UK Emergency Medical Team heads home after bringing Bangladesh diphtheria outbreak under control
Medical professionals, including doctors, nurses and paramedics, will return this weekend having spent up to 6 weeks helping more than 3,000 displaced Rohingya.

The UK Emergency Medical Team pictured at Manchester Airport. Picture: Russell Watkins/DFID
The UK Emergency Medical Team (EMT), deployed to the camps of Cox’s Bazar in Bangladesh following a deadly outbreak of diphtheria, is heading home after bringing the disease under control.
Medical professionals, including doctors, nurses and paramedics, will return this weekend having spent up to six weeks triaging more than 3000 Rohingya people.
Almost 500 people were treated for diphtheria and were it not for British help, many could have died.

Dr Derek Sloan, a consultant in infectious diseases from Fife, Scotland, examines a young boy for symptoms of diphtheria in Kutupalong, Bangladesh
Stationed across three diphtheria treatment centres, the 40-strong UK aid-funded EMT prescribed precautionary antibiotics to the displaced men, women and children suspected to have the disease. Those displaying clear symptoms were immediately given live-saving diphtheria anti-toxin.
With the outbreak now under control, local Bangladeshi health professionals working for the International Organisation for Migration (IOM) have taken over from the UK clinicians and will work to completely stamp out this disease from the camps.
Ummul Jesmin, one of the Bangladeshi nurses who worked alongside the UK EMT, has also learned vital infection prevention and control skills. These will be essential should another infectious disease outbreak like cholera occur. Pleased with the opportunity to work alongside the EMT, Ummul had nothing but praise for her British colleagues.
Ummul Jesmin, one of the Bangladeshi medics who worked alongside the UK EMT and who will continue to tackle the outbreak now that the British team is leaving.
Diphtheria, entirely preventable through vaccination, surfaced within the camps in late 2017. To date, there have been over 5,000 suspected diphtheria cases and at least 37 deaths.
The overcrowded camps, home to over 655,000 Rohingya refugees who have fled persecution in neighbouring Burma, are a breeding ground for diphtheria.
The contagious disease can cause extreme breathing difficulties and inflammation of the heart. This can lead to heart failure, damage to the nervous system and fatal paralysis.
It is especially dangerous to children; more than half the deaths recorded relate to those under the age of five. The expertise of the British clinicians has saved countless lives including that of four-year-old Settara.
Settara was brought to a treatment centre by her mother Moriam in mid-January with a fever, sore throat and in pain.
One of the nurses instantly identified that Settara was displaying symptoms of diphtheria. Doctors admitted Settara immediately and gave her diphtheria anti-toxin along with a course of antibiotics.
Whilst Settara underwent treatment, the team established that Moriam had seven other children who had all been exposed to the disease. The entire family was provided with precautionary antibiotics and Settara went on to make a full recovery.
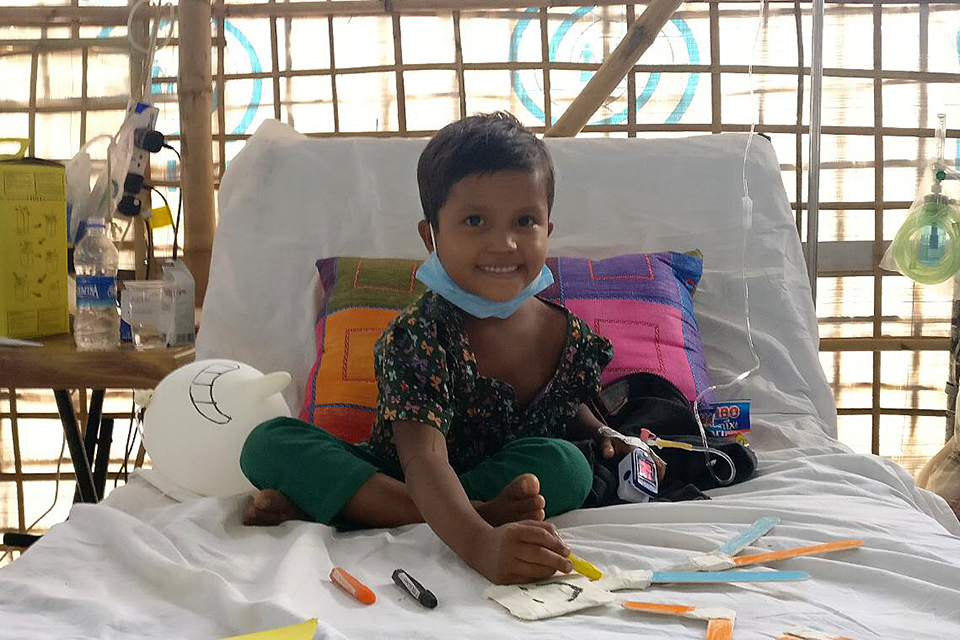
Six-year-old Sumaiya, sitting up in bed and already recovering after receiving diphtheria antitoxin treatment.
