PHE welcomes new drive to tackle TB in vulnerable groups
Public Health England (PHE) welcomes a NICE local government public health briefing which launches today to tackle TB in vulnerable groups.
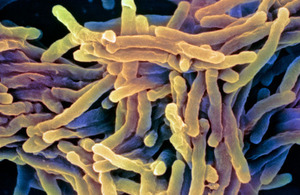
Tuberculosis
The National Institute for Health and Care Excellence (NICE) has today (25 September 2013) published a new briefing for local government on how to address tuberculosis (TB), with focus on vulnerable groups who may have difficulty accessing services. It supports local government with their wider remit for public health in communities and has been supported by, and is fully endorsed, by PHE.
TB is an infection caused by bacteria and usually affects the lungs, but can affect other parts of the body. Vulnerable groups, such as people who are homeless or in poor or temporary housing, vulnerable migrants, people who have spent time in prison, and people who misuse alcohol or other substances are at particular risk of developing the disease.
PHE’s recently published TB annual report showed 8,751 cases were reported in the UK in 2012, and those most at risk were individuals from ethnic minority groups. People with social risk factors such as a history of homelessness (2.4% - 194/8,088), imprisonment (2.8% - 225/7,918), or problem use of drugs or alcohol (2.8% - 228/8,019), as well as the elderly, also have a higher risk of developing TB.
Some of the recommendations the briefing proposes include:
-
local authorities should work with the NHS and PHE to support informed commissioning and ensure services reflect the needs of their area, as identified by local needs assessment
-
multidisciplinary TB teams should have the resources to provide a continuous service throughout the year, with rapid access to TB clinics for vulnerable groups
-
multidisciplinary TB teams should identify and support an ongoing TB education programmes for local professionals in contact with vulnerable groups, such as staff in accident and emergency departments, GPs, housing officers, people who support vulnerable migrants as well as those working in walk-in centres, hostels, substance misuse projects and prisons.
Dr Lucy Thomas, Head of TB Surveillance at PHE, said:
PHE supported NICE to develop this briefing, which identifies the actions that local authorities and partner organisations can take at a local level to help tackle TB among vulnerable groups. Implementation of these recommendations will help to reduce TB transmission and health inequalities in our most vulnerable populations.
Dr Paul Cosford, Director of Health Protection and Medical Director at PHE, said:
TB is a preventable and treatable condition, but, if left untreated, can be life threatening. Early diagnosis and appropriate treatment are key to reducing TB rates in the UK, and it is particularly important to focus on vulnerable groups who are at higher risk of developing TB and may have difficulty accessing services.
This NICE briefing gives practical advice for local authorities on how to ensure relevant health, welfare and social care services link up to strengthen TB control and improve health and social outcomes for vulnerable groups of people.
Professor Mike Kelly, Director of the Centre for Public Health at NICE said:
Local authorities are in a good position to take action on some of the social factors that contribute to the disease spreading, such as poor housing, homelessness and access to healthcare. It recommends that commissioners of TB prevention and control programmes could use health or public health resources to fund accommodation for homeless people diagnosed with active TB undergoing treatment, who otherwise wouldn’t qualify for state-funded accommodation, to help them adhere to their treatment. By addressing these factors, along with a raft of wider recommendations, local authorities can help reduce the spread of TB and improve general health outcomes.
NICE is the independent body responsible for driving improvement and excellence in the health and social care system. They develop guidance, standards and information on high-quality health and social care, as well as advise on ways to promote healthy living and prevent ill health.