COVID-19 Response - Spring 2021
Published 22 February 2021
Executive summary
The UK Government’s overriding goal is to protect the lives and livelihoods of citizens across Scotland, Wales, Northern Ireland and England. For the benefit of the whole UK, the Government has secured access to more than 400 million vaccine doses,[footnote 1] established the largest testing infrastructure in Europe, and provided an unprecedented level of financial support for businesses and individuals.
This COVID-19 Response sets out how the Government will continue to protect and support citizens across the UK and provides a roadmap out of the current lockdown in England. The Devolved Administrations are setting out how lockdown will be eased in Scotland, Wales and Northern Ireland.
Vaccines are at the heart of the UK Government’s strategy to manage COVID-19. The UK is deploying the most ambitious vaccination programme in history. So far, over 17 million people have received a vaccine across the UK.
The Government has achieved its goal to offer a first dose of the vaccine by 15 February to all those in the four most vulnerable cohorts identified by the Joint Committee on Vaccination and Immunisation (JCVI). This includes elderly care home residents, those aged 70 and over, those with conditions that would leave them clinically extremely vulnerable to serious illness and death as a consequence of COVID-19, and frontline health and social care staff. The NHS has now started to vaccinate the next set of cohorts (JCVI cohorts 5 to 9), including adults aged 50 and over and people whose underlying health conditions make them more likely to suffer serious disease. The Government aims for everyone who is 50 and over, or at risk, to have been offered a first dose of the vaccine by 15 April, and for everyone aged 18 and over to have been offered a first dose by 31 July.
The success of the vaccination rollout, alongside falling infections and hospitalisations, is paving the way for the safe and gradual lifting of restrictions. Vaccines will mean that fewer people will get COVID-19 and that those who do are far less likely to go to hospital or to die. However, not all those offered the vaccine will take it up and there are some groups, such as children, for whom the vaccine is not yet authorised. Even when vaccinated, there is still a chance people can contract the virus and pass it on. No vaccine is 100% effective and, like all viruses, COVID-19 can mutate. As a result, as lockdown is lifted, there will sadly be more cases, hospitalisations and deaths. The Government will take a cautious approach to easing lockdown, guided by the data in order to avoid a surge in infections that would put unsustainable pressure on the NHS.
Increased vaccination reduces the risk of infection leading to severe disease or death. However, as with other diseases like the flu, some degree of risk will always remain. As social and economic restrictions are lifted, it will be increasingly important for people to consider the risks for themselves, taking into account whether they and those they meet have been vaccinated or have any pre-existing vulnerabilities.
The Government has taken the best scientific advice from the Scientific Advisory Group for Emergencies (SAGE) and its working groups on the pace and sequencing of reopening. This analysis is being published by SAGE to inform the public of the scientific and evidential basis that has helped to shape the roadmap.
Due to the relatively uniform spread of the virus across the country, the Government plans to ease restrictions at the same time across the whole of England. The roadmap seeks to balance health, including mental health, economic and social factors and how they disproportionately impact certain groups, as well as epidemiological evidence.
The roadmap set out in chapter 3 outlines four steps for easing restrictions. Before proceeding to the next step, the Government will examine the data to assess the impact of the previous step. This assessment will be based on four tests:
a. The vaccine deployment programme continues successfully.
b. Evidence shows vaccines are sufficiently effective in reducing hospitalisations and deaths in those vaccinated.
c. Infection rates do not risk a surge in hospitalisations which would put unsustainable pressure on the NHS.
d. Our assessment of the risks is not fundamentally changed by new Variants of Concern.
It takes around four weeks for the data to reflect the impact of the previous step and the Government will provide a further week’s notice to individuals and businesses before making changes. The roadmap therefore sets out indicative, “no earlier than” dates for the steps which are five weeks apart. These dates are wholly contingent on the data and are subject to change if the four tests are not met.
As restrictions are lifted, maintaining good habits which minimise transmission will be important, for both individuals and for businesses. The Test, Trace and Isolate system will continue to support the easing of social and economic restrictions. It will also be important in identifying local outbreaks and Variants of Concern. Strong measures are in place at the border to mitigate the risk of importing new cases and new variants. Where a dangerous Variant of Concern is identified and is likely to pose a real risk to the vaccination programme or public health, the Government will take a highly precautionary approach, acting fast to address outbreaks. The Government will also act quickly where an area sees unmanageable virus growth or the NHS is at risk, with local intervention centred on testing, communications and enforcement.
As restrictions ease and the economy is gradually and safely reopened, the Government will carefully tailor the level of support to individuals and businesses to reflect the changing circumstances. The 3 March Budget will set out further detail on economic support to protect jobs and livelihoods across the UK. The Government will continue to provide support for the most vulnerable. Recognising that visits from family and friends are crucial for the wellbeing of care home residents of all ages, their families and friends, the roadmap includes more opportunities for visiting. Additional testing will also be provided to facilitate safer visits for residents in high risk Supported Living and Extra Care settings. The Government recognises that some groups within society have felt the impact of the pandemic more acutely, and is committed to addressing the longer-term implications of COVID-19 for those communities.
Over time, scientists expect COVID-19 to become endemic, meaning the virus will reach a stable, and hopefully manageable level. Vaccinations - including revaccination - will be key to managing the transition from pandemic to endemic state. Therapeutics and antivirals will become increasingly important, replacing most non-pharmaceutical interventions over the long-term. The Government is also committed to building resilience for any future pandemics, both domestically and on the international stage.
1. Introduction
New variant cases, hospitalisations and deaths
At the end of 2020, a new and more transmissible variant of COVID-19 (B.1.1.7) began to spread very quickly across the UK. The Government responded by reintroducing the Stay at Home order first in the regions most affected and then nationally across England. The Devolved Administrations took similar approaches.
The B.1.1.7 variant appears to have increased transmissibility compared to the original strain of COVID-19 and has grown quickly to become the dominant variant across the UK. Both strains can be spread by people with no symptoms. As a consequence, the B.1.1.7 variant led to further surges in cases, hospitalisations and deaths.
Figure 1: Rolling 7 day average of cases, hospitalisations and deaths in England since 1 March 2020 [footnote 2] (Testing capacity and policies have changed since May 2020)

First of three charts showing the 7 day rolling average for COVID-19 cases (by specimen date), patients in hospital with COVID-19, and deaths within 28 days of a positive COVID test (by date of death) in England from the start of March 2020 to the middle of February 2021.
Hospital occupancy and deaths rise in spring 2020, dip during the Summer, begin to rise again in September, and then rise sharply around December before falling after mid January 2021.
Cases show a similar pattern to hospital occupancy and deaths from September onwards.
Second and third of three charts showing the 7 day rolling average for COVID-19 cases (by specimen date), patients in hospital with COVID-19, and deaths within 28 days of a positive COVID test (by date of death) in England from the start of March 2020 to the middle of February 2021.
At the peak, NHS hospitals were caring for over 34,000 COVID-19 patients in England, approximately 80% higher than the wave 1 peak. Of these, a peak of over 3,700 were on mechanical ventilation. [footnote 3] The ability of the NHS to sustain this level of pressure was due to the dedication of the NHS workforce. Hospitals shared resources and spare capacity through mutual aid and an accelerated discharge programme that used Nightingale hospitals and other sites, to enable patients to leave hospital more quickly. The independent sector also bolstered the NHS’s capacity to perform large volumes of planned care, however some patients had their non-urgent treatments postponed. This pressure has had a regrettable increase on waiting times.
Cases, hospitalisations and deaths have fallen since lockdown started. Between 6 and 12 February, 1 in 115 people have tested positive for COVID-19 in England compared to a peak between 3 and 9 January when 1 in 50 tested positive for the virus. In Wales, this is 1 in 125 people, in Scotland 1 in 180, and in Northern Ireland 1 in 105 people.[footnote 4] In the UK, as of 16 February, 20,177 are in hospital with COVID-19, down from a peak of 39,244 on 18 January, and average daily reported deaths have fallen from a high of 1,248 to 494.[footnote 5]
Impact on economy and society
While restrictions across the last 12 months have helped control the virus, they have also had a significant impact on the economy, society and education. The latest data shows that the UK economy shrank by 9.9% in 2020, as the pandemic and associated public health restrictions drove the largest annual fall in UK GDP on record. [footnote 6] GDP in December remained 6.3% below February 2020 levels.
Figure 2: UK GDP January 2019-December 2020 [footnote 7]
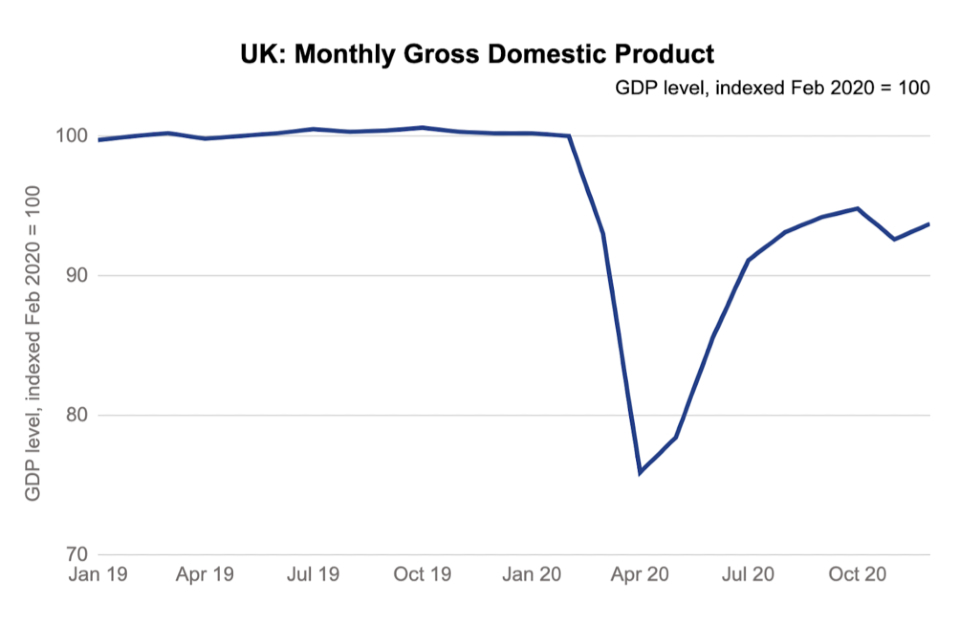
Line graph showing UK monthly gross domestic product as a percentage of GDP in February 2020, between January 2019 and October 2020, from the Office for National Statistics. The graph shows a steep fall from March 2020 of about 25%. GDP then begins to recover sharply, before showing a dip in November 2020. By December 2020, GDP has not fully recovered to the level of Feb 2020.
Businesses and their suppliers are suffering from enforced closures and restrictions on social contact - particularly aviation, pubs, restaurants and hotels, sports and events, arts, entertainment and conferences - and so are their suppliers. Even though the Government has provided over £280 billion in financial support since March 2020, jobs have inevitably been lost given the unprecedented challenge of the pandemic. [footnote 8] The number of employees on payroll fell by 828,000 between February and December 2020. [footnote 9]
The pain has not been felt equally. Staff in the hardest-hit sectors, such as hospitality, are more likely to be young, female, from an ethnic minority, and lower paid. The unemployment rate for those aged 18 to 24 increased from 10.5% in the three months to February 2020 to 13.2% in the three months to November 2020. [footnote 10] The unemployment rate for ethnic minorities has increased from 5.8% in the three months to December 2019 to 8.5% in the three months to September 2020. [footnote 11]
Figure 3: Impact on youth unemployment July 2018-2020 [footnote 12]

Line graph from the Office for National Statistics showing the UK unemployment rate from July 2018 to July 2020. The blue line shows the unemployment rate for all people. It starts just below 5%, increasing to just over 5% by July 2020. An orange line shows the unemployment rate for those aged 18 to 24. The line starts at 10%, before showing a significant increase to about 13% during 2020.
Around the country, some regions have fared worse than others. Jobs have been lost everywhere but more so in London, the West Midlands and the South East. [footnote 13] The longer restrictions are in place, the greater the risk of businesses becoming insolvent or having to close permanently.
The damage to society can be seen in the figures for violent crime and drug offences: these have risen above pre-pandemic levels in deprived areas. Mental health and wellbeing have also suffered during lockdowns, according to the UCL COVID-19 Social Study. Anxiety and depression levels are now consistently higher than pre-pandemic averages. [footnote 14] This coincides with restrictions to school attendance which have severely damaged children’s education. By February half term, studies suggest the total loss in face-to-face learning could amount to around half a school year, with two thirds of a normal year lost if the return to face-to-face education in schools is delayed to after Easter. Restrictions to school attendance have also impacted parents’ ability to work, as they have had to oversee remote learning at the same time as working from home. [footnote 15]
Figure 4: UK Depression and Anxiety levels in adults compared to pre-pandemic averages March 2020 - January 2021 [footnote 16]

Line graph with data from the UCL COVID-19 Social Study showing adult depression and anxiety levels in the UK from March 2020 through to January 2021. An orange and a blue dotted line indicate that the average depression and average anxiety scores are about 3. A solid blue line shows depression scores. These start at 7 in March 2020, slowly declining to approximately 5 by September, before rising to approximately 6 by the end of January 2021. A solid orange line shows a similar pattern for anxiety scores. These start at 6 in March 2020, declining to under 4 by September, before slowly rising again to plateau at 4.5 by the end of January 2021.
