UK funded vaccines save Rohingya children from deadly diphtheria outbreak
UK is contributing to a vaccination programme which will protect more than 350,000 vulnerable Rohingya children from a deadly outbreak of diphtheria.
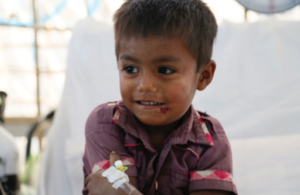
Four-year-old Anawar has beaten diphtheria thanks to the efforts of British medics in Kutupalong camp, Bangladesh. Picture: Russell Watkins/DFID
The UK has once again led the response to the Rohingya crisis in Bangladesh, by contributing to a vaccination programme which will protect more than 350,000 vulnerable Rohingya children from a deadly outbreak of diphtheria.
The vaccination campaign, which began in December, is due to run until February, has already ensured more than 315,000 children aged between six-weeks and 15-years-old, living in or near the world’s biggest camp in Cox’s Bazar, are protected.
Overcrowded camps in Cox’s Bazar are a breeding ground for contagious diphtheria, with 100 new cases every day.
Since late 2017, there have been nearly 4,000 suspected cases and at least 31 deaths. More than half the deaths relate to children under the age of five.
Diphtheria is especially dangerous for children. It is fast spreading and fatal, causing extreme breathing difficulties, inflammation of the heart which can lead to heart failure, problems with the nervous system and fatal paralysis.
In tandem with the vaccination campaign, which is being carried out by UNICEF, the UK has also provided specialist expertise in the form of British doctors, nurses, paramedics and midwives, who are treating diphtheria patients.
Only three weeks after arriving in the camps, the skills of the 40-strong UK aid-funded Emergency Medical Team have made a significant difference and saved countless lives, including that of four-year-old Anowar.
He was referred to the treatment centre at 9am last Monday (January 8), in a weak and lethargic condition and displaying symptoms of diphtheria.
Anowar’s symptoms were so severe; the clinicians decided that he needed diphtheria anti-toxin immediately in addition to a course of antibiotics. By 4pm that afternoon his health had improved significantly, and he was soon released to complete his treatment in the care of his relieved family. He is now doing well and looked healthier when he visited the treatment centre on Thursday 11 January for a check-up.
The intervention of the UK medics undoubtedly saved Anowar’s life but it has also had a wider impact as clinicians were also able to treat his entire family with precautionary antibiotics, preventing them from going through the same suffering as Anowar.
The Rohingya have fled to Bangladesh from neighbouring Burma following persecution by its military. In November 2017, the International Development Secretary visited Cox’s Bazar where she announced extra UK aid for the humanitarian crisis, ensuring more lives are not put at risk when international funding starts to run out in February 2018.
International Development Secretary Penny Mordaunt said:
It is difficult to comprehend the depth of human suffering among the hundreds and thousands of Rohingya who have fled persecution in Burma. Many have sought refuge in Bangladesh, but their plight is far from over as diphtheria, an entirely preventable disease, is claiming the lives of those who thought they had finally reached safety.
British expertise and aid is saving lives in Cox’s Bazar, preventing and treating this deadly infection, helping children like Anowar.
In today’s world, no child should die from a preventable disease. The UK is giving hope and a chance to Rohingya families.
Notes for Editors:
- DFID is funding £2million of the $4.6 million cost (£3.4 million) required to vaccinate 351,458 children aged six-weeks to 15-years-old as part of the campaign.
- The wider UNICEF vaccination campaign will also vaccinate 130,000 school children living in host communities near to the camps in Cox’s Bazar.
- Funding for this vaccination campaign has been provided from the response budget announced on 23rd October and 27th November 2017.
- Medics have worked tirelessly to ensure the swift vaccination of those most at risk. To date 315,889 children have been reached.
- DFID is working in partnership with the government of Bangladesh to ensure that children living in the camps and host communities are vaccinated against this deadly disease.
- The UK’s Emergency Medical Team (EMT) is a collaboration between DFID, the NHS, Public Health England, UK Med – a register of NHS volunteers ready to deploy to emergencies, Handicap International and the UK Fire and Rescue Service. This is the first deployment of the EMT since it was verified by the World Health Organisation (WHO) in December 2016. UK medical personnel have previously been deployed to respond to Typhoon Haiyan in the Philippines in 2013 and the Nepal earthquake in 2015.
- The deployment will be funded from DFID’s Bangladesh humanitarian budget – up to £650,000 has been earmarked for the EMT.
- Diphtheria is a bacterial infection. It most often causes infection of the upper respiratory tract. Diphtheria is most commonly spread from person to person through respiratory droplets (coughs and sneezes), or by direct contact with either respiratory secretions or infected skin lesions. Respiratory diphtheria usually occurs after an incubation period of 2-5 days. It causes life-threatening airway obstruction if untreated.
- The first suspected case of diphtheria was reported on 10 November at an MSF clinic in Cox’s Bazar. The outbreak was confirmed through laboratory testing on 04 December 2017. As of 10/1, 3,868 suspected cases of diphtheria and 31 deaths have been reported.
- In response to the diphtheria outbreak in Cox’s Bazaar, existing clinical facilitates are being converted and scaled up. This is currently being led by Médecins Sans Frontières MSF and the International Organisation for Migration (IOM). However IOM and other international NGOs are unable to manage the complex care needs of these patients, which is why they require the support of UK staff.
- IOM will provide the medical facilities for the deployment. World Health Organisation (WHO) will provide drugs. The UK’s EMT will provide a specialised clinical team, clinical oversight, some key medical equipment not available in country, and accommodation and transport for staff.
- Following the request for international assistance by the World Health Organisation on 15 December, a UK EMT team travelled to Bangladesh to conduct an emergency assessment, and recommended the deployment of the EMT.
- Staff will be rotated out of Cox’s Bazaar after three weeks. Staff will have a diphtheria booster injection before deployment and will then be at minimal risk of contracting the disease.
- The UK has currently contributed £59 million to the crisis since 25 August 2017.
- Free-to-use video content is available to download here.
General media queries (24 hours)
Email mediateam@dfid.gov.uk
Telephone 020 7023 0600
If you have an urgent media query, please email the DFID Media Team on mediateam@dfid.gov.uk in the first instance and we will respond as soon as possible.