Vaccine update: issue 330, June 2022, COVID-19 spring special edition
Published 10 June 2022
Applies to England
148 million doses of COVID-19 vaccine given in England
Thank you to all the vaccinators, vaccinees, and all of the teams working so hard to give the coronavirus (COVID-19) vaccinations – every one is a great step forward.
It’s been over one year and 5 months since the COVID-19 vaccination programme started across the UK. Since 8 December 2020, when Margaret Keenan became the first person in the world to receive her first vaccine there have been more than 148 million vaccinations given across the country.
We are seeing good uptake of COVID-19 spring booster vaccinations which are being offered to people aged over 75, adult care home residents and individuals aged 12 and over who are immunosuppressed. We really want to encourage anyone eligible who has not yet come forward to have their vaccines to make an appointment. Having positive vaccination conversations and signposting to trusted sources on information can help to address any concerns and build confidence to then take up the offer.
| Number of people vaccinated in the UK as of 7 June 2022 | |
|---|---|
| First dose total | 53,486,907 |
| Second dose total | 50,003,659 |
| Booster or third dose total | 40,029,374 |
| Total | 148,549,749 |
Dr Mary Ramsay, Director of Public Health Programmes, including Immunisation, UK Health Security Agency (UKHSA) said:
The continuing decline in case rates and hospitalisations is good news but it is still crucial to get vaccination. If you have yet to take up the offer of a vaccine or have missed your latest jab please come forward now.
If you are in a crowded, enclosed space it is still sensible to wear a face covering and remember to keep washing your hands regularly. If you have symptoms of a respiratory infection and a high temperature or feel unwell, try to stay at home or away from others – especially elderly or vulnerable people and pregnant women.
This issue of vaccine update focuses on all the new and revised resources published and the importance of the uptake of these resources to make sure everyone has their vaccination consent information, in a format which meets their needs. Thank you to everyone who has worked tirelessly to deliver this lifesaving programme.
Autumn COVID-19 boosters coming soon
The boosters would be for more vulnerable adults, alongside frontline social care and health workers, in order to maintain their protection over the winter against severe COVID-19.
As in autumn 2021, the primary objective of the 2022 autumn booster programme will be to increase population immunity and protection against severe COVID-19, specifically hospitalisation and death, over the winter period.
The Joint Committee on Vaccination and Immunisation’s (JCVI’s) current view is that in autumn 2022, a COVID-19 vaccine should be offered to:
- residents in a care home for older adults and staff
- frontline health and social care workers
- all those 65 years of age and over
- adults aged 16 to 64 years who are in a clinical risk group
Professor Wei Shen Lim, Chair of COVID-19 vaccination on the JCVI said:
Last year’s autumn booster vaccination programme provided excellent protection against severe COVID-19, including against the Omicron variant.
We have provided interim advice on an autumn booster programme for 2022 so that the NHS and care homes are able to start the necessary operational planning, to enable high levels of protection for more vulnerable individuals and frontline healthcare staff over next winter.
As we continue to review the scientific data, further updates to this advice will follow.
Throughout the pandemic, evidence has clearly shown that COVID-19 has disproportionately affected those in older age groups, residents in care homes for older adults, and those with certain underlying health conditions, particularly those who are severely immunosuppressed.
The JCVI will continue its ongoing review of the vaccination programme and the epidemiological situation, particularly in relation to the timing and value of doses for less vulnerable older adults and those in clinical risk groups ahead of autumn 2022.
The committee will announce its final plans for the autumn programme, including further detail on the definitions of clinical risk groups, in due course.
How you can continue to keep yourself and your loved ones safe
Vaccines
Get vaccinated to reduce your risk of catching COVID-19 and becoming seriously ill, and to reduce the risk of spreading the virus to others.
Fresh air
Letting fresh air in if meeting indoors, or meeting outside to disperse COVID-19 particles and reduce the risk of spreading the virus.
Face covering
Considerer wearing a face covering in crowded, enclosed spaces.
Stay at home if unwell
Try to stay at home if you are unwell.
Hand washing
Wash your hands regularly to limit the spread of COVID-19.
