Department of Health corporate plan 2013 to 2014
Updated 13 June 2014
Applies to England
Foreword
by Una O’Brien, Permanent Secretary
This document is our Corporate Plan for financial year 2013 to 2014. It shows our priorities for the next 12 months and it will be updated on a rolling quarterly basis, reflecting progress against milestones and any changes to those priorities. The priorities and commitments for the year ahead are challenging, and none of them can be delivered exclusively by the Department of Health. They demand that we work well with our partner organisations nationally and locally. But our success also depends on how confidently we, as an organisation, reflect the needs of patients and the public.
This is a landmark year for the health and care system. NHS England, Public Health England, the NHS Trust Development Authority and Health Education England have now taken up their responsibilities in full. The Department of Health emerges from the reforms as a smaller department of state, but with a renewed sense of purpose, and a clear vision of our leadership role in the health and care system.
To ensure that that the department remains lean and fit for its purpose in the new system – focussing on the things only we should and can do – we will be taking the opportunity offered by this year’s period of organisational stability to take a fresh look at our baseline of activity and costs. But this year will be defined by two issues: how we respond to the Francis report, and how, working with our partners across the health and care system we develop our role as stewards of the health and care system.
Robert Francis has set out a clear challenge to every organisation responsible for health and care. His report underlined how important it is that, at every level, we connect with the experiences of patients and the public. Over the coming years, the Department of Health will play a major role across the health and care system in leading this work, starting with our own organisation.
At every level, we will reflect the experiences of patients and the public in our work and our behaviours. So, whether it is in policy-making, in how we fund health and care and hold the system to account to parliament and the public, or in how we champion innovation and improvement, we will put the needs of patients and the public at the heart of every decision we make.
In our response to the Francis report, we said that by 2016, every Department of Health civil servant and minister will have a real and extensive connection to the frontline to help build our understanding of the impact of our work and the realities that people face. But it will be what we do with that experience that counts. In particular, through our leadership of the health and care system, we will need to amplify what we learn, and inspire the national and local organisations responsible for health and care services to aspire to the highest possible standards of support, care and treatment for the people they serve
Our ministers, non executive directors and leadership team

Image of all DH ministers

DH non executive board members and leadership team
For more information about our ministers, non executive directors and leadership team see Annex A
Our Department
Our Purpose - The Department of Health helps people to live better for longer.
We lead, shape and fund health and care in England, making sure people have the support, care and treatment they need, with the compassion, respect and dignity they deserve.
Our Responsibilities – we do this in three important ways:
- we lead across health and care by creating national policies and legislation, providing the long-term vision and ambition to meet current and future challenges, putting health and care at the heart of government and being a global leader in health and care policy
- we support the integrity of the system by providing funding, assuring the delivery and continuity of services and accounting to Parliament in a way that represents the best interests of the patient, public and taxpayer
- we champion innovation and improvement by supporting research and technology, promoting honesty, openness and transparency, and instilling a culture that values compassion, dignity and the highest quality of care above everything
Above all, DH encourages staff in every health and care organisation, including our own, to understand and learn from people’s experience of health and care and to apply this to everything we do.
Our Vision - what we want to achieve:
- people have the best possible start to life
- health is protected, wellbeing is promoted and avoidable deaths and diseases are prevented
- people are enabled to live independent and fulfilling lives, and take control of the care they need
- people who are ill or need support receive safe and effective care and are treated with dignity, including at the end of life
- health and care inequalities become a thing of the past
Our Values - We value:
People - Purpose - Working together - Accountability
Our overarching priorities

Image of grandad mum and boy
The Secretary of State’s priorities are:
- preventing people from dying prematurely by improving mortality rates for the big killer diseases, to be amongst the best in Europe, through improving prevention, diagnosis and treatment
- improving the standard of care throughout the system so that quality of care is considered as important as quality of treatment, through greater accountability, better training, tougher inspections and more attention paid to what patients say
- improving treatment and care of people with dementia, to be among the best in Europe through early diagnosis, better research and better support
- bringing the technology revolution to the NHS to help people, especially those with long term conditions, manage their health and care
The DH Leadership Team have supplemented these by adding the following priorities:
- improving productivity and ensuring value for money for the taxpayer
- focusing on improved delivery and performance
- leading transition to the future system and working together to build a sense of common purpose
- contributing to economic growth
The Department of Health is also committed to demonstrating real and meaningful progress towards achieving true ‘parity of esteem’ between mental and physical health by March 2015.
Our themes
We will deliver the department’s overarching priorities and business as usual within the following six themes.
Better Health and Wellbeing for all – helping people live healthier lives.
We will do this by improving our public health system; protecting people’s health by ensuring we have the capabilities and policies in place to address threats to public health; promoting health and wellbeing to reduce premature mortality and tackle health inequalities across all ages.
Better Care for all – helping people get better and ensuring people are treated with dignity and respect and supporting a patient-led NHS.
We will do this by reforming social care; supporting the system to improve standards of care, support and treatment and strengthen people’s ability to make meaningful choices about their care the integration of services around the individual; getting the basics right on safety in health and care; a greater focus on health outcomes.
Better Value for all – providing better quality care by improving productivity and ensuring value for money for the taxpayer
We will do this by reducing bureaucracy; promoting innovation and the use of technology in the health and care system, holding the new health and care system to account to Parliament and the public, supporting the NHS to save up to £20 billion to reinvest in frontline services; simplifying regulation of the development and adoption of new medicines and treatments.
Successful Change – delivering the transition to a more autonomous and accountable system.
We will do this by making sure the new partnership organisations, clinical commissioning groups and health and wellbeing boards are ready to take on their new responsibilities; continuing our own transformation into a smaller, more purposeful organisation, with a clear sense of its role in health and care.
Our Partners – achieving strategic clarity, building a common sense of purpose.
We will do this by developing strong relationships with our external stakeholders and establishing effective ways of working with the new organisations in the health and care system; playing our full role in delivering the government’s priorities led by other departments.
The DH itself – improving our capability and becoming a better department.
We will do this by developing new ways of working that reflect the leadership role we will play in the new system; the importance of engaging with our partners; and building understanding of our work within the health and care system the wider public. Putting equality and diversity at the heart of what we do.
Our priorities

Image shows our priorities for 2013-14
Better Health and Wellbeing for all
We will work to improve health outcomes and reduce premature mortality and health inequalities. We will ensure we have the capabilities & policies in place to address threats to public health, strengthen our public health system and promote health and wellbeing.
Improve and promote health and wellbeing throughout the whole course of life and reduce the burden of conditions associated with poor lifestyles such as obesity, smoking, drug misuse and harmful alcohol consumption.