The Government acknowledges the impact on all public services and is balancing the medium and long-term impacts with the immediate risks of COVID-19 in decision making.
The Government has committed that it will do whatever it takes to support our country through the COVID-19 pandemic. The approach to support will reflect the roadmap, tailoring the level of support as the economy reopens to reflect the changing circumstances.
Without the decisive financial interventions from the UK Government, the Office for Budget Responsibility (OBR) and the Bank of England have confirmed the outlook would be far worse. [footnote 17] Further detail of the support the Government has provided to businesses and individuals is set out in chapter 5.
Government objectives
The Government’s approach is based on the following objectives:
a. To restore freedoms sustainably, equitably and as quickly as possible without putting unsustainable pressure on the NHS, and avoiding a further lockdown. The Government will take a gradual and cautious approach to reopening in England, guided by science and the data, with resuming face-to-face teaching in schools the priority.
b. To deploy the vaccine as quickly as possible to maximise protections as restrictions are eased. The more quickly people are vaccinated, the lower their risk of developing the kind of serious infection that requires hospital treatment and may lead to death.
c. To protect the public and the NHS by having effective long-term contingency plans. The Government will ensure it has the tools to manage local outbreaks, as well as the means quickly and effectively to combat dangerous new Variants of Concern, both domestically and at the border, in close partnership with the Devolved Administrations.
d. To plan and deliver a national recovery. As the country recovers from the crisis, the Government is committed to building back better, supporting the key public services on which citizens and businesses depend, and working with global partners as the disease moves from a pandemic to an endemic state.
2. The Health Care Response: The NHS, vaccines and therapeutics
Supporting the NHS
The people of the UK owe much to the NHS and its brilliant staff, who throughout the pandemic have drawn deeply on their professionalism, skills and training to do their very best for patients.
The Government stepped in during this time of unprecedented pressure - providing £3 billion in funding to support the NHS in England during winter, and consequential funding for the Devolved Administrations. This helped expand capacity to support both COVID-19 and non-COVID-19 patients by using the independent sector and the Nightingale Hospitals to ensure smooth operation of the NHS.
Additionally, thanks to effective recruitment and returning staff, last year the NHS workforce increased by over 48,000,[footnote 18] including over 25,000 professionally qualified clinical staff. The Government quickly put in place the measures needed for around 23,000 nursing students [footnote 19] and 3,800 medical students to support their colleagues on the frontline in England. [footnote 20]
This helped to protect non-COVID-19 services, such as cancer services, urgent elective surgery and diagnostics, as far as possible. Despite high levels of COVID-19 over the winter, the NHS in England carried out more than 80% of elective treatments in December 2020 compared to the previous year. [footnote 21] While elective care waiting times have increased for some patients, even during the highest period of pressure during the pandemic this winter, the NHS had brought average waiting times to 40% lower than during the summer.
The Government will continue to work with the NHS, to ensure that it has what it needs to deal with the impact of COVID-19. The Government is also committed to ensuring that NHS staff continue to have the comprehensive emotional, psychological and practical support they need.
Since the supply and logistical challenges at the start of the pandemic, the Government has made significant strides to ensure adequate quantities of Personal Protective Equipment (PPE) for staff on the frontline across the UK. Around 32 billion items of PPE have been purchased [footnote 22] and over 8.4 billion have been distributed. [footnote 23] As a result, there can be free provision of PPE to health and social care staff until at least June 2021, and a stockpile equivalent to approximately 120 days’ usage at COVID-19 levels in the UK will cushion any fluctuations in demand. In addition, more than 70% of required long-term capacity for PPE (with the exception of gloves) is now manufactured in the UK, creating hundreds of jobs. This compares with 1% at the start of the pandemic.
The Government will work closely with the NHS to continue to ensure it is able to deliver high quality COVID-19 and non-COVID 19 care for Winter 2021 and beyond, whilst also recovering elective performance.
The Government will also work with the social care sector to develop and set out measures that should be maintained in residential and community care settings. This will include good practice developed during the pandemic such as PPE procedures, testing protocols, and cleaning regimes in individual care settings. The system will be supported by local authorities and the Care Quality Commission (CQC) to ensure high quality care and safe infection prevention and control procedures are maintained.
While for many people COVID-19 is a mild illness, for some, regardless of age, the effects can linger into the long-term. The NHS and partner organisations are already implementing initiatives to support people with prolonged symptoms following COVID-19 infection. In addition, the National Institute for Health Research (NIHR) and UK Research and Innovation (UKRI) have announced funding for a number of ambitious studies that will help the Government learn more about the long-term effects of the virus, including among people who have not been hospitalised. [footnote 24]
Vaccines
Vaccines have always been at the heart of the Government’s strategy to manage COVID-19. The Government is working with the Devolved Administrations to implement the UK’s most ambitious ever vaccination programme, helping to pave the way for restrictions to be safely lifted.
The UK was the first country in the world to give regulatory approval to a COVID-19 vaccine that had been tested in large-scale trials: the Pfizer/BioNtech vaccine was authorised for use by the independent Medicines and Healthcare Products Regulatory Agency (MHRA) on 2 December 2020. [footnote 25] This was followed the same month by authorisation for use of the AstraZeneca vaccine developed by Oxford University [footnote 26] and the Moderna vaccine in January 2021. [footnote 27] Millions of UK citizens have already received the Pfizer/BioNTech and AstraZeneca vaccines, and the Moderna vaccine will be deployed later this year.
The UK has ordered enough doses to vaccinate all of the eligible adult population – a total of 457 million doses, comprising eight different vaccines.
Table 1: UK vaccines purchased and status [footnote 28]
| Vaccine | No of doses | Status |
|---|---|---|
| Oxford/AstraZeneca | 100 million | Approved and in deployment |
| Janssen | 30 million | Encouraging preliminary phase 3 safety and efficacy data |
| Pfizer/BioNTech | 40 million | Approved and in deployment |
| Moderna | 17 million | Approved |
| GlaxoSmithKline/ Sanofi Pasteur | 60 million | Phase 1/2 trials |
| Novavax | 60 million | Encouraging phase 3 safety and efficacy data |
| Valneva | 100 million | Phase 1/2 trials |
| CureVac | 50 million (initial order) | Phase 2b/3 trials |
Phase 1 rollout
The goal of the vaccine programme is to reduce illness, deaths and hospitalisations. The Government sought advice from the JCVI about which groups of people should be vaccinated as a priority. The JCVI identified nine cohorts for prioritisation in Phase 1 of the vaccination rollout to reduce mortality – a total of 32 million people in the UK – on the basis of age, residential setting, occupation and clinical vulnerability. [footnote 29]
Data on deaths and hospitalisations by age indicates the importance of prioritising the vaccination of older groups. Analysis of COVID-19 deaths finds that 88% of deaths were in cohorts 1 to 4, with a further 11% of deaths attributed to cohorts 5 to 9. [footnote 30] Recent hospitalisation data indicates that approximately 40% of COVID-19 hospital admissions related to patients aged 75 years and over. [footnote 31] In total around 75% of admissions are related to patients aged 55 years and over who fall in cohorts 1 to 9. [footnote 32]
Table 2: Number of people in each cohort for vaccination under JCVI priorities.[footnote 33]
| Priority Group | JCVI Category | England (m) | UK (m) |
|---|---|---|---|
| 1 | Residents in a care home for older adults | 0.3 | 0.3 |
| Residential Care Workers | 0.4 | 0.5 | |
| 2 | All those 80 years of age and over | 2.8 | 3.3 |
| Frontline health and social care workers | 3.2 | 3.8 | |
| 3 | All those 75-79 years of age | 1.9 | 2.3 |
| 4 | All those 70-74 years of age | 2.7 | 3.2 |
| Clinically Extremely Vulnerable (under 70) | 1.0 | 1.2 | |
| Total priority cohorts 1-4 | ~12m | ~15m | |
| 5 | All those 65-69 years of age | 2.4 | 2.9 |
| 6 | All individuals aged 16 years to 64 years with underlying health conditions | 6.1 | 7.3 |
| 7 | All those 60-64 years of age | 1.5 | 1.8 |
| 8 | All those 55-59 years of age | 2.0 | 2.4 |
| 9 | All those 50-54 years of age | 2.3 | 2.8 |
| Total priority cohorts 5-9 | ~14m | ~17m | |
| Total priority groups | ~27m | ~32m | |
| Rest of adult population | ~18m | ~21m | |
| Total | ~44m | ~53m |
The Government’s ambition to offer everyone in JCVI cohorts 1 to 4 at least one dose of the vaccine by 15 February was met two days early. On 19 February, thanks to the deployment efforts of the NHS, over 17.2 million people had already received their first vaccine dose and 604,885 people had also received their second dose across the UK. [footnote 34] The UK has vaccinated a higher proportion of its population than any other country in the G20, in part facilitated by the decision to extend the interval between doses, enabling first doses to be distributed more widely.
Figure 5 - Proportion (%) of population vaccinated in selected comparator countries [footnote 35]

Bar chart with data from Our World in Data showing the proportion of population who have been vaccinated in the UK and in comparator countries.
In each bar, there is a blue portion, showing those who have two doses of vaccine, and an orange portion, showing those who have had one.
The bar for Israel shows it has vaccinated the largest proportion of its population, with nearly 50% of its population having received a vaccine. Over 30% have had two doses, and more than 10% have had one.
The bar for the UK shows a quarter of its population have been vaccinated, but the bar is almost entirely orange, showing those vaccinated have received one dose.
The next closest country is the United States, with over 10% vaccinations, only slightly skewed towards first doses. The bars from Denmark to Russia show that under 5% of the populations have been vaccinated.
Figure 6 - Rollout in phase 1 to publication date January - February 2021 [footnote 36]
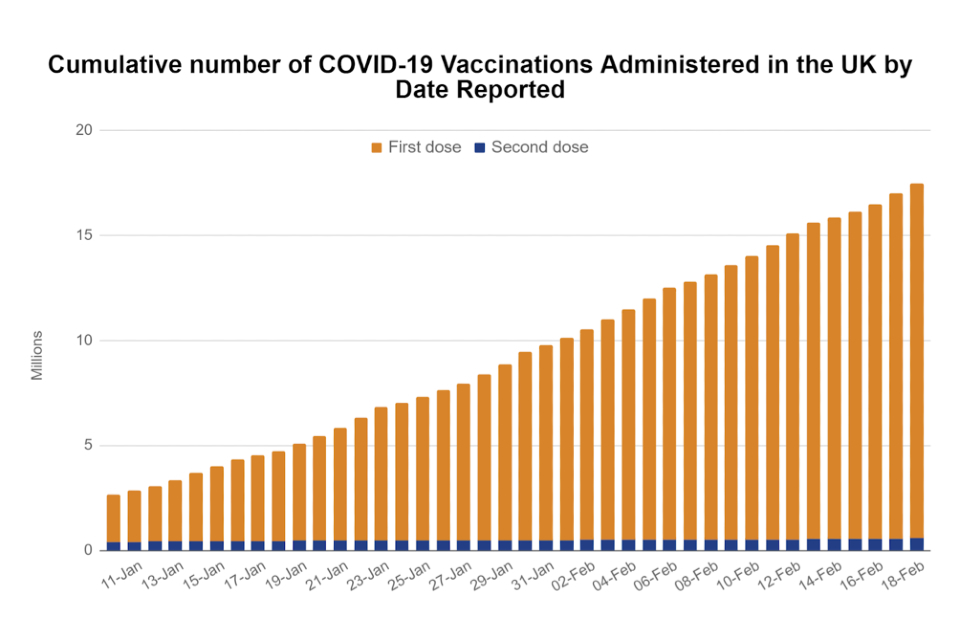
This bar chart shows the cumulative number of Covid-19 vaccinations administered in the UK by date reported, from UK government data.
The data starts on 11 January, where 2.5 million vaccines had been administered. The size of each bar steadily increases throughout the chart, showing the cumulative number of vaccinations increasing. By the 18 February, the bar shows the cumulative total is greater than 17 million.
In each bar, there is a blue portion, showing those who have second doses, and an orange portion, showing first doses. Each bar is almost entirely orange, showing that the vast majority of vaccinations being administered are first doses.
Everyone will be offered their second dose no more than 12 weeks after their first dose. This means that the Government will offer those in JCVI cohorts 1 to 4 who received their first dose by mid-February a second dose by mid-May.
The NHS has already begun offering vaccinations to people in cohorts 5 and 6. These include adults 65 and over, people whose underlying health conditions make them more likely to suffer serious disease, and unpaid carers as defined in the Public Health England (PHE) Green Book. [footnote 37]
The Government aims for everyone aged 50 and over and people with underlying health conditions (cohorts 5 to 9) to have been offered a first dose of the vaccine by 15 April, and a second dose by mid-July. At the same time, the Government urges those in cohorts 1 to 4 who have not yet taken up the offer of vaccination to do so.
Vaccine uptake
High vaccine uptake is crucial in enabling restrictions to be lifted safely; every person who gets the vaccine will help reduce the impact of the virus on themselves and society. Everyone who is eligible for a vaccine should make all efforts to get vaccinated, with both first and second doses important.