Guidance and information resources
Green book on Immunisation chapter 14a COVID-19
This chapter has been updated 22 times, please see details of the last 2 updates:
-
28 February 2022: updated to include approval of Novavax, clarification around deferral after COVID-19 infection, one-off programme for 5 to 11 year olds who are not in clinical risk groups, advice on use of the paediatric formulation in those aged 12 years, spring booster recommendations (including flexibility around timing) and expectations for an autumn booster, clarification of the management of individuals with a history of allergic reactions, updated advice on management of people who have immune thrombocytopenia (ITP) following vaccination.
-
12 January 2022: updated background to include latest data on vaccine effectiveness and booster safety; clarified and corrected chronology of booster advice. Clarified clinical advice about vaccination of 5 to 11 year olds at high risk: interchangeability of adult, fractional and paediatric doses; management of 5 to 11 year olds who are about to become immunosuppressed; advice on third primary doses for severe immunosuppression, including updated definitions for severe immunosuppression for younger children.
COVID-19 vaccinations received overseas
The COVID-19 vaccinations received overseas guide provides clinical advice on whether additional doses would be beneficial to enhance protection for those who received COVID-19 vaccinations overseas.
COVID-19 vaccinator competency assessment tool
The COVID-19 vaccinator competency assessment tool has been developed to support the training and assessment of healthcare workers involved in delivering the COVID-19 vaccine programme.
Resources for eligible patients, their parents and carers
The leaflets below are available free to order or download. They have been translated into 29 languages and in alternate formats such as large print (English), braille, British Sign Language videos and audio (English).
COVID-19 vaccination guide for parents of children 5 to 11 years of age leaflet.
What to expect after your child’s COVID-19 vaccination leaflet.
A guide for parents of children aged 5 to 11 years at high risk leaflet.
Easy-read resources for children and young people and their parents or carers are available.
Resources for children and young people aged 12 to 17 are available to download and order.
COVID-19 vaccination for those with a weakened immune system leaflet.
Social media cards
All the social media cards have been rebranded to UKHSA. Please share them in your networks. There is a set of 2 for each of the 19 languages including Ukrainian and Russian.
Social media resources promoting COVID-19 vaccination in migrant communities in London and nationally are available to download.
Social media resources promoting COVID-19 vaccination for pregnant women are available to download
COVID-19 Maximising Uptake vaccination programme
The Bristol, North Somerset and South Gloucestershire (BNSSG) Healthier Together COVID-19 Mass Vaccination Programme’s vision is to vaccinate all eligible people in BNSSG (population approximately 1 million) and aims to leave no one behind, particularly those at higher risk of severe illness and death from COVID-19.
Stakeholders who developed and delivered the Maximising Uptake Programme:
- BNSSG Clinical Commissioning Group (CCG)
- local authorities – Bristol, North Somerset, South Gloucestershire, and within these the BNSSG Public Health Teams
- One Care
- communities including community and faith leaders, and healthcare workers with community links
- charity sector and local voluntary groups
- Primary Care Networks (PCNs) and senior representatives
- large-scale vaccination centre leaders
- Community Interest Company: Sirona care & health
- Acute Trusts – North Bristol Trust and University Hospitals Bristol and Weston NHS Foundation Trust UK Health Security Agency (formerly Public Health England)
- Avon and Wiltshire Partnership
The programme combines strategic oversight and governance with operational groups (see structure chart below). The Maximising Uptake Programme included:
- BNSSG Gold Command
- Mass Vaccination Cell - weekly performance and oversight meetings
- NBT Trust Board (MCO)
- BNSSG CCG
- Clinical Delivery Group - daily meetings
- Partnership board - monthly strategic oversight and future planning meetings
- Maximising Uptake Group
- Task and Finish Groups
Priority group 1 – homeless
Priority group 2 – non English speaking, ethnic minorities, refugees and asylum seekers.
Priority group 3 – those living a distance from the vaccine centre; in areas of high deprivation; rural communities and Gypsy and Roma traveller population.
Priority group 4 – identified hospital patients, P3 beds.
Priority group 5 – those who may struggle to access via a vaccination centre; learning disabilities; severe mental illness; physical disabilities; drug and alcohol addiction and people with physical and sensory impairment.
