HPR volume 19 issue 11: news (4 December 2025)
Updated 19 December 2025
Outbreak of Salmonella Enteritidis in the UK, November 2025
In August 2025, the Gastrointestinal Infections, Food Safety and One Health (GIFSOH) team at the UK Health Security Agency (UKHSA) identified an increase in the number of cases of Salmonella Enteritidis caused by a single strain, identified through the analysis of whole genome sequencing (WGS) data. Following identification, the Agency – together with Public Health Scotland (PHS), Public Health Wales (PHW), Food Standards Scotland (FSS), the Food Standards Agency (FSA) and the Animal & Plant Health Agency (APHA) – initiated an outbreak investigation and began considering potential sources of the outbreak.
Salmonella Enteritidis is the most commonly reported salmonella serovar in England in humans (1) and, like all non-typhoidal salmonella, it can infect and cause disease in humans. It is spread via contact with contaminated food, the environment, as well as person-to-person transmission. Symptoms of salmonella infection include diarrhoea, stomach cramps and sometimes vomiting and fever. Salmonella generally causes a mild illness, although immunocompromised individuals may experience more severe illness.
As at 11 November 2025, there were 123 confirmed cases within this outbreak, with cases falling within a single nucleotide polymorphism (SNP) single linkage cluster based on WGS, suggestive of a common source of contamination.
Confirmed cases have been identified between 27 May 2025 and 20 October 2025. Cases were resident in England (n=120), Scotland (n=2) and Wales (n=1). For cases resident in England, the regions with the highest number of cases to date are London (n=67), East of England (n=23) and the South East (n=21).
Temporal distribution of Salmonella Enteritidis outbreak cases based on sample receipt date at reference laboratory (n=121)
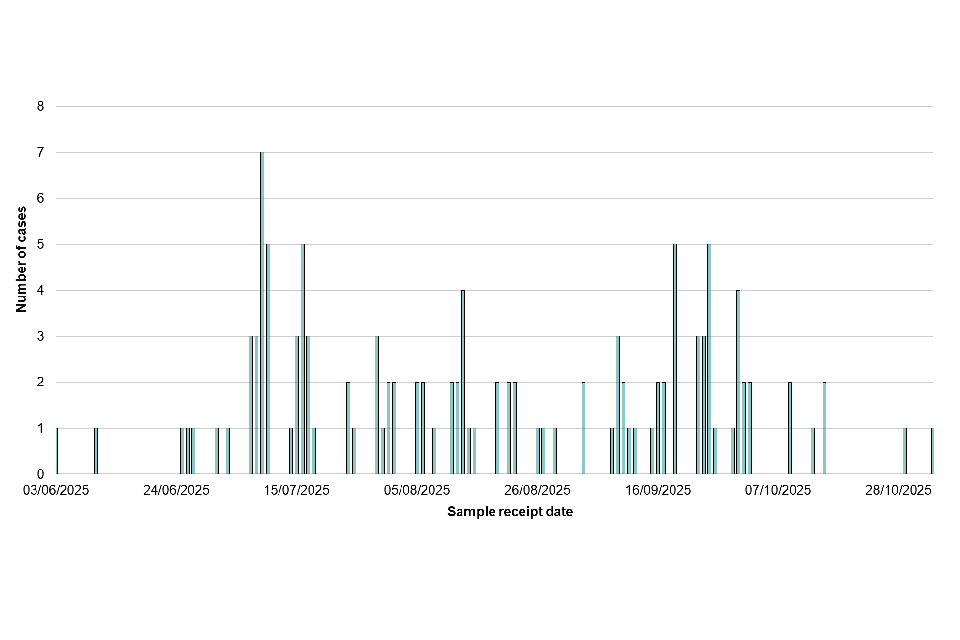
Cases range in age from 1 year to 92 years with a median age of 30. The age group most affected were those aged 0 to 9 years (n=25, 20%). Across all age groups, 56% (n=69) were male and 44% (n=54) were female.
Evidence gathered to date does not suggest that this outbreak is associated with international travel, as only 8 out of 123 cases (7%) reported travel.
The Outbreak Control Team utilised the ECDC EpiPulse platform to notify EU countries of the outbreak, and to understand whether others had identified genetically related Salmonella Enteritidis cases.
Extensive food chain investigations are ongoing to identify the source and origin of the contamination responsible for illness. A number of food businesses have been identified during this investigation, and several have been linked to the same distributor of imported eggs. The FSA has been liaising with local authority (LA) Environmental Health teams who have provided hygiene advice to food businesses where issues have been identified. The FSA are also working with LAs to undertake further enquiries into the egg supply chain, and further testing of eggs is being conducted.
