New screening will protect babies from death and disability
Today the UK National Screening Committee announced its recommendation to screen every newborn baby in the UK for 4 new genetic disorders.
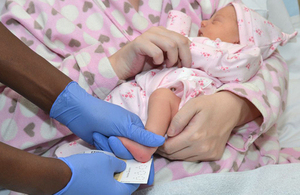
Blood spot test
This means expanding the current NHS Newborn Blood Spot Screening programme to screen for: homocystinuria (HCU), maple syrup urine disease (MSUD), glutaric aciduria type 1 (GA1) and isovaleric acidaemia (IVA).
Testing for these conditions as part of the current programme, leading to early detection and treatment, will prevent those babies affected from dying or being severely disabled for the rest of their lives.
Dr Anne Mackie, Director of Programmes for the UK National Screening Committee (UK NSC), which is supported by Public Health England, said:
We are delighted to announce our recommendation to expand the programme. We supported a pilot to look into the impacts of screening for these conditions. Since the start of the pilot in July 2012 more than 700,000 children in England have been tested for these disorders and 47 possible cases identified with 20 confirmed.
We will help similar numbers each year now the extension is being rolled out.
Babies currently have a heel prick blood test at 5 to 8 days old to test for 5 conditions where early detection and treatment will improve the long-term outcome for the child: phenylketonuria (PKU), congenital hypothyroidism (CHT), sickle cell disease (SCD), cystic fibrosis (CF) and medium-chain acyl-CoA dehydrogenase deficiency (MCADD).
The pilot programme was run by Sheffield Children’s NHS Foundation Trust in which over 700,000 babies across the country were screened for the new diseases in addition to the current 5 for which every newborn is currently screened. Following the results of this, the UK NSC was able to recommend extending the programme to screen for them.
Professor Jim Bonham, national lead for the pilot project and director for newborn screening at Sheffield Children’s NHS Foundation Trust, said:
This is fantastic news and everyone who has been involved in the pilot should be really proud of the part they have played in this development.
As a result of this study 20 children with serious but treatable disorders were discovered. We are delighted with the results because it shows how we can make an enormous difference for these children and their families, in some cases giving them the gift of life.
Ends
More information about the pilot programme and a case study is available from Sheffield Children’s NHS Foundation Trust on 0114 226 0678 or email communications@sch.nhs.uk.
Notes to editors:
- The UK National Screening Committee is independent of, but supported by Public Health England.
- Dr Anne Mackie, Director of Programmes for the UK NSC and Dr Robert Sheriff, National Operations Lead for the UK NSC will be available for interview on Friday 9 May.
- The NHS Newborn Blood Spot Screening Programme aims to identify babies who are at high risk of having certain serious but rare conditions before they develop symptoms. Screening is not the same as diagnosis; it identifies which babies need to go on to have diagnostic tests to determine whether or not they do have the condition. By detecting these conditions early it is possible to treat them and reduce their severity.
- More information about the expanded conditions is available on request.
- Public Health England’s mission is to protect and improve the nation’s health and to address inequalities through working with national and local government, the NHS, industry and the voluntary and community sector. PHE is an operationally autonomous executive agency of the Department of Health. www.gov.uk/phe Follow us on Twitter @PHE_Screening
UKHSA press office: screening