, fostering social connectedness, community resilience, promoting equity and increasing people’s control over their health and lives.
Local areas should consider how community-centred approaches that build on individual and community assets can become an essential part of local mental health plans and strategies.This should include co-production and involving those experiencing or at risk of mental illness in designing and delivering solutions that address inequalities in health.
The Health Matters edition on community assets gives more information on the important roles for NHS, local government and their partners in commissioning and delivering community-centred mental health approaches. E-learning modules are available to support implementation of the guide
4. Early detection and intervention for physical health risks
The FYFVMH emphasises the need to better meet the physical health needs of people with mental illness. This includes ensuring access to prevention and screening programmes and early recognition of health risks and appropriate intervention.
Equally Well UK is a new initiative, led by Centre for Mental Health, which seeks to promote and support collaborative action to improve physical health among people with a mental illness and reduce inequalities and offers a range of useful resources.
Physical health checks for people with severe mental illness
Via the FYFVMH, NHS England has committed to ensuring that by 2020 to 2021, at least 280,000 people living with SMI have their physical health needs met. Commissioning guidance for CCGs has been published to support this, and includes ensuring that people receive the full list of recommended physical health assessments as part of a routine check at least annually. The Improving physical healthcare to reduce premature mortality in people with serious mental illness CQUIN 2017 to 2019 provides a financial incentive to drive further integration to improve physical health care for people with SMI and also includes a focus on interoperability between primary and secondary care.
The NHS Health Check is a national programme offering a health check-up for adults in England aged 40 to 74. The programme features 3 components: risk assessment, risk awareness and risk management. The NHS Health Check is designed to help prevent and detect early signs of heart disease, kidney disease, Type 2 diabetes and dementia, although its impact is likely to benefit a number of non-communicable diseases, given a number of shared risk factors. To maximise the impact of the NHS Health Check programme and to ensure it is contributing to reducing health inequalities and increasing healthy life expectancy, local areas need to ensure not only equity of access, but also equity of outcomes from checks. The NHS Health Check Programme Health Equity Audit (HEA) guidance, produced collaboratively by PHE and local authorities, can be used to help identify the extent of inequalities in access, uptake and outcomes between different groups and areas, including those with mental health problems, and inform where to focus efforts.
The recommended physical health assessment for people with SMI aligns to the NHS Health Check but is more comprehensive. It is offered annually, to all ages and includes additional checks, personalised care planning and psychosocial support. Local areas may want to consider streamlining the delivery arrangements for the two processes where possible for those eligible.
Routinely screen and intervene for smoking and harmful alcohol use
Implementing the national Preventing Ill Health by Risky Behaviours – Alcohol and Tobacco CQUIN has the potential to reduce the risk of a physical health conditions such as heart disease as well as reduce future hospital admissions. Tools to support implementation include an e-Learning module for smoking and alcohol interventions guidance page and Knowledge Hub to share learning.
Data from the CQUIN’s first year of operation shows some improvements in the proportion of patients with mental health problems who are being routinely screened and offered support for these health risks but there is wide variation across Mental Health Trusts.
Case study: South London and Maudsley NHS Foundation Trust refocus on alcohol screening and interventions
Smoking cessation
People with a mental health condition are just as likely to want to stop smoking as other smokers and must be offered the support they need to quit. PHE’s Health Matters: Stop smoking – what works? presents the range of smoking quitting routes that are available and the evidence for their effectiveness. Guidance for conversations with patients and for frontline staff in mental health settings on how to deliver Very Brief Advice (VBA) to patients who smoke are also available.
Further resources for commissioners and providers to help people to stop smoking and to support implementation of NICE smoking and mental health guidance PH48 and PH45, include:
- Smoking cessation implementation guidance
- Good Practice for mental health services
- Guidance on using the mental health deep dive self-assessment tool on NICE smokefree compliance as well as local case studies
Make every contact count
All staff should Make every contact count and use every opportunity to have brief conversations with patients about making positive changes to their health and wellbeing.
Practical resources are available to support local implementation. The Prescribing Movement toolkit provides a range of information to support 1 minute, 5 minute and even more minute conversations on physical activity for people with different conditions including depression.
‘If a contact is to truly count, the focus should be on the individual and their needs. This may involve lifestyle areas …. It may also involve ensuring individuals can access services to support the wider determinants of health, such as housing or financial support, which may be barriers to making a healthy lifestyle choice.’ NHS England.
Optimal preconception, pregnancy and postnatal care
Whilst significant improvements have been made, continued action is needed to ensure optimal preconception and contraception support for women to improve health outcomes, as outlined in the NHS England perinatal mental health pathway. Targeted action is needed to support the needs of more vulnerable groups such as women with SMI.