Anyone with diarrhoea or vomiting should wash their hands thoroughly after using the bathroom and before preparing and handling food, cook food thoroughly, and if you have any symptoms, avoid handling food for others where possible.
Reference
Outbreak of Shigella sonnei associated with travel to Cape Verde
The UK Health Security Agency (UKHSA) has identified an increase in the number of Shigella sonnei cases caused by a particular strain of the gastrointestinal pathogen.
UKHSA, together with Public Health Scotland (PHS), Public Health Wales (PHW) and Public Health Agency Northern Ireland (PHA NI) have initiated an outbreak investigation.
Shigella sonnei (S. sonnei) is a species of Shigella, a group of gastrointestinal bacteria that can cause severe diarrhoea, fever and stomach cramps, rarely it can cause sepsis in the immunocompromised. S. sonnei is transmitted via contact with contaminated faeces either directly through person-to-person transmission or indirectly from contaminated food or water, or surfaces – infection is often linked to overseas travel to regions where shigellosis is endemic.
In October 2025, laboratory surveillance data indicated an increase in Shigella diagnoses in England, particularly Shigella sonnei (see figure 1).
Figure 1. Trends of Shigella species (spp.) and Shigella sonnei diagnoses in UKHSA’s Second Generation Surveillance System (SGSS), January 2018 to November 2025, England

Further analysis of isolates referred to the UKHSA’s Gastrointestinal Bacteria Reference Unit (GBRU) and the Scottish Microbiology Reference Laboratory – Glasgow (SMiRL-G) found that the increase in S. sonnei was driven by a single strain, identified through the analysis of whole genome sequencing (WGS) data.
Since 1 October 2025, 137 confirmed cases have been identified (see figure 2), with cases falling within a single nucleotide polymorphism (SNP) single linkage cluster based on WGS, suggestive of a common source.
Figure 2. Trend over time of Shigella sonnei outbreak cases based on sample submission date at reference laboratory
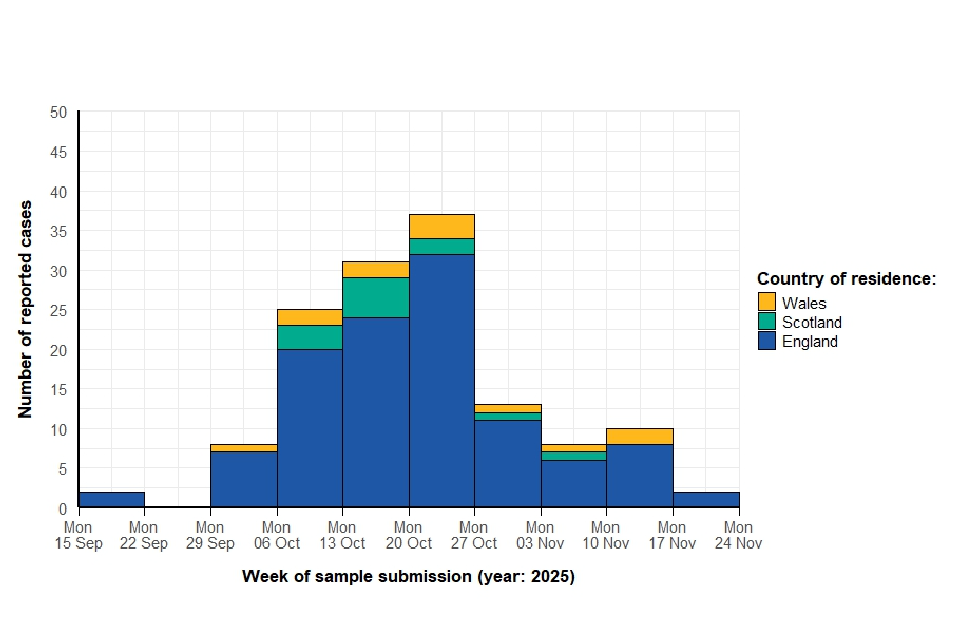
Cases are resident across all regions in England (n=113), Scotland (n=12), and Wales (n=12). Cases range in age from 0 to 81 years with a median age of 54 years. The age group most affected are those aged 50 to 59 years (n=55, 40.1%). Across all age groups, 72.3% (n=99) are female.
Evidence gathered to date suggests that this outbreak is associated with travel to Cape Verde. Of the 137 confirmed cases reported since 1 October 2025, 116 cases reported international travel – of which 109 (94.0%) travelled to Cape Verde, the majority to the Santa Maria and Boa Vista areas. For the remaining cases, travel information is not known.
