Mpox: background information
The background, symptoms, diagnosis and management of mpox virus infections.
See the mpox collection page for further resources including guidance for health professionals.
Origin and spread of mpox
Mpox is an infectious disease that is caused by the MPXV virus.
Mpox was first discovered in 1958 when outbreaks of a pox-like disease occurred in monkeys kept for research.
The first human case was recorded in 1970 in the Democratic Republic of the Congo (DRC). Since then the infection has been reported in a number of African countries and, more recently, has spread to multiple countries around the world. This includes cases in the UK.
There are 2 major types of MPXV. These are called clades and are known as clade I and clade II. Clade I was previously known as Central African or Congo basin clade, after the places it was originally found. Clade II was previously known as West African clade.
Sub-types of each clade have been identified. Clade I is split into clade Ia and clade Ib. Clade II is split into clade IIa and clade IIb. These can be broken down further into groupings called lineages. This is important as we can track different outbreaks of mpox around the world by looking at the exact type of the mpox viruses involved.
Historically, mpox was known to have been occasionally passed on from infected animals to humans, with humans sometimes passing it on to other people that they had close contact with. Since May 2022 however, cases of human mpox have been reported in multiple countries that have not previously had MPXV in animal or human populations. This has included cases in the UK. This ongoing outbreak is mostly caused by clade IIb, lineage B.1 MPXV, and is spread mostly by sexual contact.
Since August 2024, clade I MPXV has also been reported from multiple countries outside of the African region that had not previously reported it, including cases in the UK. This is mostly caused by clade Ib MPXV, and is spread mostly through close physical contact (including both sexual and non-sexual contact).
Further information on the epidemiology of mpox in the UK is available in the mpox epidemiological overview.
Information on countries currently affected by mpox is available and updated regularly by UKHSA.
Transmission
Mpox does not spread easily between people unless there is close contact.
Spread between people may occur through:
- direct contact with rash, skin lesions or scabs (including during sexual contact, kissing, cuddling or other skin-to-skin contact)
- contact with bodily fluids such as saliva, nasal mucus or semen/vaginal fluids
- contact with clothing, linen (such as bedding or towels) or other objects and surfaces used by someone with mpox
It is possible that mpox may spread between people through close and prolonged face-to-face contact such as talking, breathing, coughing, or sneezing close to one another. However, there is currently limited evidence so this will be updated as new information is available.
Spread of mpox may also occur when a person comes into close contact with an infected animal (rodents are believed to be the primary animal source for transmission to humans), or materials contaminated with the virus. Mpox has not been detected in animals in the UK.
Clinical features
The incubation period is the time between contact with the person with mpox and when the first symptoms appear. The incubation period for mpox is between 5 and 21 days.
Most people who catch mpox will recover within several weeks without any treatment. However, severe illness can occur in some individuals.
The illness begins with:
- fever
- headache
- muscle aches
- backache
- swollen lymph nodes
- chills
- exhaustion
- joint pain
However, not all people who have mpox experience all of these symptoms.
Within 1 to 5 days after the appearance of fever, a rash develops, often beginning on the face then spreading to other parts of the body including the soles of the feet and palms of the hands. The rash can also affect the mouth, genitals and anus.
The rash is made up of a variable number of lesions. These lesions change and go through different stages, shown in the images below. The lesions finally form scabs which eventually fall off.
Some individuals may not have a widespread rash, and in some cases only genital lesions are present.
Someone who has mpox is contagious until all the scabs have fallen off and there is intact skin underneath. The scabs may also contain infectious virus material.
Images of individual mpox lesions