There has been excellent uptake of the first dose of vaccine in those 70 and over - more than 90%. The Government’s aim is to continue to see high uptake for both first and second doses through all age groups and for all communities so that no-one is left behind, and to increase protection of the population as a whole. There are early signs of lower vaccine uptake in lower income and some ethnic minority groups which the Government is taking steps to address. Surveys have found that there is higher vaccine hesitancy in some Black and Asian communities, hence the need to encourage uptake in these groups specifically. [footnote 38]
As set out in the UK COVID-19 Vaccine Uptake Plan, [footnote 39] the Government is taking steps to address vaccine concerns - in part through the new Vaccination Equalities Committee, which brings together Directors of Public Health, local authorities, voluntary organisations and the faith sector to understand and find ways to overcome the specific barriers facing different communities. This includes engagement at local level via trusted religious and community leaders, sharing examples of what is known to work well in nearby areas, and encouraging community-led efforts to address vaccine disinformation. The Department of Health and Social Care, NHS and PHE are also providing information and advice on vaccines, and the Government’s Counter-Disinformation Unit, led by the Department for Digital, Culture, Media and Sport (DCMS), works to tackle disinformation and misinformation relating to COVID-19.
This community-led response can draw on accurate, detailed uptake data from the NHS to direct efforts where they are most needed. First and second doses administered in each English region are published on a daily basis; this information is further broken down by age, ethnicity and Sustainability and Transformation Partnerships (STPs) on a weekly basis. Local authority directors of public health receive daily updates on vaccine uptake in their areas, broken down to small areas (Middle Layer Super Output Areas - MSOAs) and by ethnicity.
By allocating £23 million to 60 local authorities and voluntary groups across England to fund a network of Community Champions, the Government is offering extra support to people and organisations who are able to help boost vaccine uptake in communities. [footnote 40]
Recognising that accessibility can be a factor, the NHS in England is supporting the work of local vaccination services to offer accessible services to all - such as a mobile delivery model for people who are housebound. The NHS is also taking steps to promote vaccine uptake among those caring for some of the most vulnerable in our society, including health and social care staff, and continues to monitor the effectiveness of these measures.
Phase 2 rollout
Adults under 50 who do not fall into any of the JCVI’s priority cohorts 1 to 9 will receive their vaccinations in the second phase of the rollout. This covers around 18 million people in England, and 21 million in the UK. The Government expects Phase 2 of the vaccine rollout to begin from mid-April and aims to offer everybody aged 18 and over a first dose of the vaccine by 31 July.
In line with the Government’s wider priorities, the objective for the next phase of vaccine rollout is to bring down further the number of people dying, becoming seriously ill and being admitted to hospital. This will help to protect those more at risk, reduce pressure on the NHS, and support the reopening of society and the economy. The approach must also be easy to operationalise and not so complex that it delays speed of deployment.
The Government has asked the JCVI to advise on the best strategy for achieving this aim. The JCVI’s advice will be based on the latest clinical, epidemiological, scientific and public health evidence. This includes: considering whether there are groups that remain at an increased risk of being admitted to hospital, of infection and death; and whether particular occupations or settings involve a greater risk.
Vaccine efficacy and effectiveness
PHE has studied the effect of the Pfizer/BioNTech COVID-19 vaccine on symptomatic and asymptomatic infection, and on hospitalisation and deaths from COVID-19. [footnote 41]
The data is beginning to show clearly what the benefits of vaccination are in preventing infection, preventing symptomatic cases, and in significantly reducing hospitalisation and mortality for those who do show symptoms. The details of these three elements of protection are set out below.
First, the vaccine is preventing people from catching COVID-19. Studies in healthcare workers show that one dose of Pfizer/BioNTech vaccine reduces the risk of catching infection by more than 70%. A second dose reduces the risk by a further 15%, meaning protection of up to 85% after two doses. This will help to reduce the spread of infection in hospitals and care homes, ultimately offering more protection to these vulnerable populations.
Secondly, the vaccine is preventing symptomatic cases of COVID-19 in the older people who were first eligible for vaccination. The data suggests that one dose of Pfizer vaccine reduces symptomatic cases by between 50% and 70% in those aged 70 years and over. This effect occurs about three weeks after the first dose of vaccine, and the second dose improves this protection to between 80% and 90%.
Early data for the AstraZeneca vaccine suggests a good level of protection after one dose but, as deployment of this vaccine only started in January 2021, at this stage the size of the effect is less certain.
Third, in older people (aged 80 and over) who do develop COVID-19 infection, those who are vaccinated, most of whom have so far had one dose, have a much lower chance of hospitalisation (about 40% lower) and death (around 56% lower) than those who are unvaccinated. In addition, there is early evidence that the rate of decline in hospitalisation and mortality is currently greater in those 75 years of age and above (the population so far vaccinated) than in younger age cohorts. The opposite was the case at a similar period during the first wave in April 2020.
Taken together this data suggests that a single dose of the vaccine is providing a high level of protection against symptomatic and asymptomatic infection, against hospitalisation and death from COVID-19.
Overall, this means that hospitalisations and deaths from COVID-19 will be reduced by at least 75% in those who have received a dose of the Pfizer vaccine. When combined with the reduced spread from vaccinating health and social care workers, this means that our older population are now much better protected from COVID than ever before.
The effect of the vaccine has also been seen in other countries, like Israel. Most cases in the UK are now of the B.1.1.7 variant, and the levels of protection that have been seen in healthcare workers are very similar to what has been recently published from Israel. [footnote 42] This suggests that the vaccine is working well against this strain. There are not yet enough cases in circulation to measure any effect against the other Variants of Concern.
The vaccines have transformed our efforts to tackle COVID-19 and will prevent many deaths. However, they will not guarantee protection to everyone. Vaccines will not be given to 100% of the population. This is because the vaccine is currently not authorised for some groups, such as children, and some people will not take up the offer of a vaccine. Vaccines will not be 100% effective against symptomatic infection in those vaccinated, nor will they be 100% effective against severe disease and death.
For these reasons, a significant proportion of the population could still be infected, either because they have not been vaccinated or because the vaccine is not effective for them. This is illustrated by Figure 7. This could mean that some measures to limit transmission are still needed after all adults have been offered a vaccine. These could include guidance such as “hands, face, space”, maintaining the Test, Trace and Isolate system and controls at the border (see chapter 4). The extent to which such measures will be required after all adults have been vaccinated is still unknown. As set out in chapter 3, the Government is exploring what measures may be required.
Figure 7: Illustration of potential vaccine coverage (assuming full uptake by those eligible) [footnote 43]

This illustration shows the percentage of the population who would be protected in a potential scenario for vaccine take up and vaccine effectiveness. A red portion of the illustration shows those who are ineligible for a vaccine, this is 21% of the population. A blue portion shows those who are vaccinated but may not be protected, which is 13% of the population. The largest portion is the orange section, with 66% of people being vaccinated and may be protected.
Preparing for revaccination
It is not currently known for how long people who receive a COVID-19 vaccine will be protected. This is because, as is the case with many vaccines, the protection they confer may weaken over time. It is also possible that new variants of the virus may emerge against which current vaccines are less effective. As well as working closely with manufacturers, Government scientists are seeking to better understand the impact of some Variants of Concern on the vaccines currently in deployment.
To ensure the country is prepared for these scenarios and while further evidence is gathered, the Government is planning for a revaccination campaign, which is likely to run later this year in autumn or winter. Any revaccination is likely to consist of a single ‘booster’ dose of a COVID-19 vaccine: the ideal booster may be a new vaccine specifically designed against a variant form of the virus. Over the longer term, revaccination is likely to become a regular part of managing COVID-19.
Both the Pfizer/BioNTech and Oxford/AstraZeneca vaccines which are currently being deployed in the UK appear to work well against the current dominant strains of COVID-19 in the UK. Continuing to administer these vaccines at scale remains key to bringing the virus under control and enabling restrictions to be lifted safely.
The Government is taking steps to ensure the UK continues to have access to a range of effective vaccines. Domestic capacity for vaccine production is being bolstered across the whole country: since the beginning of the pandemic, the Government has invested over £300 million to secure and scale up UK manufacturing. This includes £93 million to accelerate the completion and expand the role of the Vaccines Manufacturing Innovation Centre at Harwell, and £127 million to establish a site in Braintree as a Cell and Gene manufacturing and innovation centre. The Government has also funded - through upfront payment for vaccines - the expansion of the Valneva factory in Livingston, Scotland and secured a 24-month “fill and finish” reservation with Wockhardt in Wrexham, North Wales.
A new partnership has also been established with vaccine manufacturer CureVac. The agreement will leverage the UK’s world-leading expertise on genomics and virus sequences to allow new varieties of vaccines based on messenger RNA (mRNA) technology to be developed quickly against new strains of COVID-19 should they be needed. Vaccines based on mRNA can potentially generate vaccines more quickly than other approaches and be more flexible and durable against germs that tend to evolve through mutation, such as coronaviruses and influenza. An initial order of 50 million doses of this vaccine has been placed for delivery later this year if required. [footnote 44] This will help ensure the Government can rapidly develop and deploy vaccines against any new variants, or similar new diseases, in the future.
International vaccines strategy
The Government wants to be at the forefront of spreading the benefits of COVID-19 vaccines around the world. The health of every country depends on the whole world having access to safe and effective vaccines, therapeutics and diagnostics.
The Government has pledged it will share the majority of any future surplus COVID-19 vaccines from the UK’s supply with COVAX, the international initiative to deliver equitable access to two billion vaccines, to protect a billion people in 2021. [footnote 45] The Government has also donated £548 million in funding for COVAX, making it one of the biggest donors. [footnote 46]
The UK will use its G7 presidency to encourage leaders to increase their funding for COVAX in support of equitable access to vaccines. In addition, the UK is working closely with global bodies and international partners such as the Coalition for Epidemic Preparedness Innovations (CEPI) and Gavi (the Vaccine Alliance that delivers vaccinations to half the world’s children) to ensure that low and middle income countries can access COVID-19 vaccines, treatments and tests.
Therapeutics
Effective treatments continue to be vital in reducing the risk to lives and of serious illness. Therapeutics are also invaluable for those in whom the vaccine does not prevent disease.
For this reason, the Government is supporting an advanced programme of clinical trials of therapeutic treatments. Thanks to patients who have enrolled onto clinical trials to test potential therapeutics, the NHS, working with the National Institute for Health Research (NIHR), and investment from UK Research and Innovation, the UK has led the way in the discovery of life-saving treatments, which have been made available to patients in the UK and across the world. Last year, a UK trial [footnote 47] discovered the benefits of dexamethasone, which reduces the risk of mortality by 20% for patients on oxygen and reduces risk of mortality by 35% for ventilated patients. This year UK trials [footnote 48] have demonstrated that tocilizumab can further reduce mortality and length of hospital stays. The benefits of tocilizumab are in addition to dexamethasone and these treatments are now being used in hospitals across the UK to save lives and reduce pressures on the NHS. When used in combination, dexamethasone plus tocilizumab or sarilumab reduce the risk of death for hospitalised patients by between a third to a half. [footnote 49]
More results are expected for medications used to help regulate or normalise the immune system, anticoagulants, anti-virals, and therapeutic antibodies for use by patients in different stages of the illness and various care settings, including hospitals and intensive care, primary care and care homes. The Government is also monitoring whether prophylactic therapies could reduce the number of patients vulnerable to COVID-19 despite vaccination, as well as therapies for those who continue to suffer the effects of COVID-19.
The UK Government has worked closely with the Devolved Administrations throughout the pandemic to ensure the UK has access to effective treatments for COVID-19, and will continue to do so. This includes through RAPID C-19, a multi-agency initiative that includes the Devolved Administrations, which has enabled rapid access to safe and effective treatments for patients right across the UK.
3. Roadmap
This roadmap is a step-by-step plan to ease restrictions in England cautiously, starting with schools and colleges. The Devolved Administrations are setting out separate plans for Scotland, Wales and Northern Ireland. Recognising the importance of clarity for those who live and work in different parts of the UK, particularly in cross-border communities, the Government will continue to work closely with the Devolved Administrations.
Lockdown has had a significant impact on the economy and businesses. As set out in chapter 1, it has also had a damaging impact on people’s quality of life and mental health. Decisions on when to lift restrictions, and in which order, seek to strike a balance between the epidemiological evidence and advice, the impact lockdown is having on people’s health (including mental health and disproportionate impacts on certain groups), wellbeing, and the economy.
The success of the vaccine programme means the Government can begin to chart a course out of lockdown. However, the Government will take a cautious approach to easing lockdown, which is guided by the data in order to avoid a surge in cases which would put unsustainable pressure on the NHS and claim more lives before people have the chance to take a vaccine.
In order to inform the pace and sequencing of the roadmap, the Government commissioned advice and modelling from SAGE and its sub-groups. This is being published so that the public can see the evidence which has informed the design of the roadmap.
Principles for easing
The design of the roadmap has been guided by some important principles. In the absence of significant regional disparity, the Government will ease restrictions at the same time across the whole of England. Due to the current relatively uniform spread of the virus across the country, the four steps out of lockdown set out in the roadmap are designed to apply to all regions. Decisions on easing restrictions will be led by data rather than dates. It takes around four weeks for the data to show the impact of easing restrictions and the Government will provide a further week’s notice to the public and businesses ahead of any further changes. For that reason, there will be at least five weeks between the steps in the roadmap. The indicative, ‘no earlier than’ dates in the roadmap are all contingent on the data and subject to change.