This strain of S. sonnei does not have any genomic resistance determinants against common antimicrobials used to treat traveller’s diarrhoea.
International communications and investigations are ongoing. Travellers seeking advice can visit the NaTHNaC (National Travel Health Network and Centre) website TravelHealthPro for up-to-date travel health guidance, including specific information for Cape Verde: NaTHNaC – Cape Verde.
General advice on the avoidance of traveller’s diarrhoea is available at NaTHNaC - Travellers’ diarrhoea.
ESPAUR annual report in summary
The annual English Surveillance Programme for Antimicrobial Utilisation and Resistance (ESPAUR) report, published by UKHSA on 13 November, covers activity up to March 2025 and data on resistance and usage to the end of 2024. Some of the key findings of the twelfth report are presented below. Further details are available from the comprehensive main report, the lay summary and the associated infographics (1).
Antimicrobial resistance
In 2024, antibiotic resistant bacteria identified from blood samples (bacteraemia) continued to increase.
The latest national surveillance data analysing pathogens of public health importance due to antimicrobial resistance show that in 2024, there were 92,100 reports of people in England with bacteraemia, a 4.4% increase in numbers of bacteraemia since 2019 (88,181) (Figure 1). An estimated 20,484 bacteraemia cases in England were antibiotic-resistant in 2024, which is a 13.1% increase since 2019 (18,103). Twenty-two percent of bacteraemia episodes were resistant to one or more critical antibiotics in 2024 (1), up from 21% in 2019, highlighting that the increase in resistant bacteraemia episodes is attributable largely to the increase in bacteraemia episodes rather than solely due to an increase in resistance.
An estimated 8,394 patients with Gram-negative bloodstream infections died within 30 days of their episode in 2024. Data showed that mortality was higher among patients infected with antibiotic resistant strains (all-cause 30-day mortality 17.2%, n=2,379) and carbapenemse-producing Gram-negative organisms isolated from a sterile site (all-cause 30-day mortality 24.1%, n=68) compared to those who had antibiotic-susceptible Gram-negative bacteraemia (14.7%, n=5,952).
Figures 1. The burden of bacteraemia and resistant bacteraemia

There is substantial regional and demographic variation in the burden of overall bacteraemia incidence and antibiotic-resistant bacteraemia in England. The highest number and rates of bacteraemia and resistant bacteraemia were seen in those living in the most deprived areas, who had a 47.2% higher rate of resistant bacteraemia when compared to those in the least deprived areas (43.3 vs 29.4 resistant bacteraemia cases per 100,000 population). This range has increased from 2019 where the rate of resistant bacteraemia at that time was 29.0% higher in the most deprived quintile compared to the least deprived (Figure 2). When stratified by age and ethnicity, the greatest burden of bacteraemia and resistant bacteraemia in England was seen in those aged over 74 years old and the highest proportion of resistant bacteraemia was observed in the Asian or Asian British ethnic group when compared to all other ethnic groups.
Figure 2. Rate of resistant bacteraemia by Index of Multiple Deprivation from 2019 to 2024

Antimicrobial usage
The UK’s National Action Plan (NAP) for AMR 2024 to 2029 set the UK-wide target to reduce antimicrobial use by 5% from the 2019 baseline by 2029. In 2024, the total NHS antibiotic consumption was 2% lower than the 2019 (pre-pandemic level) with a marginal increase of 0.9% compared with 2023, suggesting a stabilisation of prescribing patterns following the pandemic-related disruptions (Figure 3).
Figure 3. Total consumption of antibiotics increasing towards pre-pandemic levels

In 2024, antibiotic consumption in primary care accounted for 79.6% of all antibiotic use within the NHS. Overall antibiotic consumption in primary care has increased from 2019 to 2024 (1.71 in 2024 compared with 1.66 items per 1,000 inhabitants per day in 2019) (Figure 4). A decrease in antibiotic prescribing was observed in general practice and in dental care where levels fell below 2019 levels. Antibiotic use in the ‘other community’ setting accounts for 34.5% of total NHS antibiotic use (0.061 items per 1,000 inhabitants per day). With the introduction of the Pharmacy First, which is included in the ‘other community’, there has been an observed increase in this setting which exceeded 2019 levels (0.11 to 0.18 items per 1,000 inhabitants/day). In 2024, antibiotic use in secondary care was 4,663 DDDs per 1,000 admissions, a decrease when compared to 2022 (4,684 DDDs per 1,000 admissions), but at similar levels to 2019, with a 0.05% marginal increase in inpatient prescribing and decrease of 4.2% in outpatient use noted.