To identify the 5 priority groups for maximising uptake work, national evidence on COVID-19 risk and population factors affecting vaccination uptake was combined with BNSSG data on; population health held in a system-wide dataset, influenza vaccination uptake, and insights and engagement intelligence.
Structure of the Maximising Uptake Programme and priority groups [footnote 1]
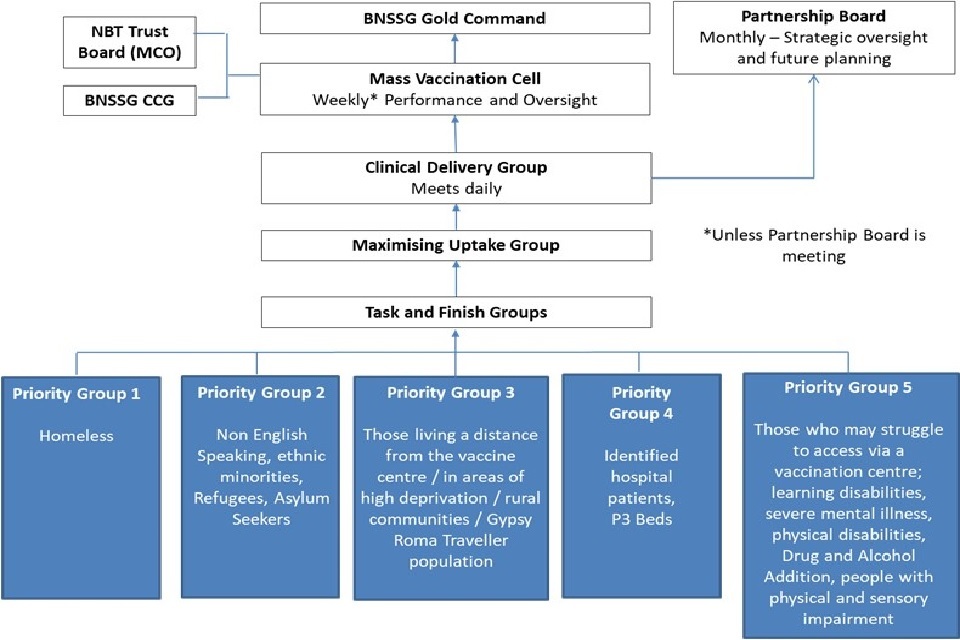
Structure of the maximising uptake programme and priority groups
There were 4 elements to the Maximising Uptake Programme, described in the table below:
| Programme element | Rationale/impact |
|---|---|
| Insight work | identify reasons for low uptake of vaccine |
| identify subgroups less likely to be vaccinated | |
| continue to improve on outreach models | |
| develop comms/engagement strategy | |
| Population health management – using data | identifying high risk for COVID-19 groups, and groups with low uptake of flu vaccines to prioritise groups for equity work |
| mapping groups geographically and to healthcare services for example PCNs | |
| iteratively testing approaches and re-evaluating priorities | |
| Communication and engagement | using trusted sources of advice regarding the vaccine |
| use most effective language and people to deliver messages | |
| comms via local media platforms, organisations and communities | |
| building trust and partnership working with communities | |
| Outreach work | pop up clinics |
| housebound visits | |
| vaccinating through existing support services | |
| taking the vaccine to vulnerable groups | |
| making adaptations to large scale COVID-19 vaccination centre appointments/ways of working |
Insights and communications
Insight work from December 2020 to May 2021 used the Clinical Commissioning Groups’ (CCGs) citizen’s panel, BNSSG public surveys, interviews with individuals from the priority groups and shared learning from South West CCGs and national forums.
Key insight findings informed the programme planning, gave practical suggestions for improving clinic access, addressing non-English language requirements, and targeting vaccination motivations and concerns. It also showed friends and family, local community and faith leaders, and healthcare professionals from within communities were the most trusted sources of advice. This informed the communication and engagement strategy.
Maximising uptake
Successfully maximising vaccine uptake in BNSSG has been through a multi-faceted approach as shown in the table below.
