Polio vaccine reminder for travellers to Israel, the West Bank and Gaza
Public Health England and National Travel Health Network and Centre (NaTHNaC) remind UK residents to make sure they are up-to-date with routine immunisations.
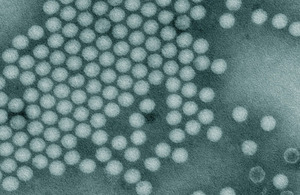
Polio virus
Travellers to Israel, or the West Bank and Gaza in Palestine, should also make sure they have had a polio containing vaccine in the past 10 years.
This follows the identification of naturally occurring or ‘wild’ poliovirus in 91 sewage samples taken from 27 sites across Israel. In addition the wild poliovirus has been identified in stool samples from 42 healthy individuals, or ‘carriers’, who are reported to have been vaccinated against polio. There have been no cases of paralysing illness caused by polio virus reported in Israel, or the West Bank and Gaza, but these findings suggest that virus is circulating in the environment and anyone who has not been vaccinated is at risk of contracting the disease.
Polio is caused by a highly infectious virus. The disease can be mild or cause no symptoms but around one in 100 infections may lead to paralytic polio - a serious illness which results in permanent disability and sometimes death. There are 3 different types of poliovirus but, following the widespread use of the vaccine, poliovirus type 2 has been eradicated. Types 1 and 3 have been eliminated from most areas of the world. Polio is contracted by eating or drinking contaminated food or water or by close contact with someone infected with the poliovirus. Polio can be prevented by having a full course of vaccination, which has been used routinely in the UK since the 1950s.
Dr Mary Ramsay, head of immunisation at PHE, said:
Israel’s last paralytic polio case was in 1988 and the World Health Organization agreed that the country was polio-free in 1992, but the fact that the virus is being found across a wide geographic area in Israel shows that it has been re-established.
Many people in the UK will already be fully immunised against polio from their routine childhood immunisations. However travellers to Israel and Palestine need to check their vaccination status before travel and should receive a booster dose if they have not had one in the past 10 years.
Dr Vanessa Field, joint director of NaTHNaC, said:
People at higher risk of exposure to polio include travellers visiting friends and relatives, long stay travellers and those visiting areas of poor sanitation, such as health workers.
Anyone who is unsure of their own or their child’s polio vaccination status should check with their GP before travel. Previous infection with polio does not mean you are immune to all types of disease.
As well as ensuring they are up-to-date with vaccinations, travellers should take strict food, water and personal hygiene precautions.
The Israeli health authorities are monitoring the situation closely. They have increased the frequency of environmental sampling and are conducting active surveillance to search for potential cases of paralytic polio. In August, a nationwide polio vaccination campaign started in Israel, targeting all children aged up to 9 years. The oral polio vaccine is being used to boost intestinal immunity in children previously vaccinated with inactivated polio vaccine in order to interrupt the spread of polioviruses. A vaccination campaign is also being considered in the West Bank and Gaza.
Ends
Notes to editors
-
Refer to the NaTHNaC country information pages for Israel specific to polio and travel health advice.
-
General information about polio is also available on the NaTHNaC website.
-
If you are traveling to any of these countries or are unsure about your risk, see your GP or travel clinic for advice as soon possible.
-
National Travel Health Network and Centre (NaTHNaC) is commissioned by the Public Health England and hosted by University College London Hospitals NHS Foundation Trust. It works in partnership with the London School of Hygiene and Tropical Medicine, the Liverpool School of Tropical Medicine, the Hospital for Tropical Diseases, the Department of Health and Public Health England to achieve its objective of improving standards in travel medicine and advice.
-
Public Health England’s mission is to protect and improve the nation’s health and to address inequalities through working with national and local government, the NHS, industry and the voluntary and community sector. PHE is an operationally autonomous executive agency of the Department of Health. www.gov.uk/phe Follow us on Twitter @PHE_uk
UKHSA press office: National Infection Service
UKHSA press office, infectious diseases
61 Colindale Avenue
London
NW9 5EQ
Photo above by CDC/ J. J. Esposito; F. A. Murphy