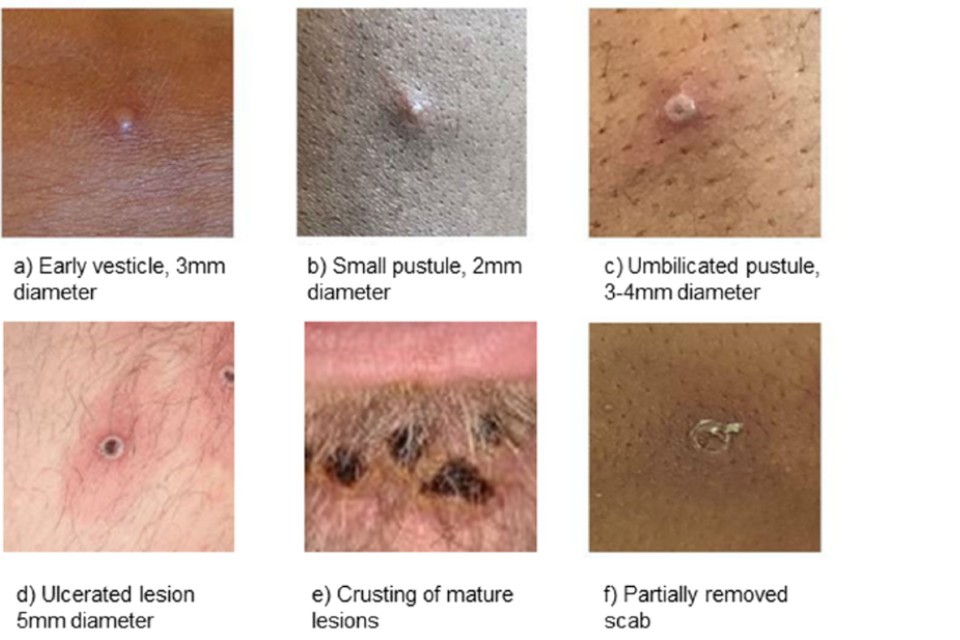
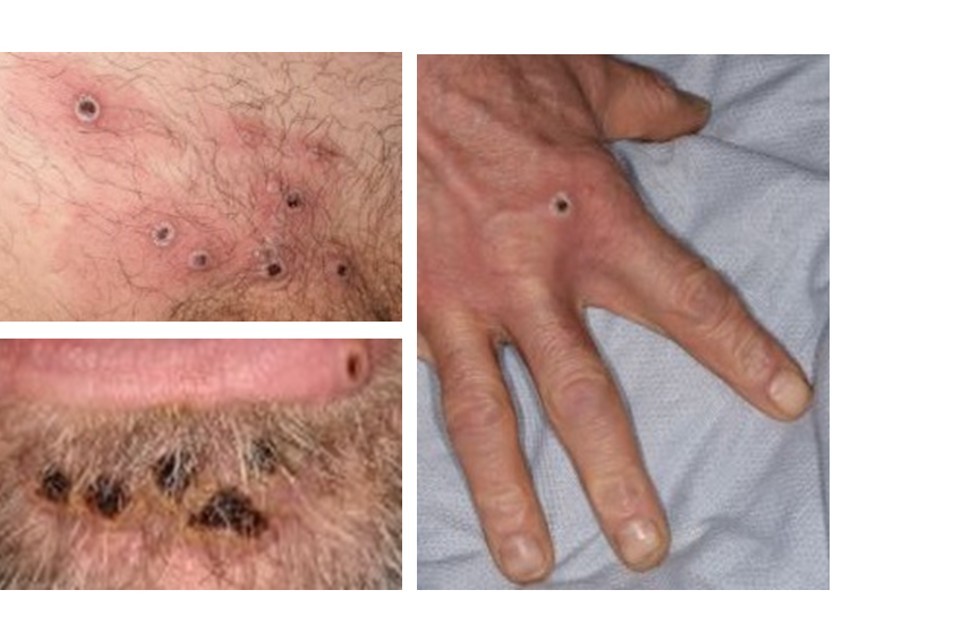
Notes
The lesions may have areas of redness or darker patches of skin around them. Lesions on black or brown skin may be harder to see.
Lesions can vary in size and may be larger than those shown in these images.
Lesions of different appearances and stages may be seen at the same point in time. The scabs that fall off may be considerably smaller than the original lesion.
Diagnosis
Diagnosis of mpox can be difficult, and it is often confused with other infections such as chickenpox. A confirmed diagnosis of mpox requires assessment by a health professional and specific testing in a specialist laboratory. See the information on when to suspect mpox, including actions for suspected cases.
In the UK, testing is available at the UKHSA Rare and Imported Pathogens Laboratory (RIPL), national laboratories in the devolved administrations and some NHS and private laboratories.
Unless clade testing is available locally, all positive samples should be forwarded to RIPL for clade testing as part of ongoing surveillance. Samples from suspected and confirmed cases of mpox should be shipped as Category B diagnostic samples. See guidance on diagnostic testing for information on how to submit samples for testing.
Treatment
Treatment for mpox is mainly supportive, which means it is aimed at treating the symptoms while your body fights the infection.
Antiviral drugs such as cidofovir and tecovirimat can be used to treat mpox patients with severe disease or those who are at high risk of severe disease.
Smallpox vaccine can be used to reduce the likelihood of infection in high risk groups and to support the control of outbreaks of mpox. While it may not prevent infection entirely, people vaccinated against smallpox (including in childhood) may experience a milder disease.
Infection prevention and control
Appropriate precautions are essential when managing suspected and confirmed cases, therefore prevention of transmission by contact and respiratory routes is required. Scabs are also infectious and care must be taken to avoid infection through handling bedding and clothing. Information on infection prevention and control measures within healthcare settings is available in the National Infection Prevention and Control Manual for England.
Mpox virus is classified as an ACDP Hazard Group 3 pathogen and all laboratory work with live virus must be conducted at full Containment Level 3 (CL3), in accordance with the Control of Substances Hazardous to Health Regulations 2002 (as amended). See the guidance on diagnostic testing for further information on handling specific sample types.
Laboratories must ensure that appropriate controls commensurate to CL3 are in place to minimise risk to laboratory workers so that they can safely perform laboratory tests that are essential to clinical care.
Further information
See WHO factsheet.
Additional mpox resources are also available on GOV.UK, including information on:
Updates to this page
-
Small updates to wording, disease background and naming conventions.
-
Added link to Confirmed cases of mpox clade Ib in United Kingdom page and clade I mpox contact tracing guidance.
-
Minor update to reflect the first detection of clade I mpox in the UK.
-
Updated links to direct to the NHS guidance on IPC measures for mpox cases in healthcare settings, and to the Green Book chapter 29.
-
Updated information on transmission.
-
Updated to include 2024 Clade I mpox outbreak.
-
Updated information on epidemiology, transmission, clinical features and diagnosis.
-
Updated to align with current epidemiology and diagnostic testing advice.
-
Updated information on submitting samples for testing.
-
Updated images of monkeypox lesions.
-
Added link to monkeypox guidance, moved guidance for primary care to monkeypox guidance page, and removed guidance for environmental cleaning and decontamination (incorporated into 'Principles for monkeypox control in the UK', available on guidance page).
-
Withdrew guidance for environmental cleaning and decontamination.
-
Updated guidance.
-
Added links to additional monkeypox guidance.
-
Updated guidance.
-
Updated with monkeypox case in England in December 2019.
-
Updated cleaning and decontamination guidance (v4).
-
Updated guidance on decontamination and cleaning.
-
Updated guidance for cleaning and decontamination.
-
Added guidance on environmental cleaning and decontamination.
-
Added primary care guidance.
-
First published.