Six-year-old Samaiya was also brought to the treatment centre in mid-January with clear symptoms of diphtheria. Just a few hours after being given diphtheria anti-toxin, she started to look and feel much better and was seen happily sitting in bed drawing pictures. Samaiya was discharged shortly after to complete her course of antibiotics at home.
The UK, having led the way in providing medical expertise to the crisis, has also helped fund a UNICEF vaccination programme which protects vulnerable Rohingya children from diphtheria.
The first round of the vaccination campaign is now complete and has ensured more than 350,000 children aged between six-weeks and 15-years-old are protected. Children are now receiving their second dose of the vaccine; 110,513 have been vaccinated in the last week alone.
International Development Secretary Penny Mordaunt said:
I have nothing but admiration and thanks for the UK medics who travelled to Cox’s Bazar over the New Year to help victims of diphtheria, who, without UK support, would have died.
These medics embody everything that the UK stands for. We are a nation which does not shy away from our responsibility. When the desperate and the displaced are in need of our help we step in. We should be incredibly proud of this.
Our team has now handed their knowledge over to medics in Bangladesh so they can carry on the fight against diphtheria. Diseases have no respect for borders and this vital work is ultimately making the world a safer place.
Notes to Editors:
- The UK’s Emergency Medical Team (EMT) is a collaboration between DFID, the NHS, Public Health England, UK Med – a register of NHS volunteers ready to deploy to emergencies, Handicap International and the UK Fire and Rescue Service. This is the first deployment of the EMT since it was verified by the World Health Organisation (WHO) in December 2016. UK medical personnel have previously been deployed to respond to Typhoon Haiyan in the Philippines in 2013 and the Nepal earthquake in 2015.
- The deployment has been funded from DFID’s Bangladesh humanitarian budget – up to £650,000 has been earmarked for the EMT.
- The EMT deployed to Cox’s Bazar on 28 December 2017 and some staff were rotated out of Cox’s Bazaar after three weeks. Replacement clinicians were deployed in mid-January. All staff were given a diphtheria booster injection before deployment.
- Following the request for international assistance by the World Health Organisation on 15 December, a UK EMT team travelled to Bangladesh to conduct an emergency assessment, and recommended the deployment of the EMT.
- In response to the diphtheria outbreak in Cox’s Bazaar, existing clinical facilitates have been converted and scaled up. This was led by Médecins Sans Frontières MSF and the International Organisation for Migration (IOM). However IOM and other international NGOs are unable to manage the complex care needs of these patients, which is why they required the support of UK staff.
- IOM has provided the medical facilities for the deployment. The World Health Organisation (WHO) has provided drugs. The UK EMT provided a specialised clinical team, clinical oversight, some key medical equipment not available in country, and accommodation and transport for staff.
- Diphtheria is a bacterial infection. It most often causes infection of the upper respiratory tract. Diphtheria is most commonly spread from person to person through respiratory droplets (coughs and sneezes), or by direct contact with either respiratory secretions or infected skin lesions. Respiratory diphtheria usually occurs after an incubation period of 2-5 days. It causes life-threatening airway obstruction if untreated.
- The first suspected case of diphtheria was reported on 10 November at an MSF clinic in Cox’s Bazar. The outbreak was confirmed through laboratory testing on 04 December 2017. As of 30/1, 5,120 suspected cases of diphtheria and 37 deaths have been reported.
- DFID is working in partnership with the government of Bangladesh to ensure that children living in the camps and host communities are vaccinated against this deadly disease.
- DFID is funding £2 million of the $4.6 million cost (£3.4 million) required to vaccinate 351,458 children aged six-weeks to 15-years-old as part of the vaccination campaign.
- The wider UNICEF vaccination campaign will also vaccinate 130,000 school children living in host communities near to the camps in Cox’s Bazar.
- Funding for this vaccination campaign has been provided from the response budget announced on 23rd October and 27th November 2017.
- Medics have worked tirelessly to ensure the swift vaccination of those most at risk.
- The UK has currently contributed £59 million to the crisis since 25 August 2017.
General media queries (24 hours)
Email mediateam@dfid.gov.uk
Telephone 020 7023 0600
If you have an urgent media query, please email the DFID Media Team on mediateam@dfid.gov.uk in the first instance and we will respond as soon as possible.