In particular, we will:
-
reduce numbers of people dying prematurely by improving prevention, screening and early diagnosis (to enable more effective treatment), and thereby improve mortality rates for the big killer diseases, in absolute terms and relative to the best in Europe. (PHD)
-
deliver the key policy priorities for health and wellbeing in the areas of long-term conditions, premature mortality and oral health, and align the Outcomes Frameworks for Social Care, Public Health and the NHS so that they improve joint working and outcomes for the people of England. (PHD, SCLGCP & FN)
-
improve and promote health and wellbeing throughout the whole course of life and reduce the incidence of conditions associated with smoking, drug misuse, harmful alcohol consumption, obesity, poor diet, lack of physical activity, poor sexual health and violence (PHD & SCLGCP)
-
harness the potential of innovations in medical science such as genetics, embryology, organs and stem cells, including the Prime Minister’s commitment to sequence 100,000 genomes. (PHD)
-
commission relevant and timely research evidence through the National Institute for Health Research (NIHR) and the Policy Research Programme, to meet the needs of patients, professionals, the public and policy makers (RDD)
-
make it faster and easier to initiate and deliver research by helping the NHS to improve research management performance and speeding up the availability of new interventions for patients and the public (RDD)
-
improve health outcomes for people with mental health problems through the continued development of the “No Health Without Mental Health” strategy and effective stewardship of the Mental Health Act. (SCLGCP)
-
improve health outcomes for children and young people in line with the Children and Young People’s Health Outcomes Pledge and the system’s response to the Forum’s recommendations. (SCLGCP)
-
help children to make the best start in life through the further development of the Information Service for Parents, offering multimedia advice on how babies & children develop, antenatal education and advice on breastfeeding & immunisations, and by delivery of the National Health Visitor Programme and the Family Nurse Partnership Programme to increase capacity and transform services. (SCLGCP & PHD)
-
improve diagnosis through overseeing screening programmes, including the piloting of bowel scope screening. (PHD)
Create and sustain a new public health system which rebalances our approach to health, drawing together national leadership with local delivery, and a new sense of community and social responsibility.
We will:
- support the new balance of public health responsibilities between Local Government, PHE, DH and the NHS. (PHD)
- strengthen research on chronic conditions and public health across NIHR programmes, including through new Collaborations for Leadership in Applied Health Research and Care, and on in vitro diagnostics through new Diagnostic Evidence Co-operatives. (RDD)
Protect the health of the population, by ensuring we have the right policies and capabilities to protect people from a range of health threats such as those associated with pandemic influenza and terrorist attack. In particular we will:
- take urgent action to help slow down the development of antimicrobial resistance by leading work to encourage more responsible use of antibiotics in this country and internationally , and working with industry to encourage the development of new antibiotics. (PHD)
- provide strategic oversight to the development and implementation of new national vaccination programmes – seasonal flu, rotavirus and shingles. (PHD)
- protect the health of the population, by ensuring we have the right policies and capabilities to protect people from a range of health threats such as those associated with pandemic influenza and terrorist attack. (PHD)
Better Care for all
We will work to improve the quality of care for all people using services, including reforming social care, working with the NHS to strengthen people’s ability to make meaningful choices about their care and treating people with dignity and respect.
Focus on getting quality, safety and dignity right every time in care services. In particular we will:
- deliver the government’s response to the Mid Staffordshire NHS Foundation Trust Public Inquiry recommendations, working jointly with other bodies, to help increase compassion and dignity in the NHS. (SER, RDD & FN)
- deliver the Secretary of State’s Care Priority to ensure that the quality of care is as important as the quality of treatment. (SER)
- deliver a system of medical revalidation that will enable delivery of key benefits around improved quality of care, safety, efficiency and public confidence. (SER)
- improve the quality of life for those with dementia and their carers by improving health and care, research and “dementia friendly” communities and by announcing the outcome of a joint ESRC/NIHR call for research on living well with dementia and publishing the progress against the PM Challenge on Dementia. (RDD & SCLGCP)
- support delivery of national nursing strategy Compassion in Practice. (PHD)
Reform the system of social care. In particular we will:
- reform the system of adult social care to implement the White Paper & improve the legal framework, including a new funding system, to drive improved outcomes for service users and their carers, and ensure fit for purpose outcome-focused national datasets (SCLGCP)
- deliver ministers’ priorities for an efficient and effective NHS estate and facilities, particularly around supporting patient safety, care and dementia, with a focus on the NHS Constitution’s commitment to patients, staff and the wider public (IGO)
- lead the programme to improve care and support available during pregnancy, birth and the start of life. (SCLGCP)
- oversee the programme of action in response to Transforming Care – implement the Winterbourne View Review so that services for people with challenging behaviour are transformed and review the statutory autism strategy (SCLGCP)
- provide strategic direction in modernising the health and care workforce to ensure that the right skills, values, behaviours and training, is available in the right numbers, to support the delivery of high quality care and health improvement (SER & SCLGCP)
Put users and carers at the centre of decision making, with care integrated around their needs, to include embedding shared decision-making as the norm. In particular we will:
- ensure that issues raised by individual patients, their carers and representatives about the care they receive are listened to and acted upon, so as to improve an organisation’s ability to improve its standards and its culture of caring (SER)
Improve the outcomes of care services, and support innovation. In particular we will:
- improve outcomes and experience and ensure better coordinated care by publishing the Common Purpose Framework with key national partners (SCLGCP, FN)
- improve the quality and use of technology and information in the health and care system including development of a single portal for patients to see comparative data across the system (SER)
- help people stay independent, by maximising well-being and improve health outcomes through strong leadership and strategic partnerships across nursing, midwifery, health visiting & allied health professions, and grow & transform the health visitor service (PHD)
Better Value for all
We will work to increase productivity and ensure better value for money for the taxpayer, including reducing bureaucracy and supporting the NHS to save up to £20 billion to reinvest in frontline services.
Contribute to economic growth. In particular we will:
- encourage growth, value for money and better regulation by supporting delivery of national QIPP procurement work, negotiating new arrangements for branded medicines pricing, delivering the Health and Life Sciences Plan for Growth and reducing bureaucracy and costs to the business and addressing the Red Tape Challenge (FN)
- ensure England maximises its share of life sciences research collaborations and investment, contributing to the economic growth of the country, by supporting a vibrant, world-class NHS platform for research investment by the life-sciences industry and major public sector research funders, and life-sciences sponsorship and its strategy implementation. (RDD & FN)
- support growth and value for money by managing the commercial investment decisions, supporting international investment through the “golden thread”, and achieving value for money, including by managing financial implications of EU/EEA membership (PHD & FN)
Improve efficiency and reduce bureaucracy. In particular we will:
- launch and deliver a Baseline Review to reduce costs across the system (FN)
- lead strategic financial planning and discharge the Department’s financial management responsibilities effectively and efficiently by negotiating the spending settlement for financial year 2015 to 2016, developing the financing and failure regime for NHS providers, and delivering unqualified annual statutory accounts for the Department (FN)
- reform the NHS employment package to deliver the Secretary of State’s priority for high quality, safe and compassionate care, including the development and implementation of pay and pension policies, which support the recruitment and retention of skilled staff right across the NHS and independent sectors (SER)
- ensure effective implementation of reform to education and training funding, with tariffs providing greater fairness, transparency and efficiency (SER)
- review and deliver the Bureaucracy and Regulatory Review’s recommendations following the report by the NHS Confederation (SER)
- maximise the benefits available from new technology and information, including implementation of the Information Strategy, leading Secretary of State’s priority work and building the capability of the new Health and Social Care Information Centre. (SER)
- support increases in speed and cost effectiveness of trial set up in the NHS by publishing outcomes against a 70 day benchmark (70 days or less from the time a provider of NHS services receives a valid research application to the time when that provider recruits the first patient for that study) (RDD)
- commission an evaluation of the “Innovation, Health and Wealth” Strategy, to assess the effectiveness of actions to promote the spread of innovation in the NHS (RDD)
Successful Change
We will work to ensure a smooth and successful transition of the health and social care system, developing and articulating our common purpose to align our work across all organisations, and establishing a framework that can realise the benefits for the health and care system.