Returning face-to-face education in schools and colleges is a national priority. The Government has taken the difficult decision to restrict attendance in these education settings only when it has been absolutely necessary to control the virus and save lives. Returning to face-to-face education in schools and colleges must therefore be the first step in exiting this lockdown. The sequencing of easing will be driven by the evidence on sources of transmission. Outdoor activity has been prioritised because the likelihood of COVID-19 transmission is substantially lower in the open air than indoors. This restores more freedom to people more quickly while minimising the impact on transmission.
The Four Tests
Before taking each step, the Government will review the latest data on the impact of the previous step against four tests. The tests are:
-
The vaccine deployment programme continues successfully.
-
Evidence shows vaccines are sufficiently effective in reducing hospitalisations and deaths in those vaccinated.
-
Infection rates do not risk a surge in hospitalisations which would put unsustainable pressure on the NHS.
-
Our assessment of the risks is not fundamentally changed by new Variants of Concern.
Figure 8: The Four Tests
The Four Tests
- Test 1: The vaccine deployment programme continues successfully.
- Test 2: Evidence shows vaccines are sufficiently effective in reducing hospitalisations and deaths in those vaccinated.
- Test 3: Infection rates do not risk a surge in hospitalisations which would put unsustainable pressure on the NHS.
- Test 4: Our assessment of the risks is not fundamentally changed by new Variants of Concern.
The Roadmap steps
Step 1
Figure 9: Step 1
Step 1: 8 March
- Schools and colleges are open for all students. Practical Higher Education Courses.
- Recreation or exercise outdoors with household or one other person. No household mixing indoors.
- Wraparound childcare.
- Stay at home.
- Funerals (30), wakes and weddings (6)
29 March
- Rule of 6 or two households outdoors. No household mixing indoors.
- Outdoor sport and leisure facilities.
- Organised outdoor sport allowed (children and adults).
- Minimise travel. No holidays.
- Outdoor parent & child groups (up to 15 parents).
On the basis of the Government’s assessment of the current data against the four tests, Step 1 can proceed. Step 1 will start with schools on 8 March, and include some further limited changes on 29 March to allow families to meet outdoors as most schools break up for the Easter holidays. By the time Step 1 begins, those aged 70 and over and the clinically extremely vulnerable (JCVI cohorts 1 to 4) will have received protection from their first dose of the vaccine.
The Government has always said that returning face-to-face education in schools and colleges is a national priority. The decision to restrict face-to-face attendance in education and wraparound childcare settings has been taken only where it has been absolutely necessary to control the virus and save lives. The Government knows that being in face-to-face education is the best place for pupils and students. Returning children and young people to face-to-face education is, therefore, the first step in easing this lockdown.
There is clear evidence that time out of education can be detrimental to children’s future prospects and earning potential, with implications also for long-term productivity. [footnote 50] The Institute for Fiscal Studies (IFS) analysis also found that hours worked among all parents halved in May 2020 compared to 2014-15. Returning to face-to-face education in schools is therefore a priority of the Government, as it will minimise the substantial economic and social costs that have been associated with restricting face-to-face learning. [footnote 51]
Pupils and students in all schools and Further Education settings will return to face-to-face education from 8 March. Wraparound childcare (including childminders) and other children’s activities can restart from 8 March for all children where it is needed to enable parents or carers to work, seek work, attend education, seek medical care or attend a support group. Vulnerable children can attend these settings regardless of circumstance. Under-18 sport can take place at school as part of educational provision, or as part of wraparound care, but should not otherwise take place at this time.
On 27 January, the Prime Minister committed to providing a huge programme to help recover lost learning, recognising that the disruption of this year has had a major impact on children. This will involve a further £300 million on tutoring programmes, building on last year’s £1 billion COVID-19 Catch Up fund, as well as potential plans for summer schools developed in partnership with the education sector. The Government has also announced the appointment of Sir Kevan Collins as the Education Recovery Commissioner, to oversee a comprehensive programme of recovery aimed at young people who have lost out on learning due to the pandemic. He will be addressing factors such as curriculum content and quantity of teaching time in the coming months, to ensure the impact the pandemic has had on learning is addressed as quickly and comprehensively as possible. [footnote 52]
Students on practical Higher Education courses at English universities who would be unable to complete their courses if they did not return to take part in practical teaching, access specialist facilities, or complete assessments will also return from 8 March. Research labs and libraries can be kept open if needed.
For those Higher Education students that do not need to take part in practical teaching, and do not require access to specialist facilities or equipment as part of their studies, the Government will review, by the end of the Easter holidays, the options for timing of the return of these students. This will take account of the latest data and will then be a key part of the wider roadmap steps. Students and institutions will be given a week’s notice ahead of any reopening. The Government recognises the difficulties and disruption that this may cause for many students and their families where they remain unable to return to Higher Education settings, but it is necessary to limit the number of students who return to university at this stage to minimise travel and manage the risk of transmission. The Government has made available an additional £70 million of hardship funding this financial year, which universities can use to support students impacted by COVID-19.
The successful return of more learners to face-to-face education and childcare settings will be supported by a range of new measures, designed to minimise the spread of COVID-19. The Government applauds the huge efforts made by pupils and students, early years practitioners, teachers, lecturers and support staff to implement protective measures. The risk of transmission will be reduced by implementing the system of controls endorsed by PHE which the Department for Education will work with schools to implement. In addition to the already established rapid testing regime and regular testing of staff, there will be twice-weekly testing of secondary school and college pupils, initially with on-site testing and then home testing. All households with school children, members of their support and childcare bubbles, and those in related occupations will also be encouraged to get tested regularly.
The Government also recommends that the use of face coverings in Higher Education, Further Education and secondary schools is extended for a limited period to all indoor environments - including classrooms - unless 2m social distancing can be maintained. Face coverings are now also recommended in early years and primary schools for staff and adult visitors in situations where social distancing between adults is not possible, for example, when moving around in corridors and communal areas. All children will once again be expected to attend school, as they were in the autumn term.
From 8 March, the Stay at Home restriction will continue but it will be amended so that people can leave home for recreation as well as exercise outdoors - with their own household, support or childcare bubble, or with one person from another household. Social distancing and other safe behaviours should be followed.
In England, travel abroad for holidays will still not be permitted and, from 8 March, outbound travellers will be legally obliged to provide their reason for travel on the Declaration to Travel form.
Safe and secure elections are the cornerstone of the UK’s democracy and the Government has confirmed that COVID-Secure council, mayoral and police and crime commissioner elections will go ahead on 6 May in England and Wales. The Government has published a delivery plan for the May elections [footnote 53] setting out how local elections teams will be supported to deliver effective polls that are COVID-Secure for voters and staff. The Government will amend the regulations to enable a broader range of campaign-related activity from 8 March, but it is essential that this still takes place in a COVID-Secure way, in line with guidance and the law. The Government will be publishing further guidance for candidates, their agents and political parties on campaigning in the elections in due course, and will be engaging with the Parliamentary Parties Panel on this guidance shortly to ensure the views of political parties are taken into account. Elections are also taking place in Scotland and Wales. The Scottish and Welsh Governments are responsible for their elections with the exception of the Police and Crime Commissioner Elections in Wales. The Government is working closely with the Scottish and Welsh Governments to support the delivery of these elections.
From 8 March, every care home resident in England will be able to nominate a single named visitor who can come in for a regular visit. The visitor will have to take a rapid lateral flow test every time they visit, wear PPE and keep physical contact to a minimum. Further detail on support for care home residents and staff is in chapter 5.
As before, people can leave home for work if they cannot work from home and to escape illness, injury or risk of harm, including domestic abuse.
From 29 March there is an opportunity for some further limited changes as part of Step 1, as most schools start to break up for the Easter holidays.
By then, the lockdown will have been in place for twelve weeks, during which time people will have been unable to see their extended family and friends or spend much time outside the home. At this point, the Government will enable people to meet up in limited numbers outdoors, where they are less likely to catch the virus or pass it on.
People will be able to meet outside in groups up to a maximum of 6 people (the Rule of 6) or with one other household, though people from different households will still need to socially distance from each other. This will apply in all outdoor settings, including private gardens. Applying either limit provides greater flexibility, recognising the different situations faced by families and individuals; two households will be more helpful for families, while the Rule of 6 is likely to help people in different households to reunite outdoors, including those living alone or in shared accommodation. Those eligible to form a support bubble will still be able to do so, enabling close contact for many of those in most need of support, and will continue to be counted as part of the same household.
Guidance will set out how people can see others safely: the evidence is clear that this is safest to do in the open air, at a safe distance, while minimising the frequency of social gatherings and the numbers present wherever possible. It will remain critical - with most people still unprotected by vaccines - that people continue to follow the guidance, use common sense and socially distance from other households.
The Government will also allow outdoor sports facilities to reopen, broadening the options for outdoor exercise and recreation. These facilities, such as tennis and basketball courts, and swimming pools, can be used by people in line with the wider social contact limits. Formally organised outdoor sports – for adults and under 18s - can also restart and will not be subject to the gatherings limits, but should be compliant with guidance issued by national governing bodies.
All children will be able to access any outdoor childcare and supervised activities. Parent and child groups can also take place outdoors with a limit of 15 attendees (children under five years of age do not count towards the attendee limit.)
Children will still only be able to attend indoor childcare or supervised activities where doing so will allow parents or carers to work, seek work, attend education, seek medical attention or attend a support group. Vulnerable children can already attend these settings regardless of personal circumstance and the Government will also ensure any other child eligible for Free School Meals will be able to do so - ensuring they can attend those that are part of the Holiday Activities and Food Programme (HAF) running over the Easter holidays.
Rules around funerals will not change; these can proceed with 30 attendees and wakes with 6 attendees, though not in private homes. Weddings will still be able to proceed with 6 attendees only but will no longer be limited to exceptional circumstances.
As a result of these changes, people will no longer be legally required to Stay at Home. Many of the lockdown restrictions, however, will remain in place. Unless an exemption already applies, it will not be possible to meet people from other households indoors and many business premises will remain shut. Guidance will set out that people should continue to work from home where they can. People should continue to minimise travel wherever possible, and should not be staying away from home overnight at this stage.
Outdoor vs Indoor transmission
-
Airborne transmission is a significant route by which COVID-19 passes between people. Particles of the virus can build up and circulate in the air in the form of aerosols in enclosed spaces (even if they are large) especially where air exchange is poor. [footnote 54] This makes indoor settings more risky than outdoors, where the fresh air quickly disperses the virus to safe levels. This is confirmed by observational studies tracing people infected with COVID-19 which shows the majority of transmission occurs in indoor settings and that ‘super spreader’ events (where many people are infected at one time) are more likely indoors than outdoors. [footnote 55]
-
Though the airborne risk of COVID-19 transmission is much lower outdoors than inside, the risk of infection via larger droplets remains high if people engage in prolonged, face-to-face close contact with others. [footnote 56] Therefore, maintaining 2m distancing outdoors is still advisable. Outdoor surfaces may also still become contaminated with the virus, so it is also important to be mindful of what shared objects, e.g. playground surfaces and gate handles, are touched, and to maintain regular hand washing.
Socio-economic analysis of Step 1
-
Restricting face-to-face education has had significant and adverse impacts on children’s learning, development and mental health. By February 2021 half term, studies suggest the total loss in face-to-face learning could amount to around half a school year, with two thirds of a normal year lost if school reopening were to be delayed to after Easter.
-
As well as benefiting students directly, parents will no longer have to balance childcare and working from home. Around 53% of parents report a reduced ability to work as a result of school closures; this is more acutely felt by parents of early years and primary aged children.[footnote 57]
-
Sports, amusement and recreational activities were worth an estimated £12.8 billion in the UK in 2019 (£11 billion in England),[footnote 58] providing around 565,000 jobs (484,000 in England).[footnote 59] The easing of measures could enable some of these activities to return and take advantage of the spring/summer season and recover lost revenues. These businesses are particularly important employers for young people, with 37% of their workforce between 16 to 24 years old (compared to a national average of 11%).[footnote 60]
-
Opening outdoor sports settings will help to reduce the adverse physical and mental health effects experienced by large parts of the population, in particular children and those living alone. Exercise and outdoor sports are well documented to reduce individuals’ risk of major illnesses, such as heart disease, stroke, type 2 diabetes and cancer by up to 50% and lower risk of early death by up to 30%.[footnote 61] Physical activity is also known to help with improving mental health through better sleep, happier moods, and managing stress, anxiety or intrusive and ‘racing’ thoughts.[footnote 62]
-
Restrictions on socialising have had an adverse impact on people’s wellbeing and mental health with nearly half of adults (49%) reporting boredom, loneliness, anxiety or stress arising due to the pandemic.[footnote 63]
Step 2
Figure 10: Step 2
Step 2
At least five weeks after Step 1, no earlier than 12 April.
- Indoor leisure (including gyms) open for use individually or within household groups.
- Rule of 6 or two households outdoors. No household mixing indoors.
- Outdoor attractions such as zoos, theme parks and drive-in cinemas.
- Libraries and community centres.
- Personal care premises.
- All retail.
- Outdoor hospitality.
- All children’s activities, indoor parent & child groups (up to 15 parents).
- Domestic overnight stays (household only).
- Self-contained accommodation (household only).
- Funerals (30), wakes, weddings and receptions (15).
- Minimise travel. No international holidays.
- Event pilots begin.