Figure 4. Antibiotic prescribing in primary care from 2019 to 2024

In 2024, the proportion of Access antibiotic use has increased since 2021, which has surpassed pre-pandemic levels. Although there has been a 0.9% decrease in Access antibiotic use from 64.1% in 2023 to 63.2% in 2024, this was due to reduced primary care prescribing and a rise in ‘Other’ classification of antibiotics (2.7% to 4.0%).
New analysis of non-NHS prescribing data shows that, in 2024, 22% of total antibiotic prescribing in primary care constituted private (non-NHS) prescriptions. For further details see the ESPAUR infographics and the main ESPAUR report (1).
Antifungal use in 2024 increased by 2.0% from 2019. There was a large decrease in 2020 during the COVID-19 pandemic, usage has subsequently increased on a yearly basis.
Antimicrobial stewardship
Treat Antibiotics Responsibly, Guidance, Education and Tools (TARGET) have released new resources in the prevention and management of recurrent urinary tract infections which adds to the TARGET ‘How-to…?’ series to support primary care staff. The resources are in line with national guidance and offer evidence-based guidance for reviewing patients on long-term or repeat antibiotics for complex conditions. A TARGET Cycle of Antimicrobial Stewardship (AMS) infographic has also been developed to support the identified need for a consistent, whole-practice approach to AMS.
An evaluation of UKHSA AMS tools in England highlighted their use with web analytics showing an average of 71,588 visits to tool host websites over a 4-year period. Of the 12 tools identified, 7 had evidence of use in secondary care and 11 tools had evidence of impact in the UK, such as impact on guidance from UK national organisations. Furthermore, since 2019, there is evidence of the ESPAUR report being named in 50 mainstream media news items. The Antibiotic Guardian campaign, the Start Smart, then Focus Toolkit, the Antimicrobial Stewardship Prescribing Competencies and the ESPAUR report, were also found to have had international impact.
There has been evidence of the immediate use and knowledge mobilisation of the UK-adapted AWaRe categories. For example, the gov.uk webpage hosting the UK-adapted AWaRe categories received 1,130 unique visits within the first two months following publication. Additionally, there has been evidence of use across social media such as on LinkedIn, X (formerly Twitter), Instagram and Facebook. In addition, the tool has been knowledge mobilised through Fingertips news webpage updates, publication of a press release and succeeding articles in trade journals and disseminated through the ESPAUR Oversight Group stakeholder organisations.
Finally, in May 2024, a survey was conducted within NHS hospital trusts to explore the status of antifungal stewardship (AFS) initiatives across England with survey results compared to a 2016 baseline. Just over a third of respondents (35%, 15 of 43) had an AFS programme compared to 54% in 2016. Among trusts with AFS programmes, 87% had access to fungal guidelines compared to 76% in 2016. The main barriers to AFS, lack of staff time and competing priorities, remained the same as 2016.
Professional and public education, engagement and training
The UK NAP for AMR identifies public and professional engagement and education as key outcomes for driving behaviour change. To support this, TARGET delivered three AMS webinars in collaboration with the Royal College of General Practitioners (RCGP), which received strong engagement and positive feedback. The national rollout of TARGET training reached over 1,000 primary care professionals, with evaluations showing improved knowledge, confidence and intentions to implement AMS practice as a result, as well as a reduction in antibiotic prescribing.
Professional engagement was further supported through annual campaigns such as World AMR Awareness Week (WAAW) and European Antibiotic Awareness Day. Evaluation of WAAW in 2025 highlighted that awareness of the campaign is linked to improved understanding of antimicrobial use and resistance. Additionally, the Antibiotic Guardian campaign, which encourages pledges to support AMS, received nearly 13,000 pledges in 2024, mostly from health or social care professionals.
A UK public survey highlighted gaps in understanding of AMR, particularly among younger members of the public. To address this, UKHSA launched a public awareness campaign, introducing the mascot Andi Biotic to deliver key messages about appropriate antibiotic use and AMR. Evaluation of the campaign is ongoing, however early findings suggest that the campaign was a creative success which achieved a high engagement rate for the target audience. Public education was further addressed through the international e-Bug programme, which expanded their global partnership and delivered infection prevention and control training courses for educators working with children and young people.
Research and knowledge mobilisation
A wide range of new and ongoing research projects were undertaken in the fields of HCAI and AMR in the last year, with the publication of over 100 peer-reviewed papers from across UKHSA (Figure 5).