The PHE JSNA toolkit provides an overview of perinatal mental health issues with examples of useful resources and information.
Additional resources include early years high impact areas which includes maternal mental health and PHE preconception care resource to support coordinated, collaborative service provision within local maternity systems, across primary care and broader health and prevention services.
The charity Tommy’s has a digital preconception tool which gives women information on achieving a healthy pregnancy including their mental health.
System wide action to meet the health needs of people in contact with the criminal justice system
PHE has co-produced the publication Rebalancing Act for Directors of Public Health, Police and Crime Commissioners (PCC) and other system leaders. It provides national evidence on the needs of people in contact with the criminal justice system. Its aims are to stimulate conversations and action between local health, social care, criminal justice and other partners, to address the health inequalities experienced by people in contact with criminal justice and reduce offending behaviour. It also provides a reference for developing local needs assessments as part of the JSNA. PHE has also published a Health Needs Assessment template which provides a description of a standard report for an adult (18 years and over) prison health needs assessment (HNA) which are commissioned by NHSE every 3 years or when a new service provider is commissioned. A specific guide on older people in prison has also been published.
5. No wrong door: support available through every contact point
5.1 Improved access to services for people with co-occurring conditions
Despite the increased risk, evidence from Care Quality Commission (CQC) service user and provider surveys suggests that people with co-occurring conditions are often unable to access the care that they need from both mental health services and addiction services, and are often excluded from both services.
Providers in alcohol and drug, mental health and other services should aim to have an open door policy for individuals with co-occurring conditions, and make every contact count. Meeting the needs of those with co-occurring conditions needs to become recognised as everyone’s job and treatment for co-occurring conditions should be available through every contact point.
Better care for people with co-occurring mental health and alcohol and drug use conditions sets out how commissioners and providers can and should work together to improve access to services which can reduce harm, improve health and enhance recovery, so that services respond effectively and flexibly to presenting needs and prevent exclusion.
This guidance highlights the importance of joint commissioning across mental health and alcohol and drug services, integrated and coordinated care for individuals with co-occurring conditions and access to recovery support and wrap around services. It points out the need for crisis mental health care to be available round the clock and to be responsive to the needs of those with co-occurring conditions, including when people are intoxicated when they present to services.
5.2 Drug related deaths
PHE is working with drug treatment providers to support improvements in their identification of, and clinical responses to, those most at risk of a drug related death. It is also working to encourage local authorities and their commissioned services to expand the availability of naloxone, the ‘antidote’ to heroin overdose.
With the publication of drug death figures for 2017, we may now be seeing the first signs that this work is helping to reverse the upward trend in drug misuse deaths, but the numbers are still too high. This was the first decrease in drug misuse deaths in England since 2012 and follows annual increases totalling 60% from 2012 to 2016. PHE is updating 2011 guidance on local drug death review processes and helping local areas to audit their understanding of, and responses to, drug and alcohol deaths.
6. Build a confident, competent and committed public mental health workforce
Local partners responsible for leadership and workforce development should incorporate within their workforce development plans the 6 ambitions from the PHE Public mental health leadership and workforce development framework within their workforce development plans and take action on the priorities.This includes supporting the development of a workforce that is confident, competent and committed to improving the quality of life and healthy life expectancy of people living with mental illness and tackling inequalities.
Primary care staff and others working in non-mental health roles need to be able to meet the needs of people with a mental illness and ensure equitable access to services. Skills for Health, Health Education England, and Skills for Care have produced the Mental Health Core Skills Education and Training Framework for the general workforce who come into contact with people with mental illness.
Physical health and prevention should also be within the skill set of mental health service professionals so they can identify and meet physical health needs and have seamless referral pathways to other services. Training mental health staff in Making Every Contact Count will give them the confidence to have brief conversations with patients about how to improve their overall health and wellbeing.
Every local authority is encouraged to have an elected member mental health champion as part of their leadership responsibilities.
Additional information resources for health care professionals include:
- Improve the physical health of people with mental health problems: Actions for mental Health Nurses. This sets out actions in 8 key areas that are associated with particular risk factors for physical ill-health.
- PHE All our Health: mental health and wellbeing is part of a series of resources to help all healthcare professionals prevent illness, protect health and promote wellbeing
- The Charlie Waller Memorial Trust provides train the trainer programmes in mental health and wellbeing for practice and community nurses.
Resources
Read the PHE public mental health collection
Download supporting references.
Download the Health matters infographics
Read the Health matters blog.
Read case study: Mental health: improving employment and health outcomes
Read case study: Smoke-free implementation in the Sheffield NHS trust
Read case study: South London and Maudsley NHS Foundation Trust refocus on alcohol screening and interventions