As set out above, around four weeks is required to see the impact of the previous step in the data and the Government has committed to provide a further week’s notice to businesses. Step 2 will therefore take place no earlier than 12 April, subject to an assessment of the data against the four tests. If Step 2 is delayed, subsequent steps will need to be pushed back in order to maintain the necessary five week period to assess the impact of each step and provide notice.
This step will reopen some sections of our indoor economy and more outdoor settings, restoring jobs and livelihoods and enabling people to access some of the activities and services which are most important to them.
Social contact rules in England will not change further at this point. Outdoor gatherings must still be limited to 6 people or 2 households as in Step 1, and no indoor mixing will be allowed unless otherwise exempt.
Additional premises will be able to reopen but should only be visited alone or with household groups: non-essential retail; personal care premises such as hairdressers, salons and close contact services; and indoor leisure facilities such as gyms and spas (but not including saunas and steam rooms, which are due to open at Step 3). Overnight stays away from home in this country will be permitted and self-contained accommodation - those that do not require shared use of bathing, entry/exit, catering or sleeping facilities - can also reopen, though must only be used by members of the same household. The Government will open public buildings such as libraries and community centres. Activities such as driving tests may also resume.
The majority of outdoor settings and attractions can also reopen, including outdoor hospitality, zoos, theme parks, drive-in cinemas and drive-in performances events. The rules on social contact outdoors will apply in these settings.
Hospitality venues will be able to open for outdoor service, with no requirement for a substantial meal to be served alongside alcoholic drinks, and no curfew. The requirement to order, eat and drink while seated (‘table service’) will remain.
All newly open settings must abide by the social contact rules. The Government will continue to enforce restrictions and require businesses to demonstrate robust strategies for managing the risk of transmission and to ensure social distancing rules are followed. Local authorities and the police will continue to provide support and advice to newly reopened settings, enabling them to operate safely. Where businesses do not follow the rules, the appropriate enforcement action will be taken.
This will be accompanied by mitigations including workforce testing and continued social distancing guidance.
People should continue to work from home where they can, minimise domestic travel where they can. International holidays will still be prohibited.
At Step 2, the Government will take a decision on extending the number of care home visitors to two per resident and set out a plan for the next phase of visits.
All children will be able to attend any indoor children’s activity, including sport, regardless of circumstance. Parent and child groups of up to 15 people (not counting children aged under five years old) can restart indoors.
At this point, funerals can continue to proceed with up to 30 attendees. Weddings, receptions, and commemorative events including wakes will be able to take place with up to 15 attendees (in premises that are permitted to open).
Socio-economic analysis of Step 2
-
Non-essential retail was estimated to be worth £44.6 billion of Gross Value Added (GVA) [footnote 64] in the UK in 2019, employing around 1.2 million people.[footnote 65] Closing this sector has led to a high take-up of the furlough scheme in the wider wholesale and retail sector where use of the furlough scheme peaked at 1.9 million in April, and 740,000 at the end of November in the UK. [footnote 66] People from ethnic minorities are overrepresented in this sector, making up 16% of workers, as are young people (35% are 16 to 24). Women also make up a greater proportion of employees (66% compared to 47% nationally). [footnote 67]
-
Hospitality is a core part of the UK’s economy. The whole Accommodation and Food Services sector was estimated to be worth £57.6 billion in the UK 2019 (£48.5 billion in England), providing jobs for 2.5 million people (2.1 million in England). This sector has been one of the hardest hit by the pandemic: GVA output fell by 91% in April and 89% in May 2020, compared to February 2020.[footnote 68] The November restrictions also hit the hospitality sector hard, with GVA falling back to 65% below its pre-pandemic level. This sector has also had large parts of its workforce on furlough: in the first wave 1.6 million jobs were furloughed at its peak; at the end of November 1.1 million jobs in this sector were on furlough. Between 25 January and 7 February, 62% of businesses in accommodation and food services had paused trading.[footnote 69]
-
Personal care activities accounted for £21.1 billion in the UK in 2019 (£18.9 billion in England), providing 566,000 jobs (507,000 in England). Women are significantly overrepresented in this sector, making up 85% of the workforce.
-
Public buildings and spaces play a vital role in the economic and social life of communities. Libraries, and other community centres, are valuable and safe places, often to the most vulnerable groups in society. They provide both services to local communities and spaces to socialise. All public spaces have important benefits that help create local attachments and sense of belonging to a community.
Step 3
Figure 11: Step 3
Step 3
At least five weeks after Step 2, no earlier than 17 May.
- Indoor entertainment and attractions.
- 30 person limit outdoors. Rule of 6 or two households (subject to review).
- Domestic overnight stays.
- Organised indoor adult sport.
- Most significant life events (30).
- Remaining outdoor entertainment (including performances).
- Remaining accommodation.
- Some large events (expect for pilots) - capacity limits apply.
- Indoor events: 1,000 or 50%.
- Outdoor other events: 4,000 or 50%.
- Outdoor seated events: 10,000 or 25%.
- International travel - subject to review.
Step 3 will take place no earlier than 17 May, and at least five weeks after Step 2, following a further review of the data and the four tests. Again, the Government will announce one week in advance whether restrictions will be eased as planned.
In Step 3, all but the most high-risk sectors will be able to reopen. In all sectors, COVID-Secure guidance will remain in place and premises must not cater for groups larger than the legal limits. Sectors which will reopen include:
a. Indoor hospitality, with no requirement for a substantial meal to be served alongside alcoholic drinks, and no curfew. The requirement to order, eat and drink while seated (‘table service’) will remain;
b. Remaining outdoor entertainment, such as outdoor theatres and cinemas;
c. Indoor entertainment, such as museums, cinemas and children’s play areas;
d. Remaining accommodation, such as hotels, hostels and B&Bs;
e. Adult indoor group sports and exercise classes; and
f. Some large events, including conferences, theatre and concert performances and sports events. Controlled indoor events of up to 1,000 people or 50% of a venue’s capacity, whichever is lower, will be permitted, as will outdoor events with a capacity of either 50% or 4,000 people, whichever is lower. The Government will also make a special provision for large, outdoor, seated venues where crowds can be safely distributed, allowing up to 10,000 people or 25% of total seated capacity, whichever is lower. In addition, pilots will run as part of the Events Research Programme to examine how such events can take place without the need for social distancing using other mitigations such as testing (see paragraphs 132 to 134).
At this step, weddings, receptions, funerals, and commemorative events including wakes can proceed with up to 30 attendees. A broader range of stand-alone life events will also be permitted at this step, including bar mitzvahs and christenings.
At Step 3, the Government will further ease limits on social contact, enabling the public to make informed personal decisions. It will remain important for people to consider the risks for themselves, taking into account whether they and those they meet have been vaccinated or are at greater risk.
The Government will continually review the evidence of vaccine efficacy, including its impact on transmission. As soon as possible, and no later than Step 3, the Government will update its advice on social distancing between friends and family, including hugging. Until then, people should continue to keep their distance from anyone not in their household or support bubble, and keep up habits such as regular hand washing and letting in fresh air.
The Government will lift most legal restrictions on meeting others outdoors, but gatherings of more than 30 people outdoors will remain illegal. Indoors, people will be able to meet socially in a group of 6, or with 1 other household, though it may be possible to go further than this at Step 3 depending on the data. People will be asked to follow guidance on how to meet safely, for example by minimising the size of gatherings and meeting outdoors where possible.
The Government will continue to advise the public to work from home where they can. The Government will work closely with the Devolved Administrations who will have their own respective rules and regulations on travel in Northern Ireland, Scotland and Wales. The Global Travel Taskforce will report on 12 April with recommendations aimed at facilitating a return to international travel as soon as possible while still managing the risk from imported cases and Variants of Concern. Following that, the Government will determine when international travel should resume, which will be no earlier than 17 May.
Socio-economic analysis of Step 3
-
The arts, entertainment and recreation sector (excluding sports, amusement and recreation) has been hit very hard by the pandemic. Pre-COVID-19, this sector was worth £18.3 billion GVA UK wide (£15.5 billion in England) and had 473,000 jobs (400,000 in England). GVA output in the arts, entertainment and recreation sector as a whole compared to February fell by 46% in April, and subsequently to 33% in November; in no month since March has output been above 77% of pre-pandemic levels.[footnote 70] The sector as a whole has also had a high take-up of the furlough scheme, with 455,000 furloughed at peak in spring, and 293,000 furloughed at the end of November. Between 25 January and 7 February, 44% of businesses in the arts, entertainment and recreation sector have paused trading.[footnote 71] Reopening these sectors can allow these businesses to recover revenues and bring back employees.
-
The relaxation of social contact rules is likely to have a positive impact on wellbeing as people will be able to socialise and meet friends and family indoors for the first time in several months. Restrictions on social contact have had adverse mental health and wellbeing impacts.
Step 4
Figure 12: Step 4
Step 4
At least five weeks after Step 3, no earlier than 21 June. By Step 4, the Government hopes to be able to introduce the following (subject to review):
- No legal limits on social contact
- Nightclubs.
- Larger events.
- No legal limit on life events.
Step 4 will take place no earlier than 21 June, and at least five weeks after Step 3, following a further review of the data against the four tests. As before, the Government will announce one week in advance whether restrictions will be eased as planned.
With appropriate mitigations in place, by Step 4, the Government aims to:
a. Remove all legal limits on social contact, publishing accompanying guidance on how best to reduce the risk of transmission and protect ourselves and loved ones;
b. Reopen the remaining closed settings, including nightclubs and enable large events, including theatre performances, above the Step 3 capacity restrictions, subject to the outcome of the scientific Events Research Programme (set out in paragraphs 132 to 134) and potentially using testing to reduce the risk of infection, subject to further evaluation; and
c. Remove all limits on weddings and other life events, subject to the outcome of the scientific Events Research Programme.
As set out above, some measures may be required even after all adults have been offered a vaccine, because neither coverage nor effectiveness of the vaccine will be 100%. As a result, a significant proportion of the population will remain vulnerable to infection, some of whom will also be vulnerable to severe disease and death. This is reflected in the modelling of different scenarios for unlocking restrictions, which shows that the risk of further cases, hospitalisations and deaths remains after the adult population has been vaccinated, though modellers advise there is considerable uncertainty in these figures.
The Government is therefore establishing four programmes of work to consider different aspects of how the UK should handle COVID-19 from summer onwards.
COVID status certification
COVID status certification involves using testing or vaccination data to confirm in different settings that people have a lower risk of transmitting COVID-19 to others.
The Government will review whether COVID-status certification could play a role in reopening our economy, reducing restrictions on social contact and improving safety. This will include assessing to what extent certification would be effective in reducing risk, and the potential uses to enable access to settings or a relaxation of COVID-Secure mitigations. The Government will also consider the ethical, equalities, privacy, legal and operational aspects of this approach and what limits, if any, should be placed on organisations using certification. It will draw on external advice to develop recommendations that take into account any social and economic impacts, and implications for disproportionately impacted groups and individuals’ privacy and security. The Government will set out its conclusions in advance of Step 4 in order to inform the safe reopening of society and the economy.
Large events
DCMS and the Department for Business, Energy and Industrial Strategy have been working with representatives from industry and civil society to explore when and how events with larger crowd sizes, less social distancing or in settings where transmission is more likely (i.e. indoors), will be able to return safely. This includes sports events, music festivals and large weddings and conferences.
Over the spring the Government will run a scientific Events Research Programme. This will include a series of pilots using enhanced testing approaches and other measures to run events with larger crowd sizes and reduced social distancing to evaluate the outcomes. The pilots will start in April.
The Government will bring the findings from across different sectors and different settings to determine a consistent approach to lifting restrictions on these events. Depending on the outcome of this work, the Government hopes to be able to lift restrictions on these events and sectors as part of Step 4.
International travel
The Government’s objective is to see a safe and sustainable return to international travel, for business and pleasure. When it is safe to do so the UK will again be the destination of choice for international visitors from around the world. In the short-term, the Government will continue to protect the vaccine rollout and mitigate against the risk posed by imported variants.
Vaccinations could offer a route to that safe and sustainable return. Once more is known about the evidence of vaccines on transmission and their efficacy against new variants, the Government can look to introduce a system to allow vaccinated individuals to travel more freely internationally.
The UK is working with other countries who have started similar programmes, to lead global efforts to adopt a clear international framework with standards that provide consistency for passengers and industry alike. The Government will make this a reality through ongoing work with the World Health Organisation and other multilateral organisations, the UK’s presidency of the G7 this year, and by working with other international partners.
However, any such system will take time to implement. It will be heavily dependent on improved scientific understanding about the role vaccination plays in reducing transmission. Introducing such a system also needs to be fair and not unduly disadvantage people who have yet to be offered - or gain access to - a vaccine. That being the case, the Government does not expect this solution to be available quickly, and restrictions like those in place across the world are likely to continue for the near future.
The Government recognises that international travel and tourism bring many economic and other benefits to communities across the UK. The aviation sector in the UK drives large direct exports and is a critical enabler of wider UK trade and economic activity. It facilitates around £95 billion of the UK’s non-EU trade exports,[footnote 72] directly contributes £22 billion to the UK economy[footnote 73] and supports half a million jobs. International travel is particularly important in gateway cities and underpins the competitiveness and global reach of the UK’s national and regional economies, supporting jobs in hospitality, in retail and in our world class museums, theatres and visitor attractions. It is also the case that global restrictions have hit airlines, airports, cruise and travel operators particularly hard. The resumption of safe travel will be particularly important for these businesses.