Manage the transition to the new health and care system architecture. In particular we will:
-
lead the coherent design of, and transition to, the new health and care system through legislation to reform the Care and Support System and implement the Health and Social Care Act, publishing the Common Purpose Framework for integrated care, and ensure effective management of the portfolio of ex-PCT and SHA property (SCLGCP & FN)
-
lead the transformation work in the Department of Health so it can fully deliver its new role, including clearly defining and communicating the Department’s role in the system, and deliver wider Civil Service Reform changes (IGO)
-
programme manage the completion of the transition & legacy work, which the Department of Health and all new bodies in the system, will need to carry out during financial year 2013 to 2014, culminating in a fully functioning, efficient and effective new health & care system (IGO)
-
ensure there are proper governance and accountability arrangements in place across the new health and social care system so that DH and Arm’s Length Bodies meet their public and Parliamentary accountabilities (SER)
-
refresh the Mandate and establish effective accountability arrangements for the NHS England (NHSE), support NHSE and Monitor as they take on accountability for the NHS payment system, in particular by developing the tariff for financial year 2014 to 2015 (FN)
-
support primary legislation to establish the Health Research Authority as a non-Departmental public body in order to give it even greater stability and independence (RDD)
Establish the framework for beginning to realise the benefits of reform. In particular we will:
-
support the development of Health Education England and the Local Education and Training Boards and establish effective accountability arrangements (SER)
-
support Health and Wellbeing Boards to realise their potential, working with partners to ensure that the boards can work effectively locally to improve services and outcomes (SCLGCP)
-
support the functions of Public Health England by establishing NIHR Health Protection Research Units in 12 priority topics (RDD)
-
support, monitor, oversee and drive delivery and overall implementation of the Information Strategy for Health and Social Care, ensuring alignment with the Government Digital Strategy where appropriate (SER)
-
support others to meet their statutory duty to promote research by continuing to work as appropriate with the NHS England, Clinical Commissioning Groups and Monitor (RDD)
-
co-ordinate the department’s response to Open Public Services and refresh the Outcomes Framework (FN)
-
ensure a more transparent process of Death Certification is put in place, with robust safeguards and a unified system of certification and payment; independent advice from medical examiners, improved quality of data (PHD)
Our Partners
We will work to develop stronger partnerships – working across government, with our external stakeholders and establishing effective ways of working with our new partnership organisations.
Build partnerships with our stakeholders. In particular we will:
- enable the voice of the Voluntary and Community Sector and develop our understanding of their role in the health and social care system (SCLGCP)
- provide leadership, stewardship and alignment of communications activity across the health and care system. (SER)
- work through our sponsorship of Healthwatch England to build an effective local network that empowers local people and communities to present their views and experiences to feed into local and national policy decisions about care services. (SCLGCP)
Sponsor our arm’s length bodies (ALBs) effectively. We will develop excellent relationships with our ALBs and executive agencies. In particular we will:
- implement and manage an effective operating model for sponsorship of NHS England (FN)
- work effectively with local government, NHSE and Public Health England (PHE) to assure the effective public health and adult social care contribution to improved outcomes for individuals and communities (PHD & SCLGCP)
- build and embed effective assurance and sponsorship systems and capabilities within the Department of Health, which support and assure the new arms length bodies and build common purpose across the wider health and care system. (IGO)
- sponsor and develop relationships with our Arm’s Length Bodies, including Health Education England (HEE), Health Research Authority (HRA), NHS Litigation Authority, NHS Business Services Authority (NHS BA), Monitor, National Institute for Health and Care Excellence (NICE), NHS Trust Development Authority (NHS TDA), Medicines & Healthcare products Regulatory Agency (MHRA), NHS Blood & Transplant (NHSBT), Human Fertilisation & Embryology Authority (HFEA), Human Tissue Authority (HTA) and Care Quality Commission (CQC) to provide appropriate stewardship and enable them to flourish (SER, PHD, FN & RDD)
- Lead the setup of Health and Social Care Information Centre (HSCIC) to establish its role as the main information and technology partner within the health and care sector (SER)
Assist other government departments. We will build stronger, mutually supportive relationships with other government departments – with them supporting our goals, and us supporting the wider goals of the Government as a whole. In particular we will:
- lead effectively and seamlessly for the UK Government on health issues overseas, including in the EU, WHO, ensuring other government departments (OGDs) and civil society have full opportunity to present their views and influence the UK delegations (PHD)
- establish a network of partnership engagement across government to share learning and pool resources to improve the way government works with others (SER)
The DH itself
We will continue to work to improve our capability – developing new ways of working that reflect the leadership role we will play in the new system, the importance of engaging with our partners, and to build understanding within the health and care system and the wider public of our work.
Improve our efficiency and effectiveness as a Department of State. Across the breadth of our business we will:
- lead the change work in the Department of Health to foster a common culture amongst staff to ensure the health needs of patients and the public are placed first in all we do (IGO)
- ensure that all Department of Health civil servants have sustained and meaningful experience of the frontline (All)
- create the environment & provide the core policies and processes to enable leaders and managers to build high performing teams where performance is well managed and people are developed to maximise their contribution to the success of the Department (IGO)
- review the Department’s relationships with other Government Departments (OGDs) to take a more strategic approach to cross government working (SER)
- develop new guidance and training materials on working with corporate partners and stakeholders and implement a corporate partner system of senior account managers for key DH stakeholders to strengthen external relationships (SER)
- improve the use and understanding of evidence and insight in the development of policy and communications across DH. (SER)
- equip people, within the context of Civil Service Reform, with the new and improved capabilities they need to deliver new functions, new / changed processes and systems, and underpinning values and behaviours within the Department and the wider system. (IGO)
- ensure that corporate services continue to improve and adapt to meet the business needs, comply with wider civil service requirements, and achieve best value (IGO)
