Newborn babies screened for more rare conditions
Every baby born in England from the 5 January will be offered screening for more rare conditions to prevent premature disability and death.
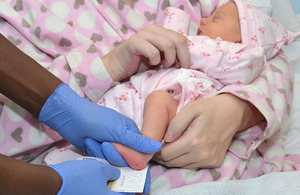
Newborn baby having a blood spot test
All newborn babies in England will be offered screening for 4 additional rare genetic disorders from today (5 January 2015).
Public Health England’s NHS Newborn Blood Spot Screening Programme has been expanded to screen for the following rare, but potentially disabling conditions: homocystinuria (HCU), maple syrup urine disease (MSUD), glutaric aciduria type 1 (GA1) and isovaleric acidaemia (IVA).
Testing for these conditions, leading to early detection and treatment, will prevent those babies affected from dying or being severely disabled for the rest of their lives.
Public Health Minister Jane Ellison said:
This is really welcome news. Expanding the screening has the potential to make a huge difference to the lives of babies born with rare genetic disorders. Detecting the disorders early can help prevent babies being severely disabled or even dying, which is absolutely vital for the families affected.
Dr Anne Mackie, Director of Programmes for the NHS Screening Programmes, part of Public Health England, said:
Screening for these rare disorders has the potential to benefit around 30 children in England each year. The early identification of these conditions can prevent death and significantly improve the quality of life for those living with these conditions.
The test will be performed using the same blood test that babies currently have at 5 to 8 days old. This sample is already used to test for 5 conditions which form the NHS Newborn Blood Spot Screening Programme: phenylketonuria (PKU), congenital hypothyroidism (CHT), sickle cell disease (SCD), cystic fibrosis (CF) and medium-chain acyl-CoA dehydrogenase deficiency (MCADD).
Sixteen-month old Phoenix Thompson from Lincolnshire was diagnosed with GA1 through the pilot programme at Sheffield Children’s Hospital.
Phoenix’s mother, Michelle Thompson, said:
It is unexplainable how important the screening was for us. It means Phoenix can receive the care and treatment he needs. It doesn’t bear thinking about what would have happened if the condition wasn’t picked up early.
Ends
Notes to Editors
-
The following interviews are available on request: A family affected by one of these serious conditions, Dr Anne Mackie, Director of Programmes for the NHS Screening Programmes and Professor Jim Bonham, national lead of the pilot programme, Sheffield Children’s Hospital.
-
Information on the NHS Newborn Blood Spot Screening Programme and the additional conditions is available.
-
The UK National Screening Committee was able to recommend extending the programme to screen for the additional conditions following the results of a pilot programme, coordinated by Sheffield Children’s NHS Foundation Trust, in partnership with the South Yorkshire Collaboration for Leadership in Applied Health Research and Care. Pilot areas included: Sheffield, Manchester, Leeds, Birmingham and London (Guy’s and St Thomas’ NHS Foundation Trust and Great Ormond Street Hospital).
-
New learning resources are now available for those involved in the screening programme: a resource on the expanded screening programme; a resource for those involved in taking blood spot samples.
-
Public Health England exists to protect and improve the nation’s health and wellbeing, and reduce health inequalities. It does this through world-class science, knowledge and intelligence, advocacy, partnerships and the delivery of specialist public health services. PHE is an operationally autonomous executive agency of the Department of Health. Website: www.gov.uk/phe. Twitter: @PHE_uk, Facebook: www.facebook.com/PublicHealthEngland
UKHSA press office: screening