Therefore, the Government is keen to find ways to work closely with the industry to ease restrictions on international travel gradually and sustainably.
The Department for Transport will lead a successor to the Global Travel Taskforce, with an ambition to develop a framework that can facilitate greater inbound and outbound travel as soon as the time is right, while still managing the risk from imported cases and variants. This will look to take a risk-based approach, making use of the suite of measures the Government already has in place such as testing and isolation and the recommendations from the first Global Travel Taskforce last year.
The Taskforce will report to the Prime Minister and work with UK representatives of the travel sector, including airlines and airports. It will report on 12 April, with recommendations aimed at facilitating a return to international travel as soon as is possible, while still managing risk from imported cases and Variants of Concern. Following that, the Government will determine when international travel should resume, which will be no earlier than Step 3. The decision on when international travel can resume will be dependent on the global and domestic epidemiological picture, the prevalence and location of any Variants of Concern, the progress of vaccine rollouts here and abroad, and what more the Government has learned about the efficacy of vaccines on variants, and the impact on transmission, hospitalisation and deaths.
In addition, the Global Travel Taskforce run last year committed the Government to publish a Tourism Recovery Plan in support of the sector. The Government intends to set out proposals in the spring, including plans for a world class marketing campaign to welcome back visitors to the UK as soon as it is safe to do so.
Restrictions on international travel will need to remain in place for the moment. However, following the Taskforce’s report in April, the Government will take a decision on when these can be removed, which will be no earlier than Step 3 (17 May). This decision will be dependent on the global and domestic epidemiological picture, the prevalence and location of any Variants of Concern, the progress of vaccine rollouts here and abroad, and what more we have learned about the efficacy of vaccines on variants, and the impact on transmission, hospitalisation and deaths.
Social distancing
Social distancing is difficult and damaging for businesses and, as a result, it is important to return to as near to normal as quickly as possible. Ahead of Step 4, as more is understood about the impact of vaccines on transmission and a far greater proportion of the population has been vaccinated, the Government will complete a review of social distancing measures and other long-term measures that have been put in place to limit transmission. The results of the review will help inform decisions on the timing and circumstances under which rules on 1m+, face masks and other measures may be lifted. The review will also inform guidance on working from home - people should continue to work from home where they can until this review is complete.
| Step 1 | Step 2 | Step 3 | Step 4 | ||
|---|---|---|---|---|---|
| 8 March | 29 March | No earlier than 12 April. At least 5 weeks after Step 1. | No earlier than 17 May. At least 5 weeks after Step 2. | No earlier than 21 June. At least 5 weeks after Step 3. All subject to review. | |
| Education | - Schools and colleges open for all students - Practical Higher Education courses |
As previous step | As previous step | As previous step | |
| Social contact | - Exercise and recreation outdoors with household or one other person - Household only indoors |
- Rule of 6 or two households outdoors - Household only indoors |
- Rule of 6 or two households outdoors - Household only indoors |
- Maximum 30 people outdoors - Rule of 6 or two households indoors (subject to review) |
No legal limit |
| Business & Activities | - Wraparound care, including sport, for all children | - Organised outdoor sport (children and adults) - Outdoor sport and leisure facilities - All outdoor children’s activities - Outdoor parent & child group (up to 15 parents) |
- All retail - Personal care - Libraries & community centres - Most outdoor attractions - Indoor leisure inc. gyms (individual use only) - Self-contained accommodation - All children’s activities - Outdoor hospitality - Indoor parent & child groups (up to 15 parents) |
- Indoor hospitality - Indoor entertainment and attractions - Organised indoor sport (adult) - Remaining accommodation - Remaining outdoor entertainment (including performances) |
- Remaining businesses, including nightclubs |
| Travel | - Stay at home - No holidays |
- Minimise travel - No holidays |
- Domestic overnight stays (household only) - No international holidays |
- Domestic overnight stays - International travel (subject to review) |
- Domestic overnight stays - International travel |
| Events | - Funerals (30) - Weddings and wakes (6) |
- Funerals (30) - Weddings, wakes, receptions (15) - Event pilots |
- Most significant life events (30). - Indoor events: 1,000 or 50% - Outdoor seated events: 10,000 or 25% - Outdoor other events: 4,000 or 50% |
- No legal limit on live events - Larger events |
4. Keeping people safe and responding to threats
Behaviours
Even as restrictions are lifted, it is essential that everyone carries on with the good habits that reduce transmission: remembering ‘hands, face, space’ and letting fresh air in, getting a test on the first sign of symptoms and self-isolating if it is positive. It is safer to meet outdoors and to avoid large gatherings.
Businesses must also continue to take necessary precautions as restrictions ease. The overwhelming majority of the businesses that remained open during the pandemic did so in a COVID-Secure way. The Government will update COVID-Secure guidance to provide further advice on how businesses can improve fresh air flow in indoor workplaces and introduce regular testing to reduce risk. Local authorities will also continue to offer advice.
As England moves through the roadmap steps, the Government will continue to monitor existing enforcement powers and modify them if necessary. The police and local authorities are able to take action against people who break the law and apply sanctions, for those businesses that are not operating safely.
Figure 13: Safe Behaviours
Safe Behaviours
- Wash hands frequently, for at least 20 seconds.
- Wear a face covering in enclosed environments.
- Maintain space with anyone outside your household or bubble.
- Meet with others outdoors where possible.
- Minimise the number of different people you meet and the duration of meetings, if possible.
- Let fresh air in.
- Download the NHS Test & Trace app.
- Get a test immediately if you have symptoms.
- Self isolate if you have symptoms, have tested positive, or had contact with someone with COVID-19.
Test, Trace and Isolate
The Test, Trace and Isolate system will help to support the easing of social and economic restrictions and keep people safe.
NHS Test and Trace, working in partnership with PHE, local authorities, businesses, schools, universities and others, now has capacity for approximately 800,000 PCR (polymerase chain reaction) tests per day, across the UK [footnote 74]. As the virus becomes less prevalent, the Test, Trace and Isolate system will become ever more important in identifying local outbreaks rapidly, allowing the Government to take swift action to manage them and respond to new Variants of Concern.
Current Test, Trace and Isolate system
Over 80 million PCR tests have been conducted - more than one for every person living in the UK.[footnote 75] More than 85% of in-person tests now return results the next day, an improvement of more than 52% since December, and the median distance travelled to one of over 850 test sites is approximately 2 to 3 miles.[footnote 76]
As around 1 in 3 people with COVID-19 do not have symptoms, the Government has established widespread asymptomatic testing. This is conducting around 2.4 million rapid tests per week, including to all NHS and Adult Social Care staff and, since January, all school staff.
Tracing performance has also improved. Between 4 and 10 February, 93.6% of close contacts were reached and told to self-isolate, compared to 60% in October. Over 90% were reached within 72 hours of the person they were in close contact with testing positive. This work is done in close partnership with local authorities, with over 300 local contact tracing partnerships in place.
The NHS Test and Trace COVID-19 App has been downloaded over 21 million times and, since September, has notified over 1.7 million users across England and Wales to isolate.[footnote 77] Developments continue in response to user feedback, including the introduction of a ‘book a test’ venue alert. The App also helps the public to understand how best to protect themselves, makes it easy for users to check in to venues and sends alerts that users may have been exposed to COVID-19 at a venue they have visited.
The Government has also deployed new tools to support people to self-isolate, including making available £110 million for the Test and Trace Support Payment.
Responding to Variants of Concern and intervening locally
All viruses regularly mutate as they replicate to create new ‘variants’. Most mutations have no effect and are not a cause for any concern. Some, however, pose an increased risk to public health due to changes in transmissibility, infection severity, ability to evade immune responses, or the virus’s susceptibility to therapeutic treatments. These variants can be detected within the country - as with the B.1.1.7 variant - or imported from abroad.
The UK is a global leader in genome sequencing, which in positive cases allows the identification of Variants of Concern, and continues to scale up its capacity. The Government is also working with diagnostics providers to adapt PCR tests to detect specific Variants of Concern once they have been identified. This, combined with whole genome sequencing, should enable mutations to be detected more rapidly, enabling action to be taken. The UK will also provide sequencing support for other countries should they need it, helping to track variants wherever they appear in the world and in turn shaping the UK’s border policies. Despite this progress, the risks posed by Variants of Concern remain significant. Identifying and determining the extent of the risk posed by a new variant may take some time, during which it could spread through the community, making it essential that the Government is able to act in a sensible and proportionate way as the evidence is still emerging.
Where a dangerous Variant of Concern is identified and is likely to pose a real risk to the vaccination programme or public health, the Government will take a highly precautionary approach, acting fast to address outbreaks. The Government is developing an enhanced toolkit of measures to address Variants of Concern, including surge PCR testing, enhanced contact tracing, communications and targeted enforcement
The Government cannot rule out reimposing economic and social restrictions at a local or regional level if evidence suggests they are necessary to contain or suppress a variant which escapes the vaccine.
Where an area sees virus growth which could put the local NHS under unsustainable pressure, the Government will also act swiftly. Local authorities and public health leaders have been at the forefront of efforts to tackle the virus in our communities. While the Government is now in a position to look towards an easing of restrictions, it is important to continue to support local authorities to keep doing their most important public health work in responding to the virus over the coming months.
The Government is therefore announcing a further £400 million funding for the Contain Outbreak Management Fund (COMF) from 1 April, taking total COMF support across 2020-21 and 2021-22 to £2 billion. This is to cover further public health activities in 2021-22, and further details will be announced in due course. In March, the Government will publish an updated COVID-19 contain outbreak management framework for local areas, which will set out how national and local partners will continue to work with the public at a local level to prevent, contain and manage outbreaks. This will include details of the enhanced toolkit of measures to address Variants of Concern.
Testing: going further
Table 3: Testing - going further
| Testing strand | Status |
|---|---|
| Workplace testing: twice-weekly testing for all those unable to work from home. | Testing available for all who have to leave the home for work. |
| Community Testing: local authority-led testing available at asymptomatic test sites on an ongoing basis. | Testing live in over 260 local authorities in England. |
| NHS frontline staff: twice-weekly home testing. | Testing live. |
| Care homes: three tests a week for staff, monthly PCR testing for residents. | Testing live. |
| High-risk extra care and supported living: three tests a week for staff, monthly PCR testing for residents. | Testing will go live from late February. |
| Domiciliary carers: weekly testing. | Testing live. |
| Schools and colleges: twice-weekly testing of teachers and secondary school and college pupils. | Live for teachers - full rollout for pupils from 8 March. |
| Universities: twice-weekly testing for all students and staff currently on-site. | Testing live. |
| Hauliers: testing to enable cross-border travel. | Testing live. |
| Other settings (including prisons and hospices): mix of PCR and rapid testing | Testing live. |
Rapid testing in education settings is now well established, with more than 3 million rapid COVID-19 tests conducted in schools and colleges in England since 4 January. This includes two tests for those secondary school pupils and college students who have returned, and regular testing for all staff. At universities, 600,000 tests have also been taken on site since last year; they are encouraged to offer twice-weekly tests to everyone attending.[footnote 78] When more pupils and students return to face-to-face education in schools and colleges on 8 March the Government will introduce twice-weekly testing of secondary school and college pupils, starting with testing on site in the first two weeks and then home testing. All households with school children, members of their support and childcare bubbles, and those in related occupations will also be encouraged to get tested regularly.
In January, the Government offered regular asymptomatic testing for people who have to leave home for work, to reduce risk to individuals and keep businesses open. A major effort across the private and public sector has already resulted in interest from over 12,000 UK organisations, with over three million tests distributed to employers. The Government’s offer of free test kits to workplaces for staff who cannot work at home will be extended to until the end of June. Organisations, including those yet to open, will need to register interest before 31 March. The Government will keep this under review as vaccine deployment continues and will investigate how testing could be used to support the recovery.
Workplace testing case study:
Apetito was an early adopter of workplace testing. While testing is voluntary, early engagement with staff has meant an extremely high participation rate: only one member of the cohort of staff initially invited has opted not to take part. Having begun with 500 staff involved in manufacturing and distribution, they have now expanded to their delivery drivers. Having conducted over 5,000 tests, positivity is around 1.2% - meaning they have found 66 asymptomatic cases they would otherwise not have found, allowing their business to continue functioning effectively, and to continue providing meals to vulnerable groups, with greater safety for both customers and staff.
The Community Testing Programme is also being extended until at least the end of June. Launched in December 2020, as a partnership between national and local government, this rapid testing scheme was expanded in January for all local authorities in England to use and nearly all have now joined. This enables asymptomatic testing for local public services, small businesses, self-employed people and communities that have been disproportionately affected by the virus.
A new Community Collect model will be launching so that families, small businesses and the self-employed - who have found it harder to access regular testing - can take away rapid tests from some Government and local authority sites. People will also soon be able to have rapid lateral flow tests delivered straight to their home, allowing them to carry out tests when it is most convenient. This will provide ready access to rapid lateral flow tests for those who require access to regular testing.
NHS Test and Trace will continue to improve the Tracing system, based on feedback from users and even stronger partnerships with local authorities.
The Government will also expand support for those self-isolating. While self-isolation is critically important to halting the spread of the disease, it is never easy for those affected. The Test and Trace Support Payment Scheme will continue into the summer, and will be expanded to cover parents who are unable to work because they are caring for a child who is self-isolating, and the funding made available for local authorities as part of this to make discretionary support payments will be increased to £20 million per month. There will be more funding too to help local authorities ensure people self-isolating have access to practical support, such as food deliveries or help with their caring responsibilities, and support for wellbeing. In addition, the Medicines Delivery Service that has been established to help clinically extremely vulnerable people will be extended to provide essential deliveries for self-isolators without access to alternatives.