- implement the DH Digital Strategy and become a “Digital First” Department of State, in line with Civil Service Reform (SER)
- ensure DH meets its obligations under the Equality Act, and deliver its Equality Objectives Action Plan commitments to improve the quality of its policy making, analysis and evidence base (SCLGCP)
Improve our own capability, including actions arising out of our Capability Action Plan. In particular we will:
- develop and transform the Department by leading the growth of the Department’s policy, strategic and analytical capability; implementing a new finance operating model; and providing a high quality procurement and commercial function to deliver the department’s business efficiently (FN)
- develop and implement a new finance operating model, via the Financial Management Improvement programme (FMIP), as part of the future DH programme, based on customer-focused expert services and a clear definition of roles/expectations (FN)
- develop the DH Staff Health and Wellbeing programme to help drive a change from awareness and engagement activity through to measures of success and impact on staff health and wellbeing (SER)
- improve capability and understanding within the health and care system by supporting the Department to understand and meet SofS’s new statutory duties to promote research, reduce health inequalities and improve quality (RDD, SCLGCP & FN)
Our roadmap for the year ahead

Image of raodmap
Quarter 1
Read how we performed against milestones for quarter 1 Annex B
Quarter 2
Read how we performed against milestones for quarter 2 Annex C
Quarter 3
Read how we performed against milestones for quarter 3 Annex D
Quarter 4
Read how we performed against milestones for quarter 4 Annex E
Information and Group Operations : January to March 2014
- complete post implementation transition work, and establish a legacy closedown team to oversee remaining residual activity during financial year 2014 to 2015
- undertake year-end assessment of sponsor capability
- complete next stage of DH’s Change Programme
- complete dementia schemes and initiate final draft of dementia report
- commence pre-migration work for first wave implementations of shared services for finance, HR and payroll
Public Health : January to March 2014
- roll-out the Bowel Scope Screening Programme to 30% of the country
- put in place strategy to sequence 100,000 whole genomes
Social Care, Local Government & Care Partnerships : January to March 2014
- announce Strategic Partners scheme for financial year 2014 to 2015
- publish Statutory Review of Autism Strategy
- secure increase in Family Nurse Partnership places to 13,000
- develop action plan for the government commitment on Information Sharing to Tackle Violence under the remit of the Task and Finish Group
- publish declaration on confidentiality and suicide prevention
- publish Health Working Group report on child sexual exploitation
Finance & NHS : January to March 2014
- put in place new pricing arrangements for branded medicines
- submit plan for the transformation of Business Services Authority and delivery of BSA commercial review
- respond to NAO hospital waiting lists study report
Research & Development : January to March 2014
- announce successful NIHR Health Protection Research Units
- commence contracts for designation and funding of NIHR Collaborations for Leadership in Applied Health Research and Care
- reconfigure Local Clinical Research Networks
Resources
Indicative Budget Allocations for financial year 2013 to 2014
This chart sets out further detail on how our settlement will be allocated for the financial year 2013 to 2014 across our key programmes and activities
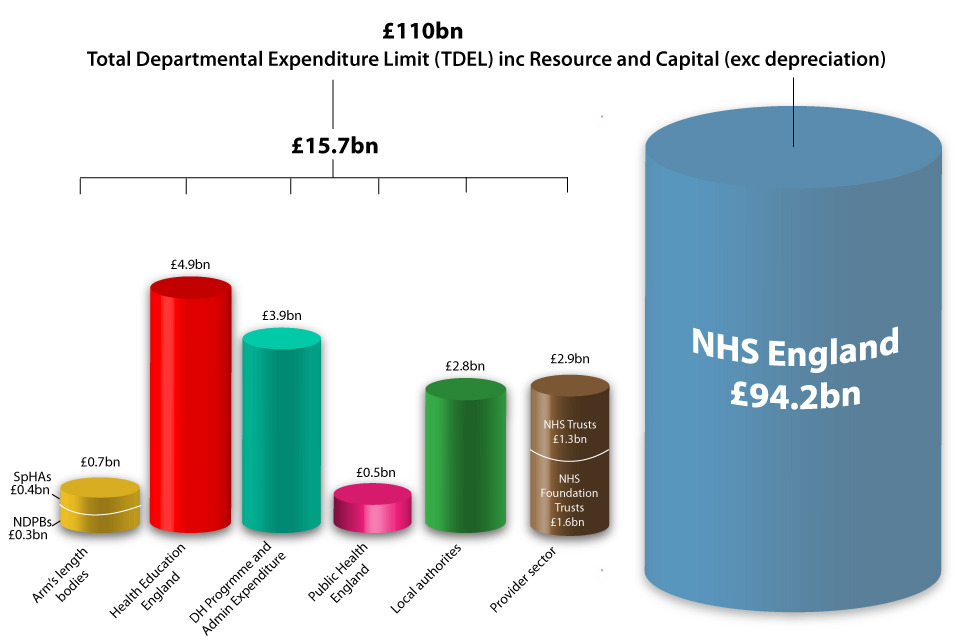
Chart showing financial allocations for 2013-14
Our resources
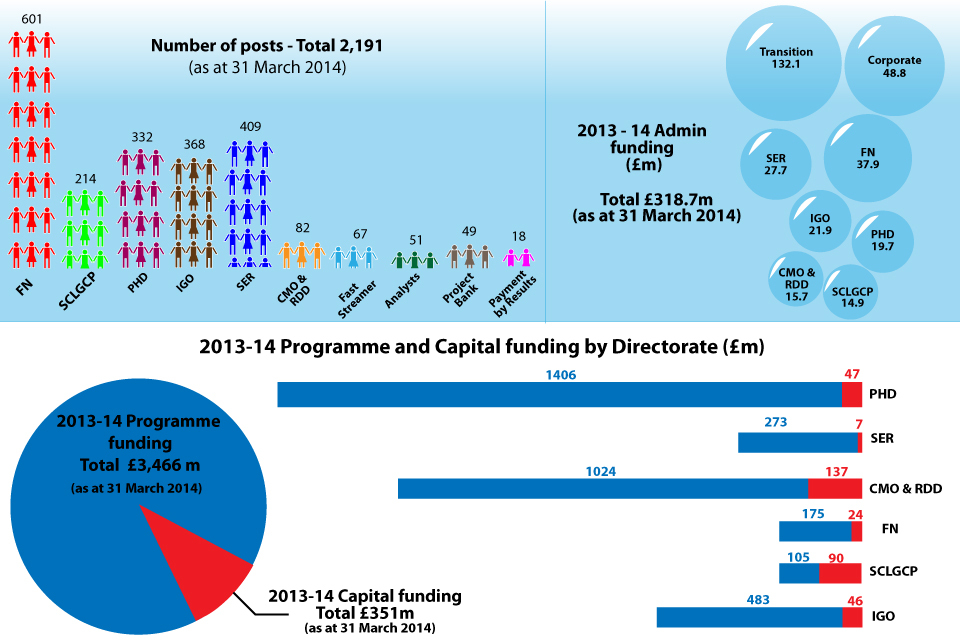
Our resources - as at 31 March 2014
Our achievements in financial year 2012 to 2013

Image showing DH achievements in 2012-13
Better Health and Wellbeing for all
- we launched the 2nd phase of the Be Clear on Cancer campaign and were nominated as best new brand by the Marketing Society
- we concluded the second-hand smoke campaign in May having received 58,400 orders for SmokeFree Kits, 36,500 orders for Quit Kits and 450,000 visits to the SmokeFree website
- we launched several high-profile public health campaigns, including the successful “Stoptober” where support was provided to those staff who wished to use this opportunity to stop smoking
- we successfully launched the Pertussis (whooping cough) programme for pregnant women
- we signed a Memorandum of Co-operation with the Equality and Human Rights Commission to continue improvement in equality
- we successfully delivered the Olympic and Paralympic Health Programme
- we initiated the national roll out of personal budgets for chronic/long-term conditions
- we increased access to NICE recommended psychological therapies for depression and anxiety to meet a minimum of 10% amongst the adult population
- over 125,000 people signed up to the information service for patients which we have extended to cover babies up to 6 months old
Better Care for all
- we published the Patient Choice Framework which gives a clear statement to patients and the public of the choice available to them
- we published the Adult Social Care Outcomes Framework for 2013 to 2014
- we launched HealthWatch nationally and enabled the first local HealthWatch to be set up
- we established Health Education England and NHS Trust Development Authority
- NHS111 took its 1 millionth call; now covering 10% of the population
- we made £22 million available to 21 pioneering research projects to boost dementia diagnosis rates and develop new treatments
- we published the final report of the department’s review following the events at Winterbourne View hospital, including clear timeframes for action to improve outcomes for people with learning disabilities, autism and challenging behaviours
- we published the Care and Support White Paper and developed the implementation plan
- we published the Draft Care and Support Bill for pre-legislative scrutiny
- we extended the information service for patients to cover babies up to 6 months old – over 70,000 people have signed up to the service
- we invited the NHS to bid for £50m capital to fund improvements for people with dementia
- we provided £800m over 5 years for new Biomedical Research Centres and Units to pull advances in basic science into benefits for NHS patients
- we have agreed an implementation framework for the mental health strategy
- we engaged 471,466 patients in NIHR Clinical Research Network Portfolio studies, 11,466 more than in 2011
- we published the Social Care White Paper
- we have commenced the process of Medical Revalidation regulation ensuring doctors keep up to the professional standards expected
- we published with the National Skills Academy the Leadership Qualities Framework for Adult Social Care
Better Value for all
- we achieved £5.8bn savings in financial year 2011 to 2012 towards delivering £20bn QIPP savings by financial year 2014 to 2015 and we are on target for achieving £5bn in financial year 2012 to 2013 ahead of trajectory
- we contributed to the Government’s plans for economic growth through a range of National Institute for Health Research (NIHR) initiatives that support collaborations between the life sciences industry and the NHS research infrastructure
- we supported 364 new life-sciences industry studies through the NIHR Clinical Research Network, 77 more than in 2011
- we implemented a suite of NHS Pay and Pensions reform programmes that will provide value for money for patients and the public