Figure 5. AMR peer-reviewed publications from April 2024 to March 2025 by UK National Action Plan for AMR 2024 to 29 outcome

Finally, annual feedback surveys continue to show that a large proportion of ESPAUR report users continue to endorse the report to other stakeholders (92.3%, 359 out of 389). UKHSA also continues to work to knowledge mobilise the report with a recent evaluation finding widespread use of the ESPAUR report in English hospitals, usually through referencing in annual AMS/IPC reports. There is also evidence of wider use across the UK and internationally, including references within NICE guidance, in a patient safety alert, and in national stewardship papers, such as the Surveillance of Antimicrobial Use and Resistance in Northern Ireland Annual Report and the UK One Health Report, as well as references to the ESPAUR report as an exemplar of reporting in papers from the European Centre for Disease Prevention and Control and the global Leading Health Systems Network.
Reference
1. UKHSA (2025). English surveillance programme for antimicrobial utilisation and resistance (ESPAUR): report 2024 to 2025
GRASP annual report in summary
UKHSA has published its annual Gonococcal Resistance to Antimicrobials Surveillance Programme (GRASP) report, presenting the latest data on antimicrobial resistance in Neisseria gonorrhoeae in England and Wales.
One ceftriaxone-resistant Neisseria (N.) gonorrhoeae isolate was detected in the sentinel surveillance programme for the first time in 2024. This isolate was also detected in real-time through direct referral of suspected ceftriaxone-resistant isolates to the Agency’s Sexually Transmitted Infections Reference Laboratory (STIRL). This case was associated with travel to the Asia Pacific region.
Through referral of resistant isolates outside of the sentinel surveillance system, 15 cases of ceftriaxone resistance have been detected in the first 8 months of 2025, exceeding the total number detected for the whole of 2024 (n=13). Most cases continue to be associated with travel to the Asia Pacific region.
Most gonococcal isolates remain highly susceptible to ceftriaxone. Although the percentage of isolates with reduced susceptibility to ceftriaxone (minimum inhibitory concentration (MIC) >0.03 mg/L) remains low at 1.7%, it has increased consecutively since 2021.
Cefixime resistance decreased from 5.6% in 2023 to 3.1% in 2024. Reduced susceptibility to both ceftriaxone (MIC >0.03 mg/L) and cefixime (MIC >0.06 mg/L) was associated with the presence of mosaic or semi-mosaic penA alleles, with penA-34 accounting for 88% of mosaic alleles overall.
Reduced susceptibility to azithromycin (epidemiological cut-off value (ECOFF) >1 mg/L) was 13.6%; however, 90% of isolates with reduced susceptibility had an azithromycin MIC of 2 mg/L, immediately above the ECOFF.
Nearly all isolates (90.7%) were considered resistant to tetracycline (MIC >0.5 mg/L). A quarter of isolates (25.9%) were resistant to penicillin (MIC >1 mg/L), nearly double that recorded in the previous year. Ciprofloxacin susceptibility was predicted from genomic data in 2024, and resistance decreased from 58.6% in 2023 to 46.4% in 2024.
Multilocus sequence typing (MLST) results provided insights into the underlying gonococcal population structure. The top 10 sequence types (STs) accounted for 68.8% of the isolates, which was comparable to 2022 to 2023; however, shifts in the composition and relative proportions of the top 10 STs were identified. Common STs differed in their patterns of antimicrobial susceptibility, and fluctuations in their prevalence will have contributed to changes in overall resistance.
Prescribing data demonstrated excellent adherence to the UK guideline for managing infection with N. gonorrhoeae, with 97.0% of individuals receiving the recommended first-line of ceftriaxone 1g intramuscular (IM) monotherapy in 2024.
A decision was made to change the medium for testing 2024 GRASP isolates. A full validation of the new medium was carried out; this included testing of 6 WHO control strains and confirmed improved performance. Systematic shifts between the previous and new media were observed for MICs of azithromycin, cefixime and penicillin, therefore changes in prevalence of resistance to these agents may be under- or over-estimated in previous years. For further details, please see Appendix 1.
Sexual health services should report cases of suspected treatment failure to UKHSA via the online HIV and STI Data Exchange (access is restricted to registered users).
Infection reports in this issue
Laboratory confirmed cases of pertussis in England: annual report for 2024
Mycoplasma pneumoniae surveillance in England and Wales, October 2020 to September 2025
Emergence and outbreak of Clostridioides difficile ribotype 955 in England
Laboratory reports of hepatitis A infections in England and Wales: 2024
Laboratory surveillance of streptococcal bacteraemia in England: 2024 update
Vaccine coverage
RSV vaccine coverage report in older adults for catch-up cohorts in England: October 2025
RSV maternal vaccination coverage in England: July 2025