Building a Test, Trace and Isolate system for the future
As regular testing will have a key role to play in future, the Government is working to establish an effective private market for tests. Providers must meet a regulatory framework so that the public can have confidence in these tests and the Government will set up new validation processes for new tests to the private market.
In time, it is possible that testing becomes a viable alternative to self-isolation for contacts of infected people. The emergence of new variants has meant this is not yet feasible, but the testing programme is being primed to deliver this when the time is right. The evaluation, which has thus far involved around 12,000 people across 21 organisations and 180 sites, will be expanded in the coming months and include a large-scale programme with schools.
Measures at the border
Managing the risk of new cases entering the UK has become even more important with the rise of new variants across the world. The UK already has in place a strong set of measures. All passengers, from any country, must have completed their Passenger Locator Form and comply with an extensive programme of testing. Every inbound passenger is now required to provide proof of a negative test result before departure, to take a test on days two and eight after arriving in the UK and before they end isolation. Genomic sequencing of all positive tests is undertaken to seek to catch any new variants.
In addition, the only travellers allowed into the country from “red list” countries (those that pose the highest risk of imported new variants) will be residents of the UK and Ireland. On arrival they must isolate for 10 days in the new Managed Quarantine Service. They are also subject to the same testing requirements as other arrivals. The Government also has in place - in partnership with carriers - a strong set of checks to ensure that everyone is complying with these requirements and doing their part to keep people safe when travelling to the UK.
These measures offer protection in the current context. The Government will act swiftly if evidence emerges that suggests more countries should be added to the “red list”. Likewise, if evidence emerges that vaccines deployed in the UK are sufficiently effective against Variants of Concern (or the situation in those countries changes) countries may also be removed.
This regime enables the UK to manage the risk of importing new cases and new variants. However, there will come a point where these restrictions will need to be superseded by a more facilitative model, making greater use of assets like the Test to Release Scheme, which allows arrivals to end isolation early if they pay for a private COVID-19 test. The Global Travel Taskforce’s report will be critical to this, after which the Government will determine when international travel should resume, which will be no earlier than 17 May.
5. Economic and social support
Since the emergence of COVID-19, the Government has taken swift action to save lives, support the NHS and mitigate damage to the economy. The Government has put in place an unprecedented economic package which has provided businesses and individuals with support and certainty over the course of the pandemic.
The Government has spent over £280 billion to support people’s jobs, businesses, and public services across the UK.[footnote 79] At the Summer Economic Update, the Government announced further support for businesses, individuals and public services, and in response to the public health restrictions put in place over the winter, the Government announced additional measures in the Winter Economy Plan and the Spending Review.
The Government’s world-leading economic response to COVID-19 is the largest package of emergency support in post-war history. As highlighted by the OBR and the Bank of England, without the action taken by the Government, the outlook would be much worse.
For example, the furlough scheme has helped to pay the wages of people in 9.9 million jobs in the UK, with £46.4 billion being paid out in grants, protecting jobs which may otherwise have been lost, while grants for the self-employed have paid out £18.5 billion.[footnote 80] [footnote 81] The Government has also provided a wide range of loan schemes, business grants, business rates relief, tax cuts, mortgage holidays, increased welfare support, tax deferrals, and the Kickstart and Restart schemes.
This is all part of a comprehensive Plan for Jobs protecting, creating and supporting employment in every region and nation of the UK. As the public health situation has developed with new variants emerging, the Government has also ensured that businesses and people have certainty by extending furlough and business grants.
Economic support
The Government is committed to do whatever it takes to support the country through the COVID-19 pandemic and support will continue.
The 3 March Budget will outline the next stage in the Government’s Plan for Jobs including further detail on economic support to protect jobs and livelihoods across the UK.
The approach will reflect the steps set out in the roadmap: as restrictions ease and the economy is gradually and safely reopened, the Government will carefully tailor the level of support to individuals and businesses to reflect the changing circumstances.
Despite unprecedented levels of financial help, the Government also recognises that it will not be possible to preserve every job or business. So the Government will continue to help people to find new jobs, acquire new skills or start new businesses as we build back better from the pandemic.
The Government was able to provide significant economic support because the UK entered this crisis with strong public finances. As the Chancellor of the Exchequer has set out previously, it is not sustainable to borrow at this current level over the medium term. This means the Government has a responsibility, once the economy recovers, to return to a sustainable fiscal position.
Support for the most vulnerable
There are around 4 million people in England identified as Clinically Extremely Vulnerable and therefore at high risk of serious illness or death should they become infected with COVID-19. This includes 1.7 million Clinically Extremely Vulnerable individuals who have been identified through a new risk prediction model, QCovid, which takes into account health and personal factors, and can identify someone who is at a higher risk from COVID-19.[footnote 82] This group has been prioritised for vaccination.
Everyone who has been made aware they are Clinically Extremely Vulnerable is currently advised to follow shielding guidance, limiting time outside the home to exercise and attending medical appointments only. There is separate advice for people who are Clinically Extremely Vulnerable who live in Scotland, Wales or Northern Ireland. The Government anticipates that it will no longer be necessary to advise shielding beyond the end of March 2021. The Government will confirm advice and next steps nearer the time to keep Clinically Extremely Vulnerable people safe.
There is a further group of people who have been identified as Clinically Vulnerable, and as such at moderate clinical risk of serious illness or death should they become infected with COVID-19. People who are Clinically Extremely Vulnerable or Clinically Vulnerable are prioritised for vaccination. The Government’s expectation is that vaccination will offer vulnerable people increased protection from becoming seriously ill. The Government is considering the long-term support that may be needed for the Clinically Extremely Vulnerable, particularly for those who cannot be vaccinated or do not receive a significant increase in immunity from the vaccine.
Support for care home residents and staff
The Government recognises the enormous effort of all those working in Adult Social Care who have worked tirelessly over the past year to protect some of those most vulnerable to COVID-19. The extra pressures this year has brought cannot be underestimated. That is why alongside extensive efforts at a local level, the Government has stepped in to support the social care sector and workforce. This includes £4.6 billion of emergency grant funding to local authorities to address the pressures on local services caused by the pandemic and over £1.1 billion paid out through the Infection Control Fund to support providers to prevent and control transmission of COVID-19.[footnote 83]
The Adult Social Care Winter Plan set out the steps the Government is taking to support care providers to protect people in care, including those with learning disabilities, from COVID-19. For example, care home staff are now being tested twice weekly with rapid lateral flow tests in addition to a weekly PCR test, and free PPE is being provided to the social care sector until the end of June, with this offer now being extended to unpaid carers. Over the winter the Government provided £120 million additional funding to help local authorities boost staffing levels and £149 million to support rapid testing of staff and facilitate visits from family and friends (prior to the current restrictions coming into force).[footnote 84] The Government will continue to work closely with the sector to support it in protecting staff, residents and carers from COVID-19. The success of the vaccine programme means that 95% of eligible older adult care home residents have been vaccinated, which equates to 89% of all older adult care home residents. With the impact of the current restrictions and adherence to infection control measures, the number of outbreaks in care homes has been falling steadily since the beginning of January.[footnote 85]
While the vaccine is bringing much needed hope and protection, until more is known about its impact on transmission, people in need of care and their carers should continue to adhere to all infection control measures that are in place now. The risks may be higher with new and emerging variants that are more transmissible and there is a need to monitor the effectiveness of the vaccine on these new variants.
However, the Government recognises that visits from loved ones are crucial for the wellbeing of care home residents of all ages, and their families and friends, which is why the roadmap includes more opportunities for visiting. From 8 March every care home resident will be able to nominate someone who can come in for regular visits. However, when the data shows it is safe, the Government wants to go further and allow more visitors. At Step 2 of the roadmap the Government will look carefully at the effectiveness of the vaccine for people living in care homes, as well as levels of infection in the local community, especially of any new variants. The Government will take a decision at that point on extending the number of visitors to two per resident, as in December, and set out a plan for the next phase of visits for people in residential care.
In addition to these new measures, care homes should continue to allow visits for other loved ones through arrangements such as substantial screens, visiting pods, visits behind windows or outdoor visiting. In the event of an outbreak in a care home, the home should immediately stop visiting (except in exceptional circumstances such as end of life) to protect residents, staff and visitors who might be vulnerable to COVID-19. More detail on these changes will be published in updated guidance in the week of 1 March.
The Government also recognises that some residents need more support. Residents with, for example, advanced dementia, learning difficulties or Autism, may need a particular trusted person to perform some personal care tasks. Without this support, their health may be in danger of deteriorating very rapidly. In this type of situation, the Government will provide extra support to those visitors, whose visit is essential to the resident’s immediate health and wellbeing and who are providing personal care, like help with washing and dressing or eating well. With the agreement of the care home, these visitors will have access to the same testing and PPE as care home staff so that they can play this important caring role. More detail on these changes will be published in updated guidance to support care homes to facilitate visits for residents and their loved ones.
Additional testing will also be provided to facilitate safer visits for residents in high risk Supported Living and Extra Care settings. It remains the case that many residents in Supported Living and Extra Care settings will be able to receive visits by forming a support bubble.
The Government recognises the vital role unpaid carers play, especially during this difficult period, and recognises the need for support groups (including day services) to continue. Organised groups of up to 15 people can therefore continue to meet and free PPE will continue to be available through local authorities or local resilience forums to support staff working in day services. In addition, the Government is providing regular testing for staff in high-risk day services to support them to continue to operate as safely as possible.
Disproportionately impacted groups
The Government recognises that some groups within society have felt the impact of the pandemic more acutely, and that ongoing restrictions and requirements will fall unequally. There are groups which have been disproportionately affected during the pandemic. These include ethnic minorities, with wave one deaths for Black African, Pakistani and Bangladeshi men 4.5, 2.7 and 3.5 times higher respectively than White British men of the same age, and continued high rates of mortality (4.8 and 4.1) among Pakistani and Bangladeshi communities in wave two.[footnote 86] Also those in high-risk occupations such as taxi drivers[footnote 87] and social care workers and those living in the most deprived areas where first wave mortality rates for men and women were more than double those in the least deprived areas.[footnote 88] In addition, indicative estimates for those with disabilities, suggest that more disabled women were 1.4 times, more-disabled men 1.1 times, and men and women with a medically diagnosed learning disability 1.7 times more likely to die from COVID-19 than non-disabled people of the same sex. These estimates take account of factors such as underlying health conditions and geographical circumstances but as yet no single factor can be identified to explain the increased risks. Across all of these groups, multiple underlying socio-economic factors contribute to high case and death rates[footnote 89].
The Government has put in place a number of measures to mitigate disproportionate impacts. As the Government eases restrictions, it will ensure that those who have been worst hit by COVID-19 are protected and supported, and that the unequal impacts of COVID-19 continue to be addressed. This includes:
a. Increasing community testing in disproportionately impacted groups and for the employees of small businesses and workforce testing in higher risk occupations.
b. Providing local authorities with key vaccine data to help them to counter mis-information around vaccines in communities. Mis-information disproportionately affects some ethnic minority groups. The Government will also encourage the voluntary sector to support the vaccine rollout at the community level.
c. Protecting those in high risk institutional settings such as prisons, residential settings for asylum seekers and immigration detention centres. The Government will expand testing capacity in prisons, provide guidance in a range of languages for asylum seekers to support for self-isolation and introduce safety measures in institutional settings or accommodation for vulnerable people.
d. Providing additional support for those facing indirect impacts of COVID-19 including supporting domestic abuse and safeguarding services, and disadvantaged students recovering from lost learning.
e. Ensuring support is available for individuals facing disproportionate impacts on their mental health and wellbeing. In addition to the Wellbeing and Mental Health Support Plan for COVID-19, published last year, the Government will publish an Action Plan setting out further measures to respond to and mitigate the impacts on mental health across the population.
f. Protecting rough sleepers. The Government has committed funding to 2022 for local authorities to protect rough sleepers. The focus is on providing long-term sustainable support to local authorities, through the Rough Sleeping Initiative and the Rough Sleeping Accommodation Programme.
g. Supporting vulnerable families. The £170 million Covid Winter Grant Scheme was announced on 8 November and is now being delivered by local authorities to support vulnerable families in need this winter and beyond.[footnote 90] This will be extended until the end of the Easter holidays (16 April 2021). This Government will also support families with disabled children as restrictions are lifted.
The Government is committed to tackling obesity and other comorbidities that pose an additional risk for severe outcomes in people with COVID-19. The ‘Better Health’ campaign was launched last year to encourage people to embrace a healthier lifestyle and to lose weight if they need to, with a range of evidence-based tools and apps providing advice and support.
The Government is committed to addressing the longer-term implications of COVID-19 for communities that have been disproportionately impacted, some of which were already disadvantaged before the pandemic. The Government is drawing on the knowledge and expertise of medical professionals and the best available evidence to develop and test new approaches to control the spread of the virus in order to protect affected individuals, communities and the NHS.
6. Long term
Transition from pandemic to endemic
Over time, scientists expect COVID-19 to become endemic, meaning the virus will reach a stable, and hopefully manageable level. It may have seasonal surges. Scientists do not yet know how or when that transition will occur.