Successful Change
- we managed the transition programme and successfully delivered the new Health and care system, abolishing SHAs and PCTs, transforming NHS management, creating a new Public Health system and transferring major new responsibilities to local authorities
- we delivered a restructured, more efficient DH, with improved capabilities, while managing the transition programme
- we fully established the NHS Commissioning Board (now NHS England) and Public Health England and completed the transfer of functions to the Health Research Authority
- we established Health Education England to deliver excellence in education and training and quality in patient care
- we developed the NHS Property Services Limited to provide a solution for the future ownership and management of the PCT estate
Our Partners
- we published the Armed Forces Covenant to meet requirement of Armed Forces Act 2011, providing transparency on delivery of Government commitments
- we ensured that from 29 October 2012 compensation payments to the seriously injured, under the Armed forces Compensation Scheme, will not need to be used to pay for social care
- we secured £50 million, from the Capital Funding Programme for Energy Efficiency funding, to support an NHS aim of carbon reduction of 10% by 2015
The DH itself
- we delivered the best Parliamentary Questions/Freedom Of Information/Ministerial Correspondence performance in Whitehall – during a period of ministerial change and transition
- we published the DH Digital Strategy, which will make DH a digital leader in Whitehall
- we established a Partnerships and Information division that will focus on improving the DH’s relationships with national stakeholders
Our arm’s length bodies
Image showing logos of DH arm's length bodies
Our ALBs have published information about:
- what they do
- what they achieved in financial year 2012 to 2013
- their business priorities for financial year 2013 to 2014
departmental leaders talk about the role of their directorates
Departmental leaders talk about the role of their Directorate
Annex A
Our ministers
Rt Hon Jeremy Hunt MP, Secretary of State for Health
Responsibilities include:
- overall financial control
- oversight of NHS delivery & performance, and implementation of reform
- relationship with NHS England and Monitor
Norman Lamb MP, Minister of State for Care and Support
Responsibilities include:
- older people, including dementia
- long-term conditions
- adult social care
- quality regulation, NHS Constitution, Health and Wellbeing boards
Jane Ellison MP, Parliamentary Under Secretary of State for Public Health
Responsibilities include:
- preventing avoidable mortality
- relationship with Public Health England and the public health system
- health protection and improvement
- vaccination
Dr Daniel Poulter MP, Parliamentary Under Secretary of State for Health
Responsibilities include:
- patient experience
- nursing, midwifery, allied health professionals
- NHS workforce including pay, pensions, education and training
- health visiting
Earl Howe, Parliamentary Under Secretary of State for Quality (Lords)
Responsibilities include:
- reform including NHS England and Clinical Commissioning Groups
- primary and urgent care, including dentistry
- economic regulation and provider policy
- research and development
Our non-executive board members
Catherine Bell
Catherine has been a non-executive Board member since December 2010. Catherine spent her executive career as a civil servant, and was Permanent Secretary at the Department for Business, Innovation & Skills. She now holds a number of non-executive roles across the public, private and not-for-profit sectors.
Peter Sands
Peter was appointed a non-executive Board member in April 2011. Peter has been Group Chief Executive of Standard Chartered plc since 2006, following four years as Group Finance Director. Prior to this, he was Director and senior partner at McKinsey & Co. Peter had been with McKinsey since 1988 where he worked extensively in the banking and technology sectors in a wide range of international markets. Before joining McKinsey, Peter worked for the UK’s Foreign and Commonwealth Office.
Chris Pilling
Chris is Chief Executive Officer of Yorkshire Building Society and was appointed a non-executive Board member in March 2011. Previously Chris spent six years at HSBC in various posts (including Head of Customer Service & Sales for its national branch network) and chief executive of First Direct.
Mike Wheeler
Mike has been a non- executive Board member at the Department of Health since 2006 and is chair of the Department’s Audit and Risk Committee. He is a senior adviser or non-executive director of various institutions both in London and overseas. A large part of Mike’s career was spent at the integrated accounting firm, KPMG.
Our leadership team
Una O’Brien, Permanent Secretary and Accounting Officer
Responsibilities include:
- overall leadership of the Department of Health, which is responsible for the nation’s health and wellbeing, setting priorities, driving improvements and providing funding and accountability to reflect what people value most
- as the Department’s Accounting Officer, answerable to Parliament for ensuring DH runs efficiently and spends its money appropriately
Professor Dame Sally Davies, Chief Medical Officer and Research and Development
Responsibilities include:
- independent advisor to Secretary of State for Health and the UK Government on all medical matters
- Chief Scientific Advisor to the Department
- supporting the government to ensure decisions on health and social care are based on the most up to date and reliable research evidence
- enabling research in the NHS to support economic growth
Charlie Massey, Director General: Strategy and External Relations
Key directorate objectives:
- set the policy, strategy and outcomes for information to support patients and public
- oversee the framework to improve engagement between the Department and the public, to improve policy-making and outcomes
- work with stakeholders across the system to lead policy on pay, pensions, education and training
- lead on behalf of the whole system, the government’s response to the Francis Inquiry
Karen Wheeler, Director General: Information and Group Operations
Key directorate objectives:
- manage successful delivery of the transition programme and ongoing legacy
- lead work to build new Department capabilities – people, systems, processes and estates – alongside Civil Service
- develop and implement excellent corporate governance, audit, assurance and sponsorship for DH and ALBs
- deliver ministers’ priorities for efficient, effective NHS estates and facilities
Felicity Harvey, Director General: Public Health
Key directorate objectives:
- strategy, policy and outcomes for public health, sponsoring PHE and working with NHS England and ALBs to improve and protect population health
- lead on international business, representing Government overseas on health issues
- provide professional leadership and advice on public health and community nursing
- lead for science and bioethics, including embryology and genetics
Jon Rouse, Director General: Social Care, Local Government and Care Partnerships
Key directorate objectives:
- set the strategy, policy and outcomes for dementia, older people, people with disabilities, mental health, children and families, health inequalities, offender health, military health and social exclusion
- oversee social care finance and investment and lead across government on carers
- build effective partnerships with local government, voluntary and community sectors to improve health and care outcomes.