Outreach activity in BNSSG Maximising Uptake Programme to end May 2021.
| Outreach activity | Dates of activity | Outcomes – vaccines delivered |
|---|---|---|
| Outreach clinics | March – end May 2021 | 2,567 first doses |
| April – end May 2021 | 715 second doses | |
| Housebound vaccines by Community Interest Company Sirona care & health | to June 2021 | 1,781 vaccines (first and second doses) |
| PCN vaccinations | ongoing | unknown – delivering majority of vaccines in BNSSG, and also doing outreach/engagement work, and housebound visits |
| maximising uptake programme supported identification/outreach to priority group patients | ||
| Large scale vaccination centres | ongoing | unknown – delivering vaccines at scale and working with maximising uptake team to increase accessibility/acceptability to priority groups |
Impact
For some priority sub-groups vaccination uptake figures trended towards the BNSSG average, with trends coinciding with outreach and engagement activities.
Figure 1: Uptake of COVID-19 vaccination for lower super output areas (LSOA) of BNSSG with higher proportions of people with non-English first language or from ethnic minority groups, for JCVI cohorts 1 to 5
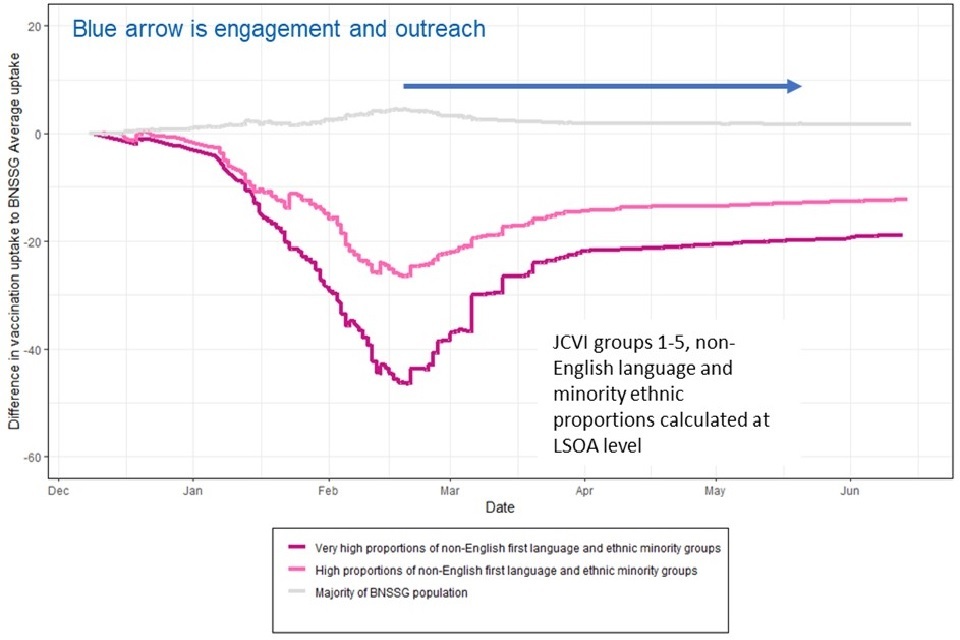
Uptake of COVID-19 vaccination for lower super output areas (LSOA) of BNSSG with higher proportions of people with non-English first language or from ethnic minority groups, for JCVI cohorts 1 to 5
In the complex context, it is difficult to attribute cause and effect. As vaccination decisions are mostly driven by influence within community networks, it is likely that both engagement work and outreach work had wider impact than is indicated by the doses delivered in the outreach clinics. Including whole programme costs, outreach vaccinations alone were delivered at a cost of £15 per dose. For reasons given above, this likely overestimates the cost per additional vaccine achieved through the overall maximising uptake programme. The evidence-based approach to prioritisation and delivery will further have increased cost-effectiveness. Figures 2 to 5 show results for the different priority groups and sub-groups, showing areas of success and where further work is needed.