Vaccines will be key to managing the transition from pandemic to endemic state. Therapeutics and antivirals will also be increasingly important and replace most non-pharmaceutical interventions over the long term.
Living with the virus
Like some strains of flu, COVID-19 is a relatively mild illness for much of the population, but it is more dangerous to vulnerable groups. The Government will ensure the country can live with the virus in the longer-term without imposing restrictions which bear heavy economic, social and health costs. The outcome of the four programmes of work set out in chapter 3 (large events, COVID-Certification, international travel and social distancing) will inform Government policy on living with the virus.
In addition to a comprehensive revaccination programme, set out in chapter 2, the Government will also use the Test, Trace and Isolate system to keep the virus in check. This includes regular asymptomatic testing in sectors with the highest risk of transmission, as well as testing in the workplace to help protect employees from infection and keep businesses open. The UK has already stepped up domestic production of lateral flow tests. As set out in chapter 2, the Government is also investing in bolstering domestic vaccine production capacity across the whole of the UK.
Building resilience to future pandemics
To build resilience in the health system for any future pandemics, the Government is on track to establish the National Institute for Health Protection (NIHP) in April 2021. This new organisation will be responsible for monitoring, identifying and ensuring our nation’s readiness to respond to public health hazards. Combining the health protection capabilities of PHE with NHS Test and Trace, including the UK-wide Joint Biosecurity Centre (JBC), and building on the experiences of tackling COVID-19, the Government will transfer staff and systems into the new organisation over the following months. At a local level, local authorities and Directors of Public Health, working with PHE, will continue to work to manage local outbreaks engaging closely with their communities. They are supported by the national COVID-19 contain outbreak management framework, which sets out how national and local partners work with the public to prevent, manage and contain outbreaks.
The Government will also continue to ensure that any plans for future pandemics are multi-sectoral. Although the health and social care system is central to responding to a pandemic, all Departments and partners are critical to a response and will continue to improve resilience for any future pandemics.
International leadership
On the international stage, the UK is leading on a global approach to preventing future pandemics. At the UN General Assembly in September 2020, the Prime Minister set out the UK’s Five Point Plan focusing on:[footnote 91]
a. A global network of zoonotic research hubs to spot new pandemics before they begin, by identifying pathogens before they leap from animals to humans;
b. Increased research and development and manufacturing capacity for treatments and vaccines to ensure tried and tested treatments are ready to deploy against emerging threats;
c. Improved horizon scanning and early warning systems making best use of data and cutting-edge technology;
d. Strengthened protocols and guidance for dealing with health emergencies and strengthened ability to share evidence and devise new guidance during a crisis; and
e. Reduced trade barriers that have impeded the COVID-19 response.
This year, the UK will use its G7 Presidency to lead the global recovery from COVID-19, including by calling for a new, global approach to pandemics with further international cooperation on vaccine distribution and finance, while strengthening the world’s resilience against future pandemics.
As set out in chapter 2, the health of every country depends on the whole world having access to safe and effective vaccines, therapeutics and diagnostics (VTDs). The UK is supporting international efforts to widen access to new vaccines, therapeutics and diagnostics for COVID-19, and to deliver equitable access to vaccines to people living across the globe. The UK will continue to work closely with global bodies to ensure that developing countries can access COVID-19 vaccines, treatments and tests, and will use its G7 presidency to encourage other countries to do likewise.
-
https://www.gov.uk/government/news/uk-government-secures-additional-40-million-doses-of-valneva-vaccine ↩
-
https://coronavirus.data.gov.uk/details/deaths. Data up to 11 February 2021. ↩
-
https://coronavirus.data.gov.uk/details/healthcare?areaType=nation&areaName=England ↩
-
https://www.ons.gov.uk/peoplepopulationandcommunity/healthandsocialcare/conditionsanddiseases/bulletins/coronaviruscovid19infectionsurveypilot/12february2021 ↩
-
https://coronavirus.data.gov.uk/details/healthcare, https://coronavirus.data.gov.uk/details/death ↩
-
https://www.ons.gov.uk/economy/grossdomesticproductgdp/bulletins/gdpfirstquarterlyestimateuk/octobertodecember2020 ↩
-
ONS, A05 SA: Employment, unemployment and economic inactivity by age group (seasonally adjusted), January 2021 ↩
-
ONS, A09: Labour market status by ethnic group, November 2020 ↩
-
ONS, A05 SA: Employment, unemployment and economic inactivity by age group (seasonally adjusted), January 2021 ↩
-
ONS, Labour market in the regions of the UK: January 2021 ↩
-
UCL, COVID-19 Social Survey Week 46-47, 11 February 2021 ↩
-
Parent Ping Survey, January 2021 ↩
-
UCL COVID-19 Social Study: Depression and anxiety 23 March 2020 - 7 February 2021. ↩
-
Bank of England, Monetary Policy Report - November 2020. OBR, Economic and fiscal outlook – November 2020 ↩
-
NHS workforce statistics - https://digital.nhs.uk/data-and-information/publications/statistical/nhs-workforce-statistics/october-2020 ↩
-
Press release on nursing students: https://www.hee.nhs.uk/coronavirus-covid-19/hee-covid-19-student-data-collections-support-paid-placement-deployment ↩
-
Press release on medical studentshttps://www.hee.nhs.uk/news-blogs-events/news/support-shown-time-need-staggering ↩
-
NHS Digital HES monthly data: https://app.powerbi.com/view?r=eyJrIjoiZjQ2MjhmZTEtZDViOS00OWY0LTg3OGQtYmI0NWU5ODZhODM3IiwidCI6IjUwZjYwNzFmLWJiZmUtNDAxYS04ODAzLTY3Mzc0OGU2MjllMiIsImMiOjh9
Cancer waiting time statistics: https://www.england.nhs.uk/statistics/statistical-work-areas/cancer-waiting-times/ ↩
-
https://www.gov.uk/government/news/huge-increase-in-uk-personal-protective-equipment-production ↩
-
https://www.gov.uk/government/statistics/ppe-deliveries-england-8-february-to-14-february-2021/experimental-statistics-personal-protective-equipment-distributed-for-use-by-health-and-social-care-services-in-england-8-february-to-14-february-2 ↩
-
https://www.nihr.ac.uk/news/185-million-awarded-to-new-research-projects-to-understand-and-treat-long-covid/26895 ↩
-
https://www.gov.uk/government/publications/regulatory-approval-of-pfizer-biontech-vaccine-for-covid-19 ↩
-
https://www.gov.uk/government/publications/regulatory-approval-of-covid-19-vaccine-astrazeneca ↩
-
https://www.gov.uk/government/publications/regulatory-approval-of-covid-19-vaccine-moderna ↩
-
Vaccine Task Force ↩
-
These figures, and the figures in the table below, do not account for over 800,000 people who will now be prioritised for vaccination having been identified as high risk through the QCovid risk prediction model. ↩
-
NHS England, COVID19 Hospital Activity https://www.england.nhs.uk/statistics/statistical-work-areas/covid-19-hospital-activity/ ↩
-
NHS England, COVID19 Hospital Activity https://www.england.nhs.uk/statistics/statistical-work-areas/covid-19-hospital-activity/ ↩
-
As at 10 January 2021, based on NHSEI data for England, extrapolated to the UK. DHSC, UK COVID-19 vaccines delivery plan, 11 January 2021. ↩
-
As of 19th of February - https://coronavirus.data.gov.uk/details/vaccinations ↩
-
https://coronavirus.data.gov.uk/details/vaccinations. NHSE started publishing daily vaccine stats on 10 January 2021 ↩
-
PHE https://www.gov.uk/government/https://www.gov.uk/government/collections/immunisation-against-infectious-disease-the-green-book ↩
-
ONS, Opinions and Lifestyle Survey (COVID-19 module), January 2021 ↩
-
DHSC, UK COVID-19 Vaccine Uptake Plan, 13 February 2021 ↩
-
https://www.gov.uk/government/news/community-champions-to-give-covid-19-vaccine-advice-and-boost-take-up ↩
-
The source for all figures on vaccine effectiveness, except where otherwise indicated, is: https://www.gov.uk/government/publications/phe-monitoring-of-the-effectiveness-of-covid-19-vaccination ↩
-
https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(21)00448-7/fulltext ↩
-
Adapted from 210217 SPI-M-O summary of modelling on roadmap scenarios. Illustration of potential vaccine coverage. Figure demonstrates a steady state of vaccine effectiveness, once vaccines are fully rolled out. This is not a projection and assumes 100% uptake by those eligible (i.e. no hesitancy). Assumes 84% vaccine efficacy against severe disease. Assumes that vaccine efficacy in SPI-M-O summary is equivalent to real-word vaccine effectiveness. “Ineligible” group is mostly those under 18 years of age. ↩
-
https://www.gov.uk/government/news/new-vaccines-partnership-to-rapidly-respond-to-new-virus-variants ↩
-
https://www.g7uk.org/pm-announces-100-day-target-to-create-new-vaccines/ ↩
-
https://www.gov.uk/government/news/uk-raises-1bn-so-vulnerable-countries-can-get-vaccine ↩
-
The RECOVERY trial ↩
-
The RECOVERY trial and the REMAP-CAP trials ↩
-
The RECOVERY trial https://www.recoverytrial.net/news/tocilizumab-reduces-deaths-in-patients-hospitalised-with-covid-19 ↩
-
https://www.gov.uk/government/news/new-commissioner-appointed-to-oversee-education-catch-up ↩
-
https://www.gov.uk/government/publications/may-2021-polls-delivery-plan ↩
-
PHE Transmission Group: S0921 Factors contributing to risk of SARS-CoV2 transmission associated with various settings (pdf, 1,011 KB) 18th December 2020 ↩
-
SAGE: Analysis of SARS-CoV-2 transmission clusters and superspreading events, 3rd June 2020 ↩
-
SAGE EMG: Application of physical distancing and fabric face coverings in mitigating the B117 variant SARS-CoV-2 virus in public, workplace and community, 14th January 2021 ↩
-
Parent Ping Survey, January 2021 ↩
-
ONS, GDP output approach – low-level aggregates, February 2021 - (England GVA figures have been approximated from UK values) ↩
-
ONS, JOBS03: Employee jobs by industry, December 2020; ONS, JOBS04: Self-employment jobs by industry, December 2020 - (England jobs figures have been approximated from UK values) ↩
-
ONS, Employment by detailed occupation and industry by sex and age for Great Britain, UK and constituent countries 2018, May 2019 ↩
-
Mind: Physical activity and your mental health, March 2019 ↩
-
ONS, Coronavirus and the social impacts on Great Britain: 13 November 2020 ↩
-
Gross Value Added (GVA) is a measure of the value of the production of goods and services. ↩
-
ONS, Industry (2, 3 and 5 - digit SIC) - Business Register and Employment Survey (BRES): Table 2, November 2020 (Non-essential retail figure is only for employment and does not include self-employed jobs) ↩
-
HMRC,Coronavirus Job Retention Scheme statistics: January 2021 ↩
-
ONS, Estimates of the number of people aged 16 years and over in employment by occupation, sex and ethnicity, England, January 2017 to December 2019 ↩
-
ONS, Business insights and impact on the UK economy: 11 February 2021 ↩
-
ONS, GDP monthly estimate, UK: December 2020 ↩
-
ONS, Business insights and impact on the UK economy: 11 February 2021. ↩
-
https://publications.parliament.uk/pa/cm5801/cmselect/cmtrans/745/74502.htm ↩
-
https://www.gov.uk/government/news/governments-multimillion-pound-support-scheme-for-airports-opens-today ↩
-
https://www.gov.uk/government/news/nearest-testing-site-now-on-average-under-2-miles-away ↩
-
https://www.gov.uk/government/news/nhs-covid-19-app-alerts-17-million-contacts-to-stop-spread-of-covid-19 ↩
-
https://www.gov.uk/government/news/over-3-million-rapid-coronavirus-tests-in-schools-and-colleges ↩
-
https://www.gov.uk/government/collections/hmrc-coronavirus-covid-19-statistics#coronavirus-job-retention-scheme ↩
-
https://www.gov.uk/government/collections/hmrc-coronavirus-covid-19-statistics#self-employment-income-support-scheme (total of tranche 1,2,3) ↩
-
Factors include: as age, ethnicity and BMI, as well as certain medical conditions and treatments. ↩
-
https://www.gov.uk/government/publications/adult-social-care-coronavirus-covid-19-winter-plan-2020-to-2021/adult-social-care-our-covid-19-winter-plan-2020-to-2021 ↩
-
https://www.gov.uk/government/news/social-care-to-receive-269-million-to-boost-staff-levels-and-testing ↩
-
https://www.gov.uk/government/statistics/national-flu-and-covid-19-surveillance-reports ↩
-
Nafilyan et al, Ethnic differences in COVID-19 mortality during the first two waves of the Coronavirus Pandemic, February 2021 ↩
-
ONS: COVID-19 deaths by job sector, August 2020 ↩
-
PHE: Disparities in the risk and outcomes of COVID-19, August 2020 (pdf, 2.8 MB) ↩
-
ONS: Updated estimates of coronavirus (COVID-19) related deaths by disability status, February 2021 ↩
-
https://www.gov.uk/government/news/new-winter-package-to-provide-further-support-for-children-and-families ↩
-
https://www.gov.uk/government/news/prime-minister-world-must-unite-to-defeat-covid-and-prevent-future-pandemics ↩