Richard Douglas, Director General: Finance and NHS
Key directorate objectives:
- assure the performance of the new health and care system through effective stewardship and sponsorship of key ALBs
- oversee the improvement of health outcomes
- discharge DH’s financial management responsibilities effectively and efficiently, and lead on growth, value for money
- lead the growth of DH’s policy, strategy and analytical capability and the embedding of commercial skills
Annex B: Performance against milestones for quarter 1
Strategy and External Relations
| Target | Achieved (Y/N) | If not achieved; why have the milestones not been met, and what action has been taken? |
|---|---|---|
| launch new Health & Social Care Information Centre, HEE and the Local Education & Training Boards | Y | - |
| publish Dame Fiona Caldicott review of Information Governance | Y | - |
| complete re-brand DH in line with single government brand | Y | - |
| review and deliver the Cavendish Review’s recommendations | Y | - |
| complete NHS complaints handling review for Secretary of State | No | review extended to accommodate all the evidence received. Completion scheduled for September |
| Deliver formal response to Information Governance Review | No - external reasons | full Government response – including all relevant ALBs - being developed for September or October |
| publish ‘Information Strategy – one year on’ report | No - external reasons | report being developed to reflect work led by NHS England (planning guidance, safer hospital guidance and technology strategy |
| complete design of rules for new NHS pension scheme | No - external reasons | good progress has been made with business rules for the new scheme but delays encountered due to added HMT process – expected to be completed by September 2014 |
Information and Group Operations
| Target | Achieved (Y/N) | If not achieved; why have the milestones not been met, and what action has been taken? |
|---|---|---|
| put in place a sponsorship development programme to support sponsorship capabilities | Y | - |
| implement new DH governance arrangements (April to June) | Y | - |
| launch next stage of Department of Health’s change programme (May to June) | Y | - |
| announce successful dementia pilot schemes and funding allocations | Y | - |
| launch Patient-Led Assessment of Care Environment (PLACE) | Y | - |
Public Health
| Target | Achieved (Y/N) | If not achieved; why have the milestones not been met, and what action has been taken? |
|---|---|---|
| establish Public Health England | Y | - |
| agree new statutory arrangements for public health in local government | Y | - |
| publish refreshed ‘Health Visiting Call to Action’ | Y | - |
| establish UK Rare Disease Forum | Y | - |
| run side event on Anti Microbial Resistance at World Health Assembly | Y | - |
| confirm ministerial agreement to procure 100,000 genomes initiative | Y | - |
| agree new, UK-wide Front of Pack nutritional labelling scheme | Y | - |
| publish lessons learned from Drugs & Alcohol Payment by Results pilots | N - external Reasons | did not take place due to delays with the Home Office clearance process. We intend to publish by the end of September. |
Social Care, Local Government and Care Partnerships
| Target | Achieved (Y/N) | If not achieved; why have the milestones not been met, and what action has been taken? |
|---|---|---|
| review care plans - NHSE/Local Government Association Winterbourne View action | N | The small number of reviews reported as outstanding in June have now been completed. NHS England is undertaking additional work in respect of patients in secure mental health and CAMHS beds funded by specialist commissioning. |
| establish Mental Health Act Approvals Panels | Y | - |
| commence review of adult social work education | Y | - |
| publish first mental health dashboard | N | expecting publication end of August or early September |
| launch Value Based Recruitment tools | Y | - |
| publish the ‘One year On’ progress report on PM Challenge on Dementia | Y | - |
| commence Review of Statutory Autism Strategy | Y | - |
| launch domestic abuse pledge and toolkit for employers in ‘Public Health Responsibility Deal’ | Y | - |
Finance and NHS
| Target | Achieved (Y/N) | If not achieved; why have the milestones not been met, and what action has been taken? |
|---|---|---|
| issue 2013 to 2014 ‘NHS Manual for Accounts’ | N | the draft NHS Manual for Accounts is being updated for comments following consultation. A final draft will be resubmitted to Financial Reporting Advisory Board (FRAB) by early September |
| launch Department of Health’s Baseline Review | Y | - |
| ensure NHS Property Services Limited becomes fully operational | Y | - |
| publish Open Public Services update Choice Frameworks for social care and health | Y | - |
| put in place new governance structure for effective sponsorship of Monitor | N | a new governance structure has been agreed between DH and Monitor. Q1 accountability meetings have taken place and worked well. The Public Parliamentary Accountability (PPA protocol) has also been agreed. The Framework Agreement is with Monitor and HMT for sign off ahead of Monitor Board approval in September |
| include CQC related provisions in the Care and Support Bill | Y | - |
| lay regulations in Parliament on pricing and the licensing regime | Y | - |
| agree content of 2015 to 2016 Spending Settlement | Y | - |
| complete DH Core element of 2012 to 2013 statutory account for audit | Y | - |
| complete the draft consolidated 2012 to 2013 accounts for audit | Y | - |
| put in place new process of performance assurance against NHSE Mandate | Y | - |
| complete sale of Plasma Resources UK | N - external Reasons | Bain Capital purchased 80% of Plasma Resources UK (PRUK) from the Department of Health on 17 July. We are awaiting approval for the sale from the Chief Secretary to the Treasury |
Research and Development
| Target | Achieved (Y/N) | If not achieved; why have the milestones not been met, and what action has been taken? |
|---|---|---|
| complete strategic vision for research on dementia | Y | - |
| prepare legislation to establish the HRA as a Non-Departmental Public Body | Y | - |
| implement the Academic Training Programme with HEE | Y | - |
Annex C: Performance against milestones for quarter 2
Strategy and External Relations
| Target | Achieved (Y/N) | If not achieved; why have the milestones not been met, and what action has been taken? |
|---|---|---|
| complete NHS complaints handling review for Secretary of State (brought forward from Q1) | N - external reasons | this was an independent report, chaired jointly by Ann Clwyd MP and Prof Tricia Hart, and was published on 28 October |
| deliver formal response to Information Governance Review (brought forward from Q1) | Y | - |
| publish ‘Information Strategy – one year on’ report (brought forward from Q1) | No - external reasons | Secretary of State will provide updates on achievements in the autumn |
| complete design of rules for new NHS pension scheme (brought forward from Q1) | No - external reasons | finalisation across public sector schemes by HMT has caused delays, completion of the design of business rules will be in December |
| NHS Jobs system goes live | N | there were delays due to problems with the new system, the expected launch date is now November |
| develop new digital consultation product | N | on track to roll out a new digital consultation product by April 2014, several major consultations have resulted in scope of project being refined |
| submit written evidence to the NHS PRB and DDRB | Y | - |
| Fully establish governance processes for HSCIC Board | Y | - |
Information and Group Operations
| Target | Achieved (Y/N) | If not achieved; why have the milestones not been met, and what action has been taken? |
|---|---|---|
| launch the Development Ambassador Network | Y | - |
| allocate funding to NHS estates critical infrastructure priorities | No - external reasons | due to re-prioritisation, the original central capital allocation for this scheme could not be awarded. The Department will be working with the NHS Trust Development Authority and Monitor to explore ways forward in addressing the critical infrastructure risks in NHS Trusts and Foundation Trusts. This will include encouraging trusts to prioritise their own capital to reduce risks to patient safety |
Public Health
| Target | Achieved (Y/N) | If not achieved; why have the milestones not been met, and what action has been taken? |
|---|---|---|