Figure 2. Percentage of vaccinations (first vaccines) for homeless people compared to the remainder of the BNSSG population (JCVI cohorts 19)

Percentage of vaccinations (first vaccines) for homeless people compared to the remainder of the BNSSG population (JCVI cohorts 19)
Figure 3. Difference to BNSSG Average – percentage of first dose COVID-19 vaccinations by language group (JCVI groups 1 to 5) [footnote 2]
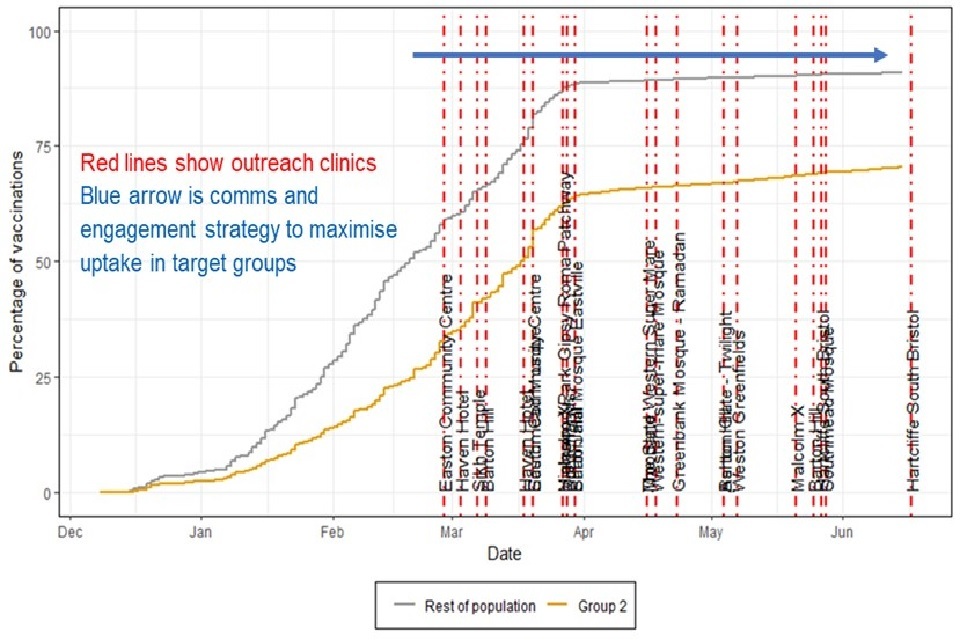
Difference to BNSSG Average – percentage of first dose COVID-19 vaccinations by language group (JCVI groups 1 to 5)
Figure 4. Difference to BNSSG Average – percentage of first dose COVID-19 vaccinations by language group (JCVI groups 1 to 5)
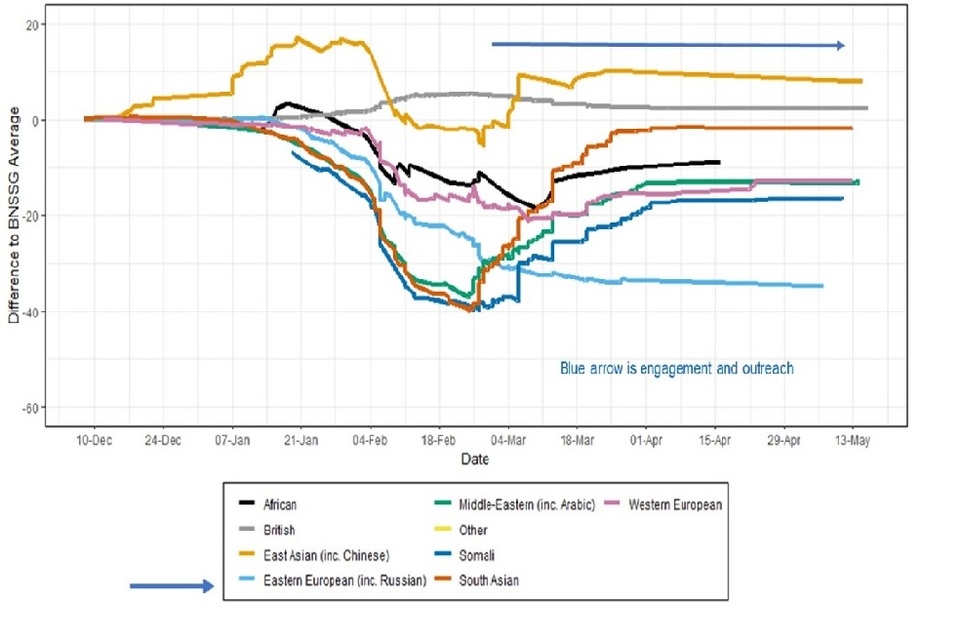
Difference to BNSSG Average – percentage of first dose COVID-19 vaccinations by language group (JCVI groups 1 to 5)
Figure 5. Percentage of COVID-19 first dose vaccinations for people in group 3 compared to the rest of the population (JCVI groups 1 to 9)
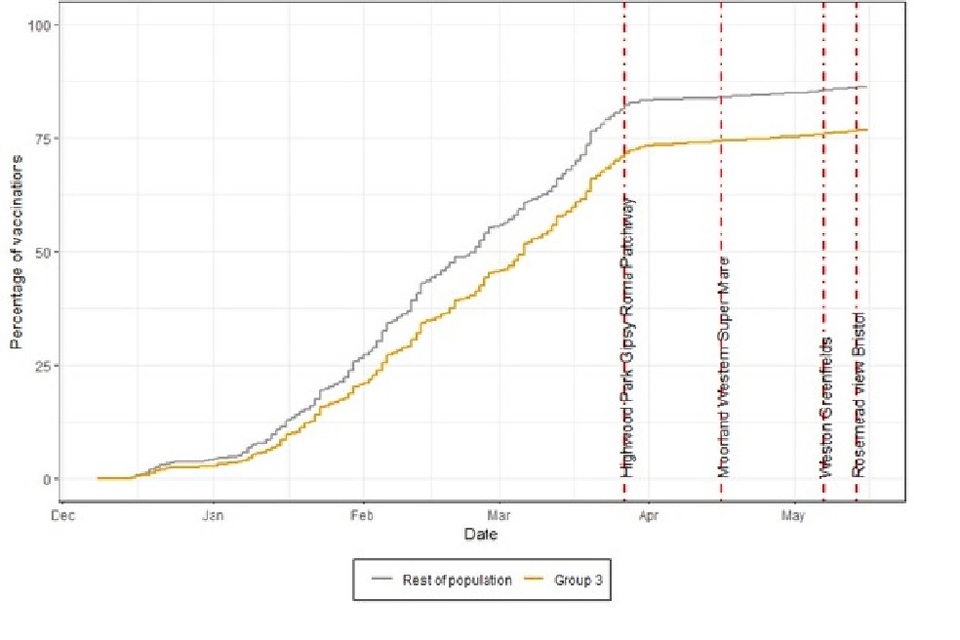
Percentage of COVID-19 first dose vaccinations for people in group 3 compared to the rest of the population (JCVI groups 1 to 9)
Uptake rates in priority group 5 sub-groups JCVI cohorts 1 to 9, to 17 May 2021
| Priority sub-group | Vaccination uptake (to 17 May 2021) |
|---|---|
| Learning disabilities [footnote 3] | 87.6% (above BNSSG average) |
| Physical disabilities [footnote 4] | 90.3% (above BNSSG average) |
| Physical and sensory impairment [footnote 5] | 92.3% (above BNSSG average) |
| Severe mental illness [footnote 6] | 80.7% (below BNSSG average) |
| Drug and alcohol dependence [footnote 7] | 76.5% (below BNSSG average) |
Successes and challenges
Partnership working between multiple stakeholders, and giving communities greater ownership, alongside an evidence-based, tailored approach to different subgroups have been critical. This programme has also been responsive to developing needs and review of the data. Successful approaches for some subgroups did not have the same impact in others. The programme has deepened its understanding of the challenges both in accessibility and acceptability of vaccination for these populations, and routes of engagement. It’s recognised that maximising uptake must remain a priority, and evaluation work will feed into this, and other vaccination/healthcare programmes.