| publish lessons learned from Drugs & Alcohol Payment by Results pilots (brought forward from Q1) | No - external reasons | Home Office delayed publication, now likely to be late Q3 |
| introduce Rotavirus immunisation into children’s immunisation programme | Y | - |
| publish EU ‘Review of the balance of competences: Health’ | Y | - |
| publish first antimicrobial Resistance report | Y | - |
| publish consultation on migrant access to NHS | Y | - |
| introduce shingles immunisation for 70-79 year olds plus catch-up programme | Y | - |
| NEW: establish programme board to oversee the actions in area 1 (to develop nurses and midwives as health promoting practitioners will be based on “Making every contact count”) | Y | - |
| NEW: reach ministerial agreement on the future of the Nursing and Care Quality Forum | Y | - |
Social Care, Local Government and Care Partnerships
| Target | Achieved (Y/N) | If not achieved; why have the milestones not been met, and what action has been taken? |
|---|---|---|
| review care plans - joint NHSE / Local Government Association Winterbourne View Action (brought forward from Q1) | Y | - |
| publish first mental health dashboard (brought forward from Q1) | N | the launch will now take place in Q3 either on its own or as part of a package of related policy announcements |
| roll out Information Service for Parents automatic sign up across maternity suppliers | No - external reasons | funding to support automatic sign up rollout has not yet been released by Cabinet Office Efficiency and Reform Group. A strategy has been agreed with Start4Life for a further approach to ERG to obtain funding release |
| undertake a scoping study which will be shared with Skills for Care for consideration as part of the ‘refresh’ | Y | - |
| Children and Young People’s Health Outcomes Annual Summit takes place | Y | - |
Finance and NHS
| Target | Achieved (Y/N) | If not achieved; why have the milestones not been met, and what action has been taken? |
|---|---|---|
| Issue 2013 to 2014 ‘NHS Manual for Accounts’ (brought forward from Q1) | N | the Manual for Accounts was approved and published in October |
| put in place new governance structure for effective sponsorship of Monitor (brought forward from Q1) | Y | - |
| complete sale of Plasma Resources UK (brought forward from Q1) | Y | - |
| complete and lay the 2012 to 2013 annual report & accounts | Y | - |
| submit DH evidence for the next Health Select Committee on CQC | No - external reasons | evidence submitted in October |
| seek approval from ministers for the commercial model for NHS Property Services Ltd | N | since April NHS PS have been focussing on post transition issues, these issue are currently with ministers |
| launch second stage dental pilots (2nd wave – salaried) | Y | - |
| provide 2014 to 2015 tariff package to NHSE and Monitor for statutory consultation | Y | - |
Research and Development
| Target | Achieved (Y/N) | If not achieved; why have the milestones not been met, and what action has been taken? |
|---|---|---|
| announce research commissioned under the National Institute for Health Research/Economic & Social Research Council joint call for research on living well with dementia | Y | - |
| commence contracts and funding for Diagnostic Evidence Cooperatives | Y | - |
Annex D: Performance against milestones for quarter 3
Finance and NHS
| Target | Achieved (Y/N) | If not achieved; why have the milestones not been met, and what action has been taken? |
|---|---|---|
| Issue 2013-14 ‘NHS Manual for Accounts’ (brought forward from Q1) | Y | - |
| Submit DH evidence for the next Health Select Committee on CQC (brought forward from Q2) | Y | - |
| Seek approval from Ministers for the commercial model for NHS Property Services Ltd (brought forward from Q2) | N | The future model for NHS will not be decided for a further two years. NHS PS is currently focussing on property disposals, and restructuring. Discussions will continue at Ministerial level |
| Publish Secretary of State’s Annual Report | N | Production and publication delayed due to report not being finalised, work on-going to complete and revised publication date to be agreed with comms. Additional resources identified to support delivery |
| Refresh Mandate and NHS Outcomes Framework | Y | - |
| Finalise proposals for the transformation of Business Service Authority | N - External Reasons | Conversations are being held with the Cabinet Office about the future model for the BSA. Agreement is expected to be reached in the next 3-6 months |
| Create National Clinical Category Review Group | Y | - |
| Update Autumn Statement Strategy for UK Life Sciences | Y | - |
| Create regional procurement skills networks | N | The on-line academy will be launched in 6 months. Other networks will be rolled-out subsequently. This workstream has been delayed as a result of focusing on appointing a Procurement Champion |
| Commence implementation of Clinical Leadership in Procurement | Y | - |
| Publish 2012-13 Reference Costs collection and 2013-14 Reference Cost guidance | Y | - |
| Order to be laid in Parliament approving Monitor’s licensing criteria | Y | - |
Information and Group Operations
| Target | Achieved (Y/N) | If not achieved; why have the milestones not been met, and what action has been taken? |
|---|---|---|
| Publish ‘Information Strategy – one year on’ report (brought forward from Q1) | N - External Reasons | A system-wide informatics strategy and information plan is being developed which will obviate the need for a “one year on” report. This milestone will therefore be removed. |
| Allocate funding to NHS estates critical infrastructure priorities (brought forward from Q2) | N - External Reasons | Due to re-prioritisation, this scheme could not be funded. Risk will be managed across the system and regulators will build in assurance that risk in managed by providers. This milestone will therefore be removed. |
| Complete Director and Deputy Director Talent Review | Y | - |
| Launch Leadership Development Programme (Team Leaders) | Y | - |
| Review package of flexible working policies for DH | Y | - |
| Complete NHS England and new arm’s length bodies accommodation | N - External Reasons | Waiting on NHS England and Public Health England to complete its accommodation in Leeds. Plans to vacate are now in place. The milestone will now be fully achieved during Q4 2013-14. |
| Make available online, GP practices which offer online access to patients’ own records | Y | - |
Public Health
| Target | Achieved (Y/N) | If not achieved; why have the milestones not been met, and what action has been taken? |
|---|---|---|
| Publish lessons learned from Drugs & Alcohol Payment by Results pilots (brought forward from Q1) | N - External Reasons | This publication was always going to be an annex to a bigger Home Office publication, and because HO have delayed their publication, this has slipped through no fault of ours. We are planning to issue a full ‘lessons learned’ document in May/June and that is all that is now needed in policy terms. |
| Agree 2014-15 Section 7A with NHS England | Y | - |
| Publish UK Rare Diseases Plan | Y | - |
| Publish 2nd annual reports from Responsibility Deal partners | Y | - |
| NEW 2014/15 Section 7A Agreement between DH and NHS England and Service Specification No. 27 published and associated allocation agreed | Y | - |
| NEW CPRD commenced Breast & Cosmetic Implant Registry pilot | Y | - |
Social Care, Local Government & Care Partnerships
| Target | Achieved (Y/N) | If not achieved; why have the milestones not been met, and what action has been taken? |
|---|---|---|
| Publish first mental health dashboard (brought forward from Q1) | Y | - |
| Roll out Information Service for Parents automatic sign up across maternity suppliers (brought forward from Q2) | N - External Reasons | Proof of concept was achieved but the process identified the need for extensive stakeholder engagement to support successful national rollout. This work is being re-scoped to be included in the 2014-15 work programme. |
| Launch updated Adult Social Care Outcomes Framework (ASCOF) for 2014-15 | Y | - |
| Publish cross government carers strategy action plan 2013-2015 | N | Development of Action Plan delayed due to pressures of work associated with Care Bill. Plan now due to be published by the end of March |
| Publish the ‘Progress on Health Care’ chapter in the Armed Forces Covenant Annual Report | Y | - |
| Report on first year progress against Winterbourne View Action Plan | Y | - |
Strategy and External Relations
| Target | Achieved (Y/N) | If not achieved; why have the milestones not been met, and what action has been taken? |