Key findings that informed the planning included the Citizen’s panel December 2020. This showed a significant minority of around 10% said they were either unlikely to accept vaccination, or unsure. It demonstrated that locally people make vaccine decisions on a range of factors, these vary by group, and are summarised below:
Drivers and barriers to vaccination identified in local insight work
Drivers for vaccination:
- prosocial approach (protection of others)
- protection of self
- community influence
- practicalities: clinic locations, GP access
- information (and sources)
Barriers to vaccination:
- safety concerns
- lack of information
- accessibility of vaccination
- acceptability or practicality of vaccination locations
- vaccine misconceptions
- fertility concerns
- mistrust of government or other official organisations
The biggest factor in someone’s decision is speaking with trusted family and friends, as shown in this survey conducted at an outreach clinic.
Survey responses to ‘What helped you decide to get vaccinated at the outreach vaccination centre?’
| Response options | Offered vaccine previously | All respondents |
|---|---|---|
| Conversations with friends and family | 72.0% | 74.8% |
| National TV or radio news or programmes | 12.0% | 25.2% |
| Online news | 8.0% | 18.1% |
| Faith or community leader | 12.0% | 14.4% |
| WhatsApp groups | 20.0% | 13.3% |
| Conversations with my GP or other medical professional | 16.0% | 11.9% |
| The chance to have my vaccine at this venue | 4.0% | 10.4% |
| Facebook, Twitter or Instagram | 24.0% | 7.8% |
| Local TV or radio news or programmes | 4.0% | 7.0% |
| Online or printed newspapers or magazines | 0.0% | 6.3% |
| Online events such as presentations or question and answer sessions | 4.0% | 4.1% |
| Other (please specify) | 0.0% | 3.0% |
Engagement and communication strategies in the Maximising Uptake COVID-19 vaccination programme
Engagement and communications methods:
- Community champions (including >100 people with influence from black and minority ethnic (BME) and deprived communities) trained on COVID-19 and vaccines.
- MECC approach training people in libraries, one stop shop (local authority), street care.
- Written and video information in other languages.
- 6 short videos with community leaders from ethnic minority communities sharing personal experience of how they’d been affected by COVID-19, worries about vaccination.
- Templated posters for fast turnaround production to be used locally, for example in clinics encouraging people to share their vaccination experiences; publicity for walk ins; can include community leader quotes.
- Language hub on the Healthier Together website of trusted resources in 22 different languages.
- Revised wording of COVID-19 vaccine appointment text message invitations from PCNs using more positively-framed language and translated to 8 languages.
- Webinars developed for ethnic minority and disabled communities, and addressing concerns for pregnancy, breast feeding and fertility, but accessible for all demographics.
- Small scale webinars run by communities in own languages, such as in Somali community and by House of Praise, by local PCNs prior to 1st dose clinics also helped to allay concerns and get people signing up for vaccinations once they became eligible.
- Videos and leaflets in different languages.
- Community-led videos made by organisations embedded within local communities, often in community language.
- Vaccinated: pull-up banners and posters encouraging people to share their experience of being vaccinated with family and friends will be available at all vaccination clinics.
-
MCO: Management and Co-ordination Organisation ↩
-
Identified by fields “prim_language” and “ethnicity” in the system wide dataset attributes table, and supplemented by field “Ethnic Category” in NHS Digital hospital Data. Note 1: Data on asylum seekers and refuges not recorded in system wide dataset. Note 2: The ethnic description of “British of mixed British – ethnic category 2001 census” is classed as “White” in this analysis. ↩
-
Learning disability identified by fields “learning_dis”, “qof_learningdis” in the system wide dataset attributes table. ↩
-
Physical disability identified by fields “phys_disability”, “cc_hemiplehia”, “amputations” in the system wide dataset attributes table. ↩
-
Physical and sensory impairment identified by fields “visual_impair”, “hearing_impair”, “macular_degen” in the system wide dataset attributes table. ↩
-
Severe mental illness identified by field “qof_mental” in the system wide dataset attributes table. ↩
-
Drug and alcohol dependence identified by “dep_alcohol”, “dep_opioid”, “dep_cocaine”, “dep_cannabis”, “dep_benzo”, “dep_other” in the system wide dataset attributes table. Note: SWD indicates a person has ever had a problem, not necessarily currently. ↩