|---|---|---|
| Complete design of rules for new NHS pension scheme (brought forward from Q1) | N - External Reasons | Almost complete - revised to January 2014 due to HMT delays |
| Complete NHS complaints handling review for Secretary of State (brought forward from Q1) | Y | - |
| NHS Jobs system goes live (brought forward from Q2) | N | Problems identified during testing of the new system have resulted in delays due to amendments required to the system. Launch now March 2014 after further user testing and training. |
| Develop new digital consultation product (brought forward from Q2) | N | On track to roll out a new digital consultation product by April 2014. Consultations held has resulted in scope of project being refined. |
| Implement revised access arrangements and complete full revaluation of NHS Pension Scheme | N - External Reasons | As before - amended implementation date of April 2014 to ensure HMT clearance, regulatory development and monitoring provisions in NHS BSA. |
| Deliver full response to Report of Mid Staffordshire NHS Trust Public Inquiry | Y | - |
| Agree Long Term Pension Contribution Structure | N - External Reasons | We are expecting to have this concluded by March/April 2014. Discussions held with TUs and Employers and need final sign off by HMT. |
| Publish updated HEE mandate for 2014-15 onwards | N - External Reasons | Working towards February 2014 publication. Earlier publication not possible due to clash with Care Bill currently going through House of Commons Committee (covers establishment of HEE as a NDPB). |
| Put in place Indemnity Review legislation | N | Funding issue with Independent Midwives UK (IMUK) unresolved. Ministerial reluctance to sign off the Impact Assessment to go to the Regulatory Policy Committee (RPC) before resolution. |
| Define roles & functions of the CQC Chief Inspectors and recruit to posts |
Research and Development
| Target | Achieved (Y/N) | If not achieved; why have the milestones not been met, and what action has been taken? |
|---|---|---|
| Announce research commissioned on physical activity | Y | - |
| Confirm newly designated Academic Health Science Centres | Y | - |
| Enhance Clinical Trials Gateway information | Y | - |
Annex E: Performance against milestones for quarter 4
Finance and NHS
| Target | Achieved (Y/N) | If not achieved; why have the milestones not been met, and what action has been taken? |
|---|---|---|
| Seek approval from Ministers for the commercial model for NHS Property Services Ltd (brought forward from Q2) | N | The future model for NHS will not be decided for a further two years. Discussions will continue at Ministerial level |
| Publish Secretary of State’s Annual Report (brought forward from Q2) | N | Decision taken not to publish a 2012-13 report since it was not a legal requirement. |
| Finalise proposals for the transformation of Business Service Authority (brought forward from Q2) | N - External Reasons | Dicussions still being held with the Cabinet Office about the future model for the BSA. Agreement is expected to be reached in the next 3 months |
| Create regional procurement skills networks (brought forward from Q3) | N | The on-line academy will be launched in 3 months. Other networks will be rolled-out subsequently. Work has been delayed pending an appointment of a Procurement Champion |
| Put in place new pricing arrangements for branded medicines | Y | |
| Submit Plan for the transformation of Business Services Authority and delivery of BSA commercial review | Y | |
| Respond to NAO hospital waiting lists study report | Y |
Information and group operations
| Target | Achieved (Y/N) | If not achieved; why have the milestones not been met, and what action has been taken? |
|---|---|---|
| Complete NHS England and new arm’s length bodies accommodation (brought forward from Q3) | Y | |
| Complete post implementation transition work, and establish a legacy closedown team to oversee remaining residual activity in 2014/15 | Y | |
| Undertake year-end assessment of sponsor capability | Y | |
| Complete next stage of DH’s Change Programme | Y | |
| Complete Dementia schemes and initiate final draft of dementia report | Y | |
| Commence pre-migration work for first wave implementations of Shared Services for Finance, HR and Payroll | Y |
Public Health
| Target | Achieved (Y/N) | If not achieved; why have the milestones not been met, and what action has been taken? |
|---|---|---|
| Publish lessons learned from Drugs & Alcohol Payment by Results pilots (brought forward from Q1) | N - External Reasons | This publication is an annex to a bigger Home Office publication, and because HO have delayed their publication, this has slipped. We are planning to issue a full ‘lessons learned’ document in May/June 2014. |
| Roll-out the Bowel Scope Screening Programme to 30% of the country | Y | |
| Put in place strategy to sequence 100,000 whole genomes | Y |
Social care, local government and care partnerships
| Target | Achieved (Y/N) | If not achieved; why have the milestones not been met, and what action has been taken? |
|---|---|---|
| Roll out Information Service for Parents automatic sign up across maternity suppliers (brought forward from Q2) | N - External Reasons | Extensive stakeholder engagement reqiured to support successful national rollout. The work is being re-scoped to be included in the 2014-15 work programme. |
| Publish cross government carers strategy action plan 2013-2015 (brought forward from Q3) | N | Development of Action Plan delayed due to pressures of work associated with Care Bill and policy development with partners. Plan to publish in May. |
| Announce Strategic Partners scheme for 2014-15 | Y | |
| Publish Statutory Review of Autism Strategy | Y | |
| Secure increase in Family Nurse Partnership places to 13,000 | Y | |
| Develop action plan for the Coalition Commitment on Information Sharing to Tackle Violence under the remit of the Task and Finish Group | Y | |
| Publish declaration on confidentiality and suicide prevention | Y | |
| Publish Health Working Group report on child sexual exploitation | Y |
Strategy and external relations
| Target | Achieved (Y/N) | If not achieved; why have the milestones not been met, and what action has been taken? |
|---|---|---|
| Complete design of rules for new NHS pension scheme (brought forward from Q1) | Y | |
| NHS Jobs system goes live (brought forward from Q2) | Y | |
| Develop new digital consultation product (brought forward from Q2) | Y | |
| Implement revised access arrangements and complete full revaluation of NHS Pension Scheme (brought forward from Q3) | N - External Reasons | Amended implementation date of April 2014 to ensure HMT clearance, regulatory development and monitoring provisions in NHS BSA |
| Agree Long Term Pension Contribution Structure (brought forward from Q3) | N - External Reasons | We are expecting to have this concluded by April 2014. Discussions held with TUs and Employers and need final sign off by HMT. |
| Publish updated HEE mandate for 2014-15 onwards (brought forward from Q3) | N - External Reasons | Home Affairs Committee clearance was sought on 12 February and received on 21 March. Anticipate that the mandate will be published on 1 May. |
| Put in place Indemnity Review legislation (brought forward from Q3) | N | Delays to the Indemnity S60 Order have occurred due to the handling of issues around the effects of implementation on independent midwives and their ability to practise as self-employed individuals outside any organisational structure. The aim is lay the Order just after the Easter recess. |
| Secure national collective agreement to changes in consultant and junior doctors’ contracts and Clinical Excellence Awards | N | Government accepted BMA and NHS Employers concerns about timescale. Government agrees that implementation of new arrangements will be from 2015 not 2014. |
| Publish Freedom of Information (FOI) & Correspondence Annual (Jan – Dec 2013) Performance Reports | Y | |
| Transfer Medical Revalidation governance oversight to NHSE | Y | |
| Put in place new NHS Pensions Scheme Design | N | Draft regulations for new pension scheme in preparation |
Research and development
| Target | Achieved (Y/N) | If not achieved; why have the milestones not been met, and what action has been taken? |
|---|---|---|
| Announce successful NIHR Health Protection Research Units | Y | |
| Commence contracts for designation and funding of NIHR Collaborations for Leadership in Applied Health Research and Care | Y | |
| Reconfigure Local Clinical Research Networks | Y |
